Clear Sky Science · en
Early-life immunological and microbial differences between East African and North European children
Why early germs may shape lifelong health
Why do allergies, asthma, and autoimmune diseases seem more common in some parts of the world than others? One idea is that children who grow up with fewer everyday encounters with microbes may end up with immune systems that are more prone to overreact later in life. This study takes a close look at that possibility by tracking the immune systems and gut microbes of young children in two very different settings: rural Malawi in East Africa and urban Finland in Northern Europe.
Two childhoods, two microbial worlds
The researchers followed 40 Malawian and 40 Finnish children through their first three years of life. At several ages, they collected blood samples to measure small immune messengers called cytokines and stool samples to analyze gut bacteria, viruses, and parasites. All children were sampled on a fixed schedule, not because they were sick at the time. The Malawian families lived in rural villages with boreholes or wells as main water sources and mostly pit latrines, while the Finnish families lived in a highly industrialized country with municipal water and sanitation. Diets also differed sharply: Malawian children ate mainly maize porridge and other plant-based foods, whereas Finnish children consumed more animal protein and fat.
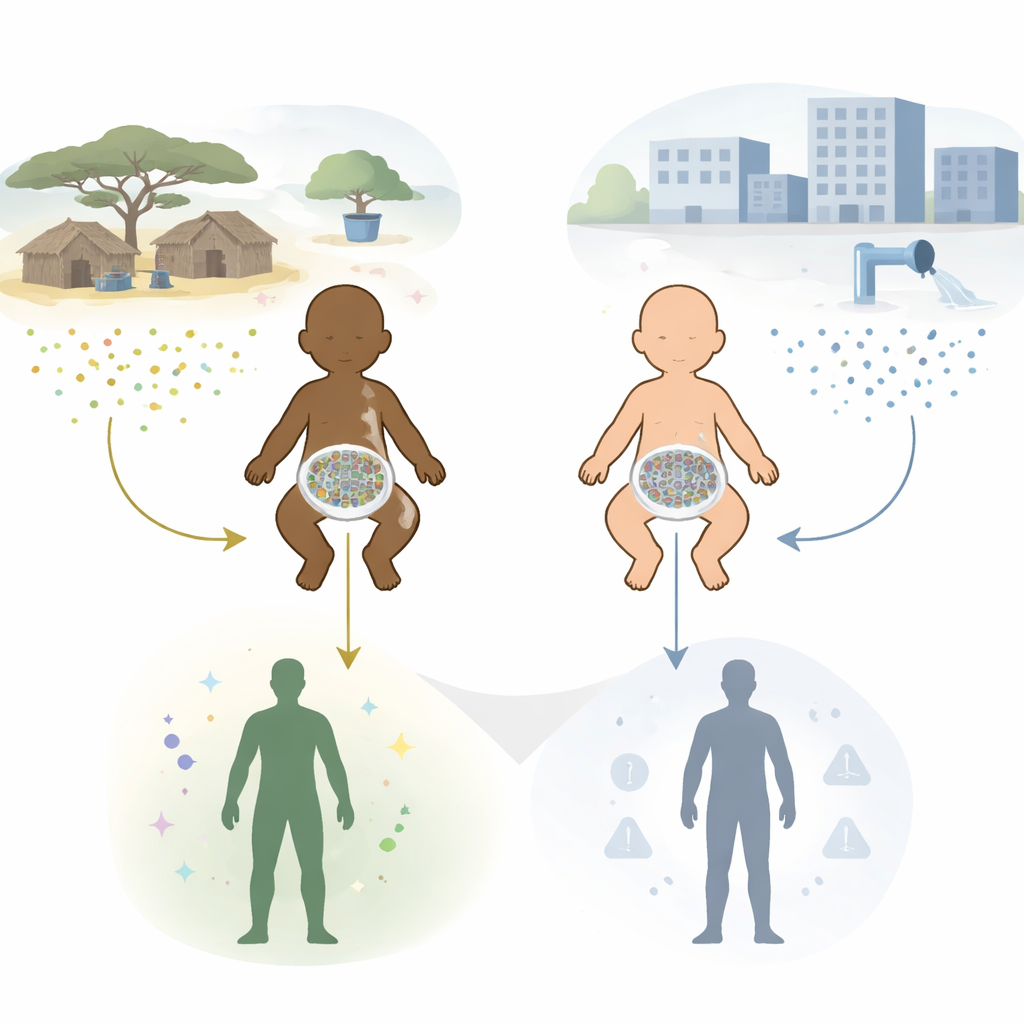
Immune alarms ring louder in Malawian children
From as early as six months of age, Malawian children had clearly higher levels of several key cytokines in their blood than Finnish children. These included signals linked to inflammation and its control. Although levels changed over time in both groups, Malawian children generally showed a pattern of stronger immune activation throughout early childhood. Breastfeeding was common and prolonged in Malawi and was associated with higher levels of some calming cytokines, suggesting that both feeding practices and ongoing infections help shape immune tone. The findings match earlier work in adults and older children showing that people in rural African settings often have more active immune systems than those in Western Europe.
Very different gut communities take shape
The children’s gut bacteria also diverged early and continued to separate with age. By six months, Malawian infants already had a different mix of gut microbes than Finnish infants. As Malawian children grew, their gut communities became richer in the genus Prevotella, a pattern often seen in traditional, plant-heavy diets. Finnish children’s guts instead shifted toward Bacteroides, typical of industrialized, protein- and fat-rich diets. Overall diversity told a similar story: Malawian guts tended to harbor more kinds of bacteria, including many rare types, while Finnish guts were dominated by fewer, more even groups. At every age checked, the overall community patterns of the two countries remained distinct.
