Clear Sky Science · en
Distinct clinical course and poor outcomes of small bowel bleeding in acute hematochezia: a nationwide multicenter study
Why this matters for everyday health
Sudden bleeding from the gut that shows up as blood in the stool is a common reason for emergency hospital visits. Most people and many doctors focus on the large intestine when this happens, but a small share of cases start higher up in the winding tube of the small intestine. This study followed thousands of patients across Japan to find out how bleeding from the small intestine differs from bleeding in the colon, and what that means for treatment, hospital stay, and survival.
Two types of gut bleeding
Doctors group these emergencies under a single label when fresh or dark red blood appears from the lower part of the digestive tract. However, the actual source can be either the colon or rectum, or the less accessible small intestine. By looking at over ten thousand people who came to 49 hospitals with sudden bleeding, the researchers could directly compare these two sources. They found that only about three in every hundred such patients had bleeding from the small intestine, yet these cases followed a clearly different path from those whose bleeding came from the colon.
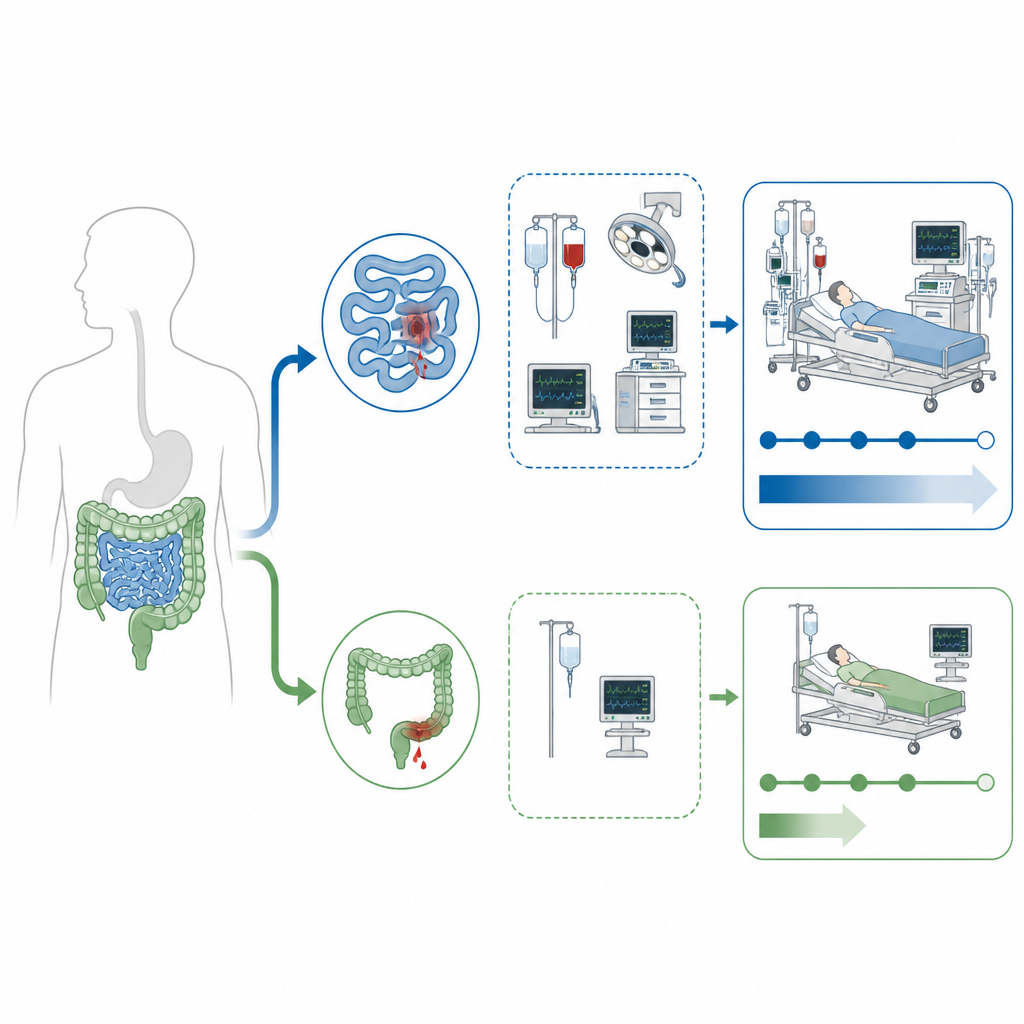
Who is more likely to have small intestine bleeding
People with small intestine bleeding tended to be younger and slimmer, and often did not report the classic crampy belly pain that many expect with gut trouble. Instead, they commonly arrived with signs of more advanced blood loss and poor nutrition, such as low red blood cell counts and low blood protein levels. Dark, tar-like stools were more frequent, hinting that blood had spent more time traveling through the gut before leaving the body. These patients more often had a history of bowel surgery, long lasting bowel inflammation, heart disease, liver scarring, or cancer, and were more likely to be taking certain painkillers or blood thinning drugs.
