Clear Sky Science · en
Retarded DNA DSB repair kinetics and augmented radiation sensitivity in Wiskott Aldrich syndrome patients
Why tiny breaks in DNA matter
For people born with Wiskott–Aldrich syndrome, everyday infections and bruises can be life‑threatening. These patients already live with fragile immune systems and a higher chance of developing cancer. This study asks a crucial question for their care: when their DNA is damaged by medical radiation or certain drugs, can their cells repair that damage as quickly and cleanly as in other people? The answer turns out to be no, and that delay may help explain both their cancer risk and how doctors should adjust treatments.
A rare disease with hidden risks
Wiskott–Aldrich syndrome is a rare inherited condition that almost always affects boys. It causes low platelets (leading to bleeding and bruising), eczema, and serious immune weakness. The root problem is a faulty protein called WASp, found in blood‑forming cells. WASp helps organize the inner skeleton of cells and supports a range of immune functions. Over 440 different gene changes in WASp are known, and they vary from severe disruptions to milder alterations. Children with these mutations face a greatly increased risk of lymphoma and leukemia, suggesting that their DNA is more prone to damage or that damage is not repaired properly.
Watching DNA damage in real time
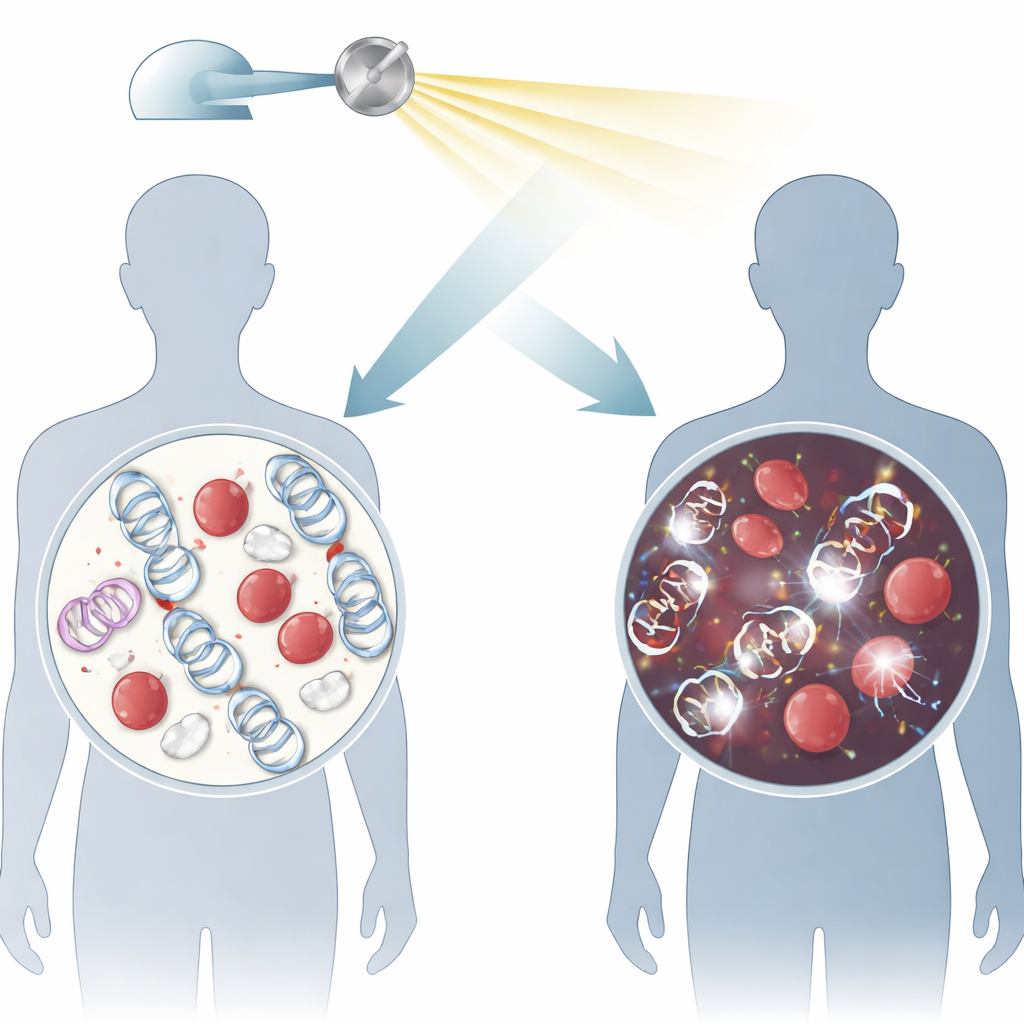
To see how well DNA damage is handled in Wiskott–Aldrich syndrome, the researchers collected blood from four boys with different WAS gene mutations, their unaffected mothers, and four healthy volunteers. They focused on one of the most dangerous kinds of DNA injury: double‑strand breaks, where both strands of the DNA helix snap. These breaks can be caused by ionizing radiation, such as medical gamma rays, and by some chemotherapy drugs. In the lab, they isolated white blood cells called lymphocytes and exposed them to a standard radiation dose similar to that used in clinical settings.
