Clear Sky Science · en
Percutaneous nephrostomy guidance by a convolutional-neural-network-based optical coherence tomography endoscope
Why safer kidney access matters
Kidney stone disease is becoming more common, and many patients need a small tube placed directly into the kidney to drain urine or remove stones. This procedure, called percutaneous nephrostomy, is done by guiding a needle from a patient’s back into the hollow center of the kidney. Although the puncture is tiny, choosing the wrong path can tear delicate kidney structures or damage blood vessels, leading to bleeding and other complications. This study introduces a new high‑resolution imaging probe, paired with artificial intelligence, that rides inside the needle tip to help doctors see exactly where they are going and avoid harm.
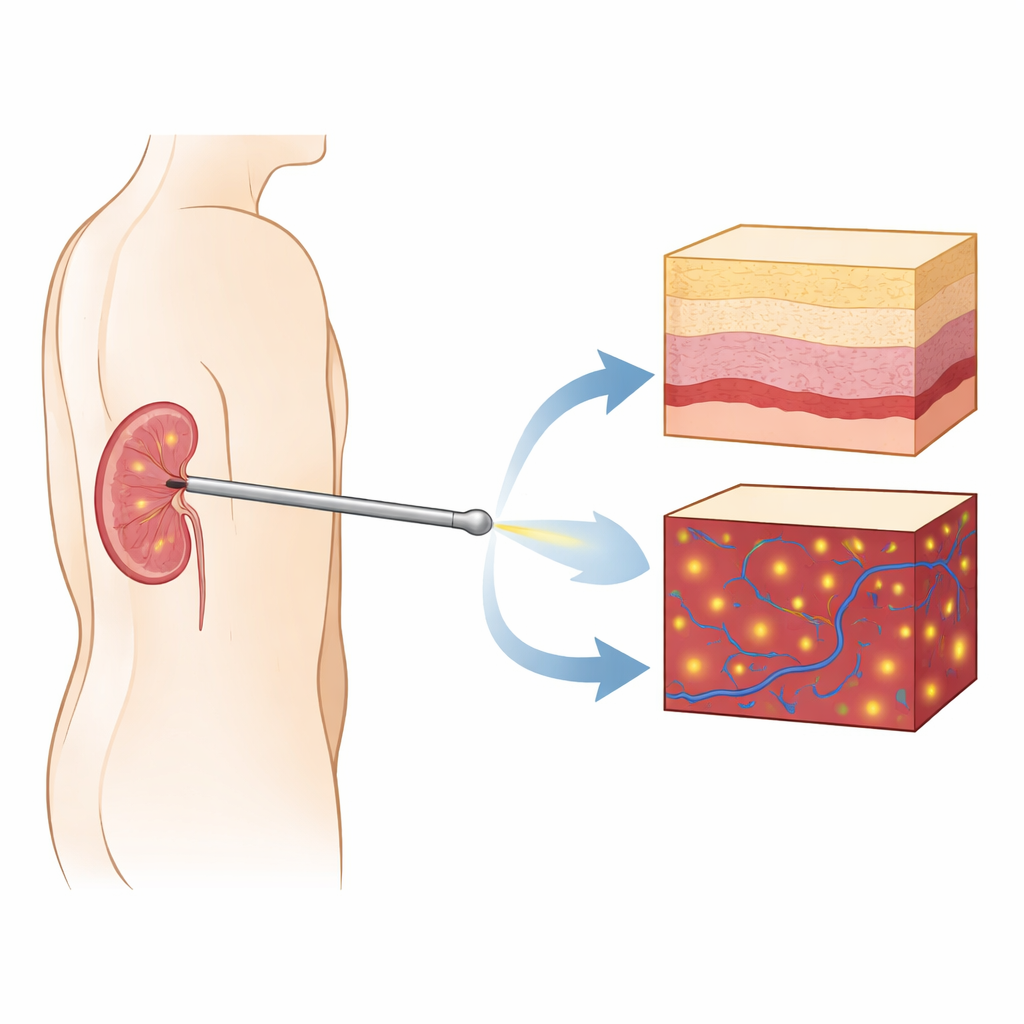
A tiny camera for inside the needle
The researchers built a forward‑looking imaging probe based on optical coherence tomography (OCT), a light‑based method that can capture cross‑sectional “slices” of tissue at micrometer resolution—about ten times finer than standard medical ultrasound. They embedded a thin gradient‑index lens inside a standard nephrostomy needle so that, during insertion, the probe can look directly ahead into the kidney. Unlike regular endoscopes that mainly show surface views, this system provides depth‑resolved images, revealing how tissue structure changes beneath the tip. The same probe can also run in a Doppler mode, which highlights moving red blood cells and thus reveals blood vessels in front of the needle before they are pierced.
