Clear Sky Science · en
Deep learning-based differential diagnosis of major depression and bipolar disorder using microglia-cellular sensors and patient-derived small extracellular vesicles
Why this matters for people with mood disorders
Depression and bipolar disorder affect hundreds of millions of people worldwide, yet doctors still diagnose them mainly by talking with patients and observing behavior. Because depressive episodes in both conditions can look almost identical, many people with bipolar disorder are first told they “just” have depression, sometimes for years. This study explores a radically different idea: using a blood sample, living brain‑immune cells, and artificial intelligence to create an objective test that can tell major depression and bipolar disorder apart with remarkable accuracy.
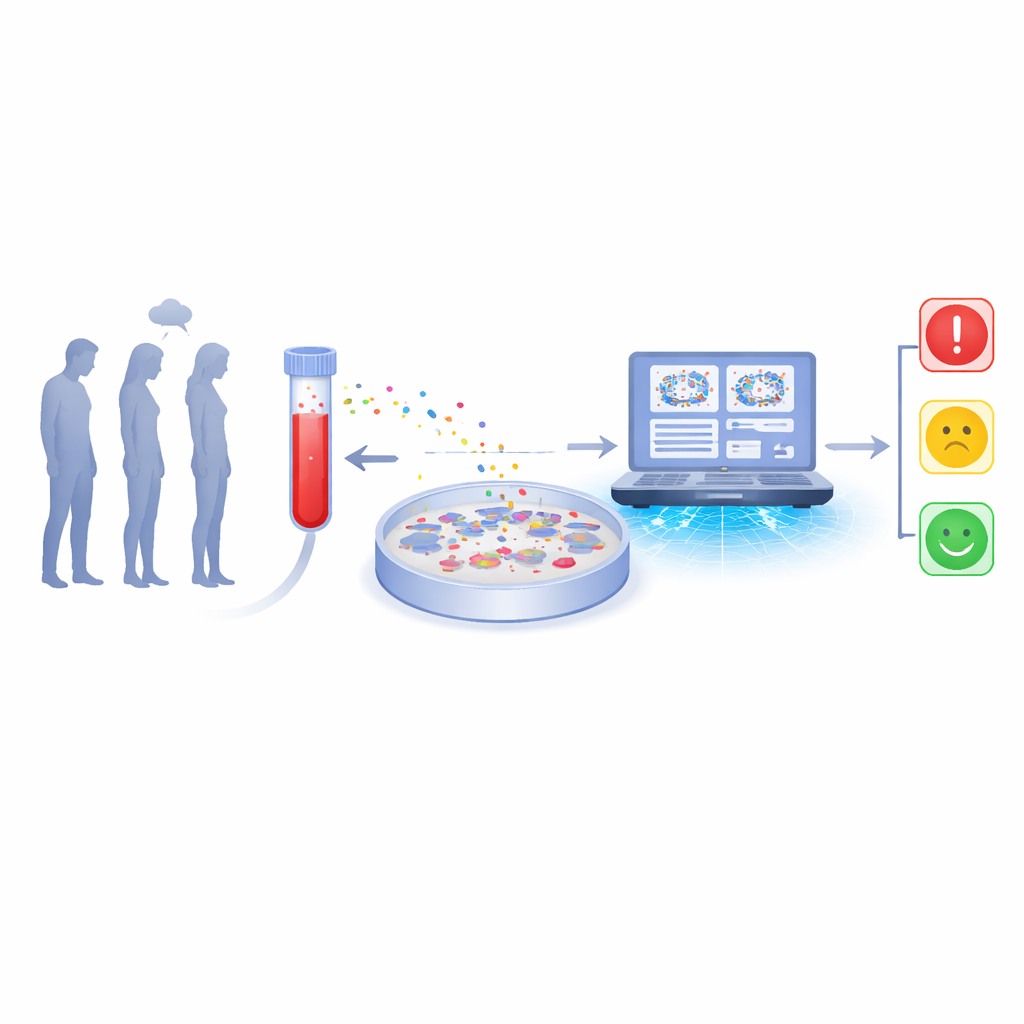
Turning a blood draw into a brain signal
The researchers focused on tiny particles in the blood called small extracellular vesicles. These are microscopic, fat‑coated bubbles released by many types of cells in the body, including cells in the brain. They carry proteins and genetic material that reflect what is happening inside those cells. Instead of trying to read this complex cargo directly, the team used the vesicles as messages and asked another cell type to "interpret" them: microglia, the brain’s resident immune cells. In the lab, microglial cells from rats were grown in dishes and exposed to vesicles purified from the blood plasma of three groups of people: those with major depressive disorder, those with bipolar disorder, and healthy volunteers.
Cells used as living sensors
Microglia are known to change their shape and internal structure when they sense inflammation or other disturbances in the brain. After a 24‑hour exposure to patient‑derived vesicles, the team fixed and stained the microglial cells with fluorescent markers so that the nucleus, cell body, and internal skeleton glowed in different colors under the microscope. Each image contained many cells, which were then automatically detected and cut into thousands of small, single‑cell pictures. The idea was that vesicles from different patient groups would nudge microglia into subtly different forms, and that these patterns, while invisible to the naked eye, could be picked up by advanced image analysis.