What happens in the hospital
Over the first month after admission, people with bleeding from the small intestine were just as likely to stop and restart bleeding and just as likely to survive as those with colon bleeding. Yet getting them through that early phase was harder. They were given larger amounts of transfused blood, had longer hospital stays, and were more likely to need radiology procedures or surgery to control the bleeding. In contrast, they were less likely to be treated successfully with a scope passed through the bowel, in part because the small intestine is harder to reach and to fully inspect. These differences add up to heavier use of hospital resources and more invasive care for a relatively small set of patients.
Longer term outlook and hidden risks
When the team looked beyond the first month, a striking pattern emerged. People whose bleeding started in the small intestine did not come back with new bleeding more often than those with colon bleeding, but they died more frequently over the next several years. Only one of these deaths was directly caused by the bleeding itself. Most occurred in people who also had cancer or other serious illnesses and whose blood tests at the first visit already suggested poor general health. The findings imply that in many of these patients, bleeding is a warning sign of an underlying serious condition rather than the main threat to life.
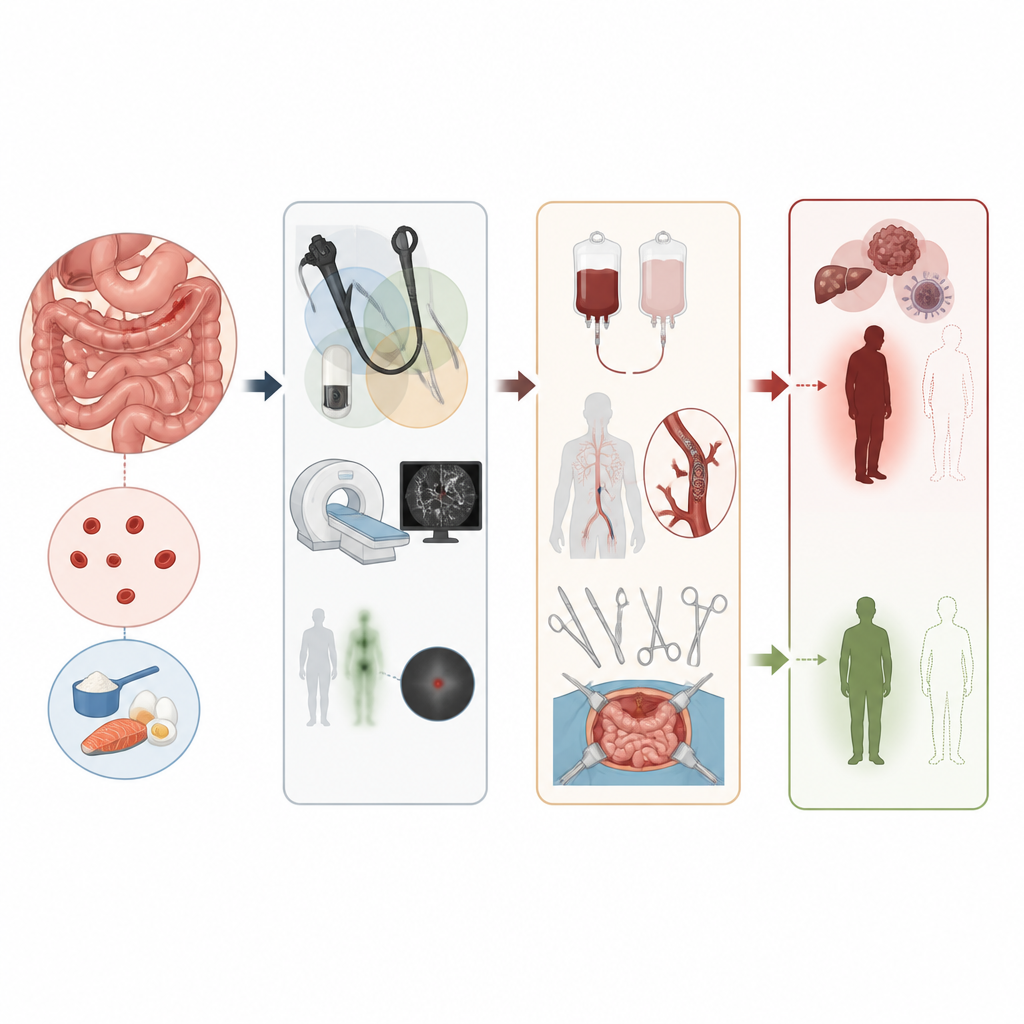
What this means for patients and doctors
This nationwide study shows that bleeding from the small intestine is uncommon but follows a distinctive and more serious clinical course than bleeding from the colon. It often appears after silent blood loss has already weakened the body, demands more intensive tests and treatments, and is linked to higher long term death rates, mainly because many affected patients also live with advanced cancer or other severe diseases. For patients, this means that when small intestine bleeding is found, close follow up of their overall health and any known major illnesses is just as important as stopping the bleeding itself.
Citation: Komaki, Y., Tominaga, N., Yamada, A. et al. Distinct clinical course and poor outcomes of small bowel bleeding in acute hematochezia: a nationwide multicenter study. Sci Rep 16, 13396 (2026). https://doi.org/10.1038/s41598-026-47311-1
Keywords: small bowel bleeding, acute lower gastrointestinal bleeding, colorectal bleeding, hospital outcomes, long term mortality