Recognizing kidney layers in real time
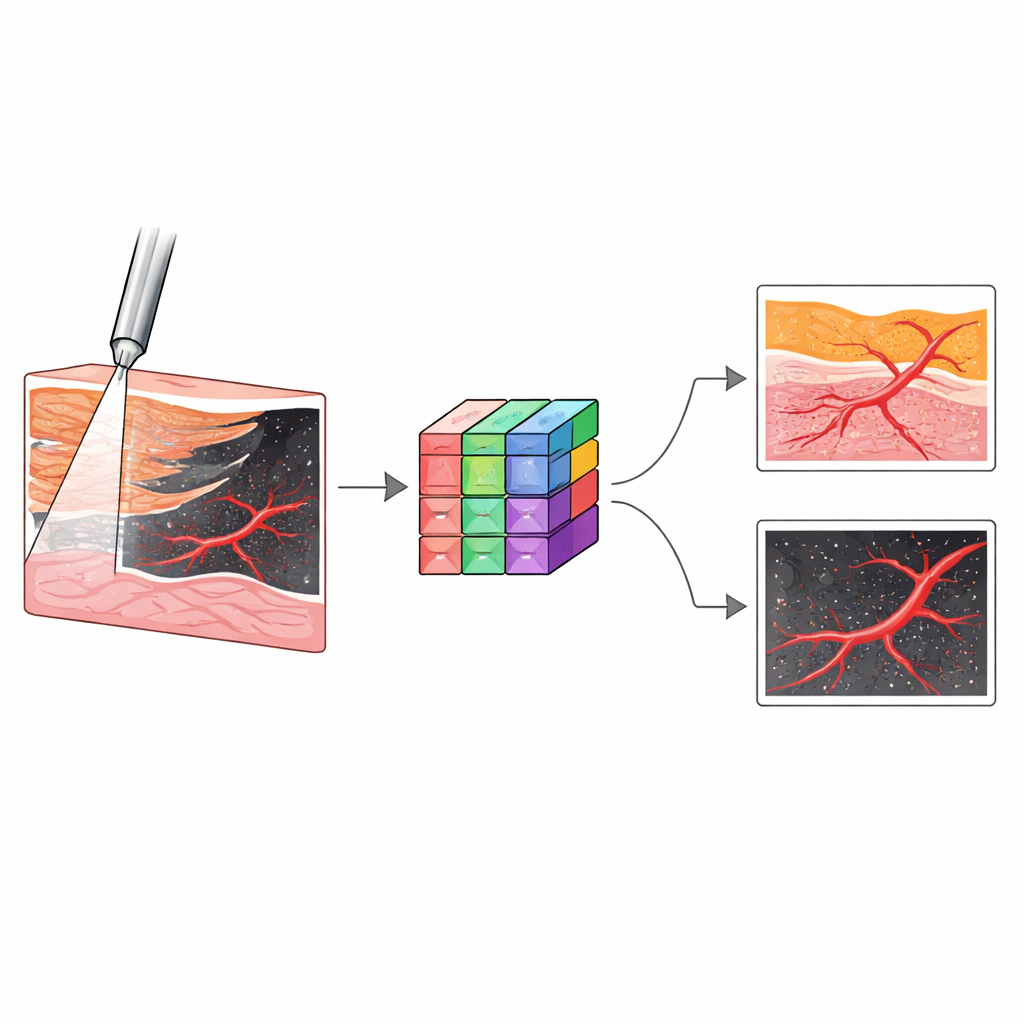
To test whether the system could tell different kidney tissues apart, the team performed experiments on 31 donated human kidneys kept under near‑normal conditions. In real procedures, the needle should pass through the outer cortex and inner medulla, then enter a cup‑like region called the calyx and finally emerge into the central urine‑collecting pelvis. Straying off course risks passing through fatty spaces between structures and tearing thin walls. The researchers systematically touched the probe to five tissue types—cortex, medulla, calyx, sinus fat, and pelvis—and captured millions of OCT images showing their distinctive patterns. For example, cortex and medulla looked smooth but differed in depth, calyx showed stripe‑like transitions, sinus fat produced bright speckled networks, and the pelvis appeared as an empty space beneath the probe.
Teaching a smart system to spot danger
Because human experts would need time and training to interpret these new images during an operation, the team turned to deep learning. They trained several convolutional neural networks to classify each OCT frame into one of the five tissue types, then selected an architecture called Inception as the best performer. In internal tests, this model correctly identified tissues with an accuracy of about 99.6%, and it retained high performance on additional kidneys it had never seen before. In a separate task, they used another neural network design, nnU‑Net, to outline blood vessels in Doppler OCT images. This model learned to distinguish flowing blood from the background tissue with very high overlap to expert hand‑drawn labels, even for vessels smaller than 0.2 millimeters across that are difficult to see with standard tools.
How it compares with today’s tools
Currently, doctors usually rely on ultrasound or X‑ray–based fluoroscopy to guide nephrostomy needles. These techniques show the overall position of the kidney and the general path of the needle, but their relatively coarse resolution makes it hard to know exactly which tissue sits at the tip, or how close a blood vessel lies. In control experiments, experienced radiologists using structural and Doppler ultrasound struggled to identify the precise tissue at the needle tip and could not reliably visualize tiny vessels. By contrast, the OCT system offered a detailed local view plus automated analysis that runs in a fraction of a second on modern graphics processors, fast enough to give feedback as the needle advances.
What this could mean for patients
The study suggests that combining a needle‑mounted OCT probe with deep learning could make kidney access procedures both safer and more efficient. In the future, a doctor could insert the usual needle with the probe inside, watch fine‑scale images appear in real time, and rely on the software to signal when the tip has entered the right cavity or is approaching a blood vessel. Fewer puncture attempts would mean less tissue trauma, lower risk of bleeding, and potentially shorter procedures and hospital stays. Although the work was done on donated kidneys rather than living patients, it lays the groundwork for clinical systems that could also help guide other needle‑based interventions, from biopsies and anesthesia blocks to targeted drug delivery.
Citation: Wang, C., Calle, P., Yan, F. et al. Percutaneous nephrostomy guidance by a convolutional-neural-network-based optical coherence tomography endoscope. Commun Eng 5, 47 (2026). https://doi.org/10.1038/s44172-026-00613-8
Keywords: kidney stone surgery, needle guidance, optical coherence tomography, medical imaging AI, blood vessel detection