Clear Sky Science · en
An eye drop combination for treating Staphylococcus aureus-induced keratitis in rats: repurposing ibuprofen
Why this eye drop study matters
Infections of the clear front window of the eye, the cornea, can turn a routine eye problem into a medical emergency and even cost people their sight. This study explores whether a familiar painkiller, ibuprofen, can be repurposed and combined with a standard antibiotic eye drop to better treat a stubborn type of bacterial eye infection caused by Staphylococcus aureus. By using a rat model, the researchers asked if this two-in-one eye drop could not only kill bacteria, but also calm damaging inflammation and protect the delicate corneal tissue.
A dangerous eye infection in focus
Bacterial keratitis is a severe infection of the cornea that often begins after a small injury or irritation, such as contact lens wear, trauma, or previous eye surgery. Among the many germs that can invade, Staphylococcus aureus stands out as a leading cause worldwide and is notorious for becoming resistant to multiple antibiotics. These bacteria can also form slimy protective communities called biofilms, which make them harder to eradicate. The result can be intense pain, redness, blurred vision, and in serious cases scarring or even blindness. Standard care relies on antibiotic eye drops, but growing resistance and tissue damage driven by the body’s own inflammatory response leave room for improvement.
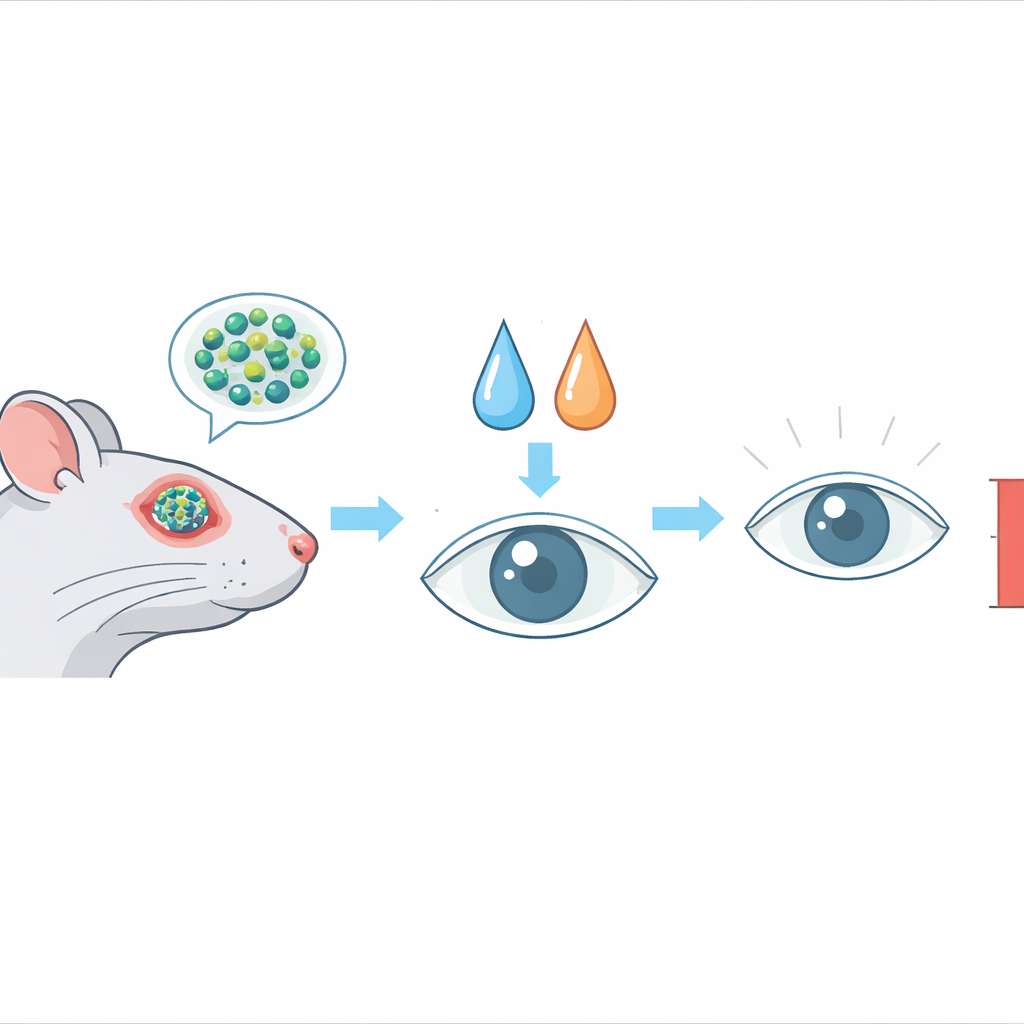
Repurposing a common drug for a new role
The team investigated whether ibuprofen, a well-known non‑steroidal anti‑inflammatory drug used for headaches and joint pain, could be harnessed to support the antibiotic levofloxacin. First, they tested Staphylococcus aureus samples taken from eye infections in Egypt. These bacteria were resistant to many commonly used antibiotics and were strong biofilm formers, making them particularly difficult to treat. In laboratory experiments, ibuprofen on its own showed direct antibacterial and anti‑biofilm activity. Even more striking, when ibuprofen was combined with levofloxacin, the amount of antibiotic needed to stop bacterial growth dropped several‑fold, showing a clear synergistic effect. The mixed eye drop also outperformed single‑drug drops in reducing bacterial counts and preventing new biofilm formation.
