Clear Sky Science · en
Evolving therapeutic strategies in mantle cell lymphoma: advancements and future directions
Why this cancer story matters
Mantle cell lymphoma is a rare form of blood cancer that used to carry a grim outlook, with many patients surviving only a few years after diagnosis. In the last decade, however, a wave of new precision drugs and immune-based treatments has begun to change that picture. This review article explains how doctors are moving away from one-size-fits-all chemotherapy toward smarter, more tailored strategies that can keep the disease in check for longer and with fewer side effects. Even for readers without a medical background, it offers a window into how modern cancer care is becoming more targeted, more personal, and more hopeful.
Understanding a complex blood cancer
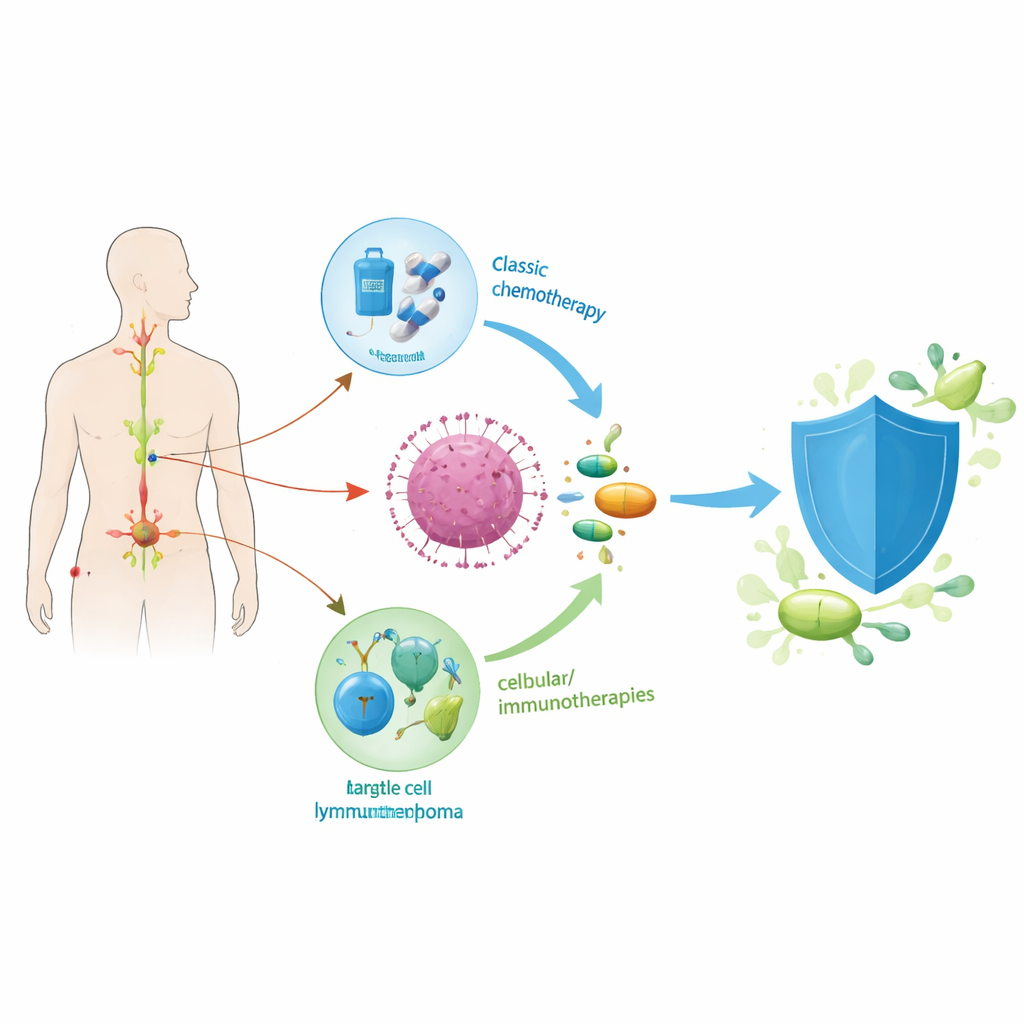
Mantle cell lymphoma arises from white blood cells called B cells, which normally help fight infections. In this disease, a key genetic glitch drives these cells to grow out of control and spread through lymph nodes, bone marrow, and sometimes organs like the spleen and intestines. Doctors have learned that mantle cell lymphoma is not a single disease: in some people it behaves slowly, while in others it is fast and aggressive. To sort patients into broad risk groups, clinicians now combine simple clinical measures (such as age and blood tests), microscope features of the cancer, genetic changes, and very sensitive tests that detect tiny traces of disease after treatment. These tools help predict who is likely to relapse early and who might enjoy longer remissions.
