Clear Sky Science · en
Targeting adipocyte ESRRA alleviates osteoarthritis via interrupting inter-organelle crosstalk of complement C3-CFD-MAC cascade
Why joint pain is more than just wear and tear
Many people think osteoarthritis happens simply because joints wear out with age. This study shows a very different picture: our joints are influenced by a hidden conversation between the liver, bone marrow fat, and cartilage. Understanding this long‑distance “organ talk” could open the door to new treatments that work far beyond the knee itself.
Fatty liver, fatty marrow, aching joints
The researchers started from a big puzzle: why do people with aging, obesity, or menopause often develop both fatty liver and fragile, painful joints? In mice, they found that when the liver fills with fat (steatosis) and the bone marrow packs with fat cells, the knee cartilage deteriorates much faster. Instead of acting as quiet storage, marrow fat cells actively release a protein called CFD, while the fatty liver pumps out another protein called C3. These two circulating factors meet in the bloodstream and in the joint, helping to switch on an immune system chain reaction that injures cartilage cells and speeds osteoarthritis. 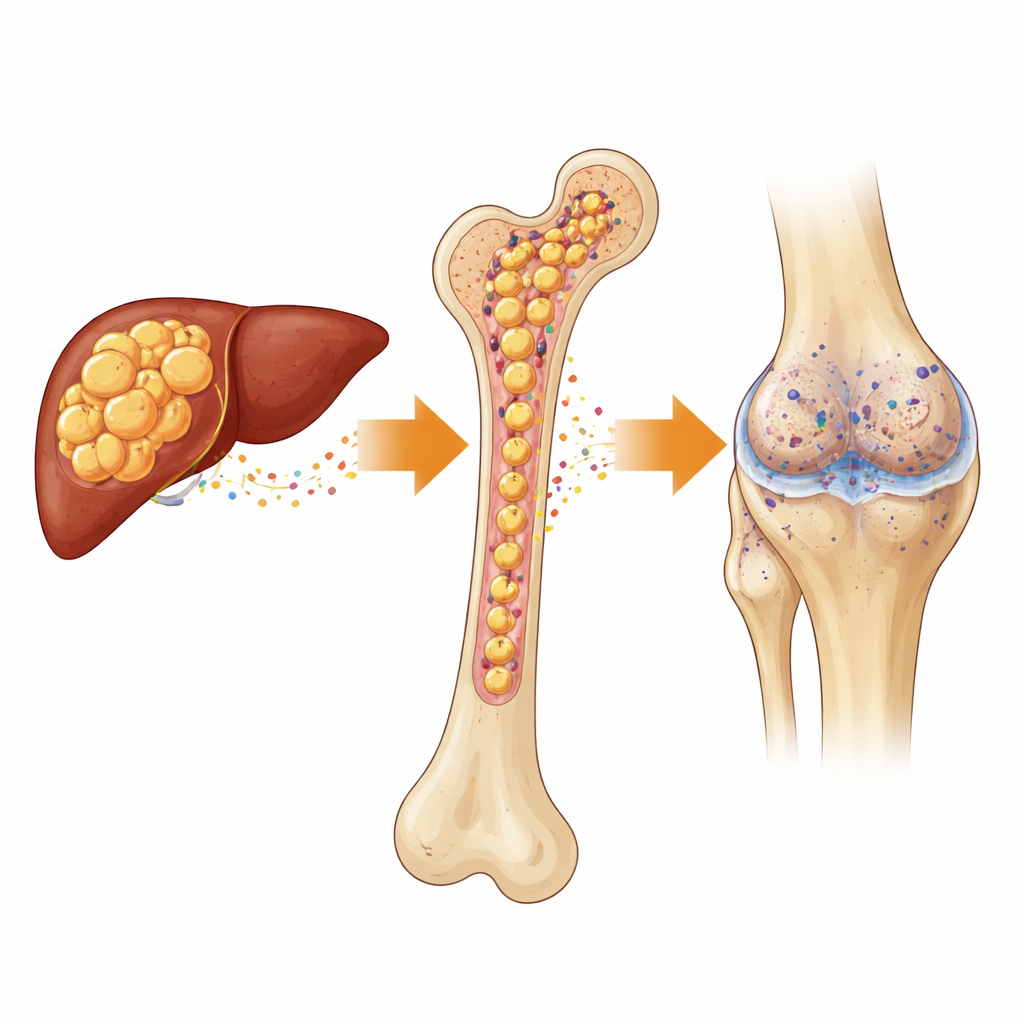
A damaging chain reaction in the joint
C3 and CFD belong to the complement system, a set of blood proteins that normally help fight infections. When overactivated, however, this system can harm the body’s own tissues. In the mice, liver‑derived C3 and marrow‑derived CFD combined to drive a powerful “alternative complement” cascade, ending in formation of small ring‑shaped complexes (called MAC) that punched into cartilage cells. Inside these cells, the damage was traced to overactivation of a signaling switch (ERK1/2) and breakdown of mitochondria, the tiny power plants that keep cells energetic and healthy. The result was a shift toward cell aging, inflammation, and breakdown of the cartilage matrix.
