Clear Sky Science · en
Routine blood tests and machine learning identify complications in high myopia
Why a simple blood test could help save eyesight
Many people know that being very nearsighted can mean thicker glasses. Fewer realize it can also quietly damage the eye itself, leading to cataracts, glaucoma, retinal detachment, and other problems that can cause permanent vision loss. The equipment needed to detect these complications—specialized eye cameras and scanners—is expensive and unevenly available, especially outside major hospitals. This study explores a surprising alternative: using the results of routine blood tests, combined with machine learning, to flag people with high myopia who may be developing serious eye complications long before symptoms appear.
From common eye problem to silent threat
High myopia, usually defined as very strong short-sightedness, is becoming more common worldwide. Beyond blurred distance vision, it stretches and thins the eye, raising the risk of cataracts, glaucoma, damage to the light-sensitive macula, and retinal detachment. Some of these conditions can be slowed or treated if caught early, but many people with high myopia do not receive regular specialist eye checks. Advanced imaging tools such as optical coherence tomography provide detailed pictures of the eye, yet they are costly, require trained staff, and are scarce in many regions. As a result, many dangerous eye changes are missed until vision is already badly affected.
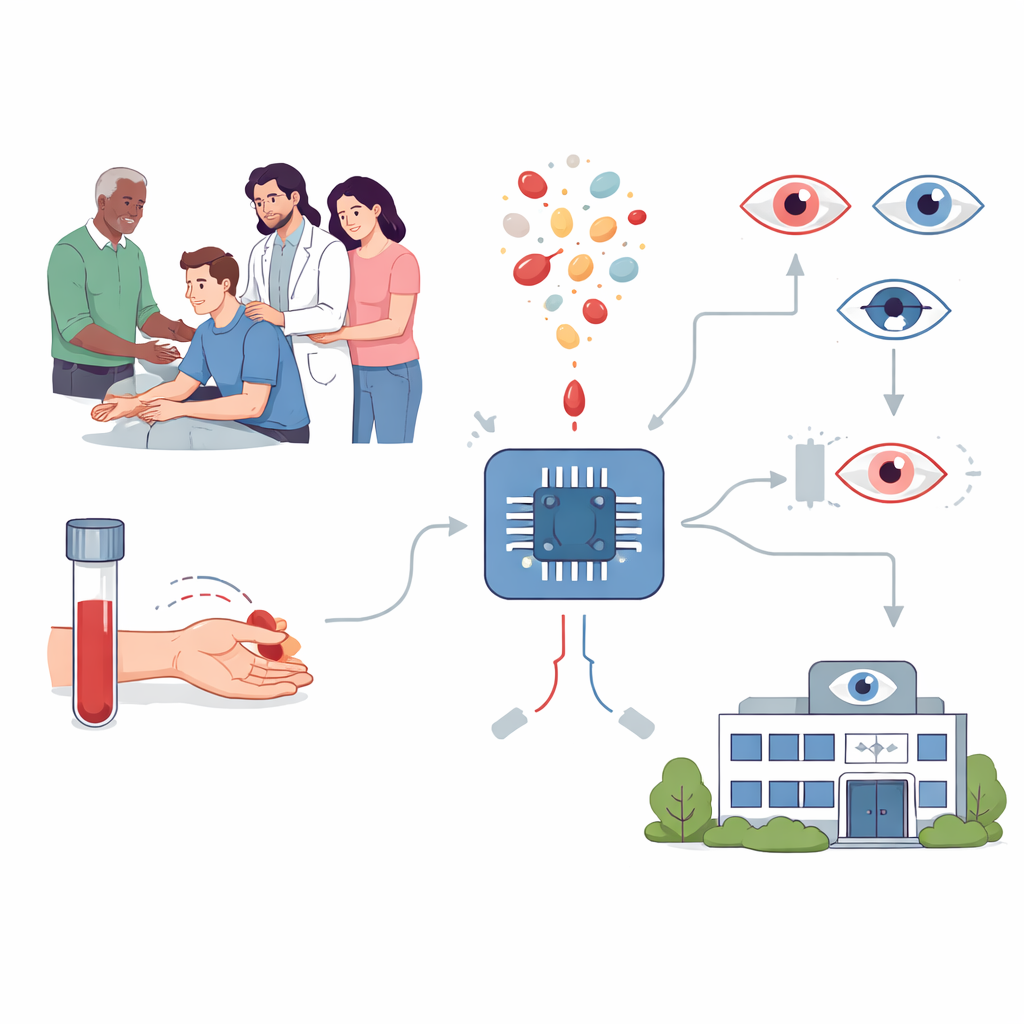
Looking for clues in everyday blood tests
The researchers asked whether information already collected during standard health checkups could help. Routine blood tests are cheap, widely available, and performed millions of times a day to monitor general health. Earlier work hinted that certain blood markers of inflammation, metabolism, and clotting are linked to eye diseases. In this study, the team gathered data from more than 10,000 people with high myopia treated at five hospitals in China. Some had no further problems; others had one of five major complications: cataract, macular degeneration, abnormal new blood vessels under the retina, glaucoma, or retinal detachment. For each person, 61 common laboratory measurements—including types of white blood cells, fat levels, and clotting measures—were fed into a range of machine learning algorithms to see whether patterns in the blood could distinguish those with complications from those without.
