Clear Sky Science · en
3D Spatiotemporal cardiac reconstruction for predicting MACE in acute myocardial infarction
Why predicting heart trouble years in advance matters
After a heart attack, many patients worry not just about surviving the first days and weeks, but about what might happen years down the road. Some people recover smoothly, while others face serious complications such as repeat heart attacks, heart failure, or sudden dangerous rhythms. Doctors have scoring systems to estimate this risk, but these tools rely on a handful of numbers and often only look a year ahead. This study explores whether modern medical imaging and artificial intelligence can turn a moving 3D picture of the heart into a much sharper, longer-term warning system.
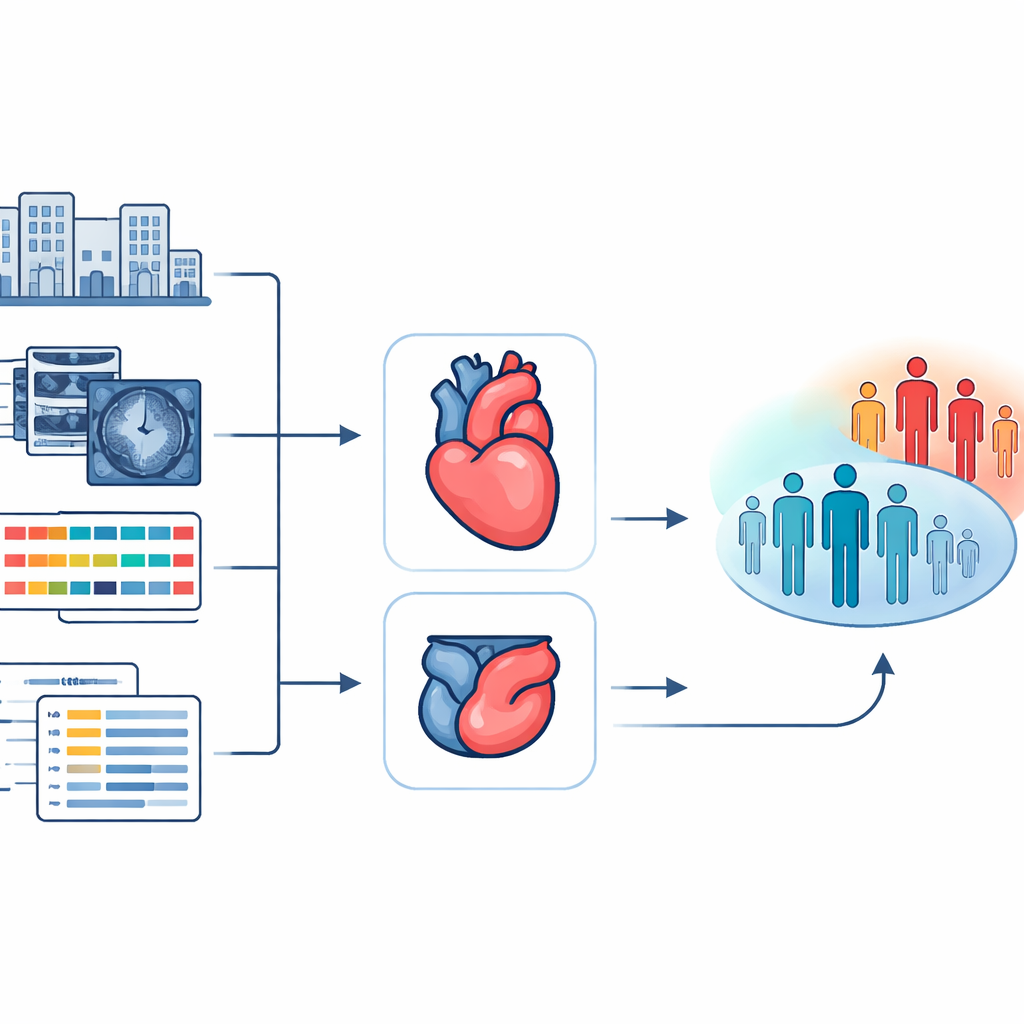
From hospital scans and charts to a unified risk picture
The researchers drew on data from more than 4,500 people who had an acute heart attack and underwent emergency artery-opening procedures. All of these patients also had a standard type of heart MRI soon after treatment, along with detailed clinical records such as age, blood tests, blood pressure, and information about the damaged heart muscle. Instead of using only pre-calculated summary measures from these scans, the team set out to use the images themselves, capturing both the shape of the heart and how it moves over time. Their goal was to build a system that could absorb this rich imaging information together with 45 routine clinical and scan-based variables and then forecast whether a patient would suffer a major cardiac problem within the next five years.