Testing the combo in infected rat eyes
To see what this meant for a living eye, the researchers created corneal infections in rats by gently scratching the surface of one eye and adding a measured dose of Staphylococcus aureus. The animals were then divided into groups: untreated infection, levofloxacin alone, ibuprofen alone, or the combination drops, given for two weeks. After treatment, the corneas were examined in two ways. At the molecular level, the team measured the activity of genes linked to inflammation, tissue‑digesting enzymes, new blood vessel growth, and cell death. At the structural level, they inspected thin stained slices of the cornea under the microscope to look for swelling, invading immune cells, abnormal blood vessels, and damage to the tissue layers.
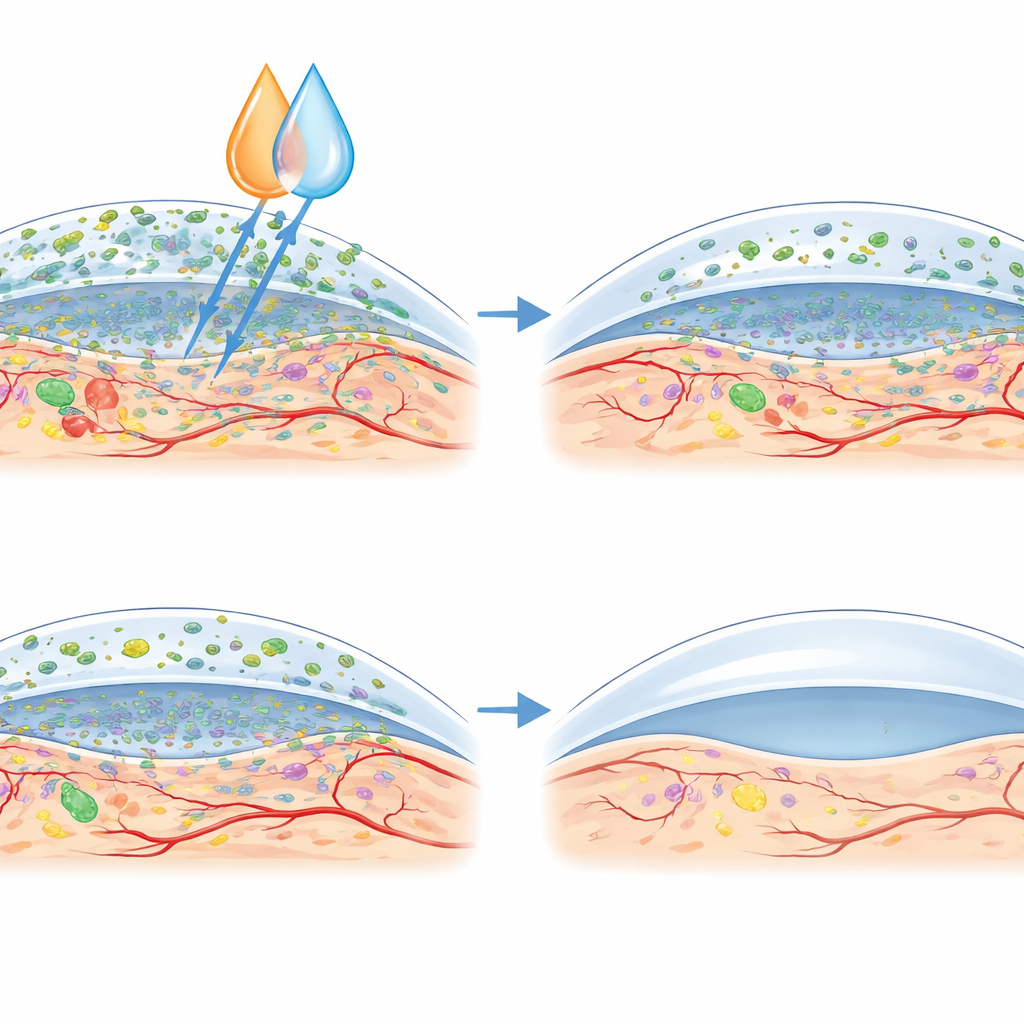
Cooling the fire inside the cornea
In untreated infected eyes, the corneas showed a storm of inflammatory signals. Genes driving inflammatory messengers, enzymes that chew through the corneal scaffold, factors that spur unwanted blood vessels, and markers of cell suicide were all turned up. Levofloxacin alone controlled bacteria but did not fully calm this molecular storm and was even associated with some ongoing harmful changes. Ibuprofen alone reduced several damaging signals and lowered biofilm mass, but infection and structural damage were still visible. The combination therapy stood out: these eyes showed the lowest levels of inflammatory and tissue‑destroying gene activity and less stimulus for new blood vessel growth, alongside reduced markers of cell death. Microscope images confirmed this, with the combined‑therapy corneas appearing closest to normal architecture, with limited inflammation and neovascularization.
What this means for future eye care
For a lay reader, the take‑home message is that pairing a standard antibiotic drop with a repurposed painkiller like ibuprofen may offer a two‑pronged defense against serious corneal infections: it helps the antibiotic work better against tough, biofilm‑forming bacteria and at the same time dampens the damaging inflammation that threatens clarity of vision. In rats, this combined eye drop led to clearer, healthier corneas than either drug alone. The authors stress that their work is still exploratory, with small animal numbers, fixed dosing, and gene‑level rather than protein‑level measurements. More extensive studies in different infections and careful safety checks in humans will be needed before such a combination could reach the clinic. Still, the results suggest a promising strategy: using an everyday medicine in a new way to protect one of our most vital senses, sight.
Citation: Seiffein, N.L., Kamel, M.AN., Ali, G.H. et al. An eye drop combination for treating Staphylococcus aureus-induced keratitis in rats: repurposing ibuprofen. Sci Rep 16, 13387 (2026). https://doi.org/10.1038/s41598-026-48096-z
Keywords: bacterial keratitis, Staphylococcus aureus, eye drops, ibuprofen repurposing, antibiotic synergy