Clear Sky Science · en
AI-based triage and decision support in mammography and digital tomosynthesis for breast cancer screening: a paired, noninferiority trial
Why Smarter Screening Matters
Most women over 50 are invited for regular breast X-ray checks to catch cancer early. These screening programs save lives, but they also strain health systems and cause anxiety when scans trigger false alarms. This study asks a pressing question: can artificial intelligence (AI) safely take over part of the work of reading breast scans, so that radiologists focus only on the riskiest cases while still finding at least as many cancers?
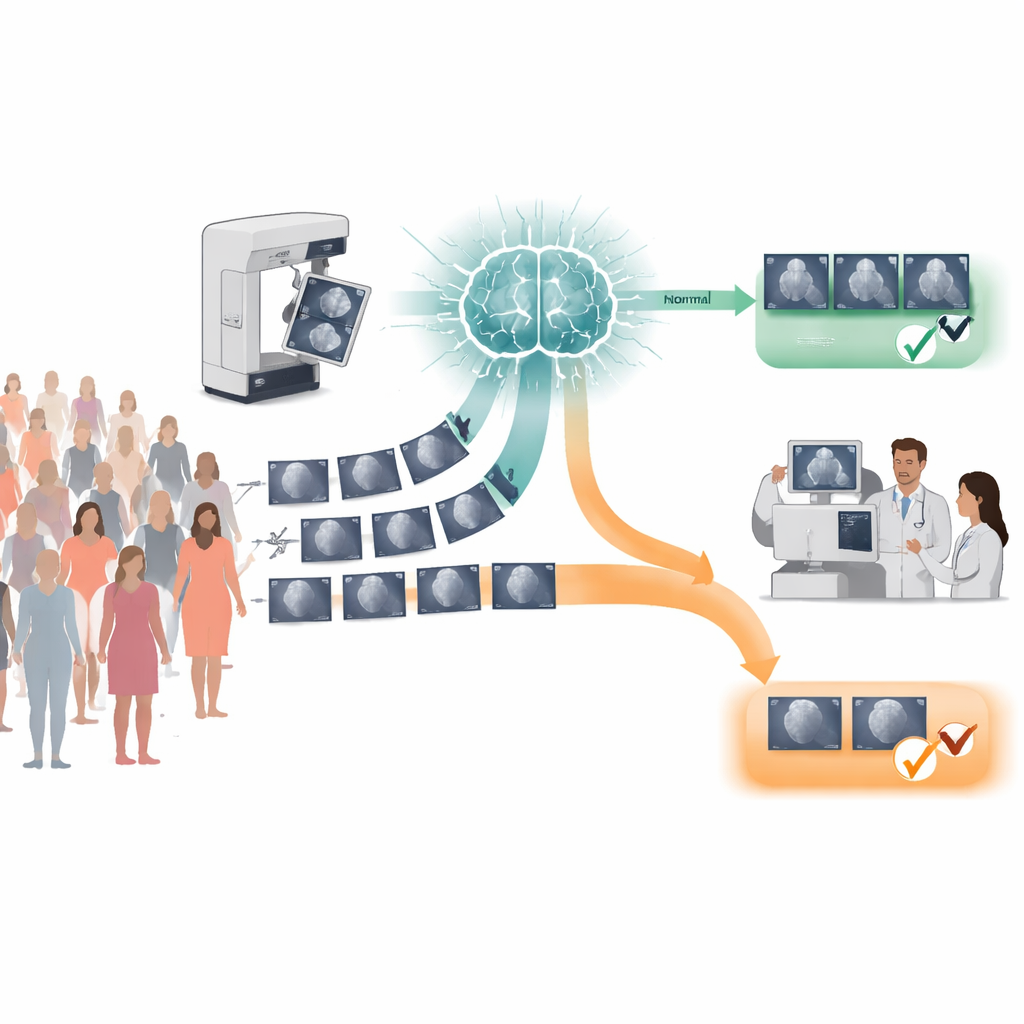
How Breast Scans Are Read Today
In many European programs, each mammogram is read independently by two radiologists. This "double reading" catches more cancers but also doubles the workload. Newer 3D-like scans, called tomosynthesis, add even more viewing time per exam. At the same time, populations are aging, some guidelines suggest starting screening earlier, and there are not enough trained radiologists in many regions. All of this makes it difficult to maintain or improve screening quality without overloading specialists.
What the Researchers Tested in Real Life
The team ran a large clinical trial in Córdoba, Spain, within an existing public screening program. Over 31,000 women aged 50 to 71 underwent either standard digital mammography or tomosynthesis. Each exam was processed in two parallel ways. First came the normal approach: two radiologists read every case without help from AI. In the second, experimental approach, an AI system analyzed the images and ranked each exam by its likelihood of containing cancer. Scans the AI labeled as low risk were automatically considered normal and never shown to a radiologist; only the higher‑risk exams were double read, this time with the AI’s visual marks and scores available as decision support.
What Happened to Workload and Cancer Detection
This AI triage strategy meant radiologists needed to read just over one‑third of all exams instead of every single one—a workload drop of nearly two‑thirds. Despite this dramatic reduction, the AI‑supported strategy actually found more cancers: about 7.3 cancers per 1,000 women screened compared with 6.3 per 1,000 using the standard method. The AI‑guided pathway picked up additional early, small, and lymph‑node‑negative tumors, the kinds of cancers where early treatment can be most beneficial. These gains were especially striking for traditional 2D mammography, where cancer detection rose more than 30 percent with AI support.
