Clear Sky Science · en
Comparative analysis of bypass vs. stent for coronary revascularization using an ex-vivo organ care system in an animal model
Why heart repair choices matter
When doctors reopen clogged heart arteries, they often choose between placing a tiny metal tube called a stent or sewing on a new vessel to carry blood around the blockage, known as a bypass. Both can quickly restore blood flow, but little is known about how they affect the heart’s fine drainage and support network over time. This study in pigs, whose hearts closely resemble human hearts, explores how these two treatments differ in the way they influence blood flow, tissue health, and the little-known lymph system that quietly clears waste from the heart.
Building a realistic heart blockage
To compare stents and bypass surgery in a controlled way, researchers first needed a safe, repeatable form of artery narrowing. They created an artificial plaque from gelatin, fats, and mineral particles designed to mimic the feel and shape of a real fatty deposit inside a coronary artery. This plaque was mounted on a standard stent and inserted into a key front artery of the pig heart, reproducing a moderate narrowing similar to human coronary disease. Because the plaque can be placed like a regular device, it offers a flexible tool for future experiments on different vessels and treatment strategies without causing disease in the whole animal.
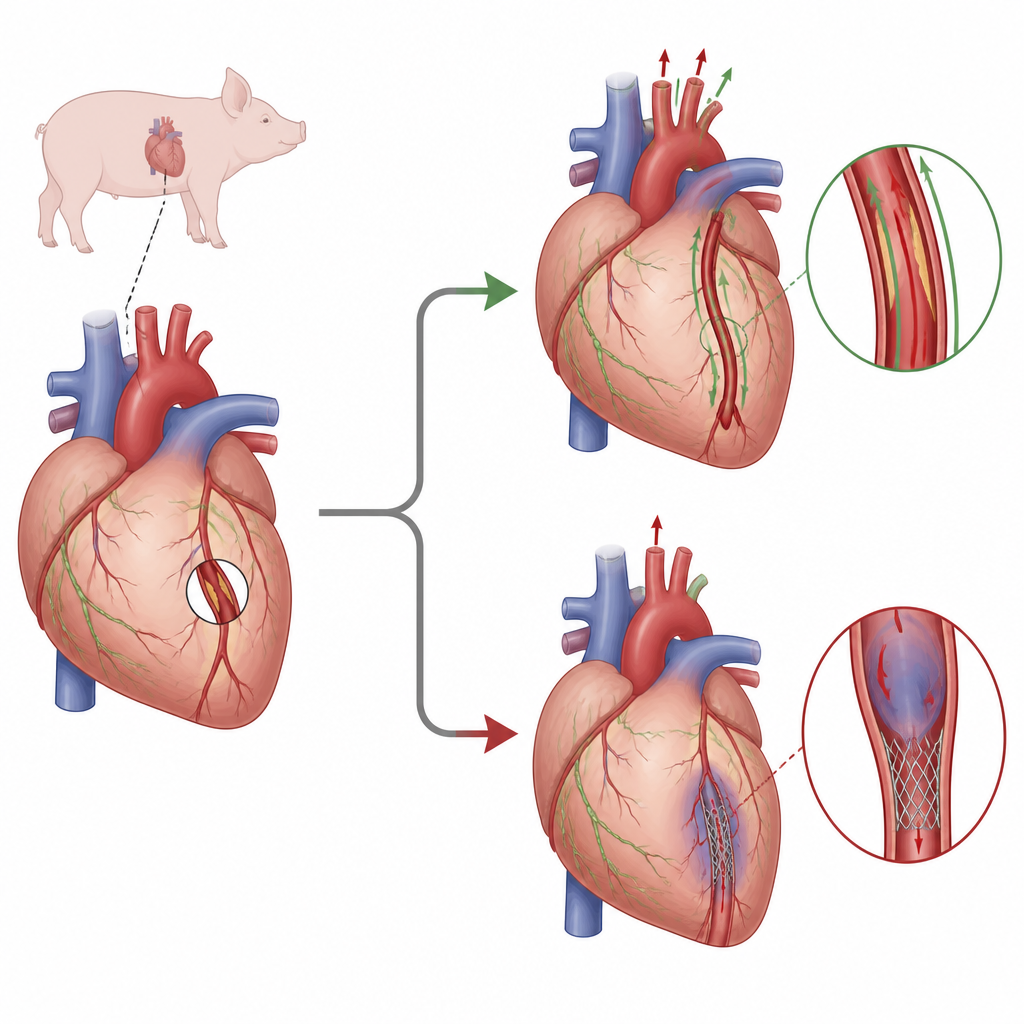
Keeping hearts alive outside the body
After the plaques were implanted, half of the pigs received a stent to push the plaque aside from within the artery, while the other half underwent bypass surgery using a chest artery grafted onto the blocked vessel. The hearts were then removed but kept beating on a special machine called an organ care system. This setup pumped warm, oxygen-rich blood through the hearts, allowing the team to study them in near-natural conditions with precise control of pressures, flows, and imaging angles. With the heart supported in this way, they could watch how fluid moved through the vessels and tissues without the complexity of a whole living animal.