Teaching artificial intelligence to read cell patterns
Simply looking at one cell at a time turned out to be too noisy: when a deep learning model tried to classify individual cells, accuracy stayed below 60 percent. The key advance came from changing how the images were organized. Instead of feeding cells in one by one, the researchers arranged many single‑cell images from the same person into tidy square grids—arrays of 5 by 5 cells worked best. These arrays acted like composite portraits of each person’s microglial response. A powerful image‑recognition network, originally trained on everyday photographs and then fine‑tuned on these cell arrays, learned to sort each grid into one of three categories: depression, bipolar disorder, or healthy control.
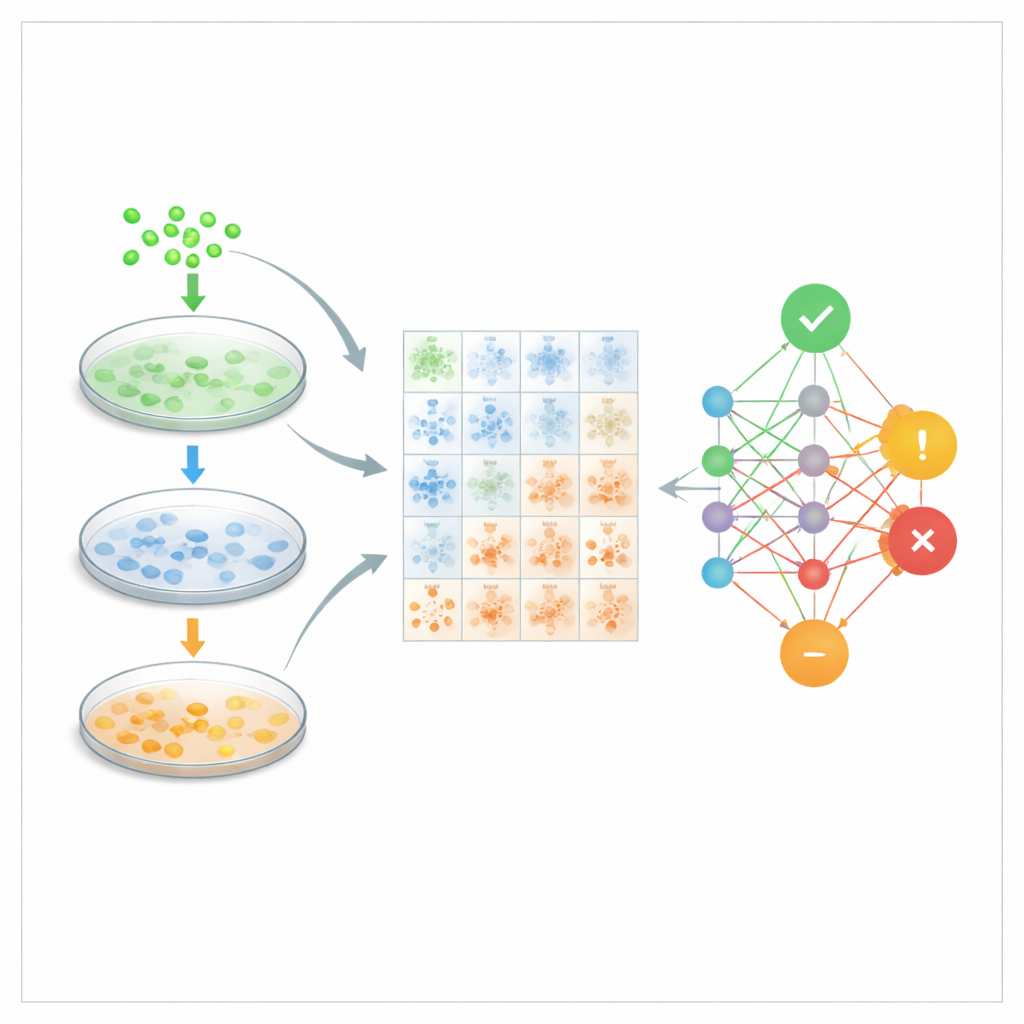
From grids of cells to a likely diagnosis
For every participant, the team generated many different arrays by shuffling the positions of the cells and slightly rotating or flipping them. Each array received a prediction from the neural network, along with a confidence score. To reach a subject‑level decision, the researchers did not simply take a majority vote; instead, they summed the confidence scores across all arrays and chose the diagnosis with the highest total. This “weighted voting” strategy took advantage of the fact that some arrays carried clearer signals than others. With this hierarchical approach—cells grouped into arrays, arrays combined into a final decision—the system correctly classified 44 out of 45 people across repeated tests, corresponding to a subject‑level accuracy of about 99 percent.
What this could mean for future mental health care
The work is still an early proof of concept, based on a modest number of participants, and it does not yet account for factors such as age, sex, medications, or life history. However, it shows that mood disorders can imprint distinct, machine‑detectable signatures on how microglial cells respond to blood‑borne signals. By pairing this biologically amplified readout with deep learning, the study points toward a blood‑based, next‑day test that could complement clinical interviews and reduce the long delays and frequent misdiagnoses that many patients endure. If confirmed in larger and more diverse groups, this kind of cell‑plus‑AI platform could become a powerful new tool in precision psychiatry, helping clinicians choose the right treatment sooner and more reliably.
Citation: Zambrano, J., Luarte, A., Contreras, J. et al. Deep learning-based differential diagnosis of major depression and bipolar disorder using microglia-cellular sensors and patient-derived small extracellular vesicles. Sci Rep 16, 11679 (2026). https://doi.org/10.1038/s41598-026-47476-9
Keywords: bipolar disorder, major depression, deep learning, extracellular vesicles, microglia