Clear Sky Science · en
A longitudinal comparative analysis of serum metabolomic signatures in children with SARS-CoV-2 infection and MIS-C
Why children’s COVID-19 chemistry matters
COVID-19 is often milder in children than in adults, but a small number develop a dangerous condition called multisystem inflammatory syndrome in children (MIS-C). Doctors still struggle to predict which child will simply have a brief fever and which might end up in intensive care. This study looks at tiny molecules circulating in the blood—metabolites—to see how a child’s body chemistry responds to the virus over time, how this differs with age and illness severity, and how MIS-C stands apart from ordinary pediatric COVID-19.
Following the chemical trail in young patients
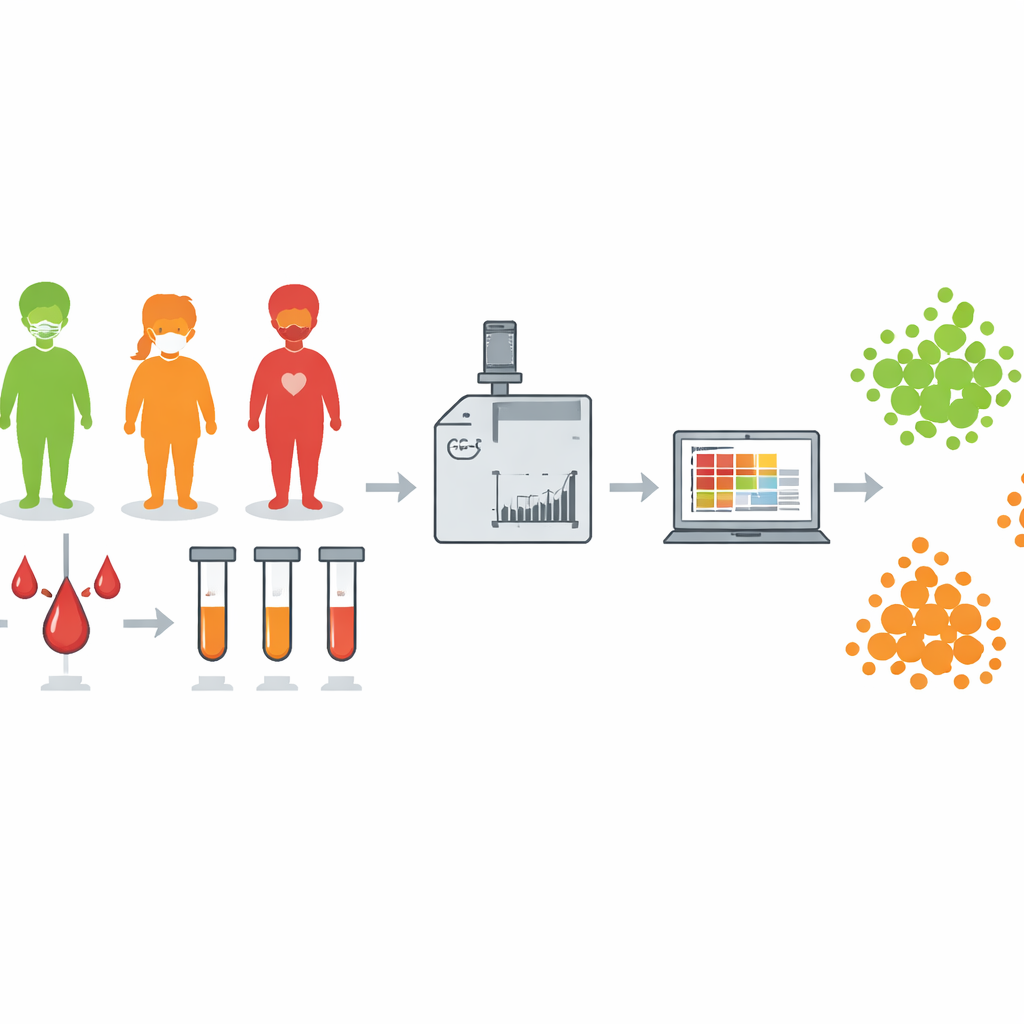
The researchers enrolled 92 children hospitalized with acute SARS-CoV-2 infection, 7 with MIS-C, and 41 healthy children of similar age and sex. From each child, they collected blood samples at several key moments: when they were admitted, during the sickest phase, at discharge, and again weeks later after they had cleared the virus. Using a technique called gas chromatography–mass spectrometry, they measured hundreds of small molecules in the blood at once. Advanced statistical tools then sorted these complex patterns to see whether infected children, healthy controls, and MIS-C patients formed distinct “chemical fingerprints.”
