Clear Sky Science · en
Single-cell impedance sensing on integrated circuit chip for fast tumor diagnosis
Why Faster Tumor Checks Matter
When surgeons remove a suspicious lump, they often have to decide on the spot how much tissue to cut out. If they remove too little, dangerous cancer cells can be left behind. If they remove too much, patients can lose healthy organ tissue they might have needed. Today’s standard lab tests are slow and complex, so doctors usually cannot get a clear answer while the patient is still in the operating room. This study presents a new chip-based test that reads tiny electrical signals from single cells to quickly gauge whether a tumor is likely benign or malignant during surgery.
Limits of Today’s Tumor Tests
Doctors now rely on scans, blood markers, and microscopic examination of tissue to diagnose cancer. Imaging tools such as ultrasound, CT, MRI, and PET can miss very small tumors, and blood markers often rise only when disease is advanced. The most trusted method involves fixing, slicing, and staining tissue, which usually takes about a week. A faster option called frozen section can give a preliminary answer in about an hour, but it is technically demanding, less accurate, and still needs skilled pathologists and careful sample handling. New optical and mass spectrometry tools can speed things up, but they require expensive equipment and complex workflows, which limits how widely they can be used.
Reading Cells by Their Electrical Fingerprint
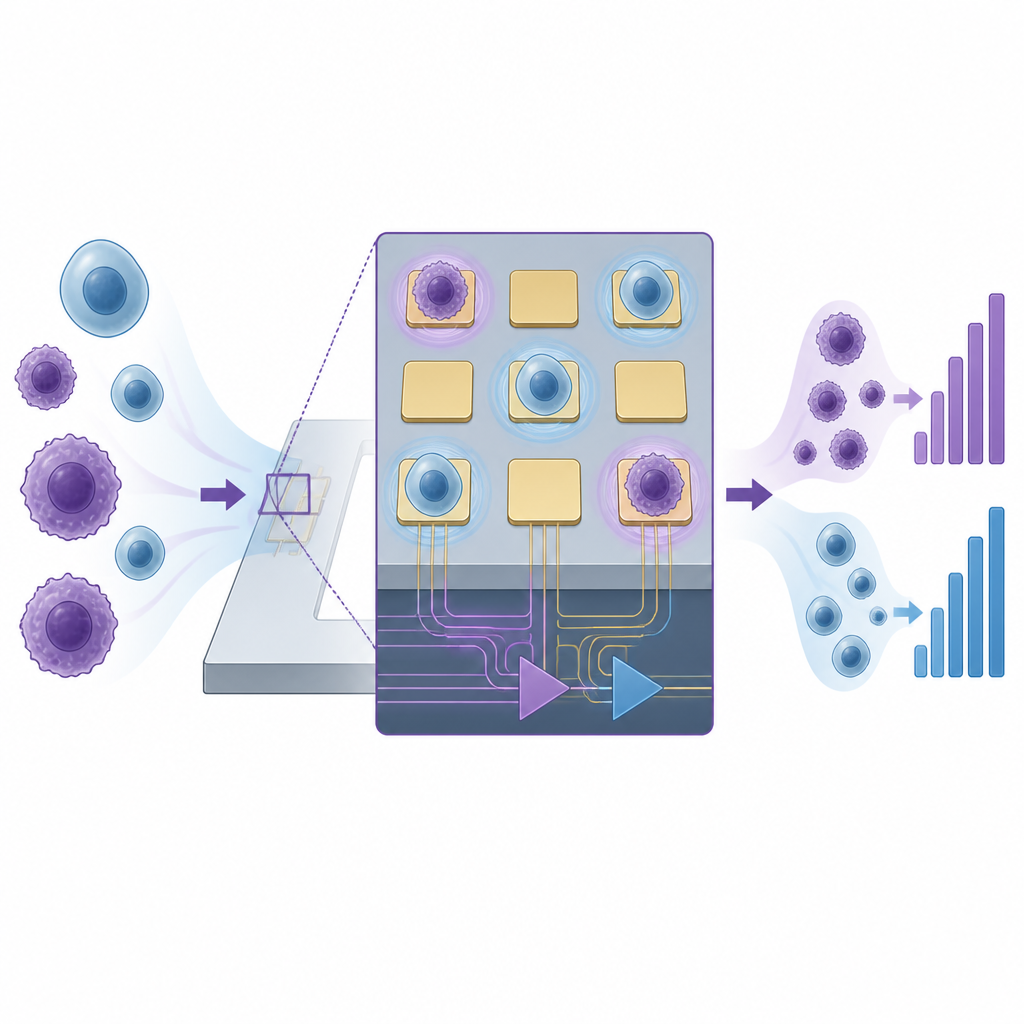
The team built on a method known as electric impedance sensing, which measures how easily an electrical signal passes through cells sitting on tiny electrodes. Cancer cells often differ from normal cells in size, membrane charge, and how they stick to surfaces. These differences change the electrical impedance measured at the cell–electrode contact. Traditional systems need large numbers of cells and long wires to external instruments, which introduce noise and blur the signals from individual cells. To solve this, the researchers placed the sensing electrodes and the readout electronics together on the same semiconductor chip, so that ultra-weak signals from single cells could be captured with high clarity.
A Low-Cost Chip Factory for Cell Sensing
To make the new test practical, the group also had to manufacture large numbers of these tiny sensor chips cheaply. They used a technique called polymer-embedded silicon fan-out to mount many integrated circuits into etched slots on a silicon wafer, then coated and patterned them together. Very small platinum electrodes were formed on each chip, just big enough to hold single cells. On a standard four-inch wafer, more than two thousand chips can be processed in one batch. This approach keeps the cost of post-processing below one dollar per chip, opening the door to disposable sensor arrays that can be used directly in the clinic without the need for careful cleaning or reuse.
