Clear Sky Science · en
Endothelial GABA protects against aortic dissection by inhibiting endothelial and mitochondrial dysfunction and maintaining vascular homeostasis
Why this heart vessel story matters
Thoracic aortic dissection is a sudden, often deadly tearing of the body’s main artery. It can strike without warning, and even with modern surgery many patients die or suffer serious complications. This study uncovers an unexpected defender inside the vessel wall—a familiar brain chemical called GABA—that helps keep the inner lining of the aorta healthy and the vessel wall intact. Understanding this hidden safety system may open the door to earlier diagnosis and new, gentler treatments that prevent the artery from tearing in the first place.
A hidden weakness in the body’s largest artery
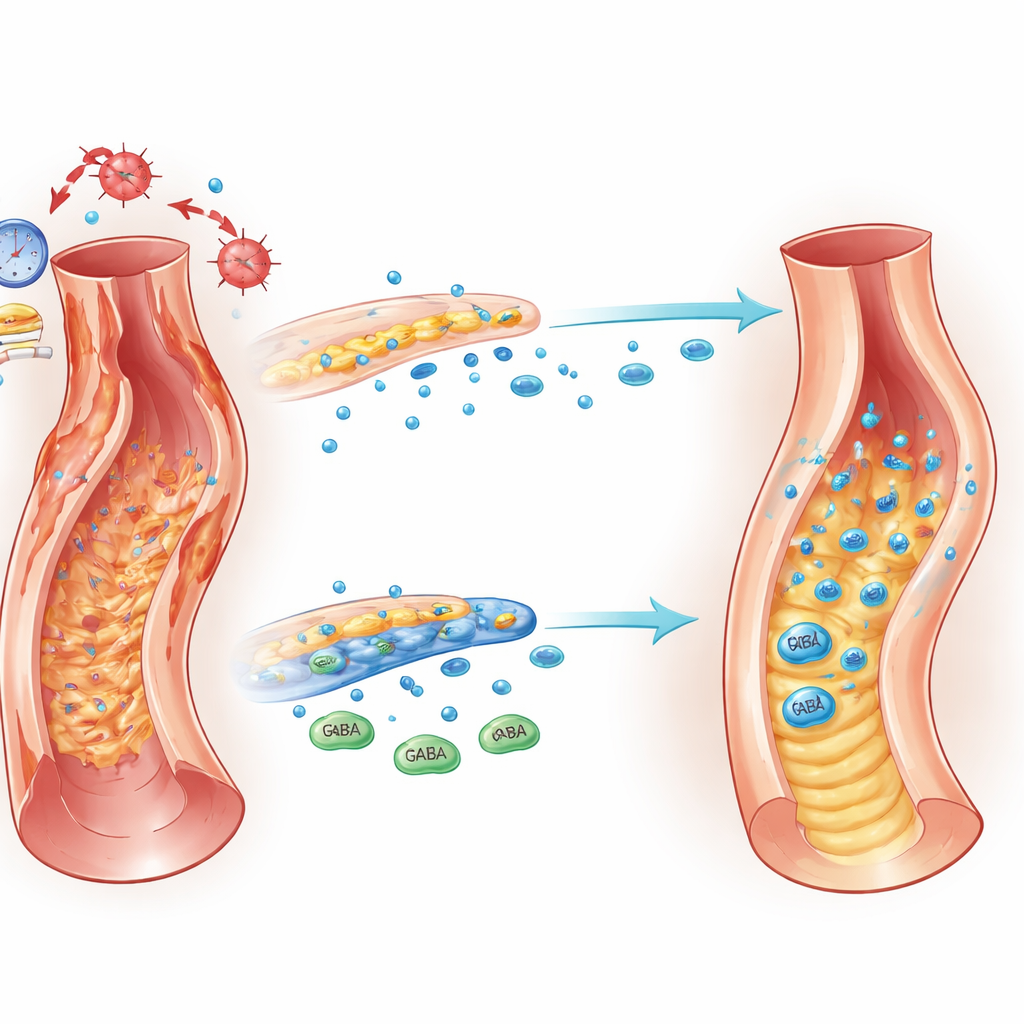
The aorta is built like a reinforced hose, with an inner lining of endothelial cells that controls what passes between blood and tissue, and layers of smooth muscle cells that provide strength and flexibility. In thoracic aortic dissection, a rip in the inner lining allows blood to surge into the wall, splitting its layers and creating a life‑threatening emergency. While past research focused mostly on the muscle cells and invading immune cells, this work highlights the importance of the thin endothelial layer. The authors show that when these lining cells malfunction—becoming leaky, inflamed, and stressed—the entire wall becomes more vulnerable to tearing.
A brain messenger shows up in blood vessels
Gamma‑aminobutyric acid, or GABA, is best known as a calming messenger in the brain. Surprisingly, endothelial cells in the aorta can also make and release GABA. Using detailed metabolic profiling of human aortic tissue, the researchers found that GABA levels are significantly lower in the inner lining of patients with aortic dissection than in people without the disease. The enzyme that makes GABA in these cells, called GAD1, was also reduced. These changes were confirmed both in vessel samples and in blood, suggesting that loss of this “calming” signal is a hallmark of the diseased artery wall.
Protecting the vessel wall in living animals
To see whether GABA is simply a marker or an active protector, the team used a mouse model in which a chemical weakens the aorta and triggers dissections. Giving these mice extra GABA, or forcing their endothelial cells to overproduce it, cut the rate of dissections, reduced deaths, and preserved the normal architecture of the vessel wall. The inner lining remained less leaky, fewer immune cells invaded, and the elastic fibers that give the aorta its spring were better preserved. In contrast, dialing down GAD1 in endothelial cells made dissections more frequent and severe. These experiments show that endothelial‑derived GABA is not just a bystander—it actively guards the integrity of the aortic wall.
