Clear Sky Science · en
GPER1 reduces skin inflammation by inhibiting keratinocyte proliferation
Why this skin story matters
Psoriasis affects millions of people worldwide, causing red, scaly, and often painful patches of skin. Behind these plaques lies a constant tug‑of‑war between skin cells that grow too fast and immune cells that flood into the area. This study uncovers a surprising peacekeeper in that battle: a lesser‑known estrogen receptor called GPER1. By showing how this molecule calms down skin cell overgrowth and limits immune invasion, the work points to a fresh, more targeted way to treat psoriasis and related skin disorders.
A closer look at troubled skin
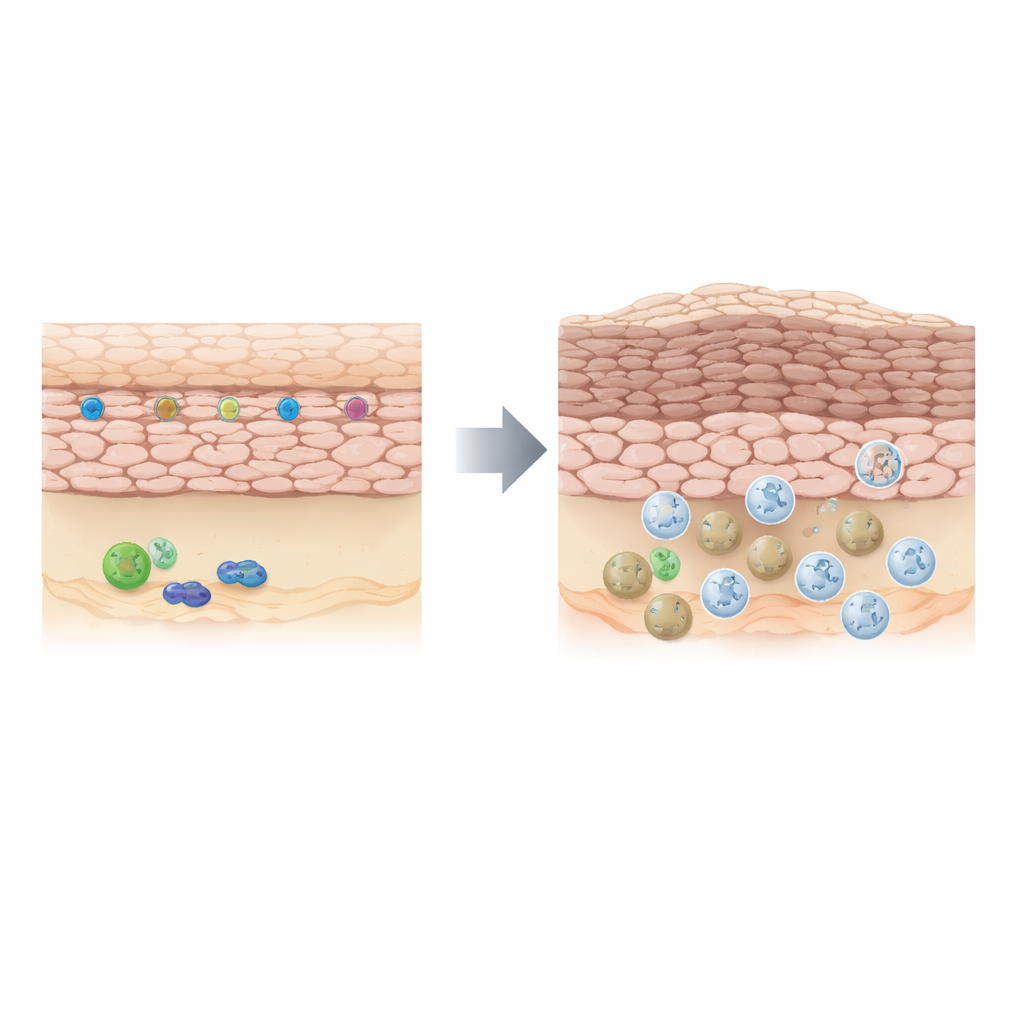
In healthy skin, outer‑layer cells called keratinocytes grow and shed in a tightly controlled cycle. In psoriasis, this balance breaks down: keratinocytes divide too quickly, piling up into thickened plaques while immune cells, especially neutrophils, infiltrate the skin and release inflammatory substances. The authors began by asking whether GPER1, a receptor that senses the hormone estrogen, might be involved. Using gene‑activity data and biopsies from people with psoriasis, they found that GPER1 and several of its downstream signaling partners were consistently less active in diseased skin than in healthy or nearby unaffected skin. Lower GPER1 levels also tracked with higher markers of inflammation and faster keratinocyte growth, hinting that this receptor normally acts as a brake on both processes.
Fish as a window into human skin
To move beyond correlation, the team turned to zebrafish, whose transparent larvae allow live imaging of skin and immune cells. They used a well‑established zebrafish strain that develops chronic skin inflammation and keratinocyte overgrowth resembling key features of psoriasis. When they disrupted the fish version of the receptor, Gper1, the larvae developed more clumps of keratinocytes at the skin surface and showed stronger neutrophil infiltration into the skin. Surprisingly, classic signs of inflammatory signaling—such as activation of an alarm pathway called NF‑κB, production of an inflammatory messenger similar to human IL‑1β, oxidative stress, and cell death—did not change with Gper1 loss. This suggested that Gper1 does not simply turn inflammation on or off, but instead shapes how the skin tissue responds to it.
