Clear Sky Science · en
Predictive value of preoperative T1 slope minus cervical lordosis for clinical outcomes after standalone laminectomy in elderly degenerative cervical myelopathy
Why neck shape matters for aging spines
As people live longer, more of us develop wear-and-tear changes in the neck that can slowly squeeze the spinal cord, a condition called degenerative cervical myelopathy. Many older adults undergo a back-of-the-neck operation, called laminectomy, to relieve this pressure. Yet surgeons still struggle to predict who will regain function and who will continue to have difficulty walking, using their hands, or living independently. This study asks a simple but important question: can the curve and tilt of the neck before surgery help forecast recovery afterward?
Understanding a common spine problem in older adults
Degenerative cervical myelopathy develops when joints, discs, and ligaments in the neck thicken and stiffen over time, narrowing the bony tunnel that shelters the spinal cord. People may notice hand clumsiness, unsteady gait, numbness, or bladder problems. In moderate to severe cases, surgery to unroof the spinal cord from behind (laminectomy) is often recommended to stop further damage and allow healing. However, laminectomy can subtly change the neck’s natural curve, raising concerns that some patients may trade compression for a new kind of strain if their spine starts to sag forward after surgery.
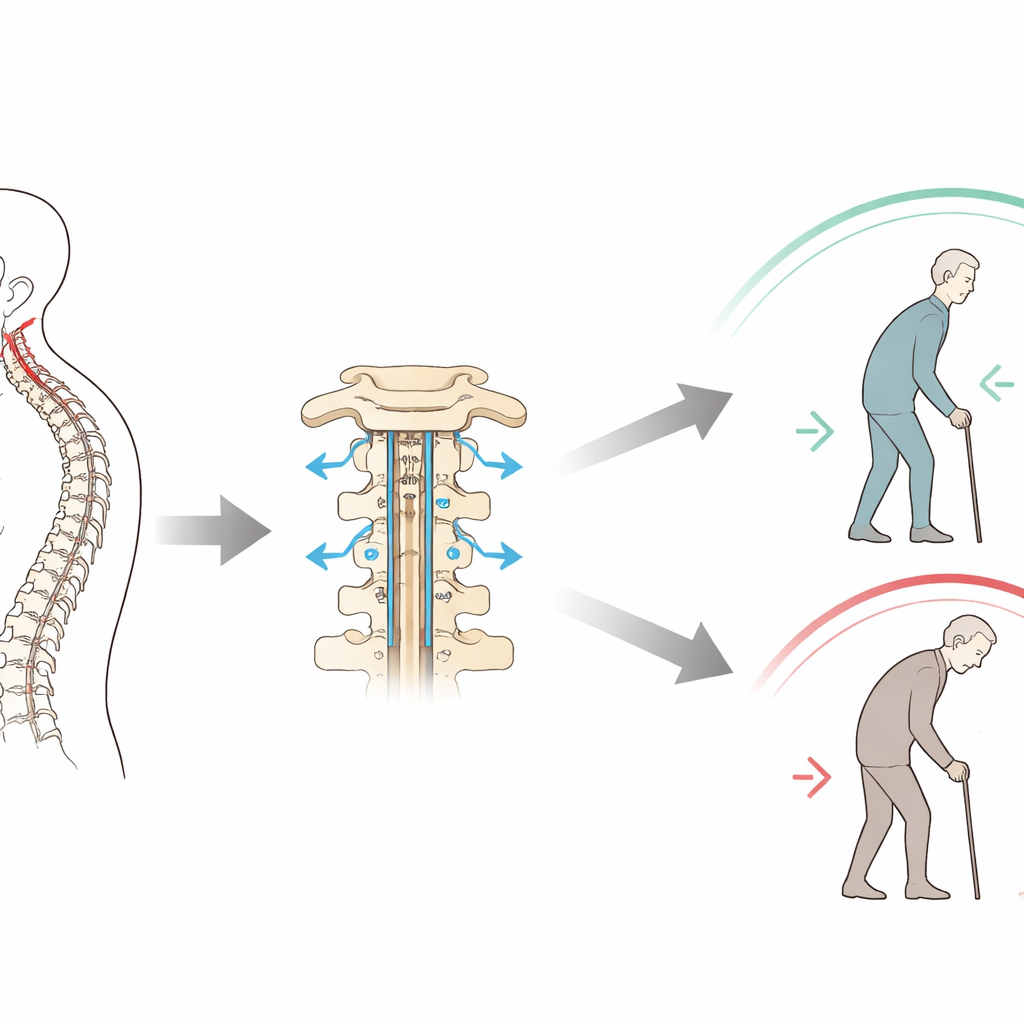
A simple angle that captures neck balance
The authors focused on a single measurement that captures how well the base of the neck and the cervical spine are “in tune” with each other. One angle (the T1 slope) reflects how steeply the top of the upper back tilts; another reflects how much the neck curves backward. Subtracting one from the other produces a mismatch score. A small mismatch suggests that the head is naturally balanced over the shoulders. A large mismatch signals that the neck must work harder to keep the head level, potentially straining muscles and joints. The researchers wondered whether this pre-surgery mismatch could predict who would meaningfully improve after laminectomy.
Following patients through surgery and recovery
The team reviewed 68 adults aged 65 and older who had multilevel laminectomy without added hardware for degenerative cervical myelopathy at a single center in Egypt. All had at least two years of follow-up, with standardized neck X-rays taken before surgery and around the two-year mark. Patients reported pain in the neck and arms on a visual scale, and their ability to walk, use their hands, and manage daily activities was scored using a widely used neurological scale. The main success benchmark was a gain of at least two points on this scale, a change considered clearly noticeable in everyday life.
