Clear Sky Science · en
Diagnoses of pulmonary embolism from non-contrast 4DCT using image processing-derived quantitative perfusion scores
Why spotting lung clots faster matters
Pulmonary embolism—blood clots that suddenly block vessels in the lungs—can be deadly within hours, yet its symptoms often mimic far more routine illnesses. The current gold-standard scan to find these clots requires an injected dye that some patients cannot safely receive. This study explores a new way to detect dangerous clots using only standard, non-contrast CT scans taken while a person breathes in and out, potentially opening clot diagnosis to many more patients and speeding decisions in busy emergency departments. 
A common scan with hidden extra information
Today, most patients with suspected pulmonary embolism receive a CT pulmonary angiography scan, which uses an iodine-based dye to highlight blood vessels in the lungs. This test is fast and accurate but carries downsides: allergic reactions to the dye, added risk to people with fragile kidneys, and extra radiation to the chest—especially concerning for younger patients. Alternatives such as nuclear medicine scans or magnetic resonance imaging can work well but are slower, less available around the clock, and often require specialized facilities. Meanwhile, many hospitals already perform four-dimensional CT (4DCT) scans, which are simply a series of regular lung CT images collected as a patient breathes. The authors asked whether these routine, non-contrast images might quietly contain enough information about lung blood flow to diagnose clots without dye.
Listening to blood flow through breathing motion
When a clot blocks a lung artery, the region of lung beyond the blockage receives much less blood. The team built on earlier work showing that by carefully measuring how the apparent “mass” of lung tissue changes between inhale and exhale CT images, one can estimate how much blood is flowing through each region—a quantity known as perfusion. Using image-processing tools and an automated lung-lobe segmentation network, they divided each lung into its five anatomical lobes and calculated how much the mass in each lobe changed between breathing phases. Smaller changes corresponded to poorer blood flow. To make these results clinically usable, the researchers transformed these continuous measurements into a simple perfusion “score” per lobe. 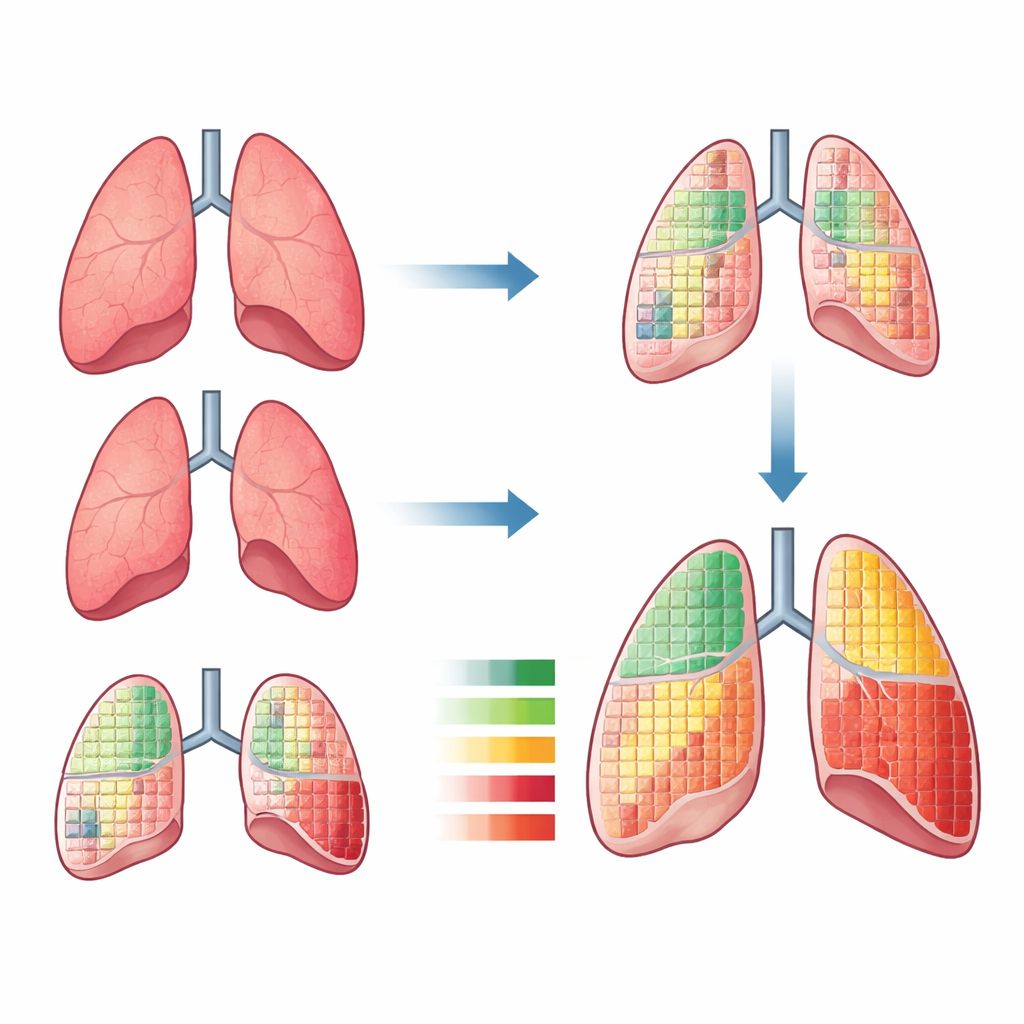
Turning complex images into a simple score
