Clear Sky Science · en
Prediction of acute kidney injury in patients with acute pesticide poisoning using the PKIP score
Why kidney damage matters after poison exposure
When someone swallows a toxic amount of pesticide, doctors focus first on keeping the person alive. But hidden damage to the kidneys can quietly develop over hours to days and sharply raise the risk of death. This study asks a practical question that matters to patients and families: can we use information from the first two hours in the emergency room to spot who is most likely to develop serious kidney problems and might need closer watching or earlier treatment?
How the body and poisons strain the kidneys
The kidneys act as powerful filters that remove waste and many chemicals from the blood. In acute pesticide poisoning, this filter system can be overwhelmed. Toxins, low blood pressure, and other organ stress can combine to cause acute kidney injury, a sudden drop in kidney function. Earlier work showed that such injury is tied to longer hospital stays and higher chances of death, but doctors lacked clear, poisoning specific rules to detect it and tools to predict who would be hit hardest.
Standard rules tested in real patients
To tackle this gap, researchers examined records from 877 adults treated for non-paraquat pesticide poisoning at a Korean hospital between 2015 and 2020. They applied widely used Kidney Disease: Improving Global Outcomes (KDIGO) rules, which define and grade acute kidney injury based on changes in blood creatinine, urine output, and the need for dialysis. Using measurements taken after arrival, they tracked kidney status for one week. Patients who developed kidney injury by these criteria had a death rate of 16.6 percent, compared with 4.7 percent in those whose kidneys stayed stable. Worse stages of kidney injury were linked stepwise to higher mortality, suggesting that the KDIGO definition is meaningful in this poisoning setting. 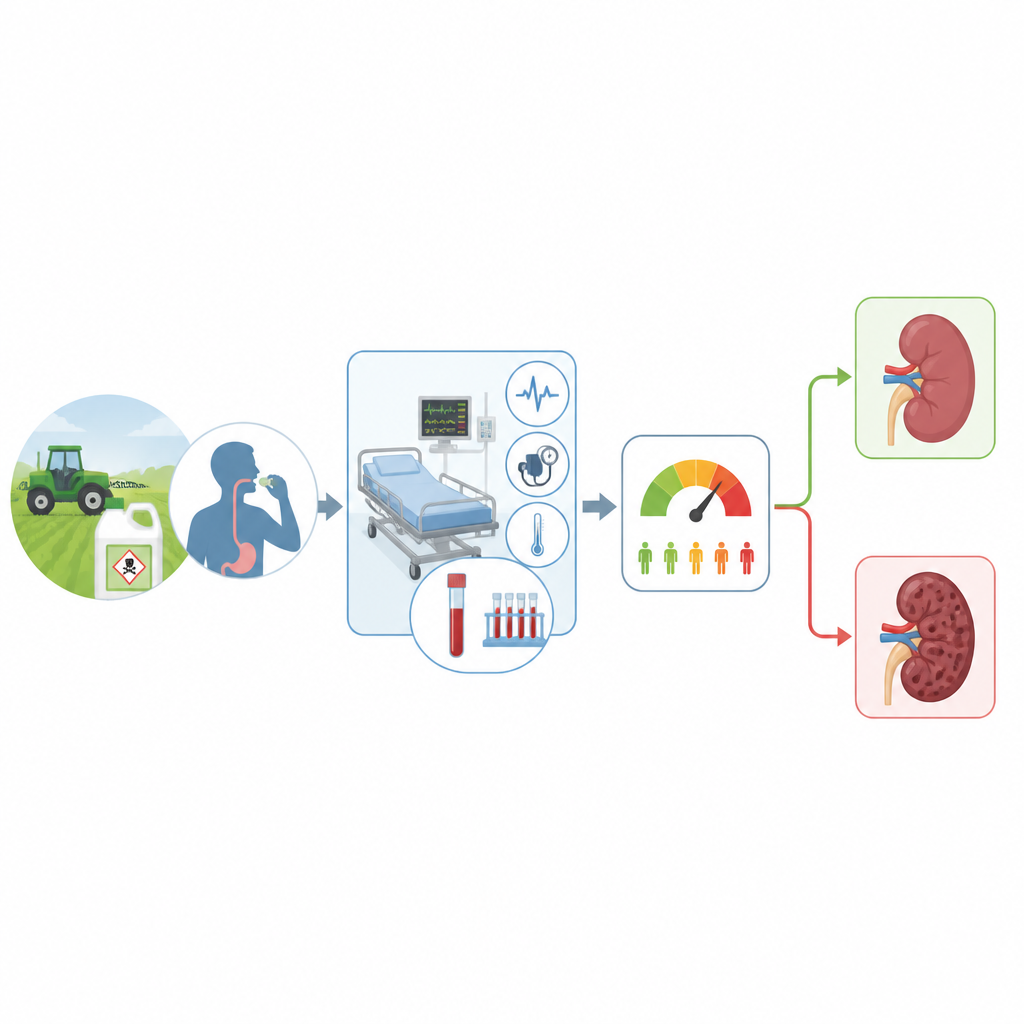
Building a simple early warning score
The team then set out to build an early warning model, called Prediction of acute Kidney Injury in Pesticide intoxication, or PKIP. They focused on information available within the first two hours in the emergency room: age, body size, body temperature, blood pressure and pulse, level of consciousness, blood tests such as white blood cell count, hemoglobin, creatinine, bicarbonate, phosphate, liver enzyme levels, as well as whether the patient had low blood oxygen or chronic kidney disease. They also included the broad type of pesticide and early urine findings like blood in the urine. Using modern machine learning techniques, they compared several algorithms and feature selection strategies, ultimately choosing a CatBoost model trained on 14 of the most informative features. 