Clear Sky Science · en
Multimodal assessment of arterial stiffness using photoplethysmography and laser Doppler flowmetry
Why the Flexibility of Your Arteries Matters
As we grow older, our arteries gradually stiffen, making it harder for blood to move smoothly through the body. This age-related change, called arterial stiffness, is closely tied to heart attacks, strokes and other cardiovascular troubles. Yet today, spotting early warning signs often requires a hospital visit and specialized equipment. This study explores whether two simple light-based techniques, already common in medical devices, could be combined to create a quick, low-cost check of artery health that might one day be done in a family doctor’s office or even with wearable gadgets. 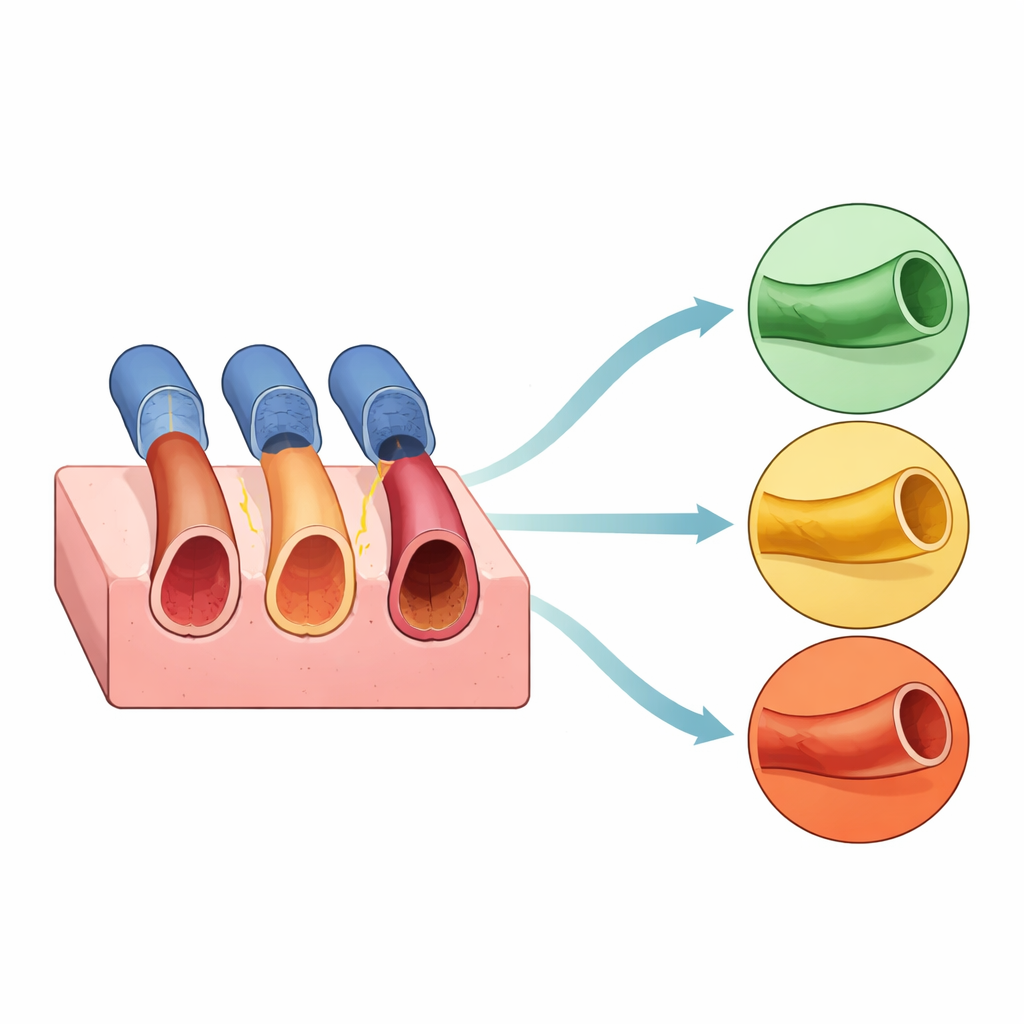
Shining Light on Blood and Vessel Health
The researchers focused on two optical methods that do not break the skin. The first, photoplethysmography (PPG), is already found in smartwatches and fingertip clips that track pulse and blood oxygen. It shines light into the skin and measures how much is reflected back, which changes with each heartbeat as blood volume in small vessels rises and falls. The second, laser Doppler flowmetry (LDF), uses a low-power laser to sense how quickly red blood cells are moving, offering a window onto blood flow in tiny vessels. Because stiff arteries expand less and can disrupt normal flow patterns, the team reasoned that carefully analyzing these two signals together might reveal how “old” or “young” a vessel is, even before symptoms appear.
