Clear Sky Science · en
Anti-DENV IgE correlates with dengue severity and triggers FcεRI-dependent basophil activation inhibited by Omalizumab
Why this matters for everyday health
Dengue is a mosquito-borne infection that can feel like a bad flu for some people, yet send others to the hospital with dangerous bleeding and shock. This study asks a simple but important question: why do some infected people get so sick while others recover with only mild symptoms? The researchers focus on a type of allergy-related antibody, IgE, and show how it may help drive severe dengue—and how an existing allergy drug might one day help stop that process.
A closer look at severe dengue
Dengue infection ranges from a short fever to life-threatening illness marked by leaky blood vessels and fluid loss. Doctors know that people who catch dengue a second time, with a different viral strain, are more likely to develop the severe form known as dengue hemorrhagic fever. Past work has mainly blamed another antibody type, IgG, for worsening infection. But IgE, better known for causing hay fever and asthma attacks, can also make blood vessels leaky by activating cells called mast cells and basophils. The team set out to see whether dengue-specific IgE appears in real patients, whether its levels track with how sick they get, and whether this IgE can actually switch on basophils in a way that might harm the body.
Tracking a risky antibody during illness
The researchers followed 98 adults hospitalized with dengue in Thailand, splitting them into two groups: those with standard dengue fever and those with the more dangerous dengue hemorrhagic fever. They collected blood at three key times: during the early fever, on the day the fever broke (called defervescence, when patients often enter the critical phase), and two weeks later during recovery. Using a specially developed lab test, they measured IgE that specifically recognized all four dengue virus types, alongside total IgE levels and substances released by mast cells.
IgE spikes when patients reach the danger zone
Across both mild and severe cases, dengue-specific IgE rose over time, peaking on the day the fever ended and then falling during recovery. This peak matched the moment when patients are at highest risk for sudden fluid leakage and shock. Crucially, people with dengue hemorrhagic fever had higher levels of dengue-specific IgE at this point than those with milder illness, even though their overall IgE levels were similar. This suggests that it is not simply being an “allergic person” that matters, but rather having antibodies that specifically recognize dengue. However, blood levels of mast-cell enzymes, which can mark cell activation, did not differ between the two groups in this adult cohort, perhaps because these signals fade quickly from the bloodstream.