Instead of directly seeing the broken DNA, the team tracked two “flare” proteins, γH2AX and 53BP1, which rapidly gather at break sites and appear as bright dots, or foci, under a confocal microscope. By counting these foci over 24 hours and fitting the data with mathematical curves, they could measure how quickly breaks formed and were repaired, and how many were still present long after exposure. This approach allowed them to compare repair speed and efficiency across patients, mothers, and healthy controls.

More damage at rest, slower repair after radiation
Even before any radiation, lymphocytes from Wiskott–Aldrich patients showed 16 to 25 times more DNA‑damage foci than cells from healthy people, a clear sign of ongoing genomic instability. Their carrier mothers, however, looked essentially normal. After irradiation, all groups showed a rapid rise in foci within minutes, followed by a peak around one to two hours. Then the number of foci gradually declined as cells attempted repair. But in Wiskott–Aldrich lymphocytes, this decline was noticeably slower. On average, the time needed for half of the radiation‑induced foci to disappear was about 1.6 times longer than in healthy controls. Twenty‑four hours later, patients’ cells still held roughly twice as many residual foci as normal cells, indicating that many breaks remained unrepaired or were repaired only very slowly. The exact degree of delay differed between patients and appeared to track with how disruptive their specific mutations were.
Why mothers are spared
The mothers of affected boys carry one normal and one faulty copy of the WAS gene. In this study, their lymphocytes had baseline damage levels and repair speeds almost identical to those of unrelated healthy men. Both the buildup and the decay of γH2AX and 53BP1 foci followed the same patterns, and the estimated repair half‑lives were indistinguishable. This suggests that in these women, the normal copy of the gene is active enough in blood cells to provide full repair capacity, sparing them from the heightened radiation sensitivity seen in their sons.
What this means for care and treatment
For families and clinicians dealing with Wiskott–Aldrich syndrome, these findings have immediate implications. Children with this condition already commonly undergo bone marrow transplantation, often after whole‑body irradiation or other genotoxic conditioning. Knowing that their cells start out with more DNA damage and clear new breaks more slowly argues for careful tailoring of radiation‑based procedures and cancer therapies. The study provides the first detailed roadmap of how DNA double‑strand breaks are handled over time in Wiskott–Aldrich lymphocytes, reinforcing the idea that these patients are unusually radiosensitive. In practical terms, safer treatment may mean adjusting radiation doses, choosing less DNA‑damaging regimens where possible, and closely monitoring long‑term cancer risk.
Citation: Pathak, R.S., Chaurasia, R.K., Sapra, B.K. et al. Retarded DNA DSB repair kinetics and augmented radiation sensitivity in Wiskott Aldrich syndrome patients. Sci Rep 16, 13142 (2026). https://doi.org/10.1038/s41598-026-37262-y
Keywords: Wiskott–Aldrich syndrome, DNA repair, radiation sensitivity, genomic instability, bone marrow transplantation