Clear Sky Science · en
Machine learning-based identification of abnormal functional connectivity in obesity across different metabolic states
Why the Brain Matters in Weight Gain
Obesity is often described in terms of calories, diets, and willpower, but this study suggests a deeper story: the wiring of the brain itself may quietly nudge some people toward overeating. By looking at how different brain regions talk to each other before and after a meal, and using powerful machine-learning tools, the researchers show that obesity is associated with a distinct pattern of weakened communication in key networks that handle food reward, self-control, and body signals. Understanding these hidden brain patterns could open the door to new treatments that target circuits rather than just scales.
How the Study Followed the Brain Through a Meal
The researchers recruited 30 women with obesity and 30 women without obesity, all between 20 and 65 years old. Participants arrived after an overnight fast and then spent four hours in the lab transitioning from hunger to fullness and back toward hunger. During this time, they drank a nutritionally controlled liquid meal and had their brain activity recorded repeatedly using electroencephalography (EEG), a noninvasive method that tracks electrical signals from the scalp. Recordings were taken at fasting, several points after the first and second halves of the meal, and up to four hours later. Blood samples for glucose and insulin and detailed measurements of body composition and eating habits were also collected to characterize each participant’s metabolic and behavioral profile.
Turning Brain Signals into Connection Maps
Instead of focusing on single brain areas, the team examined how 88 regions interacted over time, a property known as functional connectivity. They first used a technique called source localization to estimate activity inside the brain from the EEG signals, then measured how consistently pairs of regions rose and fell together in different frequency bands (such as slow delta waves or faster gamma waves). This produced thousands of potential connection features. To avoid cherry-picking, they used a data-driven machine-learning pipeline: algorithms automatically searched through this complex web to find the smallest combination of connections that best distinguished women with obesity from those without, while guarding against overfitting through careful cross-validation and label-shuffling tests.
Six Connections That Tell a Powerful Story
Remarkably, the models needed only six specific connections to identify obesity with about 95% accuracy across all metabolic states. In every case, these connections were weaker in the obese group. Several linked regions involved in sensing the body, planning movements, and evaluating rewards, but one structure stood out: the dorsal anterior cingulate cortex (dACC). This region, located near the front and middle of the brain, appeared as a central hub in high-frequency (gamma) connections to areas that process the emotional and motivational value of food, such as parts of the temporal and frontal lobes. In women without obesity, these links were strong and changed with metabolic state, reflecting flexible adjustment as one moves from hunger to satiety. In women with obesity, they remained consistently blunted, suggesting a rigid, less responsive communication channel.
What Happens When Weight Goes Down but Wiring Stays Similar
Some women with obesity were also followed through a short, intensive weight-loss program and then three months later. After weight loss, their brain connectivity patterns briefly looked more like those of the lean group, and the machine-learning model found it harder to tell them apart. Yet by three months post-diet, the old pattern largely returned, even though the weight loss was maintained. This rebound suggests that the altered connectivity is a more stable trait than the body weight itself. The findings fit with a "Bayesian brain" view in which the brain constantly predicts energy needs and compares them with bodily signals. In obesity, weakened communication between the dACC, insula, and orbitofrontal cortex may leave the brain uncertain about whether energy needs are truly met, pushing it toward a "better eat more just in case" strategy that favors ongoing cravings and overeating.