How dengue-specific IgE switches on immune cells
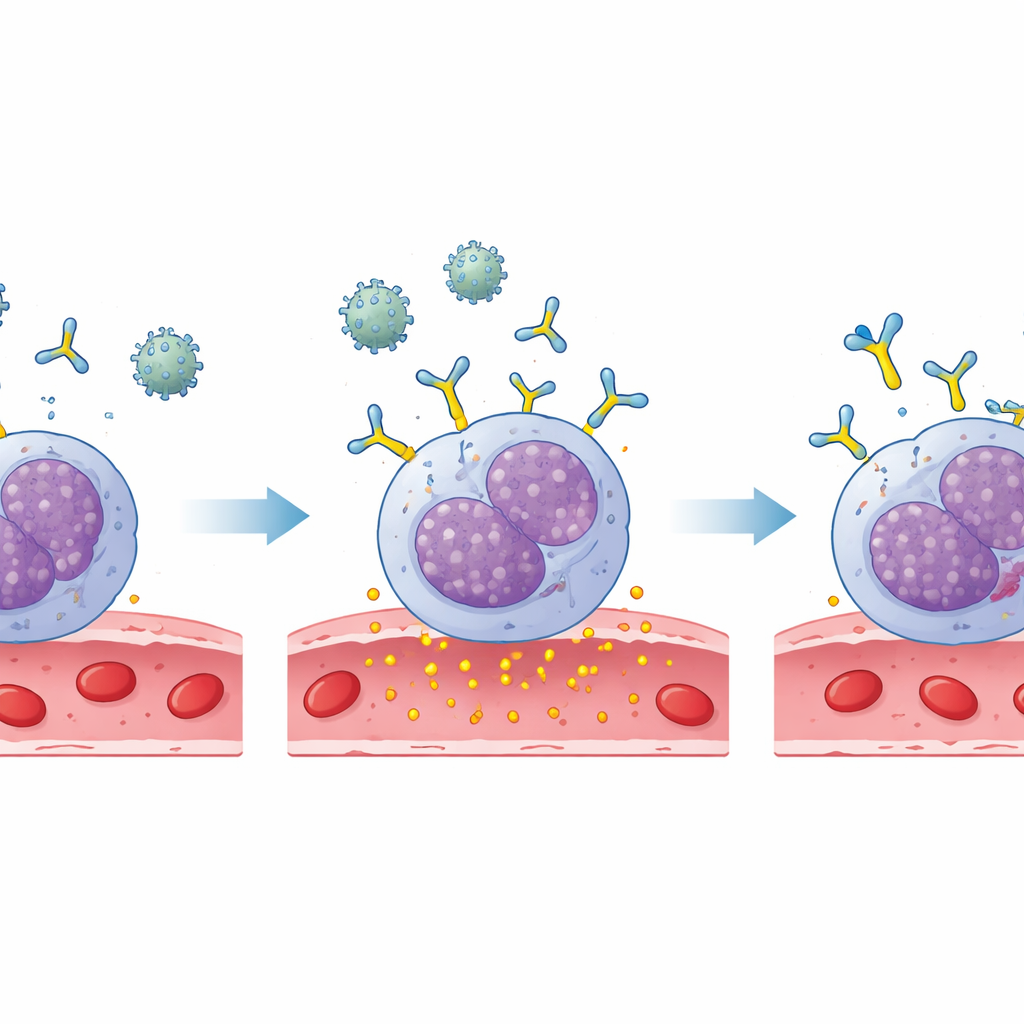
To test what this antibody actually does, the team used a laboratory basophil cell line engineered to respond when IgE on its surface is cross-linked by matching virus. They first “primed” these cells with patient plasma containing dengue-specific IgE and then exposed them to dengue virus. About one third of IgE-positive samples triggered strong cell activation, while IgE-negative samples were much less effective. This showed that, at least in the dish, dengue-specific IgE can arm basophils so that contact with the virus makes them release powerful chemical signals that could increase blood vessel leakiness in the body.
Blocking the signal with an allergy drug
The scientists then asked whether they could interrupt this activation using omalizumab, a drug already approved for severe allergic asthma. Omalizumab binds to IgE in a way that prevents it from docking on its receptors. When patient plasma was pre-treated with this drug before being added to the basophil cells, the dengue-triggered activation almost completely disappeared in most cases. Importantly, the drug had little effect when dengue-specific IgE was absent, reinforcing that it acts on this particular pathway.
What this could mean for patients
Taken together, the findings support a model in which dengue-specific IgE helps drive severe disease by priming basophils (and likely related cells) to overreact when they encounter the virus around the time the fever breaks, promoting leaky blood vessels. Not everyone with this antibody becomes severely ill, and the study was done mainly in adults without the very worst form of dengue, so more work is needed in larger and more diverse groups. Still, the work highlights dengue-specific IgE as both a warning sign of possible severe disease and a potential treatment target. Because omalizumab is already in clinical use for allergies, carefully designed trials could test whether, in a subset of high-risk patients identified at the right time point, temporarily blocking IgE might help keep dengue from tipping into its most dangerous phase.
Citation: Chan-in, W., Vacharathit, V., Tancharoen, W. et al. Anti-DENV IgE correlates with dengue severity and triggers FcεRI-dependent basophil activation inhibited by Omalizumab. Sci Rep 16, 14219 (2026). https://doi.org/10.1038/s41598-026-43199-z
Keywords: dengue severity, IgE antibodies, basophil activation, vascular leakage, omalizumab