Clear Sky Science · en
Gut microbiome composition and function reflect socioeconomic deprivation
Why Your Neighborhood Might Shape Your Gut
Where you live does more than determine your commute and your view out the window. Growing evidence suggests that the stresses and resources of a neighborhood can reach deep inside the body, even reshaping the trillions of microbes that live in our gut. This study asks a striking question: can socioeconomic deprivation—living in a more disadvantaged area—change the gut microbiome in ways that help explain higher rates of anxiety and diabetes?
Linking Place, Microbes, and Health
The researchers analyzed data from 1,390 women in the UK twin registry, all living across neighborhoods that ranged from relatively affluent to highly deprived. Instead of looking only at income or education, they used a well-established area-level score of deprivation that captures factors such as unemployment, overcrowded housing, and lack of car ownership. Each participant provided a stool sample for deep genetic sequencing of gut microbes, answered mental health questionnaires, and had blood tests to assess diabetes and related conditions. This design let the team trace connections from neighborhood context to gut bacteria and on to anxiety and diabetes.
Fewer Microbial “Neighbors” in Deprived Areas
People living in more deprived neighborhoods tended to harbor less diverse gut microbiomes, meaning they had fewer distinct microbial types in their intestines. When the researchers compared the overall microbial communities of the most and least deprived groups, they found clear differences in composition, even after accounting for age, body weight, and family relatedness. These shifts were not fully explained by diet quality or recent antibiotic use, suggesting that other aspects of deprivation—such as chronic stress, environmental exposures, or limited access to green spaces—may be quietly sculpting the microbial ecosystem within.
Missing Helpful Microbes and Energy Pathways
Diving deeper, the team identified a handful of microbial species that were strongly linked to deprivation levels. Several beneficial bacteria that produce short-chain fatty acids, especially butyrate—a key fuel for gut cells and a player in mood and metabolism—were less common in the more deprived group. At the same time, certain other species were more abundant. When the researchers examined what the microbiome was capable of doing, not just which microbes were present, they saw that key energy-related pathways were less active in those from deprived neighborhoods. Microbial processes involved in breaking down fats and running core energy cycles were dampened, hinting that the gut ecosystem in these individuals may be less efficient at maintaining metabolic balance.
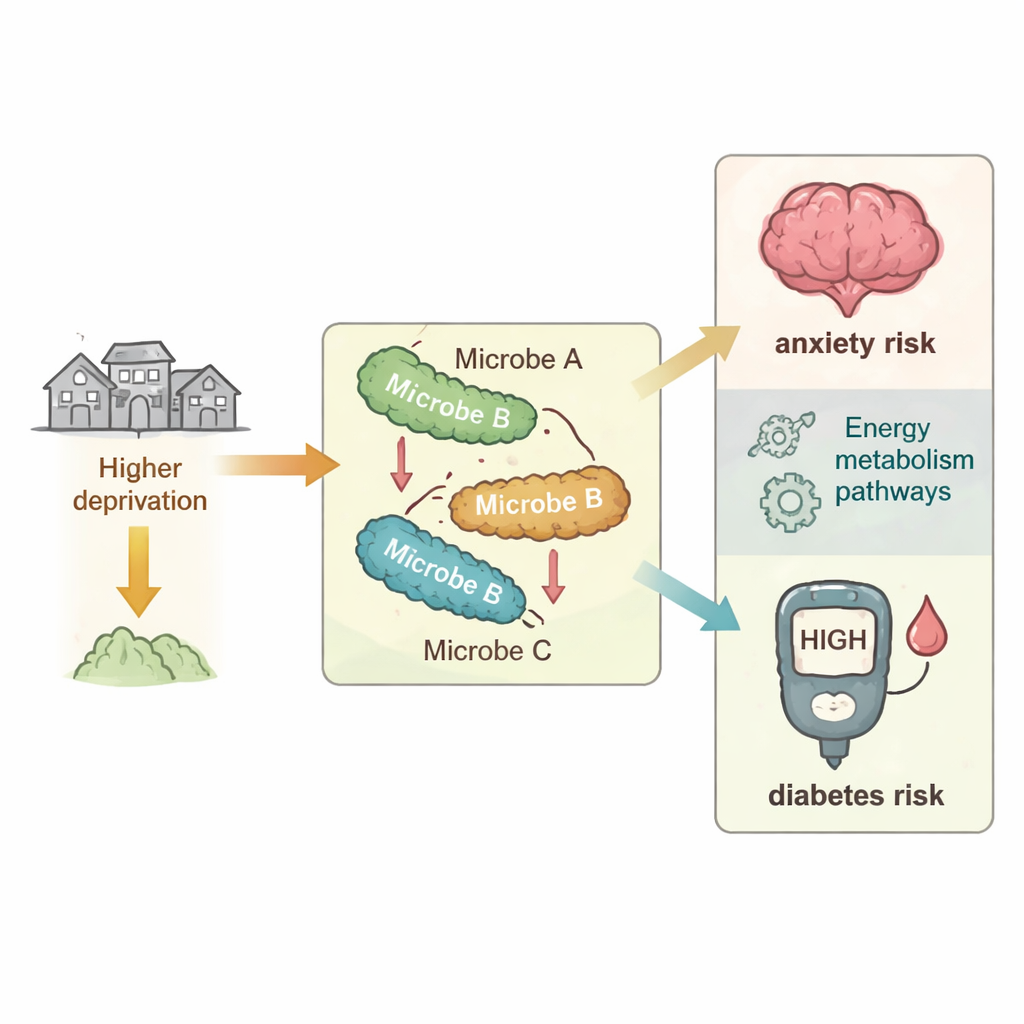
How Microbes Bridge Stress, Anxiety, and Diabetes
The study also confirmed what many public health reports have shown: people from more deprived areas were more likely to have anxiety and diabetes. Crucially, some of the microbes that were depleted under deprivation were also linked to lower anxiety and lower diabetes risk. Using statistical techniques that test for “mediation,” the researchers showed that two particular butyrate-producing species appeared to carry part of the effect of deprivation to anxiety and diabetes. In other words, living in a deprived neighborhood was associated with fewer of these microbes, and having fewer of them, in turn, was linked to higher odds of these conditions—though only a modest fraction of the total risk was explained.
What This Means for Everyday Health
For non-specialists, the takeaway is that health inequalities are not just about lifestyle choices or access to clinics; they may be literally written into our biology through the microbes that live in our gut. This study suggests that neighborhood deprivation can chip away at microbial diversity, erode populations of helpful, mood- and metabolism-supporting bacteria, and blunt important microbial energy pathways, nudging people toward higher anxiety and diabetes risk. While the work focused on women in the UK and cannot yet prove cause and effect, it strengthens the idea that supporting gut health—through better diets, reduced chronic stress, and healthier environments—could be one avenue to soften the biological impact of living in disadvantaged neighborhoods.
Citation: Lin, Y., Kouraki, A., Cheetham, N.J. et al. Gut microbiome composition and function reflect socioeconomic deprivation. npj Biofilms Microbiomes 12, 25 (2026). https://doi.org/10.1038/s41522-026-00917-9
Keywords: gut microbiome, socioeconomic deprivation, anxiety, type 2 diabetes, health inequalities