Clear Sky Science · en
Morphological plasticity and visual acuity in the natural course of epiretinal membrane-foveoschisis: A longitudinal OCT study
Why small eye changes matter
As people age, many develop a thin film of scar-like tissue on the surface of the retina at the back of the eye. In some, this film starts to tug on the very center of sight, the fovea, leading to tiny splits within the retinal layers. Doctors can spot these changes with modern scanners, but they have struggled to predict which eyes will stay stable and which will slowly lose central vision. This study followed more than a hundred such eyes for several years to learn how their structure and sharpness of sight change over time, and to identify warning signs that might call for closer monitoring or surgery.
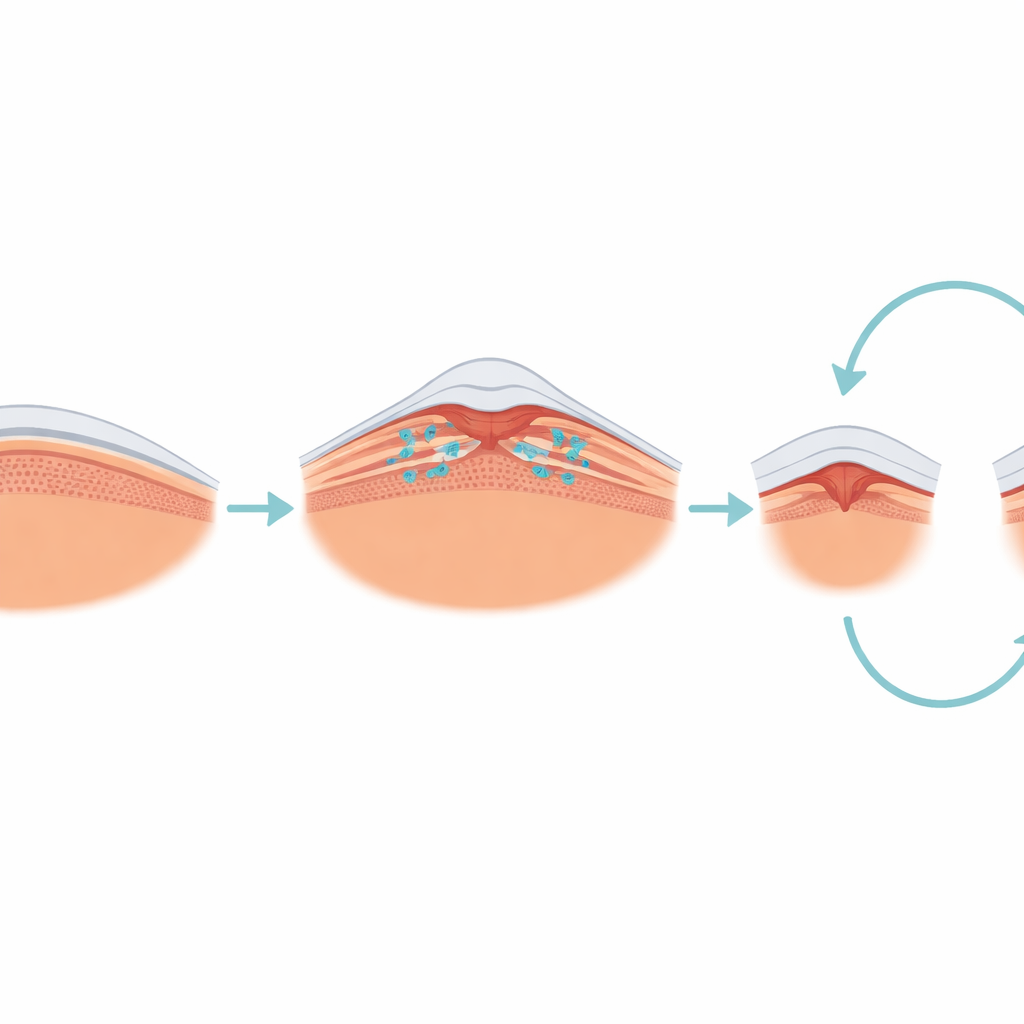
The condition at the center of vision
The researchers focused on a condition called epiretinal membrane-foveoschisis, in which a thin, contracting sheet on the retinal surface pulls sideways on the fovea and creates small splits within the tissue. Unlike more advanced types of macular damage that involve clear tissue loss, this disorder is mainly about traction and distortion. Using high-resolution optical coherence tomography (OCT) scans, the team classified each eye into simple shapes: an “open-flat” form with a relatively shallow central dip, an “open-elevated” form with raised edges, and a “closed” form in which the membrane covers the fovea completely. They then tracked how these shapes and patients’ visual clarity evolved over an average of almost five years.
Vision that mostly holds steady
Despite the sometimes dramatic appearance of the retinal scans, overall sharpness of vision changed very little in this group. On average, eyes started and ended the study with nearly the same reading on the vision chart, and the typical change was smaller than one line. About one quarter of eyes improved meaningfully, one quarter worsened, and the rest stayed about the same. Eyes that had cataract surgery during follow-up tended to see somewhat better, while those that already saw poorly at the beginning were more likely both to end up with worse final vision and, at the same time, to show some improvement relative to their own baseline. Age, sex, and basic thickness measurements of the central retina were less helpful in predicting outcome.
