Clear Sky Science · en
Targeting of ibrutinib resistance–driving pathways by miR-28 in ABC-DLBCL
Stopping Cancer’s Comeback
Many modern cancer drugs work well at first but lose power as tumors evolve ways to escape. This study looks at a stubborn form of blood cancer called diffuse large B‑cell lymphoma, focusing on a hard‑to‑treat subtype and a widely used drug, ibrutinib. The researchers ask a simple but urgent question: instead of only chasing resistance after it appears, can we prevent resistant cancer cells from rising in the first place using a tiny RNA molecule called miR‑28?
A Tough Lymphoma and a Fading Wonder Drug
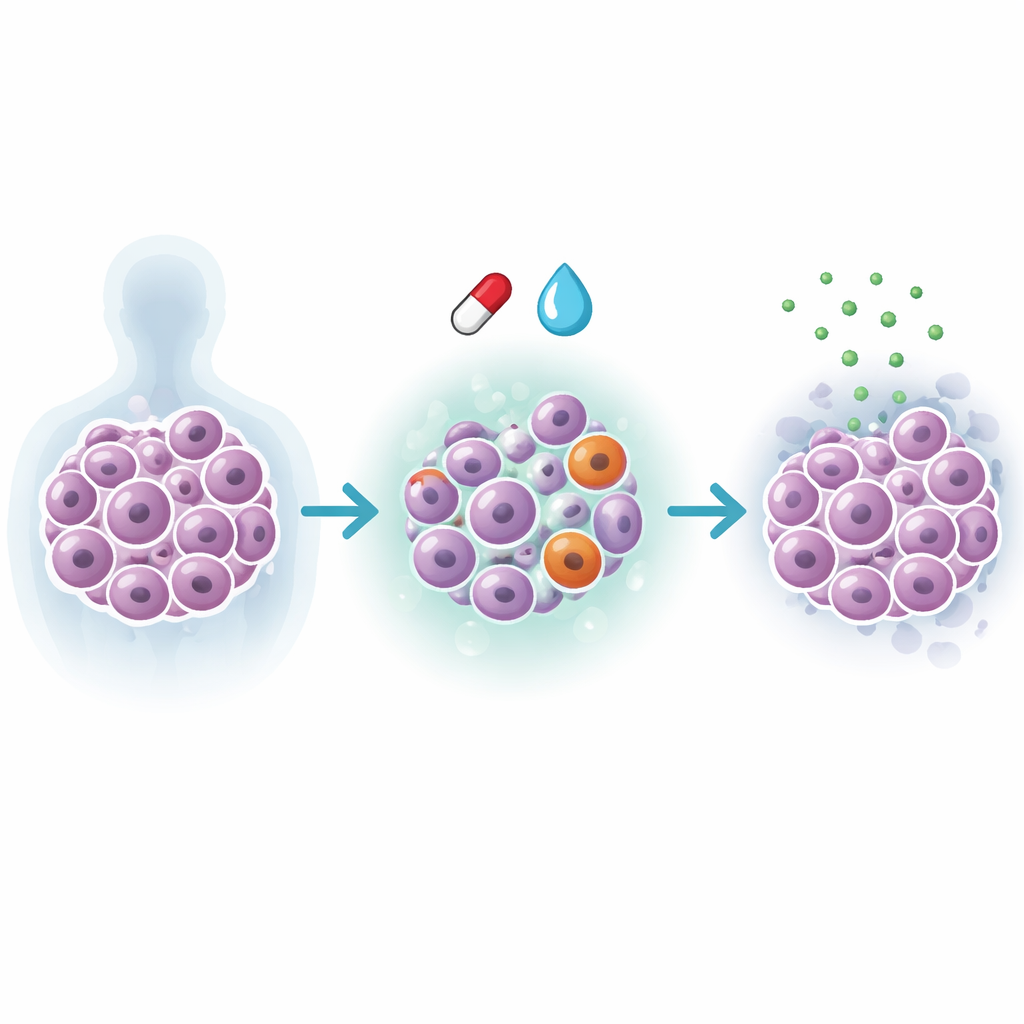
Diffuse large B‑cell lymphoma is the most common aggressive lymphoma. Standard chemo‑immunotherapy cures many patients, but those whose tumors belong to the activated B‑cell (ABC) subtype often relapse. For them, ibrutinib, a pill that blocks a key survival switch in B cells, has been a major advance. Yet its benefits are often temporary: over time, pockets of lymphoma cells adapt, survive the drug, and drive the cancer’s return. These escape routes can involve DNA mutations, but also more subtle rewiring of the cell’s control circuits and energy use that standard tests may miss.
