Clear Sky Science · en
An open B-mode ultrasound database for deep learning-based atherosclerotic plaque segmentation
Why spotting hidden artery trouble matters
Heart attacks and strokes often strike without warning, but the danger builds up slowly, as fatty deposits called plaques narrow the arteries that feed the brain and heart. Doctors can see these plaques with ultrasound scans of the neck, yet carefully tracing their shape by hand on every image is time‑consuming and prone to human error. This article introduces an open, expertly labeled image collection that lets computers learn to find these plaques automatically, with the long‑term goal of making stroke and heart attack risk assessment faster, more consistent, and more widely available.
A closer look at artery build‑up
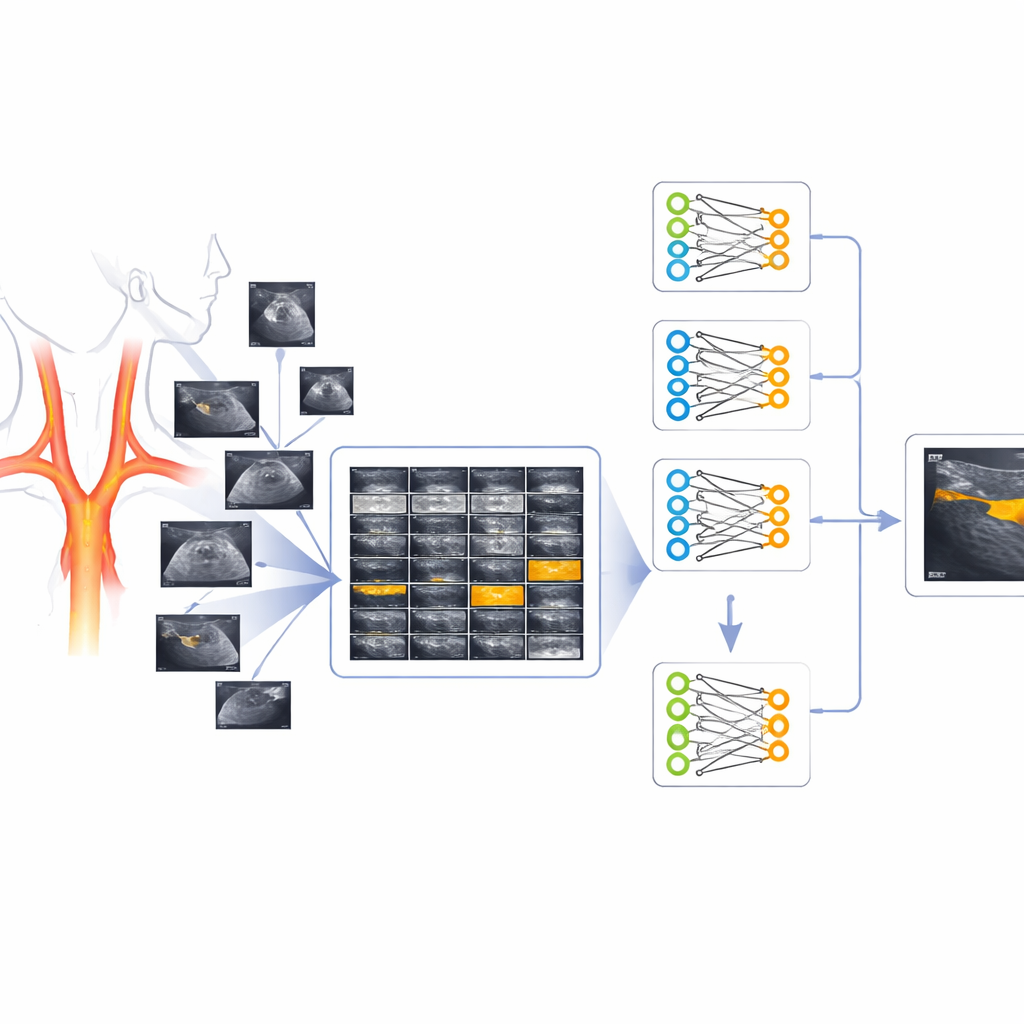
Atherosclerosis is the slow hardening and thickening of medium and large arteries as fats and inflammatory cells build up in the vessel wall. When this happens in the carotid arteries in the neck, it can reduce blood flow to the brain and increase the risk of stroke. One powerful way to estimate a person’s risk is to measure the total area covered by these plaques along the carotid artery. The catch is that before doctors or computers can measure plaque area, someone has to outline the plaque on each ultrasound image, a task that demands training, time, and consistency that are hard to sustain in busy clinics.
Why computers need better examples
Modern artificial intelligence, particularly deep learning, can learn to outline plaques automatically if it is shown enough examples where experts have already drawn the correct borders. Many past research projects have used such methods successfully, but often under idealized conditions: images carefully cropped around a single obvious plaque, with no examples of images that have no plaque at all or that contain several plaques at once. These private datasets are usually not shared, which makes it hard for other scientists to reproduce results or to know whether an algorithm would work in everyday, messy clinical reality.
