Clear Sky Science · en
Pulsed field ablation versus conventional thermal ablation for paroxysmal atrial fibrillation: 4-year outcomes in the ADVENT-LTO study
Why this heart rhythm study matters
Atrial fibrillation is the most common sustained heart rhythm problem, and it can turn life into a cycle of racing pulses, hospital visits and worry about stroke. Many patients now undergo catheter ablation, a procedure in which doctors burn or freeze tiny areas inside the heart to stop faulty electrical signals. A newer method, called pulsed field ablation, instead uses brief electrical pulses to selectively disable heart tissue. This article reports four-year results from a large clinical study comparing these two strategies, giving patients and clinicians a clearer picture of how well the newer approach holds up over time.
Two different ways to quiet a chaotic heartbeat
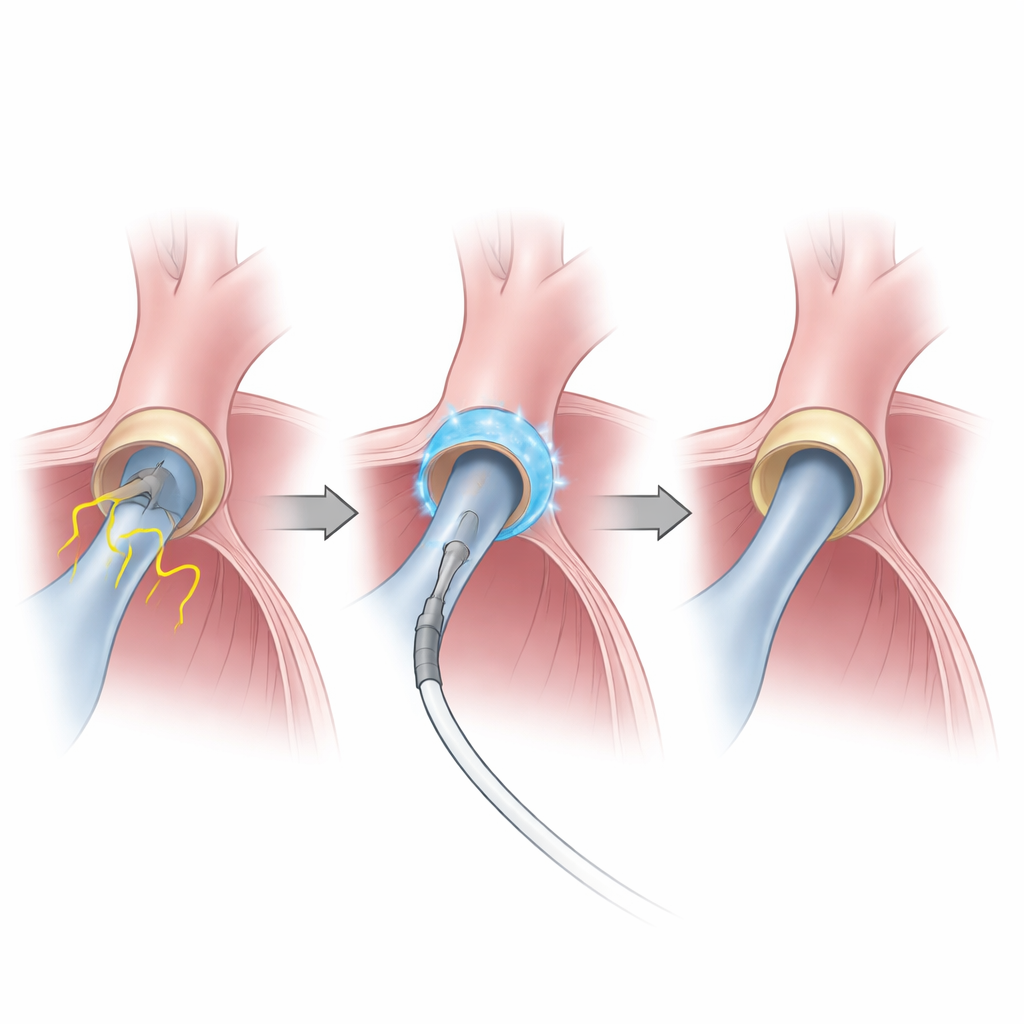
Traditional ablation techniques rely on heat or cold—radiofrequency energy or cryotherapy—to scar small regions of tissue around the veins that feed blood into the heart’s upper left chamber. These veins often act as trigger zones for atrial fibrillation. While effective, thermal methods do not distinguish well between target and nearby structures, so the esophagus, nerves or lung veins can sometimes be harmed. Pulsed field ablation takes a different path: it delivers ultra-short electrical pulses that punch microscopic holes in cell membranes, leading to cell death in heart muscle while largely sparing surrounding tissues. Earlier research suggested that pulsed field ablation is fast and safe, but most follow-up stopped at one year, leaving questions about durability and longer-term disease control.
