Clear Sky Science · en
Identification of racial disparities across MammaPrint and BluePrint subtypes in HR + HER2- breast cancer
Why this study matters
Breast cancer does not affect all communities in the same way, and Black women in the United States are more likely to die from the disease than White women, even when they have the most common type known as hormone receptor positive, HER2 negative breast cancer. This study asks whether hidden differences inside the tumor itself help explain some of that gap, and whether modern gene-based tests can guide care in ways that reduce these survival differences.
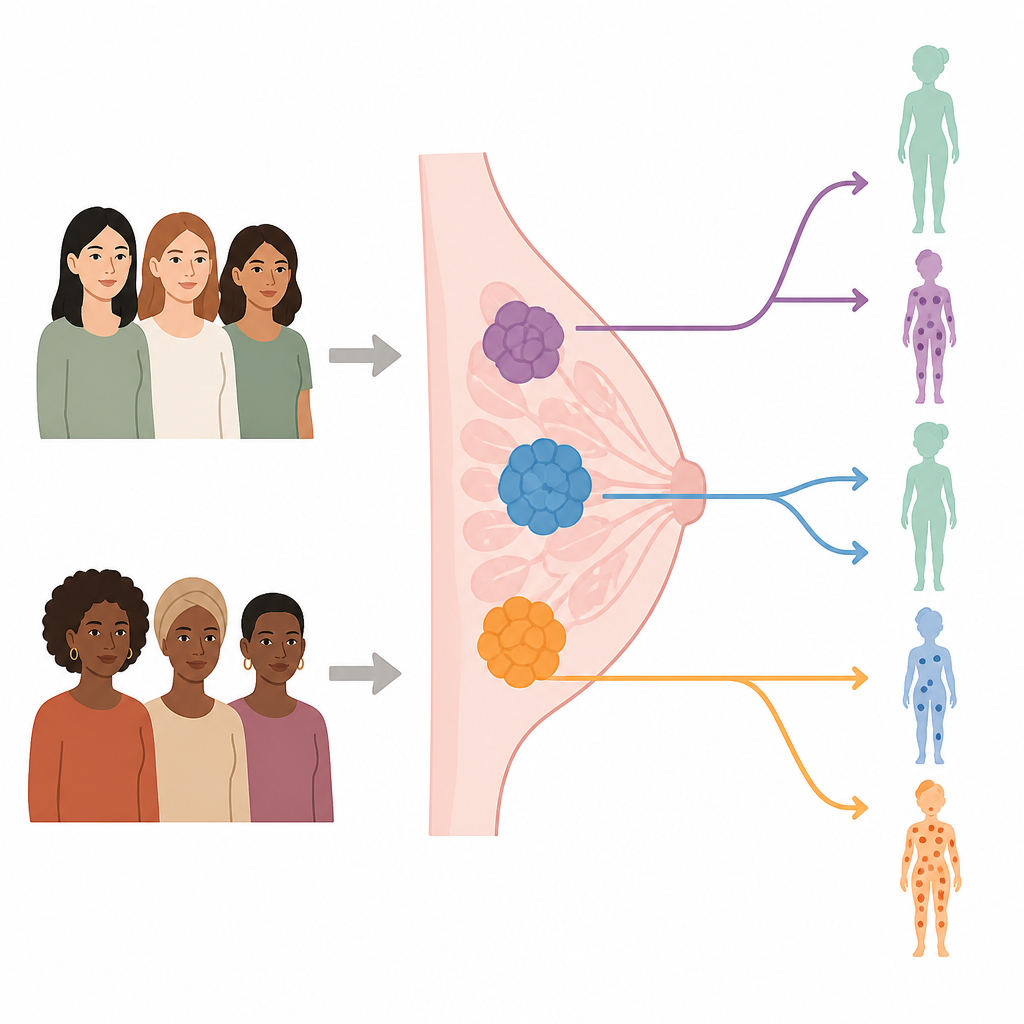
Looking inside the tumor
Doctors have long used a microscope to grade breast cancers and standard lab tests to see which hormones or growth signals they respond to. New genomic tests go further by reading patterns of activity across many genes at once. In this study, researchers used two such tests, MammaPrint and BluePrint, to classify tumors from more than one thousand women with early stage hormone receptor positive, HER2 negative breast cancer. About half of the participants self-identified as Black and half as White, and the groups were carefully matched by age and menopausal status so that differences in biology could be examined more fairly.
Different patterns by race
The gene tests sorted tumors into risk groups and subtypes. MammaPrint labeled cancers as low risk or high risk for coming back, and further split high risk tumors into two levels. BluePrint divided cancers into three broad molecular families known as Luminal A type, Luminal B type, and Basal type. The team found that Black women were less likely than White women to have the more favorable low risk Luminal A type tumors. Instead, Black women more often had high risk tumors, including Luminal B type and especially Basal type cancers, which are known to behave more like the aggressive triple negative form of breast cancer.