How a calming signal tames stressed cells
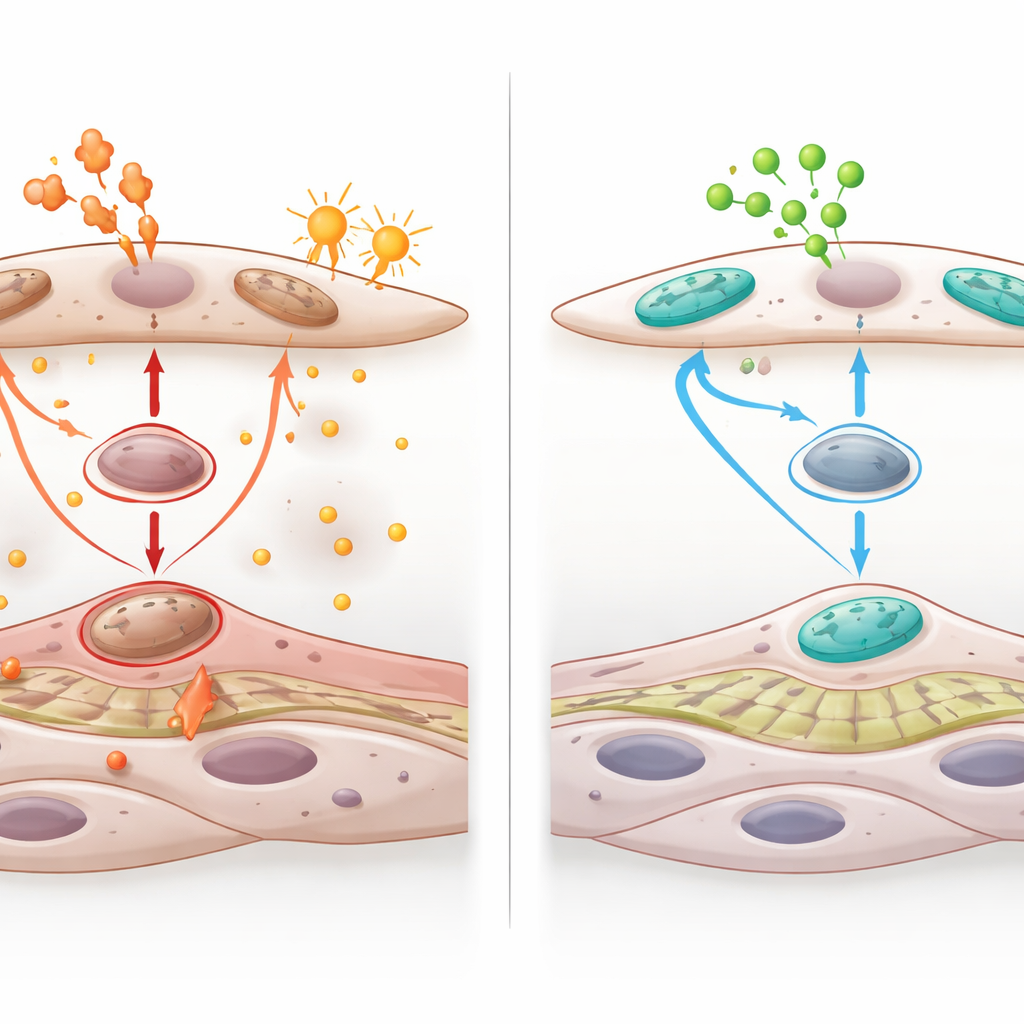
At the microscopic level, the study reveals how GABA keeps endothelial cells from going off the rails under stress. When exposed to oxidants or inflammatory cues, these cells typically suffer mitochondrial damage, pump out reactive molecules and inflammatory proteins, and attract circulating immune cells. GABA, acting through its GABAB receptor, helps maintain healthy mitochondrial shape and energy production, lowers damaging reactive oxygen, and quiets a key stress signaling route known as MAPK–c‑FOS. As a result, the cells express fewer “sticky” surface molecules, undergo less cell death, and form a more stable barrier. GABA released from the endothelium also signals to neighboring smooth muscle cells, restraining enzymes that chew up the vessel’s structural scaffold and dialing down Notch3, a protein tied to harmful muscle cell remodeling.
Toward earlier warning and gentler treatment
Because GABA made by endothelial cells spills into the bloodstream, its level can be measured in a simple blood sample. In a clinical group of patients, those with thoracic aortic dissection had substantially lower plasma GABA than healthy volunteers, and the lowest levels were seen in the more dangerous Stanford type A dissections near the heart. Statistical models combining GABA with standard cardiovascular risk scores improved prediction of who had a dissection. In plain terms, this work suggests that a drop in a “soothing” vessel chemical both weakens the aortic wall and leaves a measurable fingerprint in the blood. Restoring or mimicking this signal—potentially with drugs that selectively stimulate its receptor—could one day help keep the aorta intact and allow doctors to spot trouble before the artery tears.
Citation: Shao, L., Yu, Y., Huang, H. et al. Endothelial GABA protects against aortic dissection by inhibiting endothelial and mitochondrial dysfunction and maintaining vascular homeostasis. Sig Transduct Target Ther 11, 150 (2026). https://doi.org/10.1038/s41392-026-02619-2
Keywords: aortic dissection, endothelial cells, GABA, vascular inflammation, mitochondrial stress