Clear Sky Science · en
An immunobiliary single-cell atlas resolves crosstalk between type 2 conventional dendritic cells and γδ T cells in cholangitis
Why bile duct inflammation matters
When the tiny tubes that drain bile from the liver become inflamed or blocked, the consequences can be long‑lasting: ongoing injury, scarring, and eventually liver failure. Diseases such as primary sclerosing cholangitis often follow this path, yet the early immune events that turn short‑term damage into chronic fibrosis have remained unclear. This study maps, cell by cell, how specialized immune cells surrounding the bile ducts talk to each other during cholangitis and reveals a key communication loop that helps drive liver scarring.
The liver’s busy neighborhood around bile ducts
The researchers focused on the “immunobiliary niche” – the zone where bile duct cells, blood vessels, and resident immune cells meet. Using human liver samples and spatial transcriptomics, they showed that dendritic cells, T cells, and bile duct lining cells cluster tightly around the larger ducts. Similar arrangements appeared in healthy mouse livers. In a mouse model that mimics cholestatic bile duct injury, this niche expanded dramatically as ducts reacted to damage and immune cells crowded around them. Bile duct cells switched on genes for inflammatory signals and cell‑recruiting factors, suggesting they do more than passively endure injury: they actively call in and shape nearby immune populations.
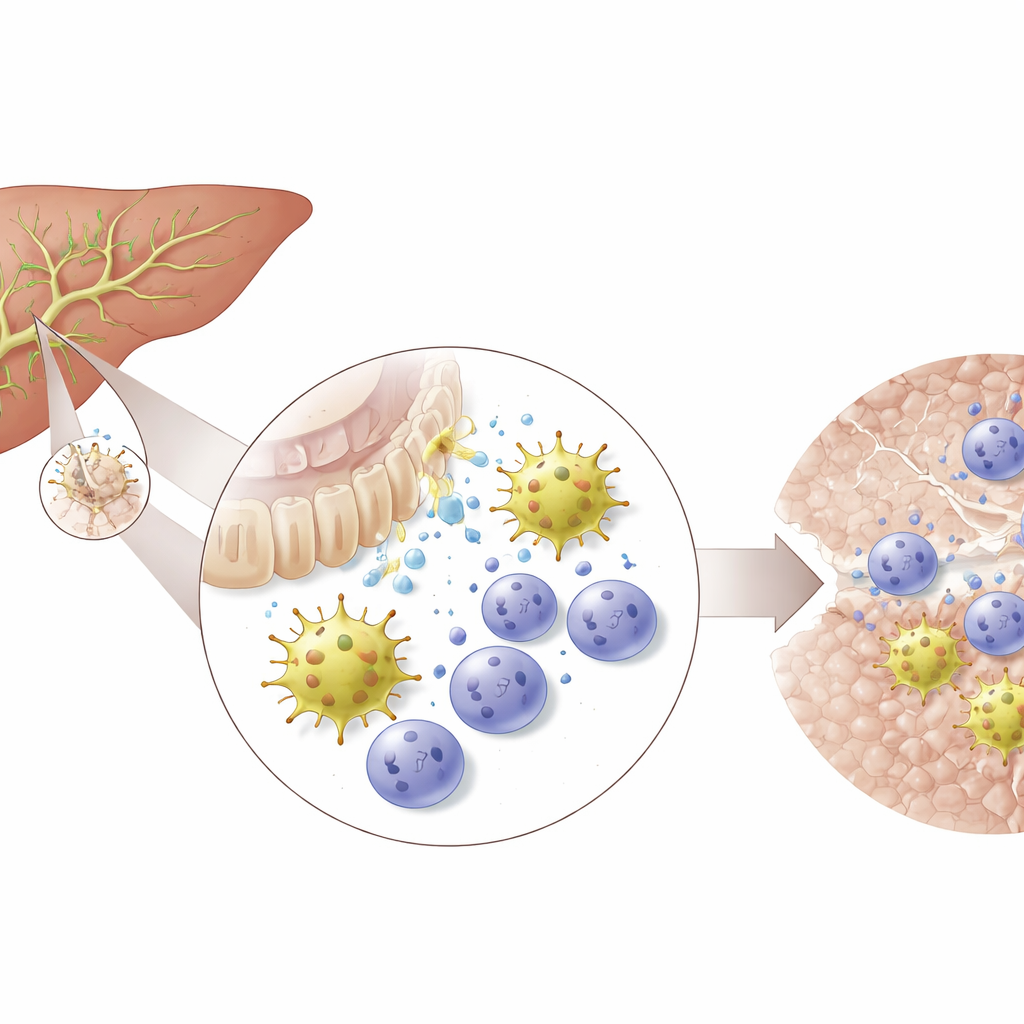
How one dendritic cell type takes center stage
Among the many immune cells present, one population stood out: type 2 conventional dendritic cells, particularly a subset called cDC2B. Single‑cell RNA sequencing over multiple time points showed that these cells became more abundant soon after bile duct injury began, outnumbering other dendritic cell types. The team reconstructed a developmental path from immature precursors to mature, tissue‑adapted cDC2B cells marked by specific genes and by signals linked to promoting a particular flavor of immune response. As disease progressed, resident mature cDC2B cells became exhausted and were gradually replaced by newly arrived precursors, which could still be steered toward either inflammatory or more restorative states depending on cues from their surroundings.
