Clear Sky Science · en
A cylindrical projection lithography-fabricated flexible on-catheter in situ integrated sensor for continuous in-artery blood pressure monitoring
Why Watching Blood Pressure from the Inside Matters
High blood pressure silently damages arteries and organs, yet doctors still rely mostly on occasional cuff readings or bulky hospital setups. This paper describes a new way to watch blood pressure continuously from inside an artery using a hair‑thin flexible sensor built directly onto a medical catheter. For patients undergoing heart or brain procedures, or those who need close monitoring in intensive care, such a tiny but accurate sensor could make blood pressure tracking safer, more comfortable, and more informative.
From Fluid Tubes to Built‑In Smart Catheters
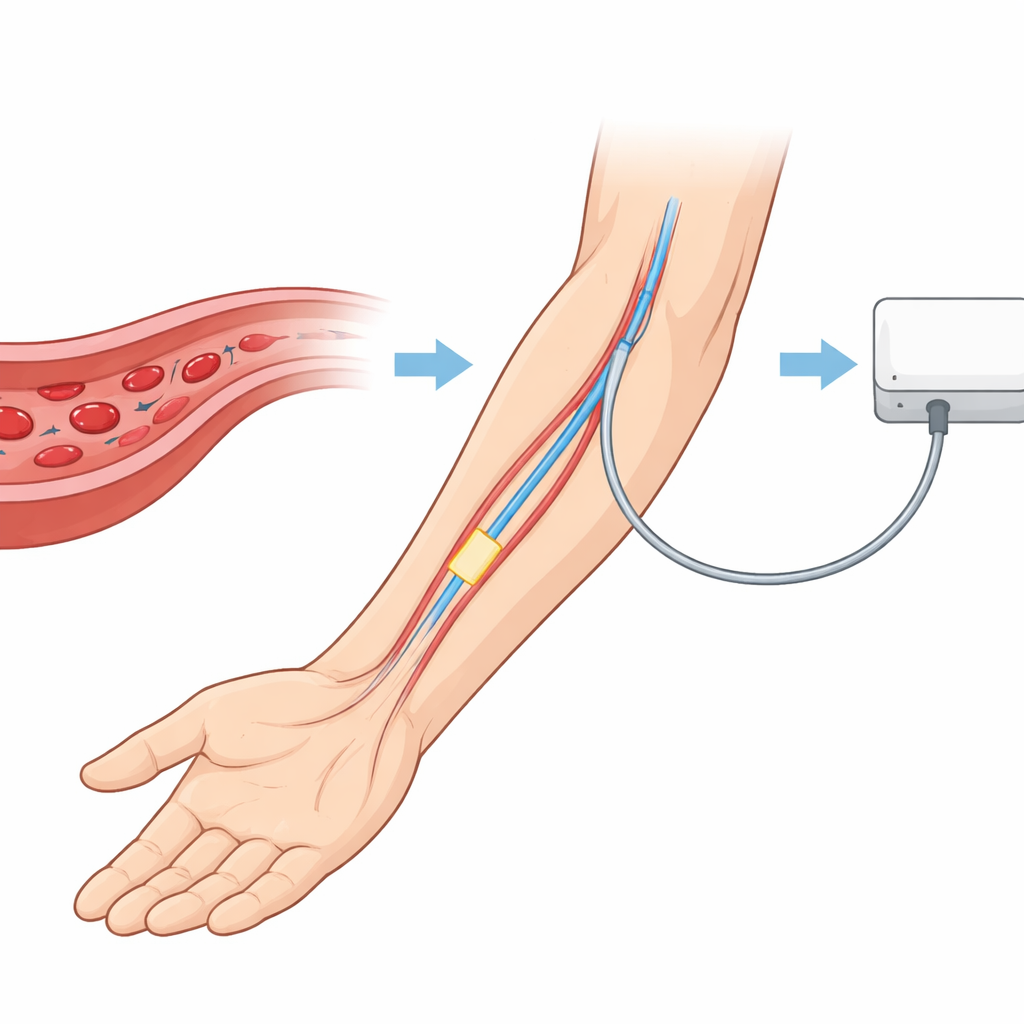
Today’s clinical “gold standard” for continuous blood pressure measurement uses long fluid‑filled tubes connected to an external pressure transducer. While accurate, these systems can distort the true pressure wave, increase infection risk, and limit a patient’s movement. Earlier generations of miniature silicon chips mounted at the catheter tip or on the side of the tube improved signal quality but introduced new compromises: the hardware adds bulk, wiring and waterproof packaging disrupt the smooth profile of the catheter, and further shrinking the chips makes them fragile and less sensitive. The authors of this study tackle these trade‑offs by abandoning the idea of gluing a separate sensor onto the catheter and instead fabricating the sensor directly on the catheter’s outer surface.
