Clear Sky Science · en
Menstrual blood-derived mesenchymal stromal cell extracellular vesicles stimulate chondrocytes and cartilage extracellular matrix synthesis in vitro
New Clues for Protecting Aching Joints
Many people, especially older women, live with the pain and stiffness of worn-out joints. This study explores an unexpected ally in the fight against joint damage: tiny healing particles taken from menstrual blood. By testing these particles on human cartilage cells and tissue in the lab, the researchers asked whether they could help joints repair themselves without relying on whole-cell transplants.
Tiny Messengers from an Unlikely Source
Instead of using living stem cells, the team focused on the microscopic packages those cells release, called extracellular vesicles. These vesicles are like molecular care packages, filled with proteins and genetic material that can change how nearby cells behave. The researchers collected menstrual blood from healthy donors, isolated the stem-like cells it contains, and then purified the vesicles those cells produced. This approach is attractive because menstrual blood can be collected repeatedly, non‑invasively, and without the ethical issues that sometimes surround other tissue sources.
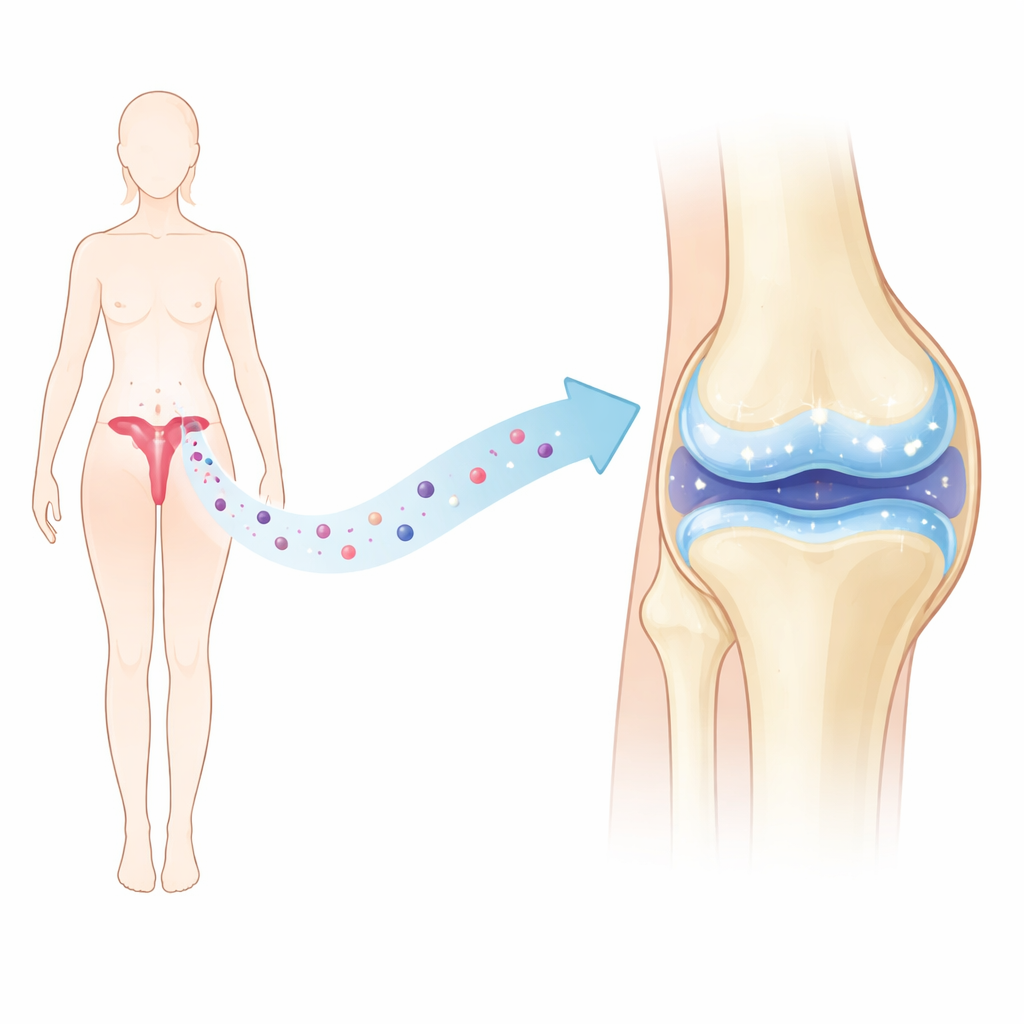
Talking to Cartilage Cells
The first step was to see whether cartilage cells, known as chondrocytes, would take up these menstrual vesicles and how they would respond. In dishes, the chondrocytes quickly absorbed the vesicles within a few hours. The vesicles did not change how fast the cells moved or divided, which suggests they were not overstimulating or harming them. However, the vesicles did boost the cells’ sensitivity to progesterone by increasing the amount of its receptor, a finding that may be especially relevant for understanding joint health in women after menopause, when hormone levels shift.
Building Up the Joint Cushion
Next, the researchers examined whether the vesicles could encourage chondrocytes to build more of the tough, slippery material that cushions joints, called the cartilage matrix. In three‑dimensional cell clusters grown under conditions that promote cartilage formation, the vesicles enhanced the production of collagen type II and other hallmark matrix components, particularly when combined with a known growth factor. Staining techniques and gene‑activity tests both showed stronger signals for cartilage-building molecules, indicating that the vesicles nudged cells toward a more youthful, matrix‑producing state.
Protecting Cartilage Under Stress
To move closer to real‑world joint damage, the team tested small pieces of cartilage taken from older women with advanced osteoarthritis. These tissue samples were exposed either to a damaging inflammatory signal or to a pro‑healing growth factor, with or without vesicle treatment. The vesicles reduced the leakage of matrix fragments into the culture fluid—a sign that less cartilage was breaking down—and helped preserve key components like collagen II and aggrecan inside the tissue. Advanced infrared measurements confirmed that vesicle‑treated samples contained more protein and sugar-rich material typical of healthy cartilage. Importantly, across a broad panel of immune signals, the vesicles did not trigger a major inflammatory reaction, suggesting a favorable safety profile in this setting.
Why This Matters for Future Therapies
Overall, the study shows that tiny vesicles derived from menstrual blood stem-like cells can help cartilage cells make more of the protective joint cushion and can limit tissue breakdown, even under inflammatory stress, at least in the lab. Because they are cell‑free, these vesicles sidestep some of the safety and logistical concerns of transplanting whole cells, while taking advantage of a renewable and non‑invasive source. If future animal and clinical studies confirm these benefits, such vesicles could one day be injected into damaged joints to slow or prevent osteoarthritis, offering a new, women‑centered avenue for joint repair.
Citation: Kugaudaite, G., Bakutyte, I., Bagdonas, E. et al. Menstrual blood-derived mesenchymal stromal cell extracellular vesicles stimulate chondrocytes and cartilage extracellular matrix synthesis in vitro. Sci Rep 16, 11059 (2026). https://doi.org/10.1038/s41598-026-40854-3
Keywords: osteoarthritis, cartilage repair, extracellular vesicles, menstrual blood stem cells, regenerative medicine