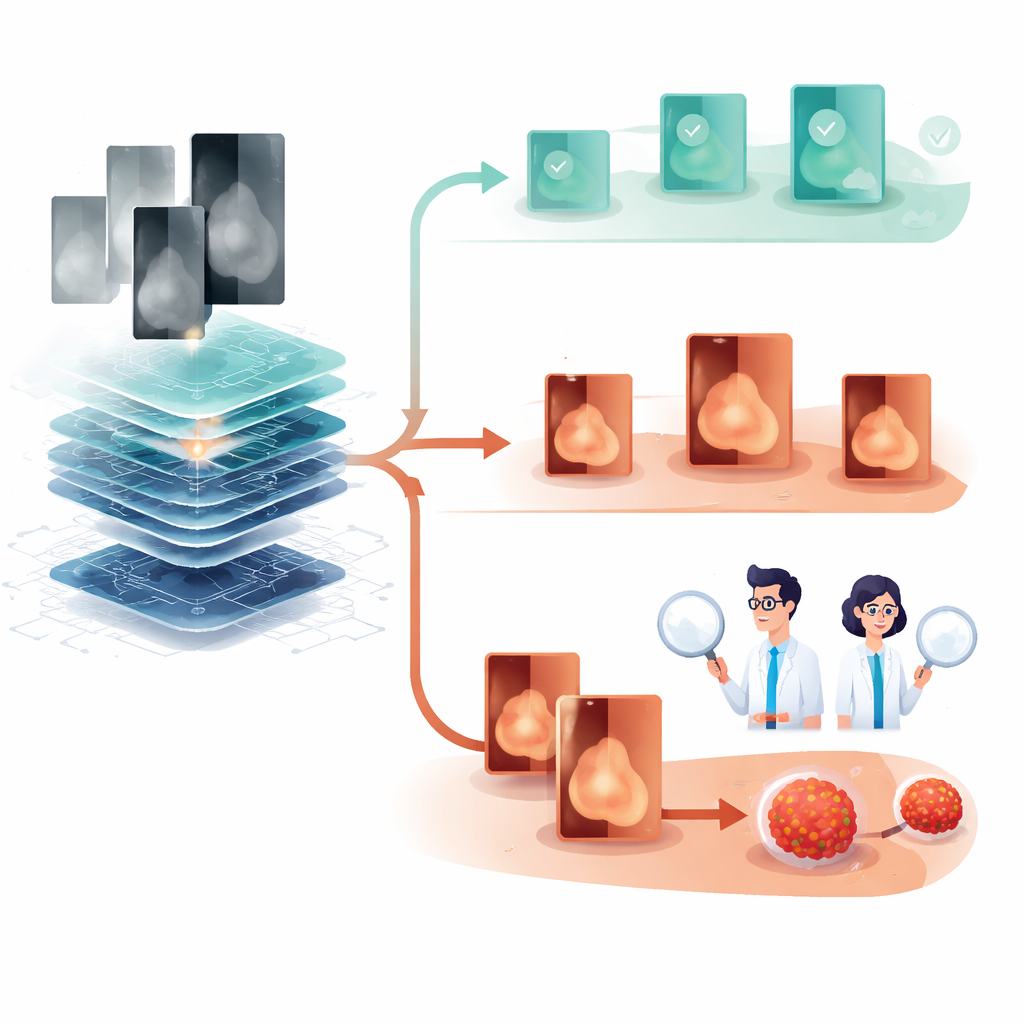
The Trade-Off: More Callbacks for Extra Checks
The price of this improvement was an increase in the number of women called back for extra testing. Overall, the recall rate rose from 4.8% with standard reading to 5.5% under the AI strategy, and the false positive rate was modestly higher. In other words, more cancers were found, but slightly more women experienced the stress of a suspicious result that ultimately turned out to be benign. For tomosynthesis, however, AI reduced workload without meaningfully changing how many women were recalled or how many cancers were found, reflecting already strong performance in that modality.
Safety, Missed Cancers and Ethical Questions
AI was not perfect: 11 cancers were given low‑risk scores and therefore would have been missed in a fully autonomous workflow. Yet the standard approach without AI missed even more cancers that the AI‑supported strategy caught. Most of the AI‑missed tumors had very subtle appearances, picked up by only one of the two radiologists in the traditional reading arm. The authors emphasize that wide adoption of AI‑only reading for many exams raises ethical and legal questions. They argue that extra safeguards—such as strict quality checks on image acquisition and continuous monitoring of AI performance—would be needed before relying on AI to label the majority of scans as normal without human review.
What This Means for Future Screening
To a lay reader, the bottom line is that carefully designed AI can help radiologists handle far more screening exams while finding at least as many, and in some cases more, early breast cancers. In this trial, letting AI automatically clear low‑risk mammograms cut radiologist workload by almost two‑thirds, maintained the accuracy of positive findings, and slightly improved overall cancer detection, although more women were asked to return for follow‑up. The study suggests that, with appropriate oversight and further validation, AI‑based triage and decision support could make large‑scale breast cancer screening both more sustainable for health systems and more effective at catching disease early.
Citation: Elías-Cabot, E., Romero-Martín, S., Raya-Povedano, J.L. et al. AI-based triage and decision support in mammography and digital tomosynthesis for breast cancer screening: a paired, noninferiority trial. Nat Med 32, 1296–1305 (2026). https://doi.org/10.1038/s41591-026-04277-x
Keywords: breast cancer screening, mammography, artificial intelligence, radiology workload, early cancer detection