A Tiny RNA with Big Influence
MicroRNAs are short strands of RNA that fine‑tune how hundreds of genes are used inside cells. They do not code for proteins themselves, but act more like dimmer switches on existing programs. miR‑28 is one such molecule, normally helping keep B cells in check. It is often reduced in B‑cell lymphomas, and earlier work showed that restoring it can slow tumor growth and makes lymphoma cells more vulnerable to ibrutinib. In this study, the authors asked whether constant miR‑28 activity could actually block the rise of ibrutinib‑resistant clones in ABC‑type lymphoma.
Watching Cancer Clones Compete
To follow how resistance emerges, the team mixed lymphoma cells that could turn on miR‑28 with control cells and grew them together under slowly increasing doses of ibrutinib. Using colored fluorescent tags and flow cytometry, they tracked how different clones waxed and waned over several weeks. In control cultures, a small fraction of cells adapted to the rising drug levels, expanded, and came to dominate — a laboratory replay of relapse in the clinic. When miR‑28 was switched on, this clonal takeover was blunted: resistant‑like clones appeared less often and overall diversity of the population stayed higher, showing that miR‑28 was actively interfering with the selection of drug‑tolerant winners.
Disrupting the Tumor’s Energy and Growth Circuits
To understand how miR‑28 exerts this effect, the researchers compared gene activity in sensitive cells, emerging resistant cells, and cells expressing miR‑28, all collected midway through the resistance‑building process. Cells on the path to resistance had cranked up programs linked to mitochondria — the cell’s power plants — and to the mTOR pathway, a central controller of growth and protein production. miR‑28 pushed these same programs in the opposite direction, dialing down many of the genes and pathways that resistant cells depend on. Direct measurements confirmed that miR‑28‑bearing cells had fewer mitochondria, made less mitochondrial energy, and showed reduced mTOR activity. In patient data from the PHOENIX clinical trial, tumors whose gene patterns resembled this miR‑28‑driven state were linked to better survival in older patients receiving ibrutinib, suggesting that the same circuitry matters in real cancers.
Turning miR‑28 into a Targeted Medicine
Finally, the team tested whether adding miR‑28 from the outside could slow established ibrutinib‑resistant tumors grown in mice. Direct injections of synthetic miR‑28 into resistant lymphomas shrank tumors, with stronger effects in resistant cells than in their original, drug‑naïve counterparts. To move closer to a practical therapy, they attached miR‑28 mimics to tiny gold nanoparticles decorated with aptamers — short DNA‑like strands that recognize surface markers on lymphoma cells. These targeted particles, delivered either into the tumor or through the bloodstream, homed to resistant tumors and curbed their growth across several lymphoma models, while control particles had little effect.
What This Could Mean for Patients
In plain terms, this work shows that miR‑28 can both prevent and attack ibrutinib‑resistant lymphoma by cutting off the energy and growth programs that resistant cells rely on. Instead of waiting for cancer to adapt and then trying to hit each new escape route, miR‑28 acts more broadly, nudging many genes at once to make it harder for resistance to take hold. Coupled with smart delivery vehicles such as aptamer‑guided nanoparticles, miR‑28 or similar microRNA‑based strategies could one day be added to existing treatments to keep powerful drugs like ibrutinib working longer in patients with high‑risk lymphomas.
Citation: Álvarez-Corrales, E., Moreno-Palomares, R., Gómez-Escolar, C. et al. Targeting of ibrutinib resistance–driving pathways by miR-28 in ABC-DLBCL. Leukemia 40, 894–905 (2026). https://doi.org/10.1038/s41375-026-02948-9
Keywords: diffuse large B-cell lymphoma, drug resistance, ibrutinib, microRNA-28, targeted nanoparticles