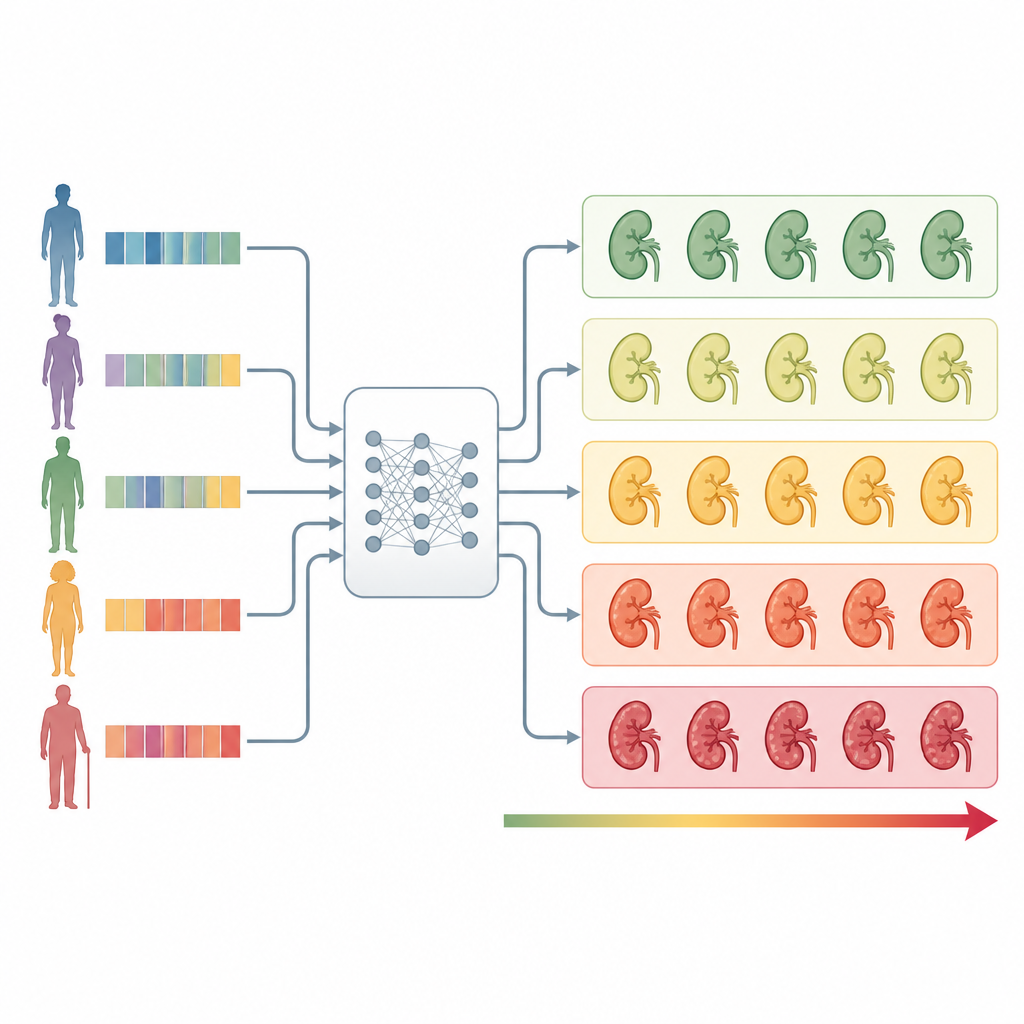
How well the PKIP score separates risk
PKIP’s predictions showed moderate accuracy at telling who would develop kidney injury, with a receiver operating characteristic area of 0.72, a common measure of discrimination. Importantly, when patients were grouped into five risk bands from minimal to severe based on PKIP’s output, outcomes diverged sharply. Only about 5 percent of those in the minimal risk group developed kidney injury, compared with about 61 percent in the severe risk group. Severe risk patients were not only more likely to suffer kidney damage, but also more likely to progress to the worst stage and to die; their mortality reached roughly 30 percent, while no deaths occurred in the minimal risk group. PKIP also outperformed a general intensive care score, APACHE II, in separating these risk levels, despite using fewer, routinely collected variables.
What this means for patients and care teams
For people with acute pesticide poisoning, this work suggests that standard kidney injury rules can identify those at higher risk of dying, and that an early, web based PKIP tool may help flag vulnerable patients long before full blown kidney failure appears. In practice, a high PKIP score could prompt doctors to monitor urine and blood tests more closely, avoid drugs that strain the kidneys, fine tune fluid therapy, and call kidney specialists sooner. The authors stress that PKIP is not perfect, was developed in a single hospital, and needs testing in other countries and with different pesticide use patterns. Still, it offers a concrete step toward more tailored care, turning the first two hours in the emergency room into a chance to prevent some of the most dangerous consequences of poisoning.
Citation: Kim, Y., Ahn, SJ., Cho, NJ. et al. Prediction of acute kidney injury in patients with acute pesticide poisoning using the PKIP score. Sci Rep 16, 15086 (2026). https://doi.org/10.1038/s41598-026-41334-4
Keywords: acute kidney injury, pesticide poisoning, risk prediction, clinical decision support, machine learning