Clear Sky Science · en
Melanoma cell inoculation improves cognitive impairment in the 5xFAD mouse model of Alzheimer’s disease
When Cancer Cells Seem to Help the Brain
Alzheimer’s disease and cancer are two of the most feared illnesses of aging, yet population studies have uncovered a curious pattern: people with cancer often seem less likely to develop Alzheimer’s, and those with Alzheimer’s may be somewhat protected against cancer. This paper digs into that mystery using mice that develop Alzheimer-like brain changes, asking a bold question: could exposure to tumor cells unexpectedly soften memory problems by tweaking the body’s immune system?
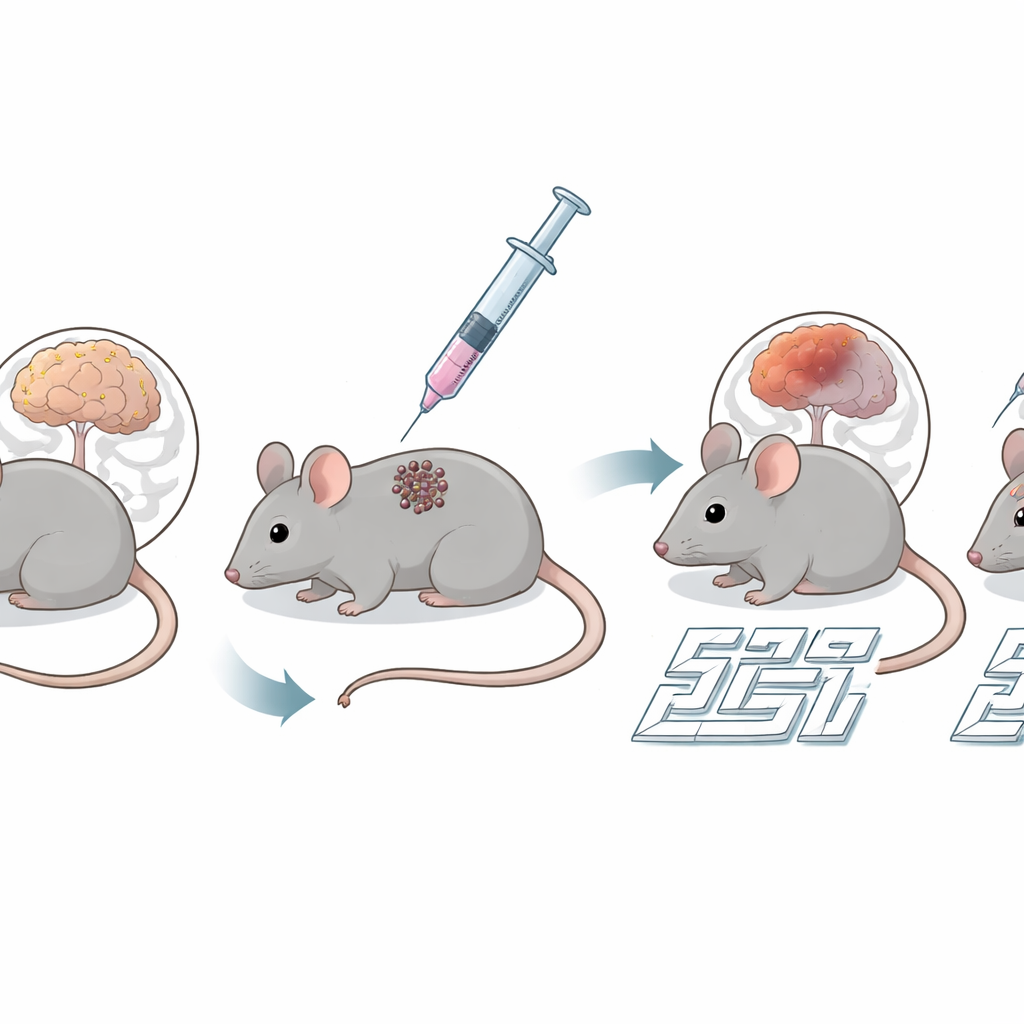
Testing an Unusual Connection
The researchers worked with 5xFAD mice, a widely used model that rapidly develops amyloid plaques and memory loss resembling key features of Alzheimer’s disease. At five months of age, these mice and their healthy littermates received a small injection of melanoma cells under the skin, or a harmless salt solution. Over the next month, the team watched how tumors grew and put the animals through two standard tests of spatial memory: a simple Y-shaped maze and a more demanding “Oasis” maze, where mice must learn and remember the location of a water reward on a platform with many possible wells.