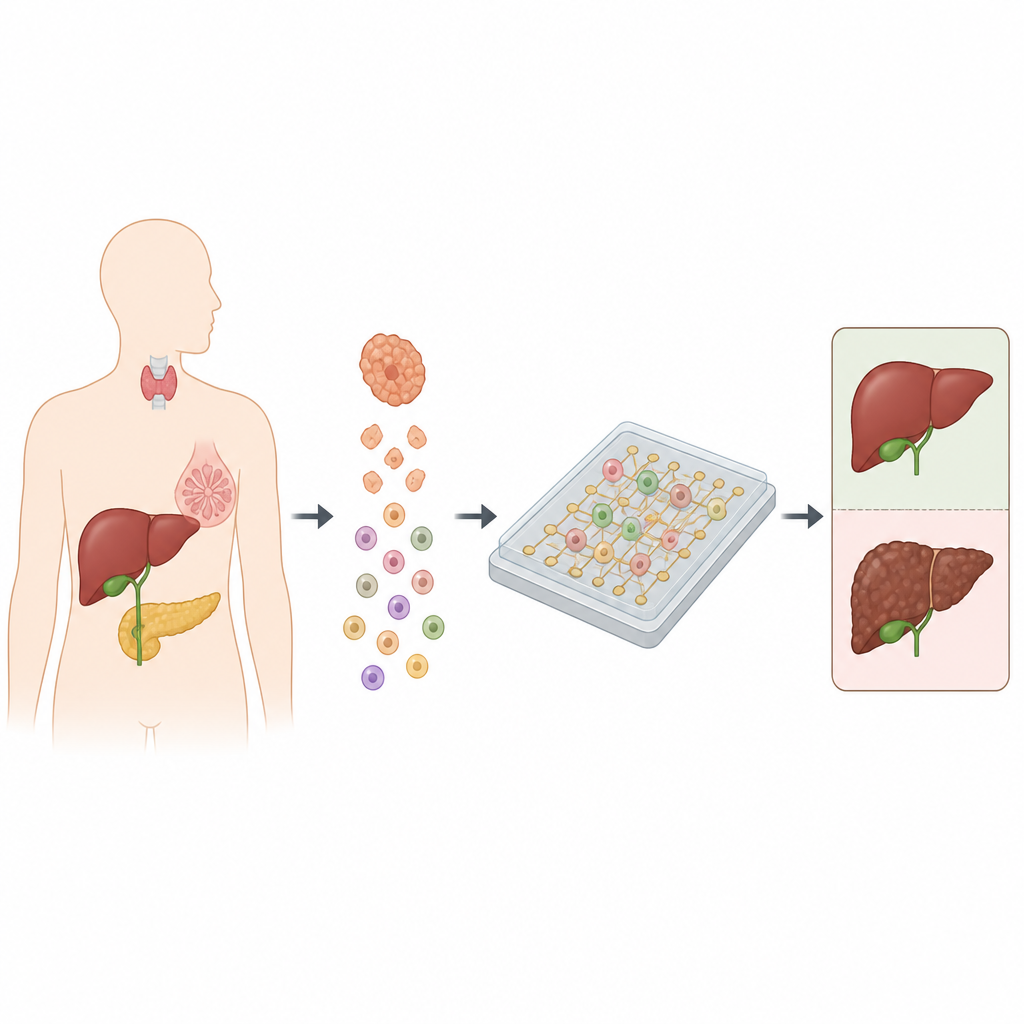
From Tissue Sample to Cancer Risk Score
In use, a small piece of tumor is first broken down into a suspension of single cells. These cells are then loaded onto the chip, where individual cells randomly land on the microelectrodes. The system sends a gentle alternating signal through the electrodes and records the impedance for each cell. Cancer cells show consistently higher impedance than non-cancerous cells, including normal tissue cells and immune cells. Instead of judging each single cell in isolation, the method looks at the overall spread of impedance values and counts how many cells fall above a threshold derived from normal tissue. The fraction of high-impedance cells is then translated into a simple risk level: low, medium, or high likelihood that the tumor is malignant.
Testing Real Tumors Across Organs
The researchers tested their platform on cell lines to confirm it could separate gastric cancer cells from normal stomach cells, and achieved about 80 percent accuracy at the single-cell level. They then moved to clinical samples from patients with tumors in the thyroid, liver, bile duct, breast, gallbladder, and pancreas. For each patient, cells from the tumor and from nearby normal tissue were measured on the chip. Tumors where more than 40 percent of cells showed abnormal impedance were classified as high risk and were later confirmed as malignant by standard pathology. Tumors with very few abnormal cells were judged low risk and matched benign findings. In liver cancer, the share of high-impedance cells closely matched the proportion of cells carrying a known liver cancer marker measured separately by flow cytometry, further supporting the method’s reliability.
What This Means for Patients and Surgeons
The study shows that a small, inexpensive chip can quickly read the electrical behavior of thousands of single cells to estimate whether a tumor is likely benign or malignant. The full process, from tissue sampling to risk readout, can be completed in about twenty minutes, fast enough to guide choices made while a patient is still in the operating room. Although further work is needed to refine cell positioning, reduce costs at larger scale, and improve long-term handling of live cells on chips, this approach points toward compact tools that can bring sophisticated tumor analysis directly into the surgical suite and help tailor treatment to each patient in real time.
Citation: Hui, W., Chen, L., Andaluz, S. et al. Single-cell impedance sensing on integrated circuit chip for fast tumor diagnosis. Microsyst Nanoeng 12, 173 (2026). https://doi.org/10.1038/s41378-026-01229-w
Keywords: tumor diagnosis, single-cell analysis, impedance sensing, integrated circuit chip, intraoperative testing