A nine-number fingerprint for eye risk
Among many tested algorithms, a type of model called a random forest performed especially well. Remarkably, the model did not need all 61 measurements. After careful feature selection, a set of just nine routinely measured markers—mainly certain immune cells (eosinophils and basophils and their percentages), platelets, uric acid, and blood fats such as triglycerides and apolipoprotein B—captured almost all of the predictive power. These markers fit with what is known about how inflammation, blood lipids, and clotting contribute to eye damage in high myopia. Using only these nine values, the model correctly separated uncomplicated from complicated high myopia with very high accuracy in the original hospital cohort, and its performance remained strong when tested in two additional hospital groups.
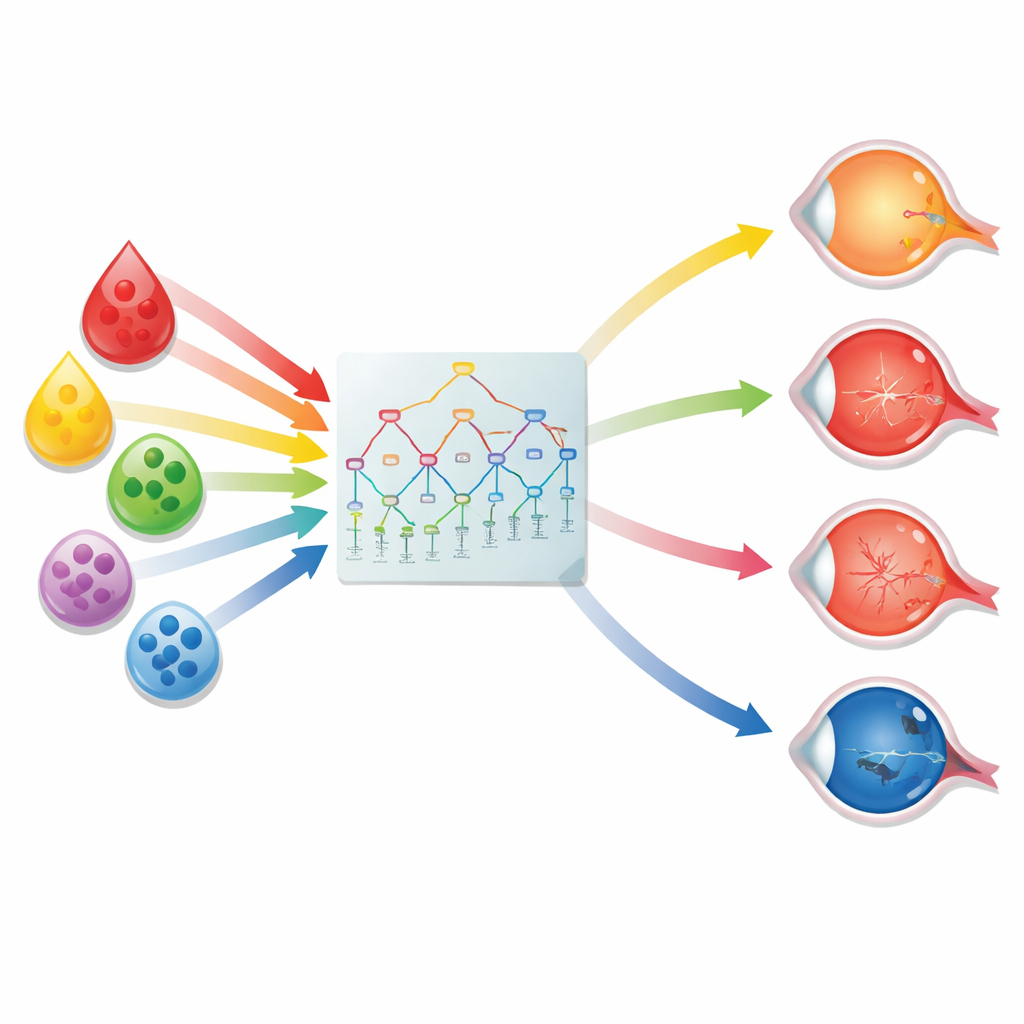
From computer model to real-world screening
To see whether this approach could work in everyday practice, the researchers embedded the nine-marker model in a simple web app that clinicians can use at the time of a blood draw. In a prospective hospital study of more than 4,500 people with high myopia, the tool labeled some as high risk and others as low risk. When these patients later underwent detailed eye examinations, those flagged as high risk were much more likely to have a true complication, and the model missed relatively few cases. The team then moved into the community, applying the model to nearly 1,900 people with high myopia identified among over 300,000 adults taking part in routine health checks. Among those the model marked as high risk and who agreed to further eye testing, nearly three out of four were confirmed to have a serious complication—far higher than would be expected if everyone were referred blindly.
What this could mean for patients and health systems
The study suggests that something as simple as a standard blood panel, interpreted through a carefully trained algorithm, can act as an early-warning system for dangerous eye disease in people with high myopia. This does not replace specialist eye imaging or examination; instead, it helps decide who most urgently needs that scarce attention. In settings where eye equipment and specialists are limited, such a blood-based triage tool could make population screening more practical and affordable, catching many cases earlier while avoiding unnecessary referrals. If validated in more countries and refined to reduce missed cases and false alarms, this approach could become a scalable way to protect sight using tests that are already part of routine care.
Citation: Li, S., Ren, J., Wang, F. et al. Routine blood tests and machine learning identify complications in high myopia. Nat Commun 17, 3930 (2026). https://doi.org/10.1038/s41467-026-70891-5
Keywords: high myopia, vision screening, machine learning, blood biomarkers, eye complications