Retinas that reshape themselves
Even though vision was mostly stable, the microscopic structure of the macula often changed in striking ways. Many eyes kept the same basic subtype over time, but roughly a third shifted from one shape to another. The common open-flat form sometimes evolved toward more complex patterns that share features with a partial-thickness macular hole, including undermined edges and true tissue loss. A small minority progressed further toward a classic lamellar macular hole or even a full-thickness hole, while a few eyes surprisingly drifted back toward nearly normal central anatomy. Throughout the group, OCT scans revealed dynamic gains and losses of tiny cyst-like spaces, increased steepness of the foveal walls, new bumps on the foveal floor, and changes in the fine reflecting line associated with the light-sensing cells.
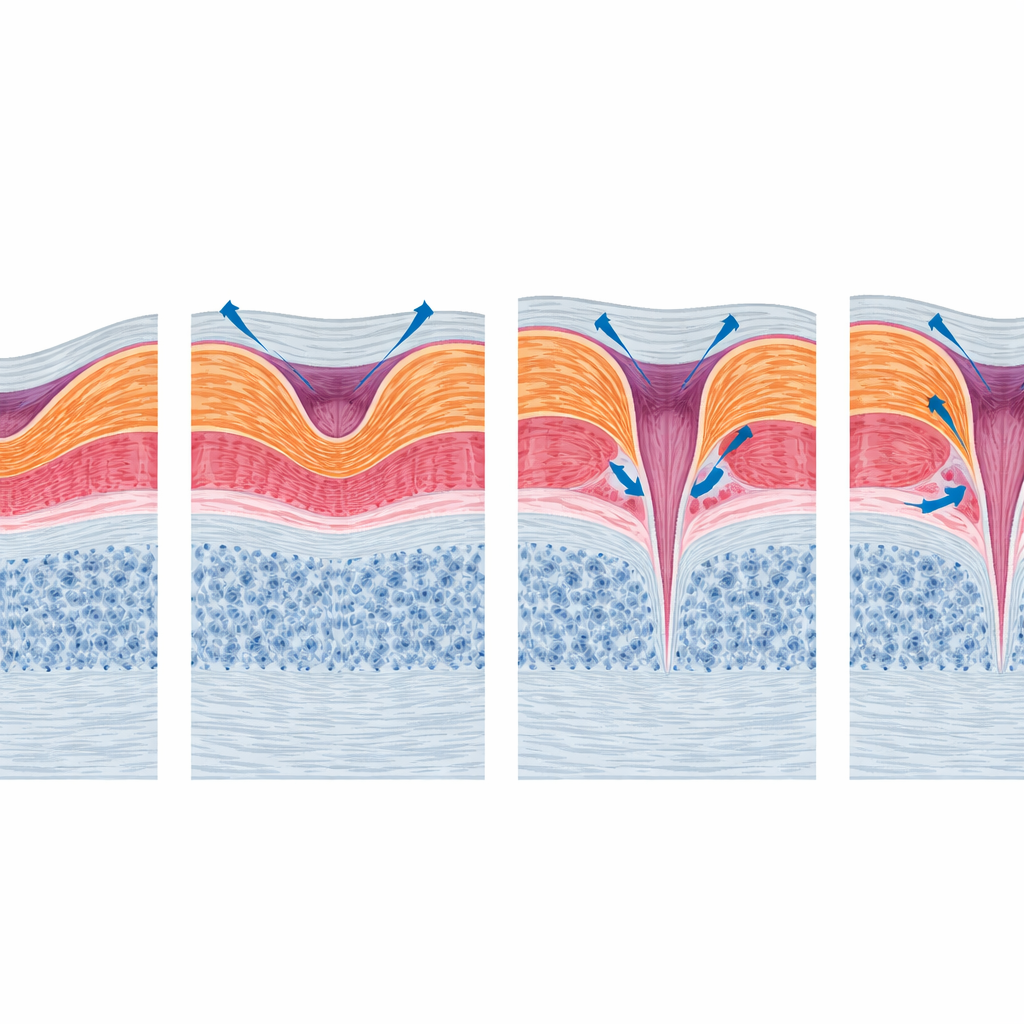
Clues hidden in fine retinal details
When the authors looked for structural features that tracked with vision, they found that not all visible distortions were equally important. Simple measures such as overall retinal thickness or the width of the split area did not reliably predict how well patients could see. In contrast, damage to the ellipsoid zone—a thin band corresponding to the inner segments of the photoreceptors—was linked to poorer sight in basic analyses, underscoring the importance of the health of light-sensing cells. However, this link weakened once starting vision and cataract surgery were taken into account, partly because relatively few eyes developed this damage. The pattern suggests that subtle injury to the outer retina may be one of several factors, alongside lens clarity and initial disease severity, that shape long-term visual function.
What this means for patients and doctors
Overall, the study paints epiretinal membrane-foveoschisis as a slow-moving, shape-shifting condition in which the central retina can remodel quite a bit without necessarily causing rapid loss of sharp vision. Most patients can be followed with regular checkups and OCT imaging rather than rushed to surgery. At the same time, the gradual appearance of tissue loss, undermined edges, and disruption in the layer of light-sensing cells may signal eyes at higher risk of future visual decline. Recognizing these structural warning signs could help clinicians tailor follow-up intervals and decide when to discuss earlier surgical treatment with those few patients whose disease is drifting toward more damaging forms.
Citation: Hetzel, A., Wenzel, C.J., Gelisken, F. et al. Morphological plasticity and visual acuity in the natural course of epiretinal membrane-foveoschisis: A longitudinal OCT study. Eye 40, 789–796 (2026). https://doi.org/10.1038/s41433-026-04304-8
Keywords: epiretinal membrane, macular disease, optical coherence tomography, visual acuity, foveoschisis