Clear Sky Science · en
Microbiota composition of the female reproductive tract and miscarriage: a systematic review and meta-analysis
Why tiny companions in the womb matter
Miscarriage is one of the most painful experiences a family can face, and in many cases doctors still cannot say exactly why it happens. This article explores an emerging suspect: the trillions of microscopic organisms that live in the female reproductive tract. By pulling together results from dozens of studies, the authors ask whether shifts in these microbes may tilt the balance between a healthy pregnancy and early loss — and what that might mean for future screening and treatments.
The hidden community inside the reproductive tract
The vagina, cervix, and uterus are home to a bustling community of bacteria, viruses, and fungi known as the microbiota. In people of reproductive age, these communities are usually dominated by friendly Lactobacillus bacteria, which help keep the environment acidic and hostile to harmful germs. But not everyone has the same microbial mix, and factors such as age, ethnicity, diet, hygiene, and hormones can all reshape this living ecosystem. Scientists have begun to wonder whether certain patterns of microbes might make it harder for embryos to implant or for pregnancies to continue, especially when no obvious medical cause can be found.
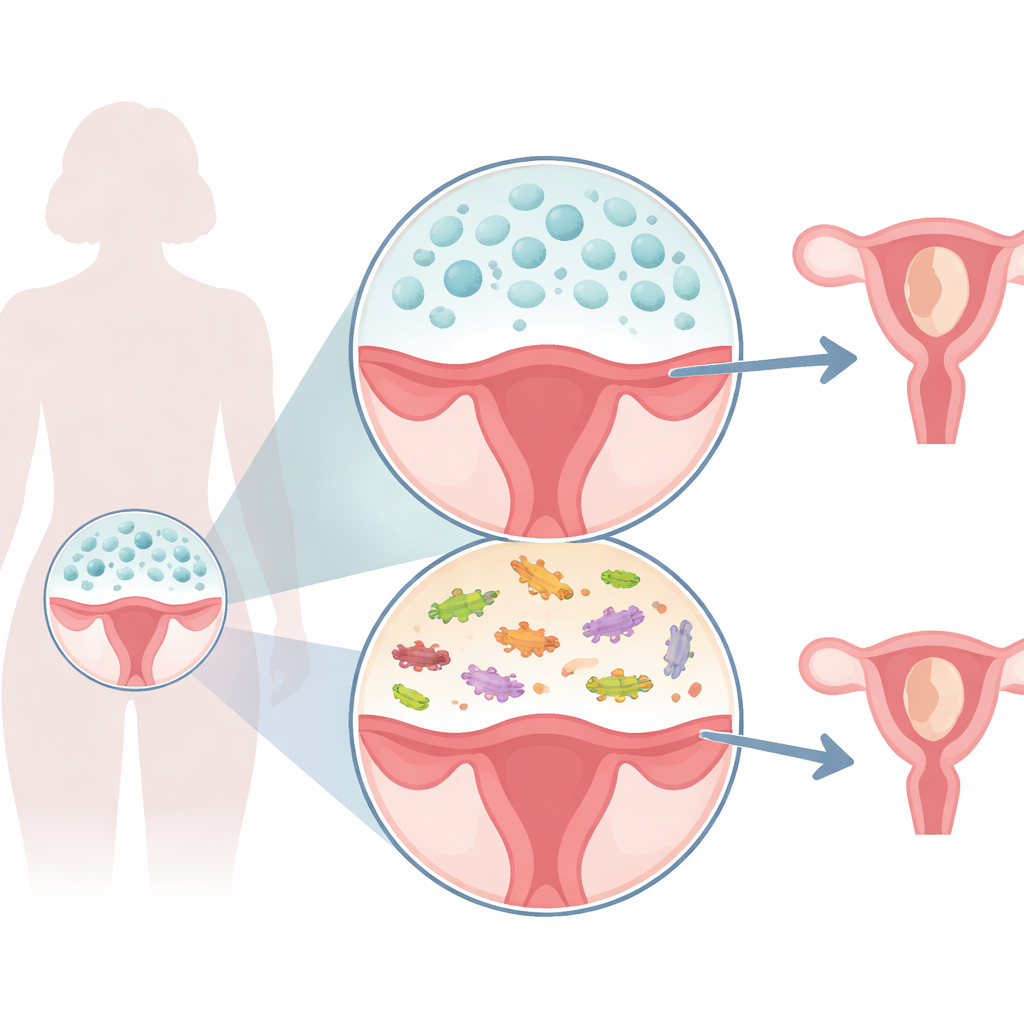
What the researchers set out to find
To get a clearer picture, the authors conducted a systematic review and meta-analysis — a kind of study that gathers and re‑analyses data from many previous investigations. They searched major medical databases and found 43 studies that used modern DNA sequencing to map microbes in the vagina, cervix, or uterus of more than 5,000 women. These women either had a current miscarriage, a history of one or more miscarriages, or no such history and served as controls. Some studies focused on one‑off, unpredictable losses (called sporadic miscarriages), while others looked at people who had lost multiple pregnancies and were thought to have a higher underlying risk.
Patterns in friendly and unfriendly microbes
Across this large body of work, one pattern stood out: women who had miscarried tended to have fewer Lactobacillus bacteria in their reproductive tract than those with ongoing or successful pregnancies. This drop in friendly microbes was clearest in sporadic miscarriage, both in the vagina and within the uterus itself. In some studies, the overall mix of species became slightly more varied when Lactobacillus declined, suggesting that the loss of a single dominant group allowed a broader cast of bacteria to take hold. A handful of studies also reported higher levels of other microbes, such as Bacteroides, Streptococcus, and Atopobium, which are sometimes linked to vaginal infections, though these findings were not consistent from one study to another.