Rebuilding the beating heart in 3D
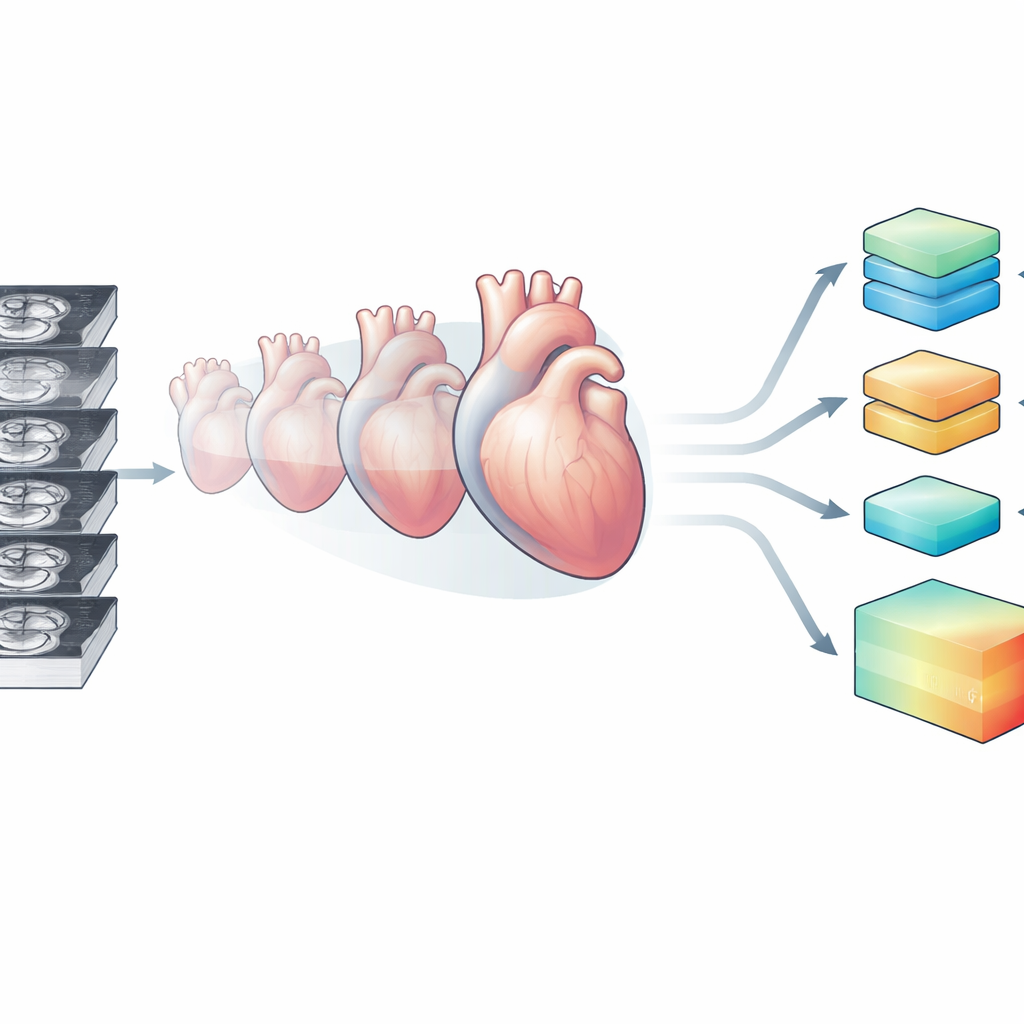
Heart MRI is usually collected as a stack of thin 2D slices taken at slightly different positions and heartbeats. This can leave gaps and misalignments, so the resulting view of the heart is incomplete and a bit choppy. To overcome this, the team created a model called ReconSeg3D that learns to reconstruct a smooth, continuous, three-dimensional heart from these slice stacks and to separate its main parts: the left and right pumping chambers and the surrounding heart muscle. Trained on public imaging datasets and then applied to the patient scans, ReconSeg3D produced detailed 3D sequences of the heart beating over an entire cardiac cycle, effectively turning a stack of noisy slices into a coherent movie of the organ’s motion in space and time.
Teaching an AI to read motion, structure, and medical history together
With this 3D "cine" reconstruction in hand, the researchers built a second model, HeartTTable, to predict long-term outcomes. This system treats the 3D beating heart like a small animated volume that can be cut into patches and frames. One part of the model focuses on how features are arranged in space, another on how they change through time as the heart contracts and relaxes, and a third part processes the numerical clinical and scan-derived variables. Using a type of architecture known for handling complex patterns, the model then lets these three streams of information interact, learning how subtle changes in motion and structure relate to a person’s medical profile and eventual outcome.
How much better is this new approach?
When HeartTTable relied only on the tabular clinical and scan-derived numbers, its performance at predicting who would have a serious event over five years was moderate. When it used only the reconstructed 3D heart sequences, predictions improved markedly, showing that the rich motion and shape information held important clues. The best results came from combining both sources: the full multimodal model reached very high accuracy for five-year risk prediction, clearly separating patients into low- and high-risk groups in survival analyses. The 3D heart representation consistently beat simpler inputs such as raw slice stacks, limited views, or single time points in the heartbeat, underlining the value of capturing the entire cardiac cycle in three dimensions.
What this could mean for patients and doctors
The study suggests that standard post–heart attack MRI scans contain far more prognostic information than current scoring systems tap into. By rebuilding the beating heart in 3D and fusing this with routine clinical data, the HeartTTable model can identify who is most likely to run into serious trouble in the next five years, far beyond the usual one-year window of existing tools. For patients, such forecasts could help guide the intensity of follow-up visits, lifestyle interventions, and medications. For clinicians and health systems, they offer a route to focus resources on those who need them most. While further testing in broader populations is needed, this work points toward a future in which a single scan and an AI model could give a detailed long-term map of a heart attack survivor’s risk.
Citation: Gao, Q., Wu, J., Gao, Y. et al. 3D Spatiotemporal cardiac reconstruction for predicting MACE in acute myocardial infarction. npj Digit. Med. 9, 325 (2026). https://doi.org/10.1038/s41746-026-02449-0
Keywords: heart attack, cardiac MRI, artificial intelligence, risk prediction, 3D heart imaging