How slowing cell growth tames immune entry
Because the main visible change after Gper1 loss was extra keratinocyte growth, the researchers tested whether this overgrowth itself helped pull neutrophils into the skin. They measured cell division directly and saw that Gper1‑deficient larvae had more dividing keratinocytes. When they treated fish with palbociclib, a drug that blocks cell‑cycle proteins, keratinocyte clumps shrank and neutrophil entry into the skin dropped, even though inflammatory signaling stayed largely the same. Boosting Gper1 activity with a selective drug reduced keratinocyte aggregates as well, although higher doses caused developmental problems in the embryos. Together, these experiments show that controlling keratinocyte proliferation can reduce immune cell infiltration without needing to dampen the entire inflammatory cascade.
Pinpointing where the receptor matters most
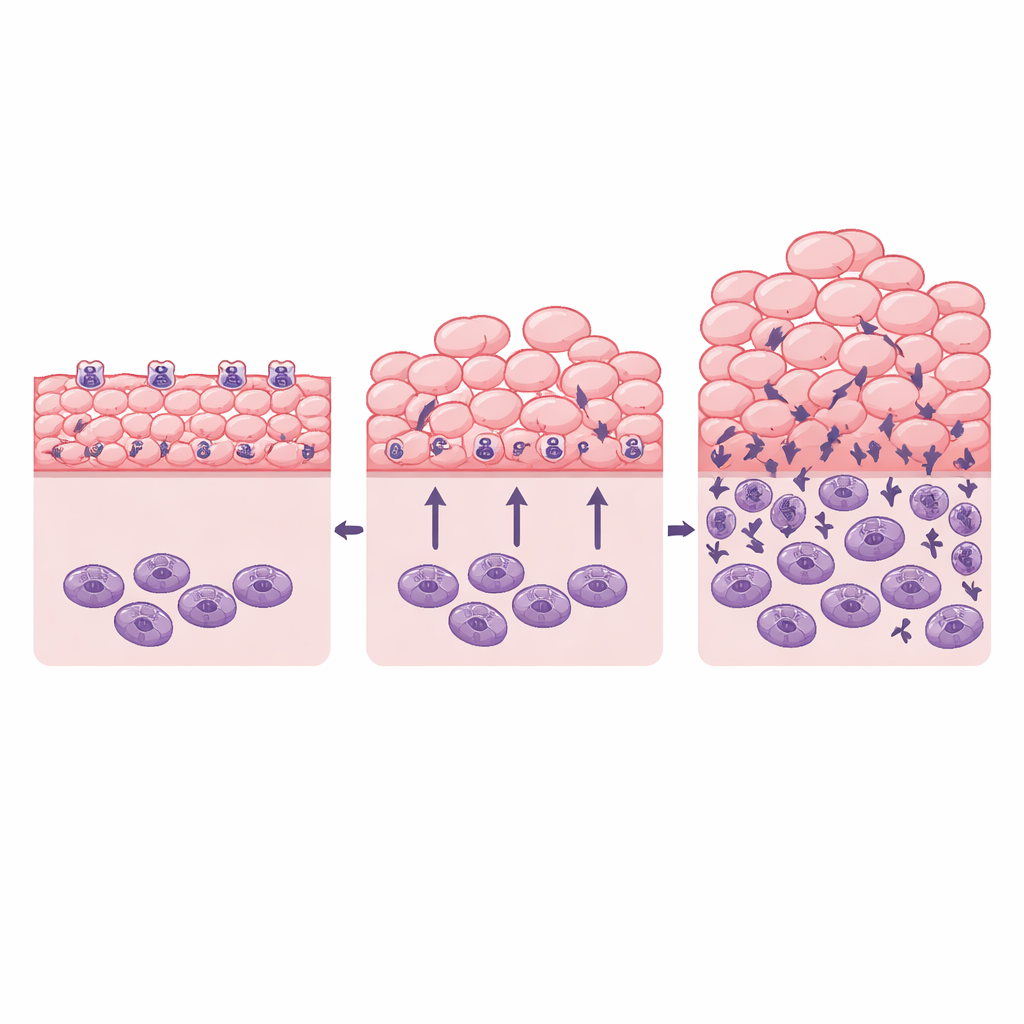
To find out which cells actually need Gper1, the scientists forced extra copies of the receptor either in neutrophils or in basal keratinocytes, the dividing cells at the bottom of the skin layer. Extra Gper1 in neutrophils did not change the skin phenotype. In contrast, overexpressing Gper1 in basal keratinocytes reduced both their proliferation and the number of surface aggregates. Additional imaging in human psoriasis biopsies showed that immune cells in plaques tend to sit extremely close to proliferating keratinocytes, reinforcing the idea that rapidly dividing skin cells open the door for immune invasion. In this view, GPER1 acts within keratinocytes themselves to keep their growth in check, and this indirectly limits how easily immune cells can enter the tissue.
What this means for future treatments
Altogether, the study identifies GPER1 as a natural safeguard against keratinocyte overgrowth and excessive immune‑cell entry into inflamed skin. Rather than directly switching off inflammation, GPER1 shapes the tissue environment so that it is less welcoming to invading neutrophils. Because GPER1 belongs to the same large receptor family targeted by many existing drugs, it may be possible to design medicines that selectively boost this pathway in skin without the broader side effects of traditional estrogen therapies. Such approaches could offer a new angle for treating psoriasis and other hyperproliferative skin diseases by calming the skin’s own growth and gatekeeping machinery instead of broadly suppressing the immune system.
Citation: Pérez-Escudero, N., Cabas, I., Corbalán-Vélez, R. et al. GPER1 reduces skin inflammation by inhibiting keratinocyte proliferation. Cell Death Discov. 12, 166 (2026). https://doi.org/10.1038/s41420-026-03059-1
Keywords: psoriasis, keratinocyte proliferation, GPER1, skin inflammation, neutrophil infiltration