The study included 123 emergency patients who all had the usual dye-based CT angiography plus a non-contrast 4DCT scan within 48 hours. Radiologist readings of the dye-based scans served as the ground truth for who truly had a pulmonary embolism. For each patient’s five lung lobes, the authors searched for numerical cut-off values that best separated lobes with healthy blood flow from those with suspected perfusion deficits. Each lobe below its cut-off was marked as “low-functioning,” and these five binary flags were simply added up to create a diagnostic score between 0 and 5. In this scheme, scores below 2 indicated no embolism, scores above 2 indicated embolism, and a score of exactly 2 was considered inconclusive. Using a leave-one-out validation approach—testing each patient with thresholds learned from all the others—the model correctly classified cases with 72% accuracy, 75% sensitivity (catching most true embolisms), and 69% specificity (correctly ruling out most non-embolism cases) when inconclusive results were allowed.
What the lobe patterns reveal
Beyond the overall score, the team examined which lung lobes tended to show low perfusion in patients with clots. On average, four of the five lobes had clearly lower perfusion values in embolism patients than in those without clots, reinforcing that the method captures real physiological changes. Certain patterns—specific combinations of affected lobes—appeared only in embolism-positive patients, while others were found only in embolism-negative patients. Interestingly, one lobe did not differ much between the two groups, and low perfusion there alone often signaled a false alarm. These insights suggest that future models might weigh different lobes unequally or exploit these spatial patterns to further refine predictions, especially once larger and more varied datasets become available.
Promise and next steps for safer clot detection
To a non-specialist, the bottom line is that this work shows it is possible to detect signs of pulmonary embolism using only non-contrast CT scans and mathematics, without injected dye or black-box artificial intelligence. The method distills rich 4D lung images into a straightforward lobe-based score that physicians can interpret and that can also return an honest “I am not sure” when the evidence is borderline. While the pilot study is modest in size and limited by image artifacts, the encouraging sensitivity and specificity suggest that, with refinement and validation on larger breath-hold CT datasets, this approach could evolve into a practical, rapid tool to flag dangerous lung clots in patients who currently have few safe imaging options.
Citation: Kuo, HT., Liu, YK., Chaki, D. et al. Diagnoses of pulmonary embolism from non-contrast 4DCT using image processing-derived quantitative perfusion scores. npj Biomed. Innov. 3, 29 (2026). https://doi.org/10.1038/s44385-026-00065-x
Keywords: pulmonary embolism, lung perfusion, non-contrast CT, 4DCT imaging, emergency diagnosis