A distinct COVID-19 fingerprint that fades with recovery
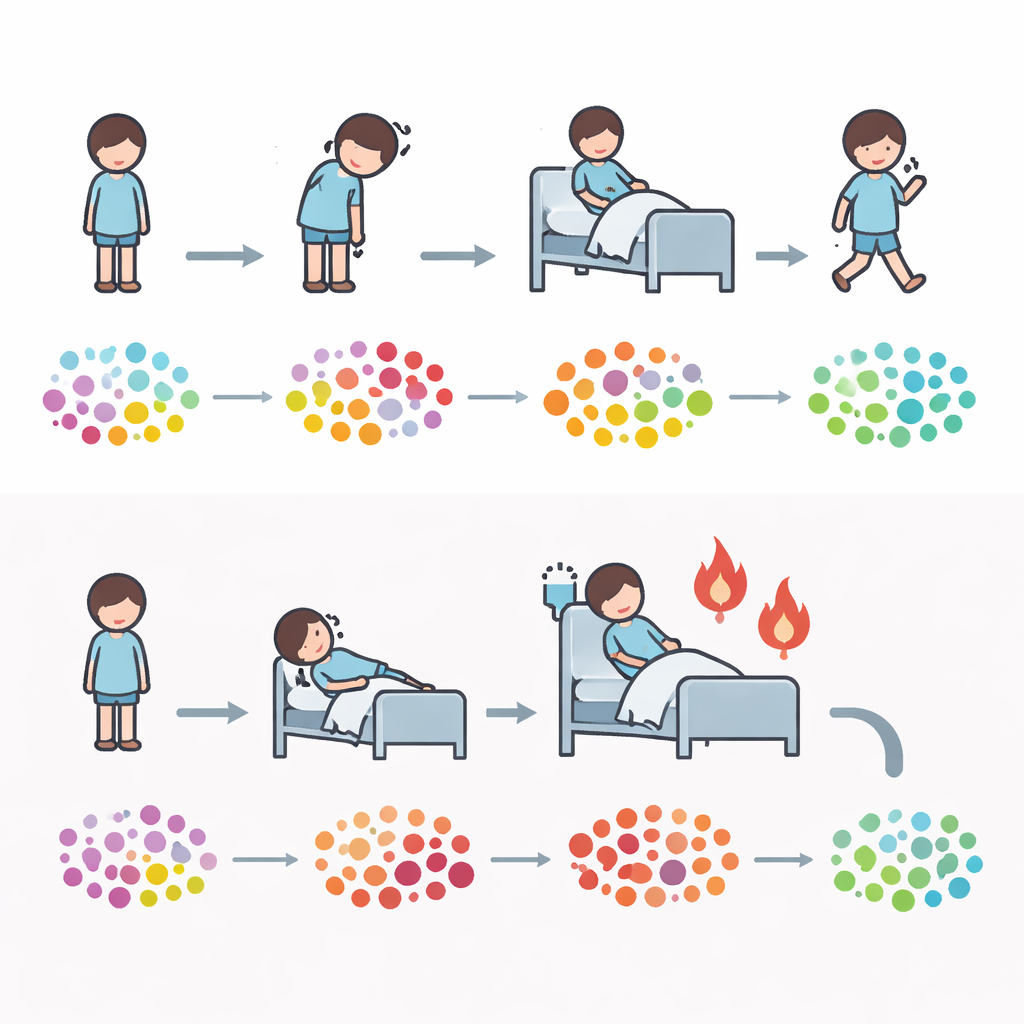
Compared with healthy children, those with acute COVID-19 showed a clearly different mix of blood metabolites. Molecules linked to sugar use, such as forms of glucose and related sugars, and to fat processing, such as specific fatty acids, were especially altered. A few sugars associated with the gut environment were increased, while several fats and energy-related molecules were reduced. When the team followed children over time, they saw that many of these changes were most pronounced during the acute illness and then gradually shifted back toward the healthy pattern once the virus was cleared and symptoms resolved. This suggests that the metabolic changes are closely tied to the active battle between the child’s body and the virus rather than being permanent damage.
Age, severity, and inflammation shape the chemical pattern
Age turned out to be important. In children younger than about three years, the blood chemistry of infected patients and healthy peers looked surprisingly similar, hinting that normal developmental changes in metabolism may overshadow the effects of the virus. In older children, however, COVID-19 left a clearer imprint, again involving sugar and fat handling and even pathways connected to sex hormones. The team also compared children with mild illness to those who were severely ill or had strong signs of inflammation in their blood tests. More severe cases showed additional shifts in fat-related molecules and compounds tied to high cell turnover and immune activation. Some fatty acids dropped as inflammation rose, possibly because the body was consuming them as fuel for inflammatory processes.
How MIS-C stands apart from ordinary COVID-19
MIS-C, which usually appears a few weeks after infection, brought its own striking chemical signature. Even when matched for age and sex, children with MIS-C had blood metabolite patterns that differed sharply from both healthy controls and children with acute COVID-19. Their profiles pointed to strongly disturbed fat metabolism, altered energy shuttling inside cells, and changes in molecules involved in cell growth and repair. Several specific metabolites were consistently higher in MIS-C than in ordinary COVID-19. Although only seven MIS-C patients were studied, these consistent differences suggest that MIS-C is not just “more severe COVID-19” but a distinct inflammatory condition with its own metabolic footprint.
What this means for children with COVID-19
Taken together, the findings show that pediatric COVID-19 is linked to a recognizable, age-dependent shift in how children process sugars, fats, and other small molecules—and that this shift largely reverses as they recover. Severe illness and strong inflammation leave deeper marks on this chemical landscape, and MIS-C sits in its own corner of this map. In the future, measuring selected metabolites in a child’s blood might help doctors spot those at risk of severe disease or MIS-C earlier and tailor monitoring and treatment before complications develop.
Citation: Lo Vecchio, A., Discepolo, V., Pierri, L. et al. A longitudinal comparative analysis of serum metabolomic signatures in children with SARS-CoV-2 infection and MIS-C. Commun Med 6, 207 (2026). https://doi.org/10.1038/s43856-026-01431-x
Keywords: pediatric COVID-19, MIS-C, metabolomics, inflammation, SARS-CoV-2