Turning down a key switch in marrow fat
The team then asked whether they could protect joints by quieting the marrow fat cells. They focused on ESRRA, a gene switch in adipocytes that responds to metabolic stress and cholesterol. Using mice engineered to lack ESRRA only in fat cells, they found that bone marrow fat no longer expanded with age or with a high‑fat, high‑cholesterol diet, even though regular body fat and blood lipids were largely unchanged. Importantly, these ESRRA‑deficient marrow fat cells made far less CFD, which meant the joint‑damaging complement cascade could not fully ignite. Aged and overfed mice without adipocyte ESRRA developed much milder osteoarthritis: their joint cartilage was thicker, their bone structure under the cartilage was more normal, and cartilage cells showed less DNA damage, less cell death, and more signs of healthy repair.
From liver–marrow crosstalk to human relevance
To connect these findings to human disease, the scientists examined public liver gene datasets and large human plasma protein studies. They saw that C3 is elevated in people with fatty liver disease, and CFD rises with age and in women with low bone density. In cell‑culture experiments, loading mouse or human liver cells with cholesterol or fatty acids boosted C3 production and release. When this C3‑rich liver medium was combined with CFD‑rich marrow‑fat medium and applied to cartilage cells, the cells rapidly developed mitochondrial damage and hallmarks of aging. Blocking CFD activity with Danicopan, an approved drug that specifically targets this protein, or reducing CFD production by chemically inhibiting ESRRA in human marrow fat cells, largely prevented these harmful effects on human chondrocyte‑like cells. 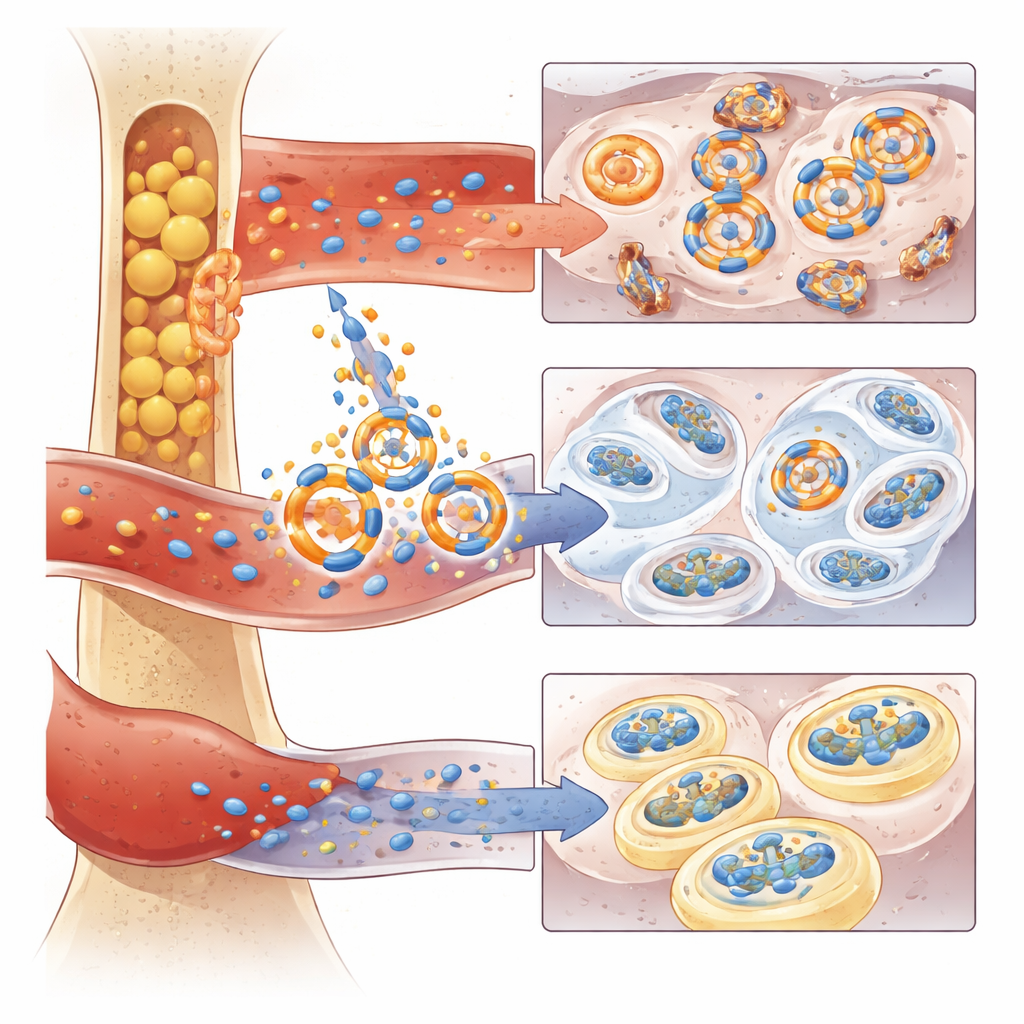