Building a realistic image collection
To bridge this gap, the authors assembled and cleaned a database of 541 ultrasound images of the carotid arteries from a high‑risk group of patients in Argentina. For each image, specialists provided a matching “mask” image in which plaque regions were marked, creating a pair: the original black‑and‑white scan and a simple black‑and‑white outline of plaque. The team carefully removed visual clutter such as crosses, numbers, and device markings, standardized all images to a square format, and ensured that both images in each pair lined up perfectly. The final collection deliberately includes scans with no plaques, scans with single or multiple plaques, and plaques located away from the image center, better reflecting what doctors actually see.
Letting neural networks draw the outlines
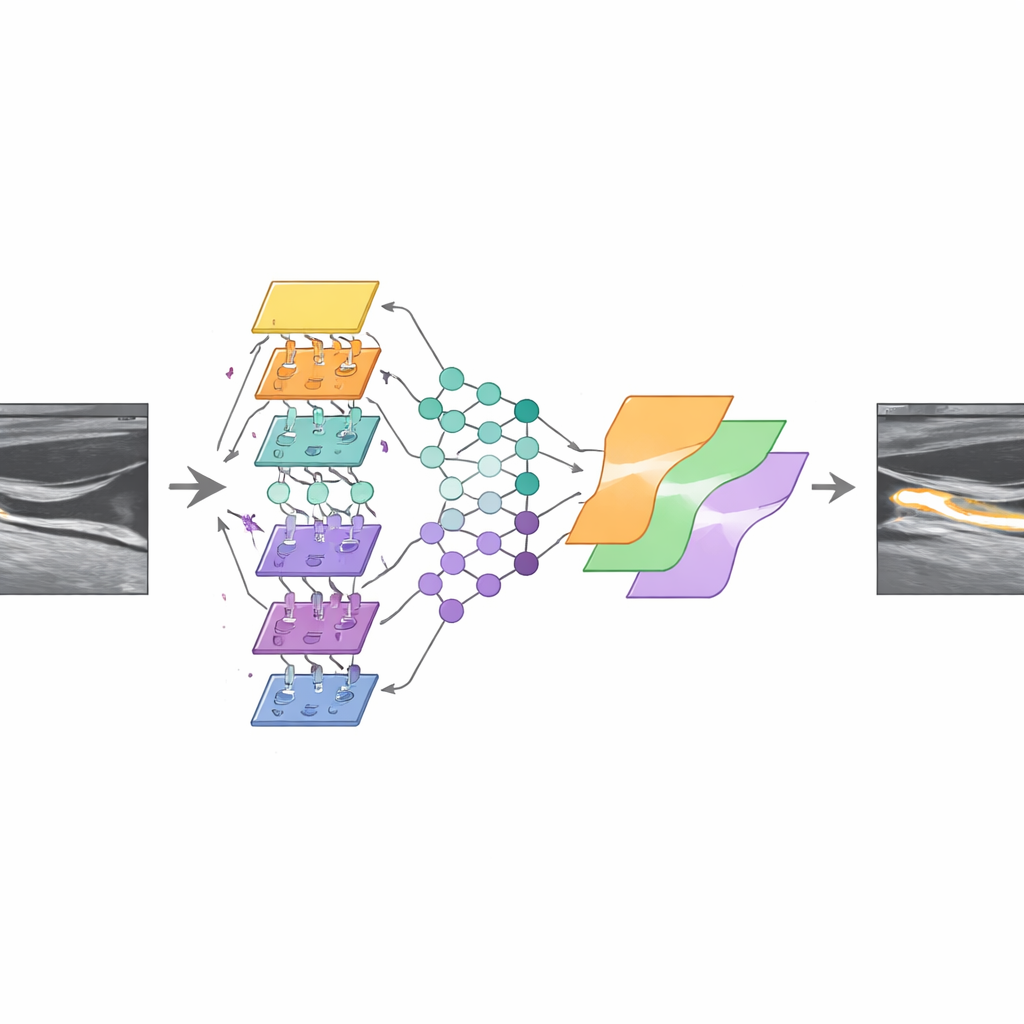
To test whether the database is truly useful for algorithm development, the researchers trained three versions of a popular image‑segmentation network known as U‑Net, each using a different backbone for detecting patterns. They expanded the training data by flipping and slightly shifting the images, then combined the three models into an “ensemble” that votes pixel by pixel on whether a spot belongs to plaque or not. On images that contained plaques, this ensemble reached a moderate level of overlap with expert tracings, similar to what different human specialists might achieve among themselves. On plaque‑free images, the combined system produced relatively few false alarms, suggesting that it learned not only what plaque looks like, but also when there is none.
What this means for future care
For non‑specialists, the key message is that this open database turns scattered, hard‑to‑access clinical images into a shared resource that anyone can use to train and test plaque‑finding algorithms. While the performance is not yet perfect and is influenced by the specific patient group and imaging equipment, the work shows that computers can approach expert‑level tracing even under more realistic and varied conditions. By making both the images and the evaluation code freely available, the study lays the groundwork for more robust tools that can help doctors quickly and consistently measure plaque burden, improving prevention strategies for heart attacks and strokes.
Citation: Rulloni, V.S., Perez, H.A., Dori, T. et al. An open B-mode ultrasound database for deep learning-based atherosclerotic plaque segmentation. Sci Data 13, 702 (2026). https://doi.org/10.1038/s41597-026-06952-7
Keywords: atherosclerosis, carotid ultrasound, medical imaging AI, plaque segmentation, cardiovascular risk