Who got better and what their necks looked like
Overall, the results were encouraging. More than four out of five patients achieved meaningful functional improvement, and neck and arm pain fell from moderate to mild levels on average. X-rays showed that laminectomy led to a small loss of the neck’s backward curve and a slight increase in the mismatch angle, but not dramatic deformity. When patients were separated into those who improved enough and those who did not, a clear pattern emerged: before surgery, those who went on to do well had smaller mismatch angles and slightly shorter symptom duration. The mismatch angle was a much stronger predictor of outcome than either of its components alone; a larger mismatch steadily lowered the odds of meaningful recovery.
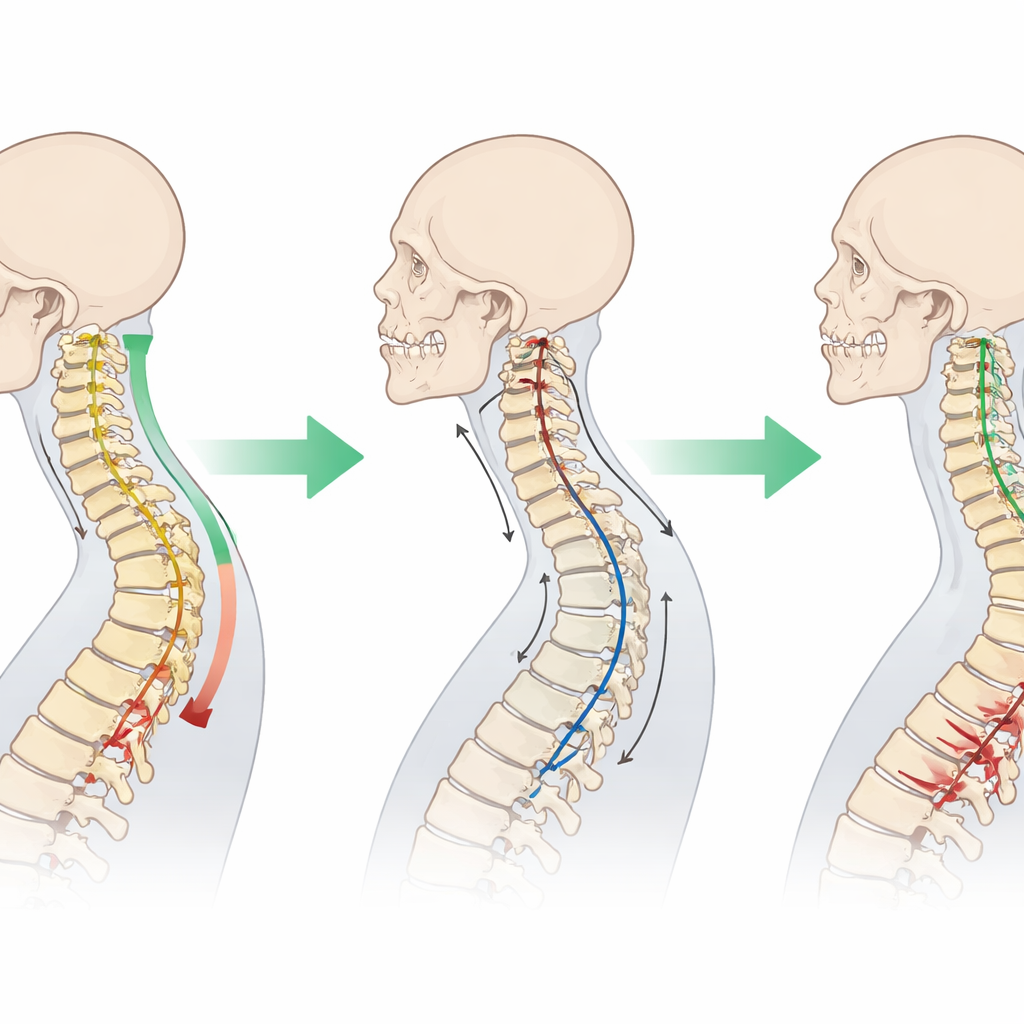
Turning angles into practical decision hints
Using statistical tools, the authors explored how specific mismatch values might guide expectations. A value around the mid-teens was associated with a very high chance of meaningful benefit from laminectomy, suggesting a relaxed, well-balanced neck that tolerates the operation well. Values above about twenty degrees were seen mainly in those with weaker improvement, hinting that these spines may already be working at a mechanical disadvantage. The authors propose a two-step view: low mismatch as a reassuring sign, high mismatch as a caution flag, and an in-between “gray zone” where other clinical details and more complex models should inform decisions.
What this means for patients and surgeons
For older adults facing surgery for spinal cord compression in the neck, this study offers a hopeful message and a note of caution. Most patients in the study improved substantially after laminectomy alone, with acceptable complication rates. At the same time, a simple preoperative angle describing how well the neck’s curve matches the body’s tilt appeared to signal who was most likely to benefit. Because the research comes from one center with a modest number of patients, the authors emphasize that these angle thresholds are not yet firm rules. Still, their work points toward a future in which a quick X-ray measurement could help tailor surgical plans and conversations, moving us closer to more personalized care for an aging spine.
Citation: Ragab, A.M., Taha, M.M., Makkia, M.A.M. et al. Predictive value of preoperative T1 slope minus cervical lordosis for clinical outcomes after standalone laminectomy in elderly degenerative cervical myelopathy. Sci Rep 16, 12356 (2026). https://doi.org/10.1038/s41598-026-46868-1
Keywords: degenerative cervical myelopathy, cervical laminectomy, spinal alignment, elderly spine surgery, surgical outcome prediction