Clear Sky Science · en
Cerebrospinal fluid cfDNA-based molecular assessment of resection extent and prognosis in glioma
Why This Matters for People With Brain Tumors
For people facing brain tumors, especially aggressive gliomas, one of the most urgent questions after surgery is, “Did the surgeons get it all?” Today, doctors mostly rely on brain scans and their own judgment in the operating room, which can miss tiny pockets of remaining cancer cells. This study explores a new, more precise way to measure surgical success by looking for tumor DNA fragments floating in the clear fluid that bathes the brain and spinal cord, potentially offering patients a clearer picture of their outlook and guiding follow-up treatment.
A Hidden Signal in Brain Fluid
Our brains are surrounded by cerebrospinal fluid (CSF), a clear liquid that cushions the brain and carries away cellular debris. When tumor cells die, they release bits of their DNA into this fluid. The researchers wondered if these DNA fragments could act like a molecular “fingerprint” of the tumor, revealing how much cancer is present before and after surgery. Instead of cutting out more tissue for testing, they used a “liquid biopsy”: a small sample of CSF taken by lumbar puncture (spinal tap) a few days before surgery and again about a week afterward.
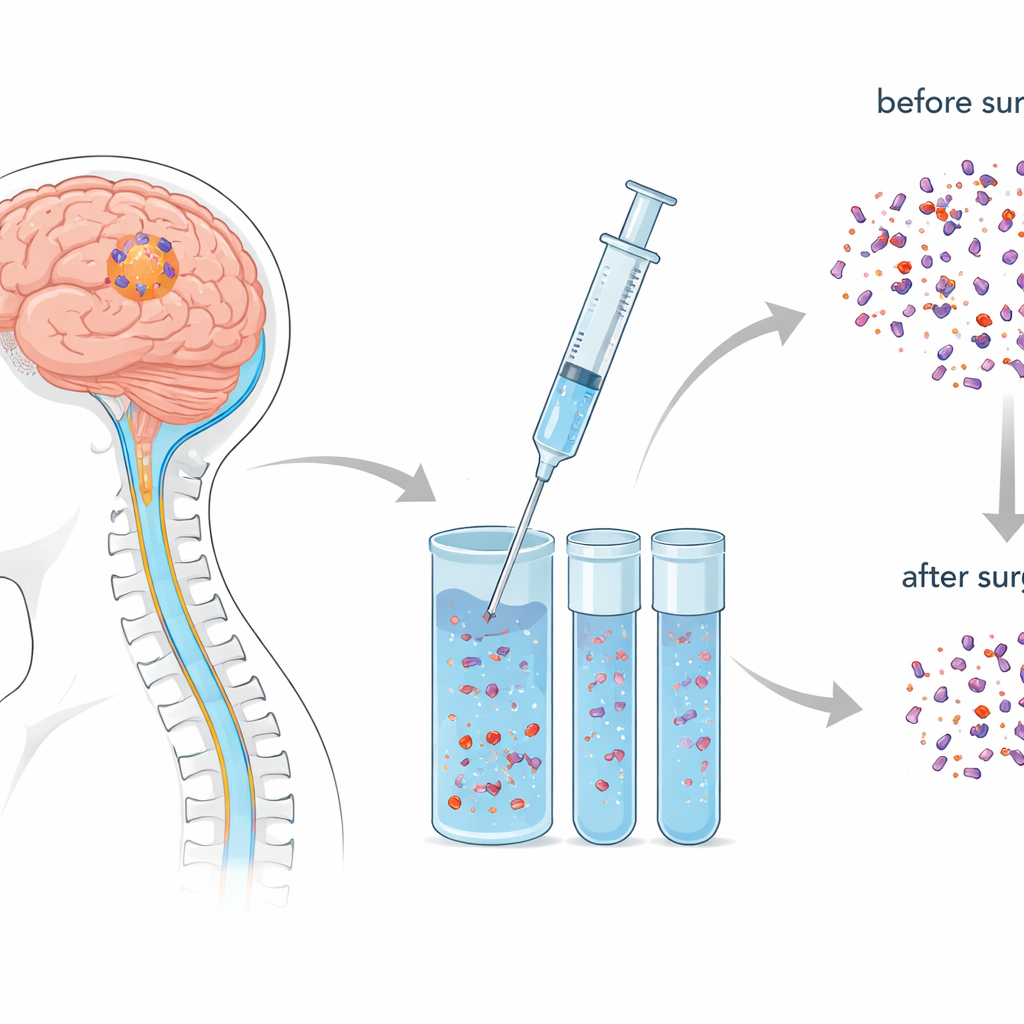
Matching the Tumor’s Genetic Signature
The team studied 32 patients with different kinds of brain tumors, most of them high-grade gliomas, the most aggressive type. They sequenced DNA from both the removed tumor tissue and the CSF samples to look for cancer-linked genetic changes. They found that the DNA in the CSF closely mirrored the DNA in the tumor itself—over 80% of the mutations seen in the tumor also appeared in the fluid. This was especially true for key cancer-driving genes often altered in gliomas. They also measured two summary numbers: how frequently mutated DNA appeared (mutant allele frequency, or MAF) and how many mutations were packed into the tumor DNA (tumor mutational burden, or TMB). Both of these measures in CSF tracked well with what they saw directly in the tumor.
Tracking What Surgery Really Removed
The central test came when the scientists compared CSF taken before and after surgery. After the tumor was removed, the amount of tumor DNA in the CSF dropped sharply. On average, the mutation frequency fell more than tenfold, and the overall number of mutations also fell by nearly 80%. Many specific cancer-driving mutations that were clearly present before surgery became undetectable afterward. However, in some patients—especially those with tumors in multiple brain areas—these cancer signals lingered, suggesting that microscopic disease remained even when scans looked good.
Connecting DNA Changes to Survival
The study then asked whether these molecular changes in the CSF could predict how long patients lived. Among people with high-grade gliomas, those whose CSF showed at least a 90% drop in average mutation frequency after surgery survived significantly longer than those with smaller drops. A similar pattern emerged when the team focused only on the most important cancer-driving mutations: patients in whom these powerful mutations nearly disappeared from the CSF tended to do better. Importantly, this information sometimes told a different story than imaging. A few patients who did not appear to have a complete tumor removal on scans still had a clean CSF DNA profile and went on to live much longer than expected, while others with seemingly complete removal on imaging still had lingering tumor DNA and poorer outcomes.
What This Could Mean for Future Care
Taken together, these findings suggest that tumor DNA in CSF could serve as a sensitive, objective gauge of how successful brain tumor surgery really was. Instead of relying only on what the eye can see on MRI, doctors might one day use this molecular readout to decide who needs more aggressive follow-up treatment, who might safely avoid extra therapy, and who needs closer monitoring for early signs of recurrence. While the study was modest in size and more research is needed, it points toward a future in which a simple fluid test helps personalize care for people with gliomas, offering clearer answers at one of the most anxious moments in their treatment journey.
Citation: Wu, J., Liu, Z., Huang, T. et al. Cerebrospinal fluid cfDNA-based molecular assessment of resection extent and prognosis in glioma. Commun Med 6, 206 (2026). https://doi.org/10.1038/s43856-026-01386-z
Keywords: glioma, cerebrospinal fluid, liquid biopsy, cell-free DNA, brain tumor surgery