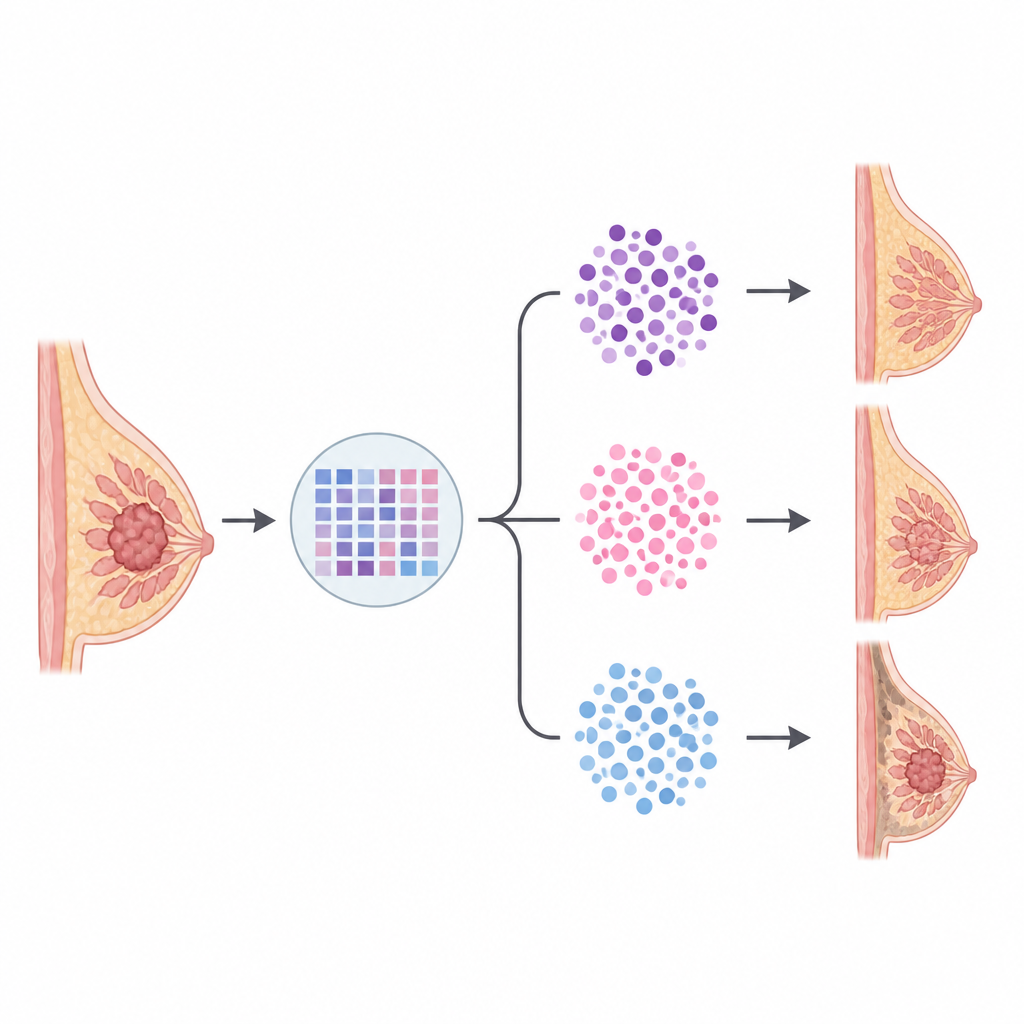
Survival linked to gene based subtype
Next, the researchers asked how these gene based groups related to the chance that cancer would return within three years. Overall, short term recurrence free survival was similar for Black and White women when race alone was considered. However, when tumors were grouped by genomic subtype, clear differences emerged. Women with Luminal A type tumors had the best three year outcomes, followed by those with Luminal B type tumors. Basal type tumors had the poorest results, with more women experiencing a return of their cancer within three years. Importantly, these patterns held true within each racial group: regardless of race, Basal and high risk Luminal B tumors carried more danger than Luminal A tumors.
Longer term outlook for Black women
For a subset of Black women followed for up to ten years, the same message appeared over a longer horizon. Those whose tumors were classified as low risk by MammaPrint or as Luminal A type by BluePrint had excellent long term outcomes, while women with high risk, Luminal B, or Basal type tumors were more likely to have recurrences or die from their disease. This suggests that gene based tests do more than simply label tumors; they help pinpoint which patients face higher danger over time and may need more intensive treatment and follow up.
What this means for patients
To a layperson, the key message is that the genes active inside a breast tumor matter at least as much as what can be seen under the microscope, and these gene patterns are not evenly distributed across racial groups. Black women in this study more often had the riskier genomic subtypes, yet within each subtype Black and White women had similar short term outcomes. This indicates that tumor biology, measured through genomic testing, helps drive survival differences, while race itself is not the direct cause. Broad access to reliable gene based tests like MammaPrint and BluePrint, along with equitable treatment based on those results, could therefore be a powerful tool to tailor therapy and narrow racial gaps in breast cancer survival.
Citation: Reid, S., Venton, L., Whisenant, J.G. et al. Identification of racial disparities across MammaPrint and BluePrint subtypes in HR + HER2- breast cancer. npj Breast Cancer 12, 68 (2026). https://doi.org/10.1038/s41523-026-00932-1
Keywords: breast cancer, genomic testing, racial disparities, MammaPrint, BluePrint