Specialized T cells that fuel scarring
The study then zoomed in on a relatively rare group of “unconventional” T cells known as γδ T cells. These cells turned out to be the main producers of IL‑17, a molecule already implicated in liver inflammation and fibrosis. The authors identified distinct γδ T cell subsets, including resident cells and more migratory cells that circulate through lymph nodes and blood. Both types could become IL‑17‑producing “γδ T17” cells, but they differed in their gene‑regulation programs and in how they likely move between tissues. Spatial mapping in mouse livers and human primary sclerosing cholangitis tissue showed that γδ T cells and cDC2B cells sit in close proximity around damaged bile ducts, placing them in ideal position to interact.
A direct conversation that worsens liver damage
By combining computational ligand–receptor analysis, in vitro co‑culture experiments, and selective cell depletion in mice, the authors uncovered a direct communication hub between cDC2B cells and γδ T cells. Dendritic cells activated by bile duct injury provided both soluble factors and contact‑dependent signals that pushed γδ T cells into an IL‑17‑producing state. One key contact signal involved a pair of surface molecules (Icosl on dendritic cells and Icos on γδ T cells). When the researchers selectively removed cDC2B cells, γδ T17 cells dropped sharply in both liver and draining lymph nodes, and early fibrotic markers decreased. Conversely, removing γδ T cells or genetically disabling IL‑17 signaling reduced liver scarring and biochemical signs of cholestasis, underscoring the fibrogenic power of this axis.
From local crosstalk to whole‑organ impact
The work also shows that this interaction is not confined to the liver itself. Using single‑cell protein and RNA profiling of liver‑draining lymph nodes, the team found that mature cDC2B cells migrate from the liver to these nodes, where they again engage γδ T cells and help shape IL‑17‑biased responses. At the epigenetic level, immature dendritic cell precursors lacked open chromatin at key signaling genes, meaning they were less able to support this crosstalk until they had fully matured. Across several models of bile duct injury, changes in this dendritic cell–γδ T cell circuit recurred, suggesting a common pathway by which acute bile duct damage can be translated into chronic inflammation and fibrosis.
What this means for people with bile duct disease
For non‑specialists, the central message is that not all immune cells around the bile ducts are equal. A specific dendritic cell subset, once activated by injured bile duct cells, programs nearby γδ T cells to make IL‑17, and together they help drive the buildup of scar tissue in the liver. Interrupting this conversation – by targeting cDC2B cells, the signals they use to activate γδ T cells, or the IL‑17 they induce – could offer new strategies to slow or prevent fibrosis in cholestatic liver diseases such as primary sclerosing cholangitis. This single‑cell atlas provides a detailed map of where and how to intervene in this critical immunobiliary circuit.
Citation: Thomann, S., Hemmer, H., Agrawal, A. et al. An immunobiliary single-cell atlas resolves crosstalk between type 2 conventional dendritic cells and γδ T cells in cholangitis. Nat Commun 17, 3455 (2026). https://doi.org/10.1038/s41467-026-71537-2
Keywords: cholangitis, bile ducts, dendritic cells, gamma delta T cells, liver fibrosis