Memory Gains Without Clearing Plaques
Alzheimer-model mice that received only the salt solution behaved as expected: they struggled to recognize the new arm of the Y maze and took long, wandering paths to find the hidden water in the Oasis maze. In striking contrast, Alzheimer-model mice that had been inoculated with melanoma cells performed far better. They again preferred the new arm in the Y maze and navigated the Oasis maze with more direct, efficient routes, reaching success rates similar to their healthy peers. These gains appeared mainly in short-term and working memory. Surprisingly, detailed staining of brain tissue showed that classic Alzheimer markers—amyloid-beta plaque burden in the cortex and hippocampus—did not decrease after melanoma inoculation. The number of star-shaped support cells (astrocytes) and resident immune cells (microglia) in the brain also remained largely unchanged.
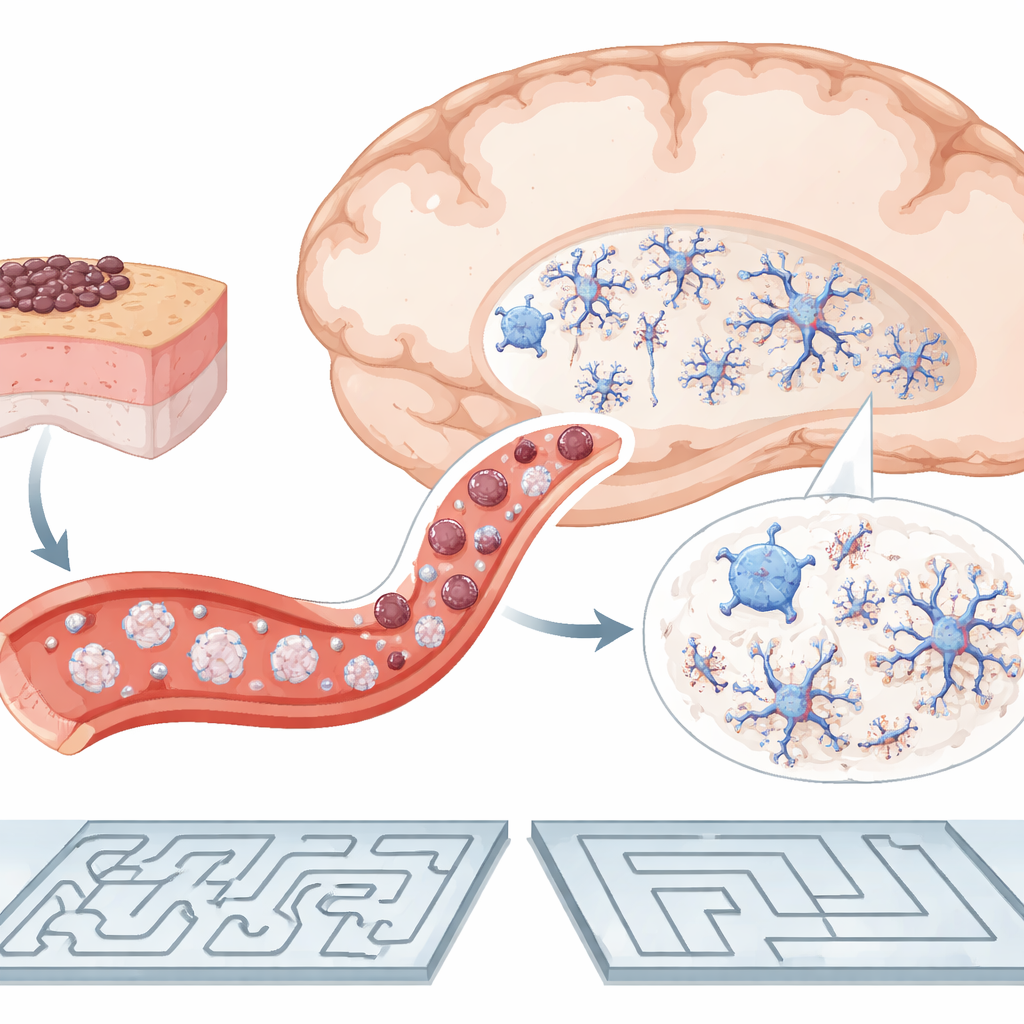
The Immune System Steps Into the Spotlight
Because the memory boost did not track with fewer plaques, the scientists turned to the immune system as a likely middleman. First, they noticed that fewer Alzheimer-model mice developed measurable tumors than healthy mice, and when tumors did grow, they tended to be smaller. That pattern echoes human data hinting that Alzheimer biology may resist cancer. Yet the cognitive benefit showed up regardless of whether a given mouse actually grew a tumor, suggesting that the critical signal comes early—possibly from the immune response to the melanoma cells themselves. In the spleen, a major immune organ, melanoma-inoculated Alzheimer-model mice showed an increased pool of myeloid cells, a family that includes many front-line defenders and tissue “clean-up” cells. Although blood levels of common inflammatory molecules did not change detectably, this shift hints that peripheral immunity was being re-tuned in a way that might influence the brain.
Quieter Brain Immune Cells Without Less Amyloid