A Thin Flexible Skin That Feels Pressure
The core of the new device, called a catheter‑based interventional pressure sensor (CIPS), is a ring of tiny pressure‑sensitive units that wrap around the catheter like a flexible electronic skin. Each unit combines shallow circular pits carved into the catheter wall and a suspended “sandwich” of materials above them. That sandwich consists of a sheet of graphene—a one‑atom‑thick form of carbon known for its strength and electrical sensitivity—together with two very soft silicone layers. When blood pressure rises around the catheter, this stack bends slightly into the pits. The graphene’s electrical resistance changes with the bending, turning the mechanical pulse of blood flow into an electrical signal that can be read out by external electronics.
Smart Wiring and Sealing for Clearer Signals
To turn this delicate structure into a practical medical tool, the researchers solve two key problems: how to collect clean signals and how to keep the sensor working reliably in liquid. They add comb‑like metal fingers, called interdigital electrodes, beneath the sensitive region to create many parallel electrical pathways. This reduces the baseline resistance, which in turn speeds up the sensor’s response, boosts sensitivity, and lowers electronic noise. At the same time, they encapsulate the sensing layer in two ultrathin coatings of medical‑grade silicone. The first supports the fragile graphene during manufacturing; the second seals off microscopic gas pathways that would otherwise cause pressure readings to drift. Together, these choices allow the sensor to respond in under four‑tenths of a second, detect a wide pressure range spanning low to well above normal arterial values, and distinguish changes as small as a few millimeters of mercury.
Engineering for the Body’s Twists and Turns
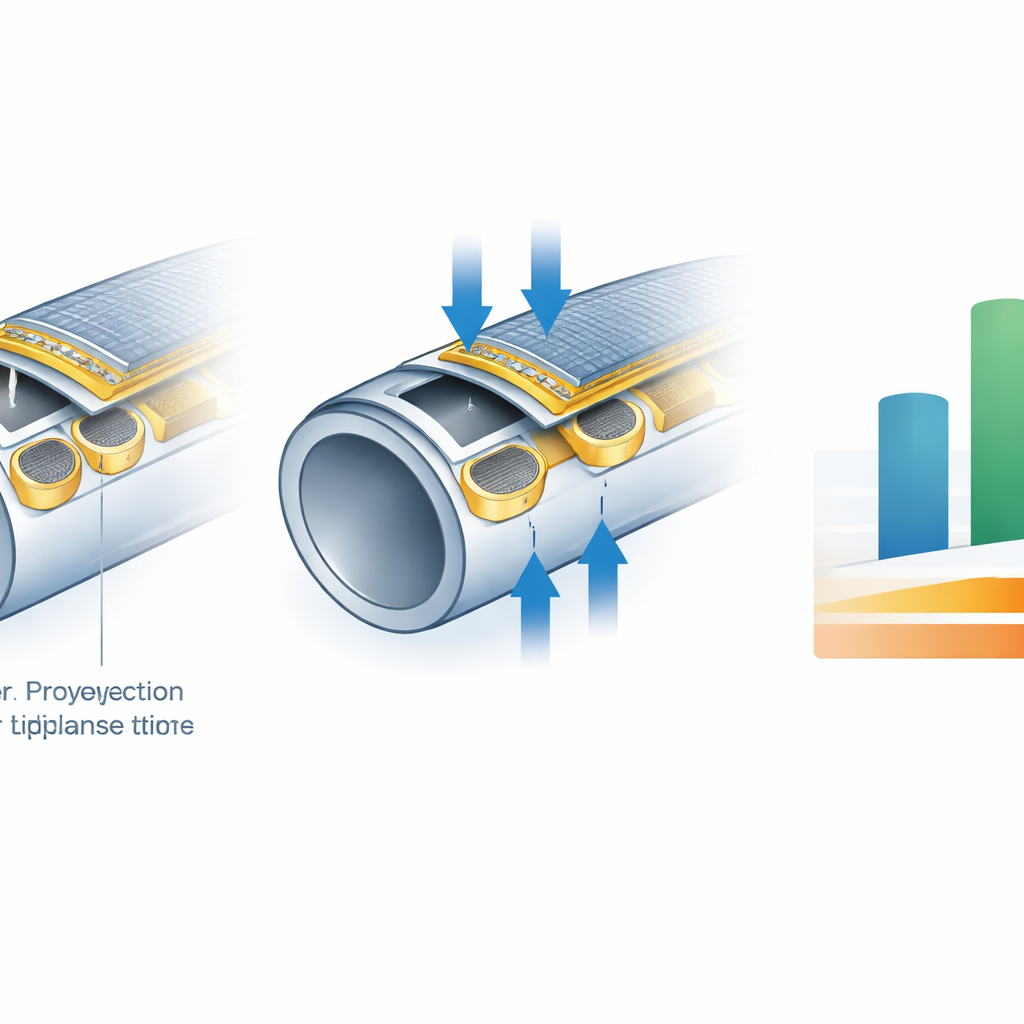
The device is built using a cylindrical projection lithography process that can pattern electronics all the way around a tiny tube only a few hundred micrometers across—thinner than a millimeter. By carving the cavities into the catheter wall instead of stacking extra layers on top, the team preserves a slim profile, adding only about 15 micrometers of thickness. This keeps the inner channel of the catheter completely open for