A plant‑derived compound that protects aging joints
Finally, the team tested whether a natural ESRRA‑blocking compound could help whole animals. They treated very old mice with andrographolide, a molecule derived from a traditional medicinal plant. Over three months, these mice showed less liver fat, lower blood levels of both C3 and CFD, reduced marrow fat, and stronger bone. Most strikingly, their knees displayed far less spontaneous osteoarthritis: fewer cartilage lesions, less thickening and scarring of the underlying bone and synovium, and reduced markers of cell aging and damage in cartilage. At the same time, proteins essential for healthy cartilage structure and cell renewal rebounded.
What this means for people with osteoarthritis
This work reframes osteoarthritis as not just a local joint problem but as the outcome of a three‑way axis linking fatty liver, bone marrow fat, and cartilage. When liver and marrow fat are overloaded, they send out C3 and CFD, which team up to form destructive complexes on cartilage cells and damage their energy factories. By turning down ESRRA in adipocytes—or directly blocking CFD—it may be possible to break this damaging chain while leaving most of the immune system intact. Although these findings are in mice and cell models, they point toward future therapies that target metabolic and immune crosstalk, offering hope for disease‑modifying treatments for age‑ and metabolism‑related osteoarthritis.
Citation: Huang, T., Wang, Z., Gao, L. et al. Targeting adipocyte ESRRA alleviates osteoarthritis via interrupting inter-organelle crosstalk of complement C3-CFD-MAC cascade. Bone Res 14, 49 (2026). https://doi.org/10.1038/s41413-026-00527-3
Keywords: osteoporosis, fatty liver, bone marrow fat, complement system, joint degeneration