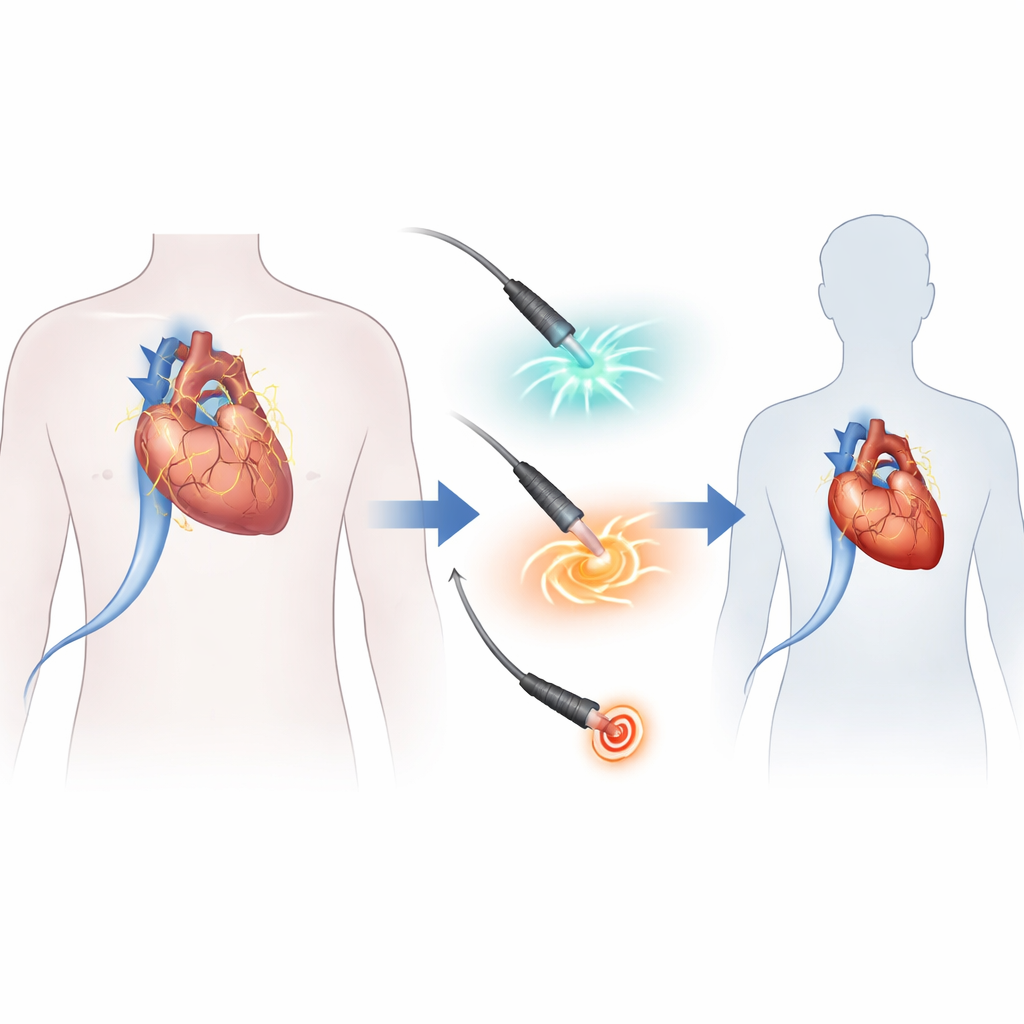
Following patients years after their procedures
The ADVENT-LTO study extended follow-up for 364 people who had originally taken part in a randomized trial comparing pulsed field ablation with conventional thermal ablation for paroxysmal atrial fibrillation, a form in which episodes start and stop on their own. All participants had already completed one year of monitoring and were contacted at least three years after their initial procedure. Roughly half had received pulsed field ablation and half radiofrequency or cryoballoon treatment. Researchers reviewed medical records, collected heart rhythm recordings from wearable monitors in most patients and asked participants to complete quality-of-life surveys, tracking whether abnormal rhythms returned, whether further hospital-based interventions were needed and whether the disease progressed to a more stubborn, persistent form.
How the two treatments stacked up over four years
By about four years after the procedure, both strategies performed well, but pulsed field ablation showed some numerical advantages. Roughly 73% of pulsed field patients and 64% of thermal ablation patients met the main success definition: no documented sustained abnormal atrial rhythms, no electrical shock to reset the heartbeat and no repeat ablation after the first three months. Most failures in both groups occurred within the first six months, after which the results leveled off. When the researchers used a stricter yardstick that also counted use of powerful rhythm-control drugs as a failure, success rates were about 68% for pulsed field and 60% for thermal ablation. Patients in the pulsed field group were about half as likely to need these medications during follow-up, and significantly fewer of them underwent a second ablation procedure.
Keeping atrial fibrillation from getting worse
One major concern with atrial fibrillation is its tendency to progress from occasional episodes to a constant or near-constant problem that is harder to treat. In this study, progression from paroxysmal to persistent atrial fibrillation was uncommon in both groups: only about 3% of pulsed field patients and 5% of thermal ablation patients developed persistent disease over four years, a difference that was not statistically meaningful. Measures of day-to-day well-being, including a questionnaire specific to atrial fibrillation and a general health survey, improved substantially after ablation and stayed better over time, with similar gains in both treatment arms. Serious events such as stroke or blood clots were rare, and there were no worrisome late complications uniquely tied to pulsed field ablation.
What this means for people living with irregular heartbeat
For patients and doctors weighing their options, these long-term findings suggest that pulsed field ablation can match, and may modestly outperform, established heat- and cold-based techniques in keeping atrial fibrillation at bay, while preserving the safety advantages seen in earlier studies. The procedure reduced the need for repeat ablations and strong rhythm drugs, and did not appear to accelerate progression to more serious disease. Although the study has limitations—it followed only those who agreed to reenroll and relied partly on chart reviews—the overall message is reassuring: the benefits of pulsed field ablation are not short-lived. As the technology becomes more widely available and additional trials report results, it is likely to play an increasingly prominent role in how cardiologists restore and maintain a steady heartbeat.
Citation: Reddy, V.Y., Gerstenfeld, E.P., Mountantonakis, S.E. et al. Pulsed field ablation versus conventional thermal ablation for paroxysmal atrial fibrillation: 4-year outcomes in the ADVENT-LTO study. Nat Med 32, 1444–1453 (2026). https://doi.org/10.1038/s41591-026-04246-4
Keywords: atrial fibrillation, catheter ablation, pulsed field ablation, heart rhythm, long-term outcomes