standard tasks such as delivering drugs or light for imaging. Tests show that the sensor’s output remains stable whether the catheter is straight or bent, and that it can undergo many pressure cycles without fatigue. The same fabrication strategy works on catheters of different diameters, suggesting it could be adapted to a variety of interventional tools.
From Lab Bench to Living Arteries
After confirming performance in air, the researchers immersed the catheter in water to mimic conditions inside blood vessels. The sensor continued to track changing pressures linearly, though with slightly reduced sensitivity due to the near‑incompressibility of liquids. The decisive test came in live rats: the team inserted the CIPS into the abdominal aorta through a standard indwelling needle, then recorded the rhythmic pressure pulses produced by the animal’s heartbeat. The device delivered clear, repeatable signals over many cycles, marking the first demonstration of a suspended‑graphene pressure sensor operating inside a living blood vessel. While longer‑term implants will require additional surface treatments to resist protein buildup and clotting, these experiments show that the concept is biologically and mechanically viable.
What This Means for Future Care
In everyday terms, the authors have turned a plain catheter into a smart, ultra‑thin pressure probe by wrapping it with a skin of graphene‑based sensors and sealing it in soft, body‑friendly materials. The result is a tool that can sit inside an artery, follow its natural curves, and report detailed blood pressure changes in real time without bulky external tubing. If translated to clinical practice, this technology could lead to more precise and less invasive monitoring during surgery and intensive care, and it opens the door to catheters that combine multiple sensing and treatment functions on a single tiny platform.
Citation: Ye, F., Hou, J., Li, X. et al. A cylindrical projection lithography-fabricated flexible on-catheter in situ integrated sensor for continuous in-artery blood pressure monitoring. Microsyst Nanoeng 12, 126 (2026). https://doi.org/10.1038/s41378-026-01242-z
Keywords: intravascular blood pressure monitoring, graphene pressure sensor, flexible catheter sensor, microelectromechanical systems, continuous hemodynamic monitoring