Clear Sky Science · en
Automated measurement of hallux valgus angles using a deep learning model: validation and comparison with surgeons of varying expertise
Why bunion care is ready for smart automation
Bunions—those painful bumps at the base of the big toe—are extremely common, and deciding how best to treat them often hinges on carefully measuring angles on foot X‑rays. Today these measurements are done by hand, taking several minutes per image and varying from doctor to doctor. This study explores whether a modern form of artificial intelligence can take over this tedious task, delivering surgeon‑level accuracy in a fraction of a second and paving the way for more consistent, accessible bunion care.
Understanding the problem in everyday terms
Hallux valgus, better known as a bunion, occurs when the big toe drifts outward and the first long bone in the foot drifts inward, creating a bony bump and often pain. Surgeons rely on two angles measured on weight‑bearing X‑rays—the hallux valgus angle between the big toe and its long bone, and the intermetatarsal angle between the first and second long bones—to decide whether surgery is needed and which procedure to choose. Drawing these angles by hand is slow, and even specialists can disagree with each other or with their own prior readings, especially in mild or borderline cases. A tool that can measure these angles quickly and consistently would be valuable in busy clinics and large research studies alike.
How the computer learns to read a foot X‑ray
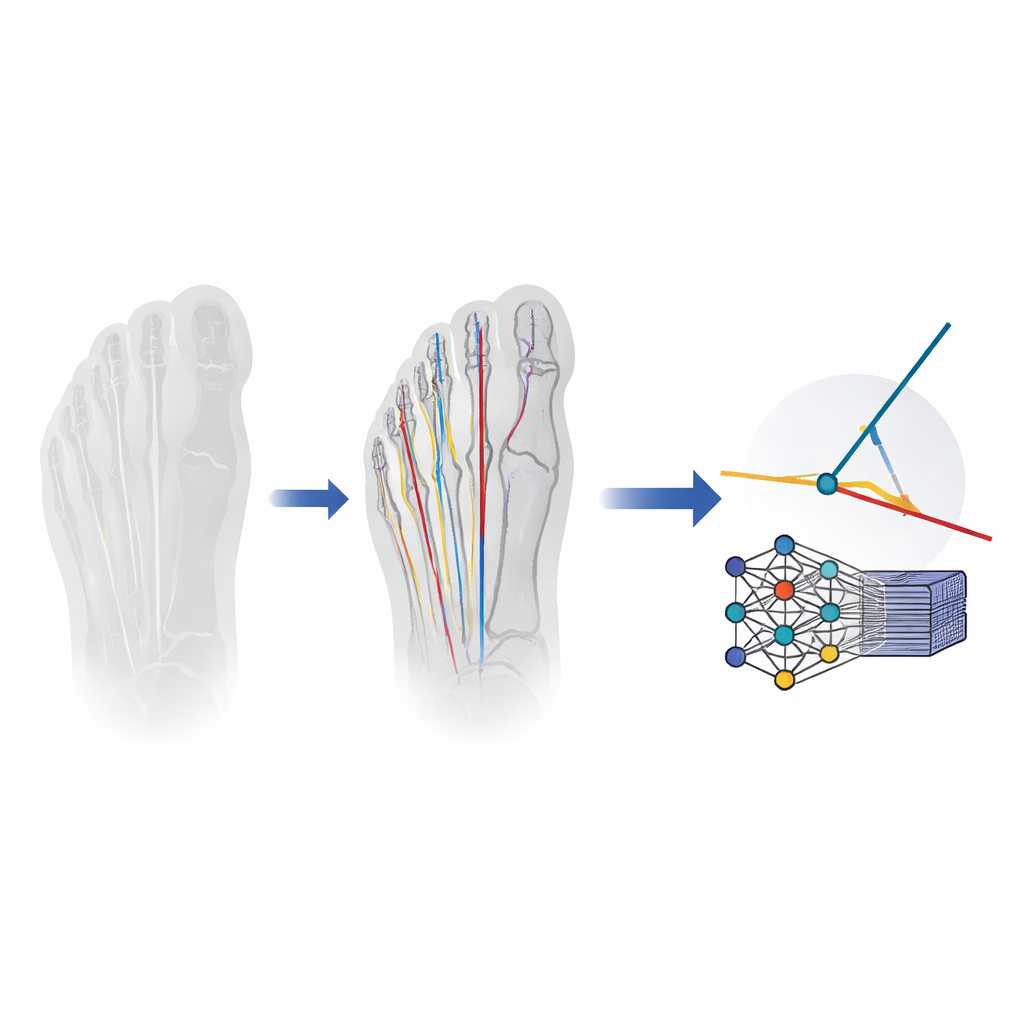
The research team built a deep learning system designed to mimic how an expert traces bone lines on an X‑ray. First, a specialized image‑analysis network automatically outlines three key bones: the big toe bone and the first and second metatarsals. From these outlines, the system calculates a straight central line through each bone, much as a surgeon would visualize when placing a ruler on the image. Once these lines are in place, simple geometry is used to compute the two angles important for bunion assessment. The model was trained and tuned on more than 2,400 standing foot X‑rays, including both patients with bunions and people with normal‑looking feet, ensuring it encountered the full range of shapes seen in everyday practice.
Putting the system head‑to‑head with surgeons
To test how well the automated measurements matched expert judgment, the authors compared the model with two foot and ankle surgeons who had three and seven years of experience, respectively. Both surgeons painstakingly marked bone lines on hundreds of X‑rays, and a senior surgeon reviewed their work to create a reference standard. The study assessed not only how closely each method matched this reference, but also how often measurements strayed far enough to be considered clinically unacceptable. The computer performed as well as the surgeons for the big‑toe angle and actually produced fewer large errors than either surgeon for the angle between the first two metatarsals, especially in normal or borderline feet where human readers tended to disagree more.
Speed, consistency, and what happens when it fails
Beyond accuracy, the most striking advantage of the automated system was speed: it measured each X‑ray in about one eighth of a second on an ordinary computer, compared with nearly two to three minutes of careful work by a human reader. This efficiency opens the door to instant, standardized measurements directly within hospital imaging systems or even on portable devices. The authors also examined cases where the model went wrong, such as low‑quality images where overlapping bones misled the software into tracing the wrong line. They suggest that future versions could be trained on more challenging X‑rays and equipped with simple internal checks to flag doubtful results for human review instead of silently reporting a flawed angle.
What this means for people with bunions
In everyday language, this study shows that a carefully trained computer program can measure bunion‑related angles on foot X‑rays about as accurately as experienced surgeons and far faster, while keeping serious mistakes relatively rare. Because the model is lightweight and publicly released, other hospitals and researchers can test it, refine it, and potentially integrate it into routine care. If future multi‑center studies confirm these results, patients could benefit from more objective, reproducible assessments of their bunions, leading to clearer surgical decisions and more consistent follow‑up over time.
Citation: Wang, Q., Wang, JH., Ji, DD. et al. Automated measurement of hallux valgus angles using a deep learning model: validation and comparison with surgeons of varying expertise. Sci Rep 16, 12280 (2026). https://doi.org/10.1038/s41598-026-42100-2
Keywords: hallux valgus, bunion surgery, foot radiograph, deep learning, medical image analysis