Watching blood and lymph move through the heart
To track the heart’s drainage system, the scientists injected a tiny amount of a radioactive tracer into the heart muscle near the tip and used advanced scans to follow its path. In healthy hearts, the tracer traveled smoothly along the main vessels toward the base of the heart, and blood flow through the muscle looked even and complete. When the main artery was tied off or treated with a stent, the tracer tended to collect just before the damaged or treated segment, suggesting that lymph flow, the “waste removal” fluid system, was slowed or interrupted there. By contrast, in hearts that had received a bypass graft, the tracer again moved freely from the tip toward the base, indicating restored drainage alongside preserved blood supply.
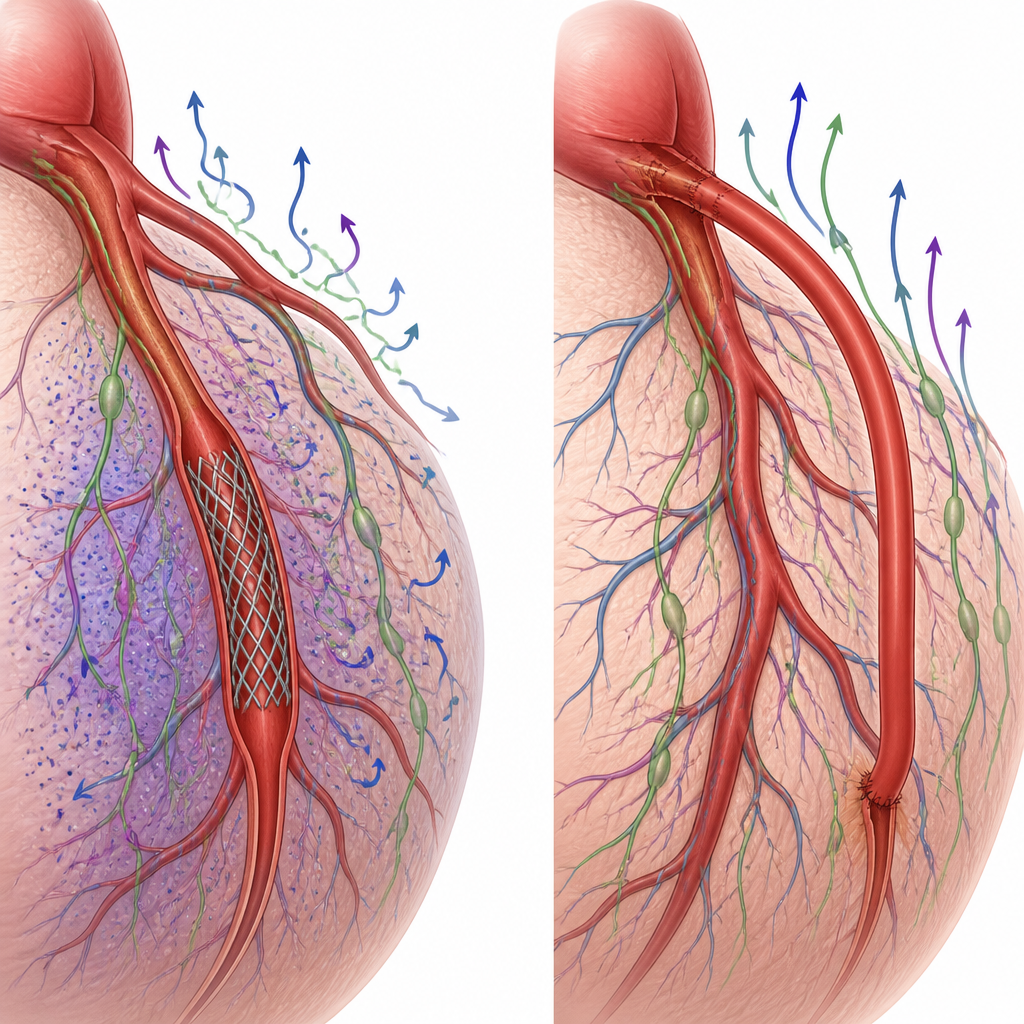
What tissue samples revealed
Microscopic examination of heart tissue added another piece to the picture. In the bypass group, the connection between the graft and the native artery remained open and smooth, with no signs of fresh clots, severe narrowing, or obvious damage to nearby nerves and tiny vessels. The stent group also showed open arteries without clear cell death in the short time frame studied, but the imaging evidence pointed to disturbed lymph flow near the treated area. Because the experiments covered only a few hours after the procedures, the researchers could not yet see slow-developing scarring or chronic injury, but the altered drainage pattern around stents hints that longer term changes may emerge over days to months.
What this means for patients
In plain terms, this work suggests that while both stents and bypasses can restore blood flow, bypass surgery may do a better job of preserving the heart’s self-cleaning system. The artificial plaque model and the beating-heart machine together form a new test bed for studying how repairs to clogged arteries affect not just blood delivery but also the fine vessels and lymph channels that support long-term heart health. For patients, the findings help explain why bypass surgery may offer more durable benefits in some cases, and they point researchers toward new ways of judging treatments by how well they protect the heart’s delicate drainage and support network, not just how widely they open a blocked artery.
Citation: Lindenhahn, P., Hinkel, R., Napp, L.C. et al. Comparative analysis of bypass vs. stent for coronary revascularization using an ex-vivo organ care system in an animal model. Sci Rep 16, 14762 (2026). https://doi.org/10.1038/s41598-026-50599-8
Keywords: coronary artery disease, bypass surgery, stent, lymphatic flow, organ care system