To see how this outside-the-brain immune activity might echo inside the skull, the team examined microglia in the hippocampus, a key memory hub. In Alzheimer-model mice given only salt solution, microglia tended to have larger, more swollen cell bodies—a shape associated with a reactive, inflammatory state. After melanoma cell inoculation, those same microglia shrank back toward a leaner, more ramified form in all hippocampal subregions, consistent with a less aggressive posture. This happened even though the total number of microglia stayed the same and amyloid plaques did not budge. The researchers also measured CXCL10, a chemokine that helps call immune cells into the brain and has been linked to worse cognition in people with Alzheimer’s. As expected, CXCL10 gene activity was higher in Alzheimer-model mice than in healthy controls, but the melanoma challenge did not clearly lower these levels, underscoring that the beneficial effect may hinge more on subtle reshaping of immune cell behavior than on broad changes in well-known inflammatory signals.
What This Could Mean for Future Treatments
Taken together, the findings suggest that a peripheral encounter with melanoma cells can partially rescue memory in an Alzheimer-like mouse model, not by erasing amyloid plaques but by nudging the immune system and calming brain microglia. The same manipulation also made the mice less prone to tumor growth, mirroring the two-way protection seen in human studies. While deliberately giving cancer cells to patients is not a treatment strategy, the work points toward a promising idea: carefully tuned immune interventions—perhaps vaccines, immune checkpoint drugs, or other ways of mimicking tumor-triggered immune shifts—might someday harness this cancer–Alzheimer’s link to prevent or slow memory decline.
Citation: Bruna-Jara, B., More, J., Lobos, P. et al. Melanoma cell inoculation improves cognitive impairment in the 5xFAD mouse model of Alzheimer’s disease. Sci Rep 16, 11263 (2026). https://doi.org/10.1038/s41598-026-40699-w
Keywords: Alzheimer’s disease, cancer–Alzheimer’s link, brain immunity, microglia, melanoma model