Clear Sky Science · en
Mapping neurophysiological biotypes of postpartum depression and underlying neural and molecular basis
Why New Mothers’ Brains Matter
Many new mothers struggle with lingering sadness, anxiety, and exhaustion after childbirth, a condition known as postpartum depression. This study asks a simple but important question: is postpartum depression really one single illness, or does it come in different biological forms that affect the brain in distinct ways? By peering into the brains of women shortly after birth, the researchers show that postpartum depression actually splits into at least two types, each with its own brain patterns and underlying chemistry. Understanding these differences could lead to more precise care instead of one-size-fits-all treatment.
Two Hidden Types of Postpartum Depression
The research team recruited 76 women with postpartum depression and 62 healthy new mothers from a hospital in China. All women had given birth within the past year and had not taken psychiatric medications. Using detailed MRI brain scans, the scientists measured gray matter volume, a basic feature of brain structure. Instead of sorting patients by symptoms alone, they used a data-driven clustering method to see whether the brain scans naturally grouped into different patterns. The strongest and most stable solution revealed two distinct brain-based subtypes of postpartum depression.
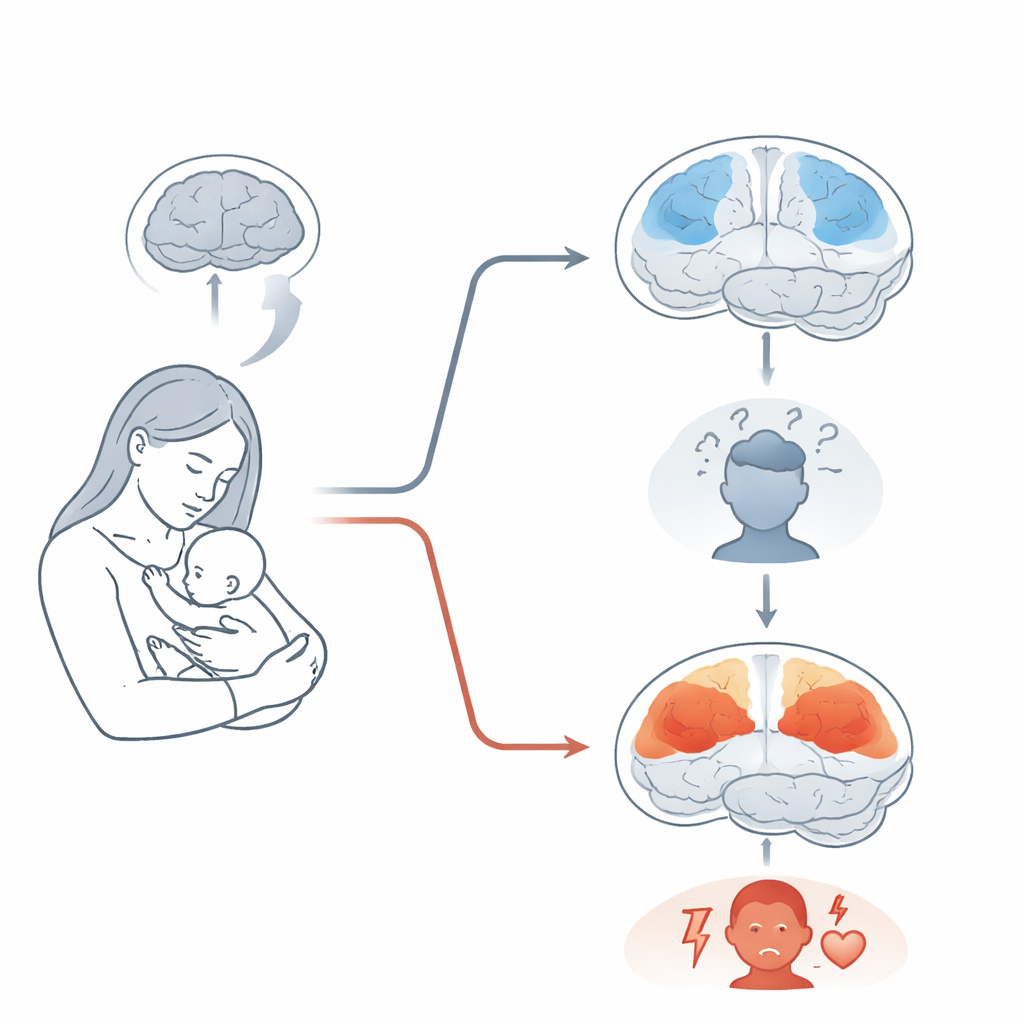
A Brain Network for Focus Versus a Network for Inner Thoughts
Women in the first subtype showed reduced gray matter in areas near the top and back of the brain that belong to the brain’s attention system. These regions help us focus on goals, process sensory information, and navigate space. In this group, smaller volume in these areas was linked to more severe depressive symptoms and changes in the hormone prolactin, which is involved in breastfeeding and stress. The authors suggest that this subtype reflects a “thinking and focus” form of postpartum depression, where mental fatigue, poor concentration, and sleep problems may be especially prominent.
When the Self-Focused Network Dominates
The second subtype looked very different. Here, women showed increased gray matter in the posterior cingulate cortex, a central hub of the brain’s default mode network. This network is most active when our minds drift inward—toward memories, self-reflection, and worry. Increases in this region may signal long-lasting overactivity of internal, self-focused thought. Women in this subtype tended to have slightly higher anxiety and perceived stress than those in the first subtype. Their brain wiring between temporal regions involved in interpreting social and emotional cues and limbic regions important for fear and memory was weaker, suggesting trouble integrating emotional information and regulating feelings.