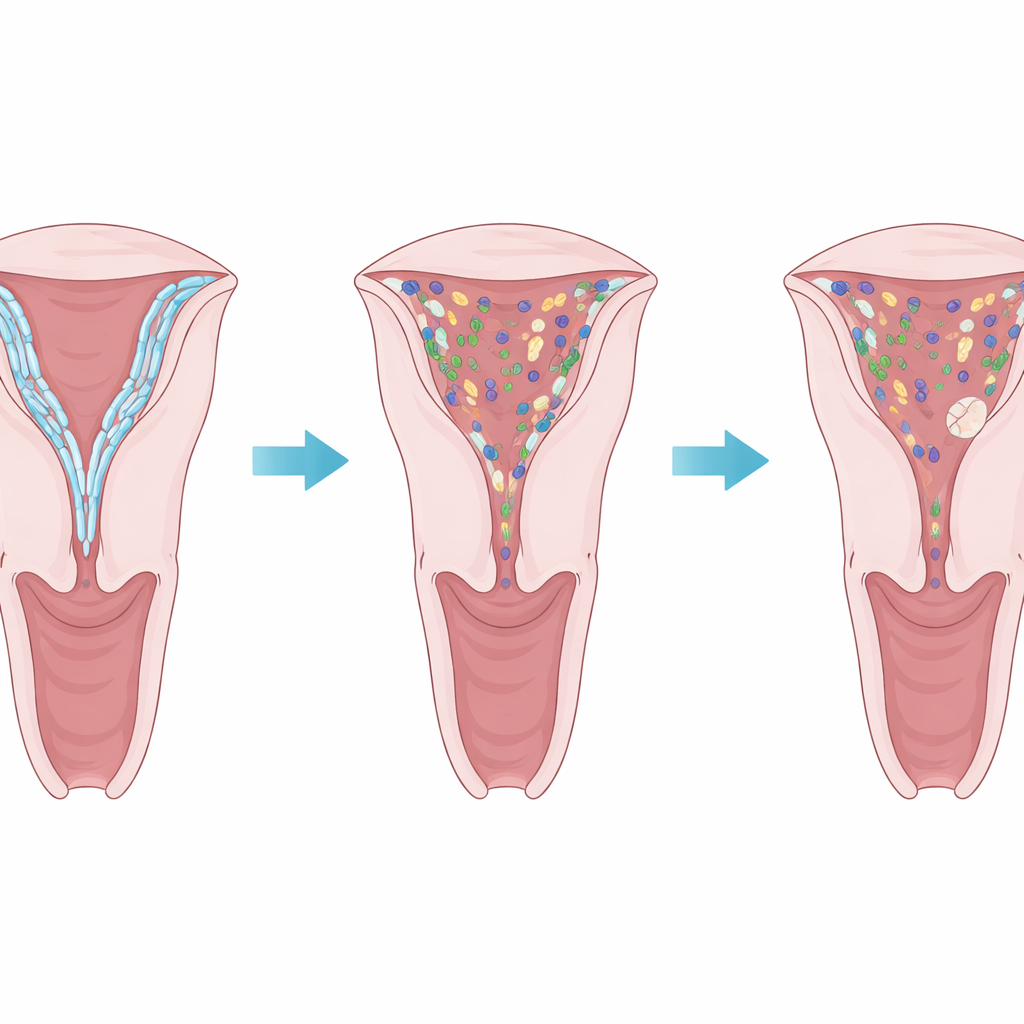
Why the evidence is still murky
Despite the striking link with Lactobacillus, the overall picture remains far from settled. The studies the authors reviewed differed in many important ways: how they defined miscarriage, when samples were taken in relation to pregnancy or the menstrual cycle, which part of the reproductive tract they sampled, how they stored and processed samples, and which DNA methods and computer tools they used. Many did not carefully control for age, previous pregnancies, or other health factors, and most were judged to be of low or moderate quality. These differences make it hard to know whether reported shifts in microbes reflect true biological changes or simply differences in methods, and they limit how confidently we can claim that microbes help cause miscarriage rather than just changing alongside it.
What this means for care and future research
The authors conclude that lower levels of Lactobacillus in the female reproductive tract are consistently associated with miscarriage and may one day serve as a warning sign or treatment target. Approaches such as probiotics, antibiotics, or even transplanting vaginal microbes from a healthy donor are already being explored, but so far have shown mixed results for improving pregnancy outcomes. Before microbiome-based tests or therapies can be trusted, the field needs larger, better designed studies that use shared standards for sampling, sequencing, and reporting. For now, the message to patients is cautious but hopeful: the microbes in the reproductive tract do seem to matter for pregnancy, but turning that knowledge into reliable prevention or treatment will require more careful science.
Citation: Black, N., Henderson, I., Quenby, S. et al. Microbiota composition of the female reproductive tract and miscarriage: a systematic review and meta-analysis. npj Biofilms Microbiomes 12, 78 (2026). https://doi.org/10.1038/s41522-025-00901-9
Keywords: miscarriage, vaginal microbiome, Lactobacillus, pregnancy loss, endometrial microbiota