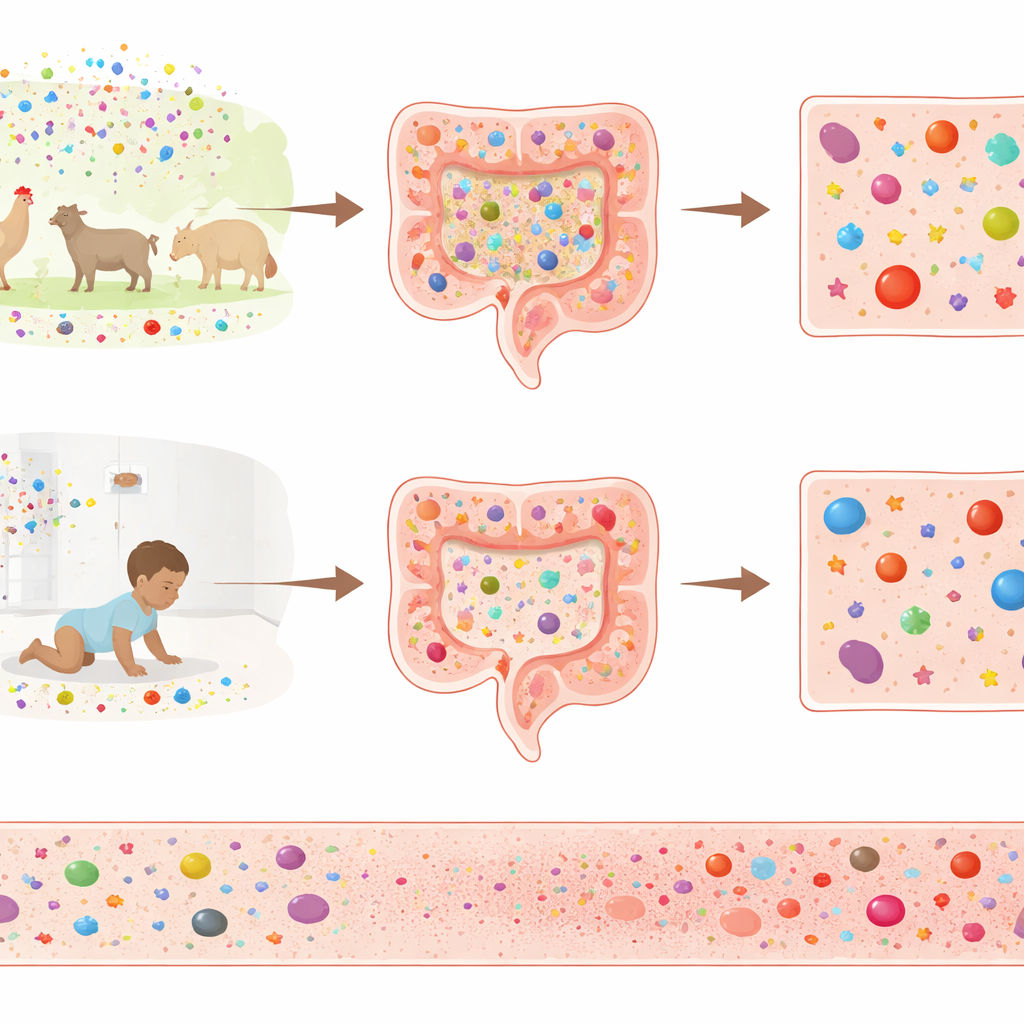
Heavier infection load and its immune imprint
Stool tests for common intestinal viruses and parasites showed that Malawian children carried a much heavier infection burden. Adenoviruses, enteroviruses, parechoviruses, rhinoviruses, noroviruses and parasites such as Giardia and Cryptosporidium were all detected far more often in Malawian samples; many children carried several at once without obvious illness. Finnish children rarely tested positive for these microbes. Using machine-learning methods, the researchers then linked particular gut bacteria and infections to specific cytokine levels at six and eighteen months. In the Finnish group, many individual microbes showed clear associations with blood signals, suggesting a tight conversation between gut and immune system. In the Malawian group, where infections were constant and varied, far fewer one-to-one links stood out, hinting at a more chronically stimulated, less easily perturbed immune system.
What this may mean for future disease risk
Taken together, the findings show that major differences in gut microbes, infection patterns, and immune activity arise within the first year of life in children growing up at opposite ends of the “microbial exposure” spectrum. Rural Malawian children encounter a wider variety of microbes and more frequent infections, and their immune systems appear more activated and perhaps more rapidly matured. Finnish children, living with cleaner water, better sanitation, and different diets, have fewer infections, distinct gut microbes, and quieter immune signals. The authors suggest that these early-life contrasts could contribute to why immune-related chronic diseases are rising as African societies urbanize and adopt Western lifestyles. Understanding how to preserve the benefits of rich early microbial exposure while minimizing the harms of infection may be key to preventing future waves of allergy and autoimmune disease.
Citation: Nurminen, N., Fan, YM., Kortekangas, E. et al. Early-life immunological and microbial differences between East African and North European children. Commun Med 6, 216 (2026). https://doi.org/10.1038/s43856-026-01482-0
Keywords: gut microbiome, early childhood immunity, microbial exposure, urbanization and health, immune-mediated diseases