Brain Wiring, Genes, and Brain Chemicals
Beyond structure alone, the study examined how different brain regions “covary” across individuals and how these patterns relate to genes and brain chemicals. In the first subtype, connections between temporal and emotional centers appeared stronger, perhaps as a strained attempt by the brain to compensate for attention problems. Gene activity linked to this pattern pointed toward disrupted energy use in brain cells and imbalanced handling of reactive molecules and proteins. The structural changes also lined up with the distribution of a glutamate receptor called mGluR5, hinting at altered excitatory signaling that could undermine clear thinking. In the second subtype, altered regions were tied to genes involved in brain development and synapse remodeling, and to several neurotransmitter systems often linked with mood and reward, including serotonin, dopamine, acetylcholine, and the brain’s own opioid-like signals. Together, these findings paint a picture of a more emotion-centered disturbance, with multiple chemical messengers out of balance.
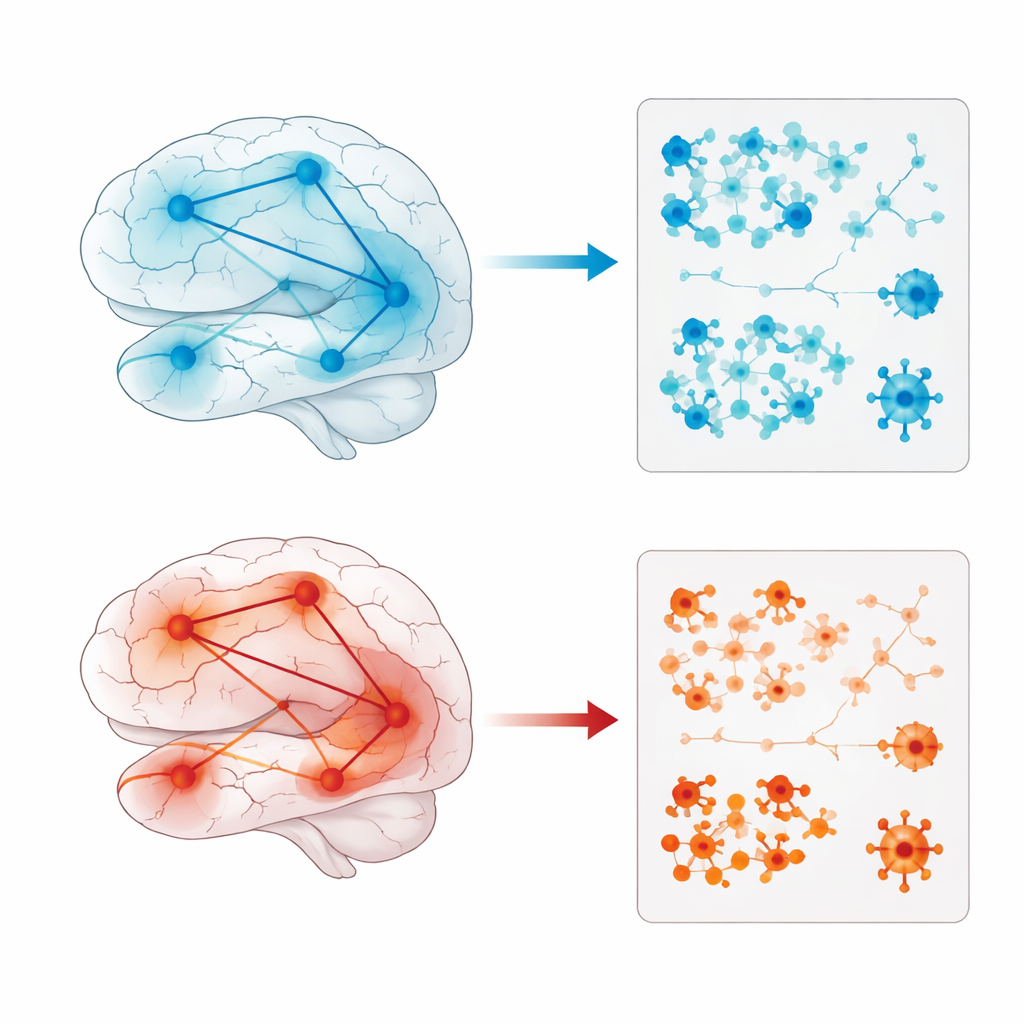
What This Means for Mothers and Care
Overall, the study suggests that postpartum depression is not a single, uniform condition. One form appears to center on disrupted attention and cognitive energy, while the other is driven more by emotional turmoil and self-focused rumination. Each type shows its own fingerprint of brain structure, wiring, genes, and brain chemistry. For families and clinicians, this means that two mothers with similar scores on a depression questionnaire may actually have very different biology behind their suffering. In the future, brain-based subtyping could help match women to more tailored treatments—such as focus on sleep and cognitive support for one group, and emotion regulation or targeted brain stimulation for the other—moving postpartum care closer to truly personalized medicine.
Citation: Chen, J., Liang, Y., Li, W. et al. Mapping neurophysiological biotypes of postpartum depression and underlying neural and molecular basis. Commun Med 6, 201 (2026). https://doi.org/10.1038/s43856-026-01477-x
Keywords: postpartum depression, brain imaging, neural subtypes, emotion regulation, personalized psychiatry