From heavy chemotherapy to targeted pills
For many years, the mainstay of treatment was intensive chemotherapy combined with an antibody drug called rituximab, often followed by a stem cell transplant in younger, fit patients. While this approach could produce deep remissions, it involved long hospital stays and serious side effects, and its benefits appeared to shrink once newer drugs were introduced. Large trials have now shown that adding a pill called a Bruton’s tyrosine kinase (BTK) inhibitor to standard regimens improves how long patients stay free of disease, and that in some cases the pill matters more than the transplant itself. In older patients who cannot tolerate very harsh treatment, combining BTK inhibitors with gentler chemotherapy has extended remissions with a more acceptable safety profile, marking a shift away from chemotherapy alone.
Building chemo-free and low-chemo approaches
A major theme of the article is the rise of “chemotherapy-free” combinations. These regimens pair immune-boosting antibodies with pills that unmask cancer cells to the immune system or block their survival signals. Early studies of such combinations—including two- and three-drug cocktails built around BTK inhibitors, venetoclax (which targets a survival protein), and immune-modulating tablets—have shown very high response rates and frequent deep clean-up of residual disease, even in patients with worrisome genetic markers like TP53 mutations. Some programs are exploring short courses of targeted therapy followed by a single infusion of engineered immune cells, with the aim of achieving long remissions without years of ongoing treatment. Although follow-up is still relatively short, these strategies hint at a future where many patients can avoid traditional chemotherapy altogether.
New hope after relapse
Despite progress, many people with mantle cell lymphoma still see their cancer return, especially after exposure to first-generation BTK inhibitors. The review details how options have broadened for this difficult group. A newer, more flexible BTK blocker called pirtobrutinib can work even when earlier BTK drugs fail and tends to cause fewer heart and bleeding problems. The most dramatic advances, however, come from chimeric antigen receptor (CAR) T-cell therapies, in which a patient’s own T cells are engineered to recognize and attack lymphoma cells. In heavily pretreated patients, CAR T cells have produced rapid and often complete remissions, including in those with high-risk disease, though side effects like fever, confusion, and infections require careful management. For patients who cannot receive CAR T cells, emerging “off-the-shelf” antibody drugs that drag the body’s T cells directly to cancer cells, as well as antibody–drug conjugates that deliver chemotherapy payloads precisely to tumor cells, are showing promise in early trials.
Looking ahead to more personalized care
The authors conclude that mantle cell lymphoma is moving from a uniformly hard-to-treat cancer toward a condition where many patients can expect longer and better-quality lives. The key drivers are smarter drug combinations, earlier use of immune-based therapies, and more refined risk tools that indicate who needs which treatment and when. At the same time, they stress that access and long-term follow-up remain major challenges: most of the newest therapies are expensive and not yet widely available, and doctors still need to learn how best to sequence them over a patient’s lifetime. For lay readers, the take-home message is that while mantle cell lymphoma remains serious, the treatment playbook is expanding fast, turning what was once a short, rigid path into a more flexible, personalized roadmap built around durable control and quality of life.
Citation: Tavarozzi, R., Maher, N., Catania, G. et al. Evolving therapeutic strategies in mantle cell lymphoma: advancements and future directions. Leukemia 40, 857–871 (2026). https://doi.org/10.1038/s41375-026-02942-1
Keywords: mantle cell lymphoma, targeted therapy, CAR T cells, BTK inhibitors, bispecific antibodies