Building Fake Arteries to Test the Idea
To test this safely and precisely, the scientists did not start with patients. Instead, they built realistic models of human leg arteries in the lab. Each model consisted of a soft block of material with an embedded tube representing a femoral artery. Three versions were made: one “healthy” and elastic, one clearly “unhealthy” and stiff, and one in between. These tubes were filled with specially prepared blood-mimicking fluids containing tiny particles that scatter light in controlled ways, allowing the team to study how different optical recipes affect the signals. They then circulated the fluids using a pump that mimicked a 60–beat-per-minute heartbeat and recorded four-minute segments of PPG and LDF data from each artificial artery. 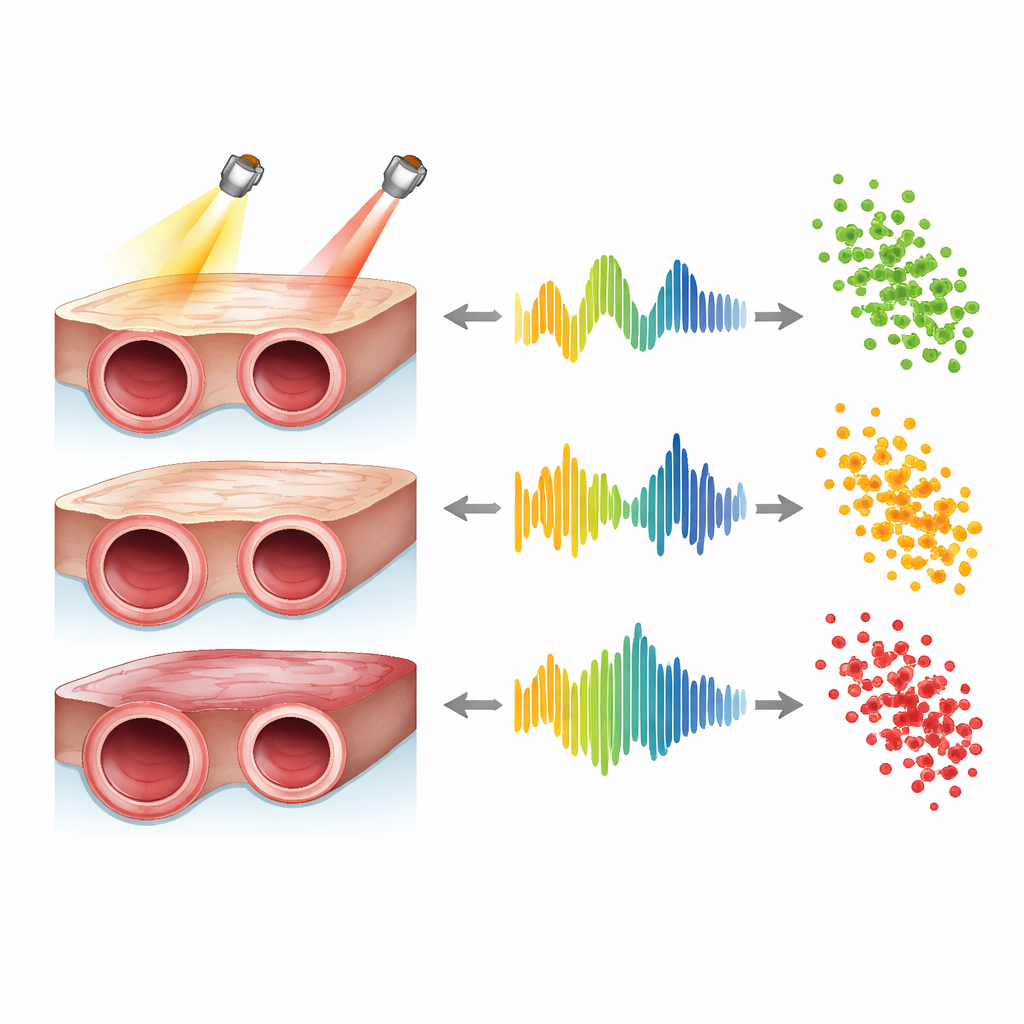
What the Light Signals Revealed
From the PPG recordings, the team extracted several features that describe each pulse wave, such as how tall it is (amplitude), how much area it covers, and how sharply it rises and falls. As expected, signals from stiffer “arteries” showed smaller, weaker pulsations than those from the more elastic model, reflecting the reduced ability of a stiff wall to expand. The laser measurements told a complementary story: as stiffness increased, the average flow signal, known as flux, dropped steadily. This matched basic fluid physics, which predicts that narrower, less flexible tubes offer more resistance and thus carry less flow. One formulation of the blood-mimicking fluid, based on a substance called intralipid, especially sharpened the differences in both volume and flow signals between healthy and diseased states, although it made one of the PPG colors harder to read.
Combining Two Views for Clearer Answers
The crucial test was whether these measurements could not only show trends but also reliably sort the three artery types. Using machine-learning algorithms, the researchers trained computer models to classify each recording as healthy, intermediate or unhealthy based on the extracted features. PPG alone, especially using red and green light, already performed well. However, when they added the LDF flow information, accuracy improved further, in some cases correctly identifying all samples in the held-out test data. This suggests that volume and flow together provide a richer fingerprint of vessel stiffness than either alone, and that subtle intermediate stages—those most important for early intervention—may be easier to detect with a multimodal approach.
From Lab Bench to Doctor’s Office
In simple terms, the study shows that gently shining light and laser beams on a vessel can reveal how supple or rigid it is, and that combining these two views makes the assessment more reliable. While these experiments were done in carefully controlled artificial models rather than in people, the results demonstrate that the technology is technically feasible and sensitive to changes in arterial stiffness. The authors argue that with further refinement, validation in volunteers and patients, and packaging into compact sensors, this dual-technique approach could evolve into a practical tool for front-line clinics. That could enable earlier detection of “ageing” arteries, better targeting of lifestyle and drug treatments, and fewer people progressing silently toward serious heart and circulation disease.
Citation: Karimpour, P., Ferizoli, R., May, J.M. et al. Multimodal assessment of arterial stiffness using photoplethysmography and laser Doppler flowmetry. npj Cardiovasc Health 3, 19 (2026). https://doi.org/10.1038/s44325-026-00115-8
Keywords: arterial stiffness, photoplethysmography, laser Doppler flowmetry, vascular ageing, noninvasive cardiovascular screening