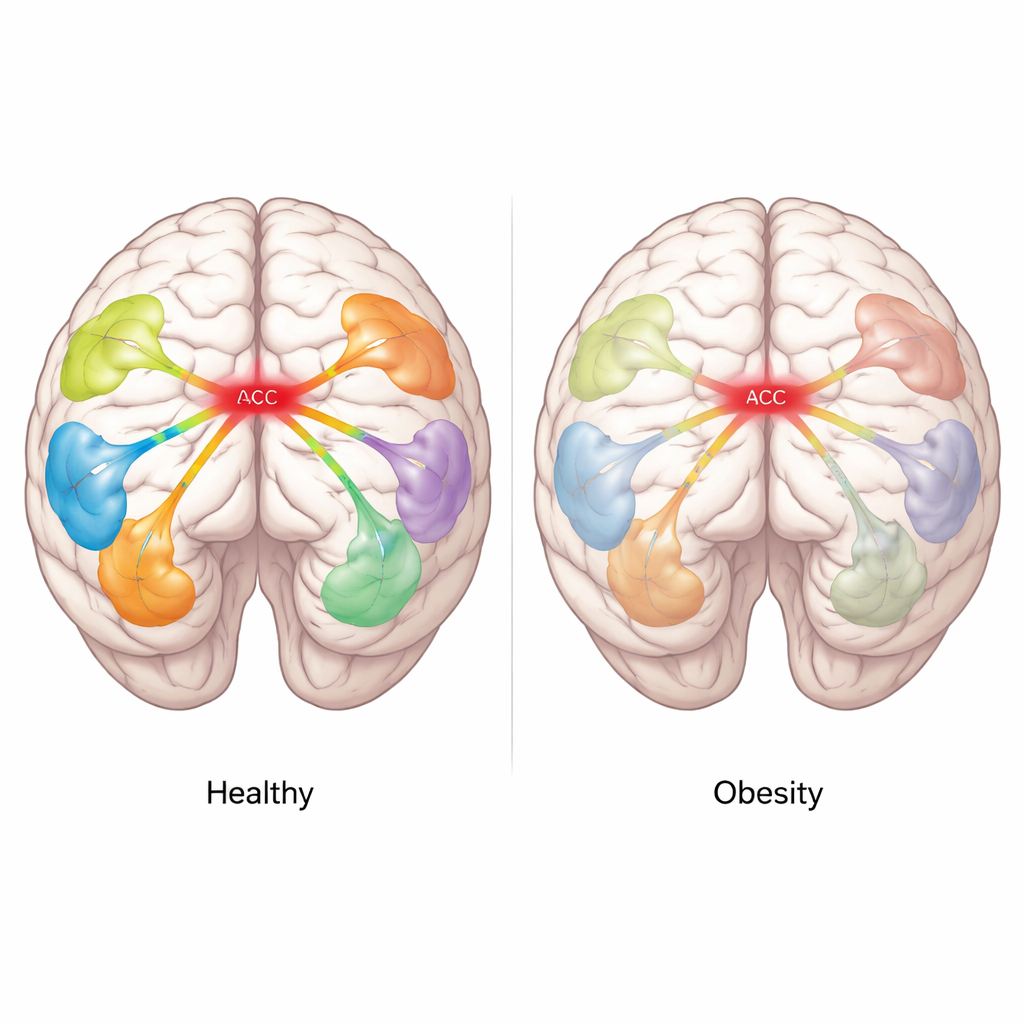
What This Means for Future Treatments
For a lay reader, the key takeaway is that obesity is not just a matter of weak willpower or simple overeating. In this study, women with obesity shared a fingerprint of disrupted brain connectivity that persisted across hunger and fullness and tended to reappear after dieting. The dACC emerged as a particularly important node, hinting that interventions aimed at restoring communication in this hub—such as carefully tuned brain stimulation or neurofeedback—might help recalibrate how the brain interprets hunger, satiety, and food reward. While more work is needed, especially in men and in people with common psychiatric conditions, this research strengthens the idea that effective obesity treatment may require rewiring thought and feeling at the brain-circuit level, not just changing what is on the plate.
Citation: Yue, Y., Manning, P., De Ridder, D. et al. Machine learning-based identification of abnormal functional connectivity in obesity across different metabolic states. Commun Med 6, 241 (2026). https://doi.org/10.1038/s43856-026-01518-5
Keywords: obesity, brain connectivity, electroencephalography, machine learning, food reward