Clear Sky Science · en
Feasibility, acceptability and usability of a thermolabile drugs storage monitoring system at patient’s home: a pilot study
Why keeping some medicines cool really matters
Certain modern medicines, especially many for cancer and immune diseases, must be kept cold almost all the time to work properly. Once these drugs leave the hospital and travel in a shopping bag or sit in a kitchen fridge, no one usually knows if they have ever warmed up too much or frozen by accident. This study tested a simple home monitoring system that quietly watches the temperature around these fragile medicines and warns patients if something starts to go wrong.
The problem with the last step of the cold chain
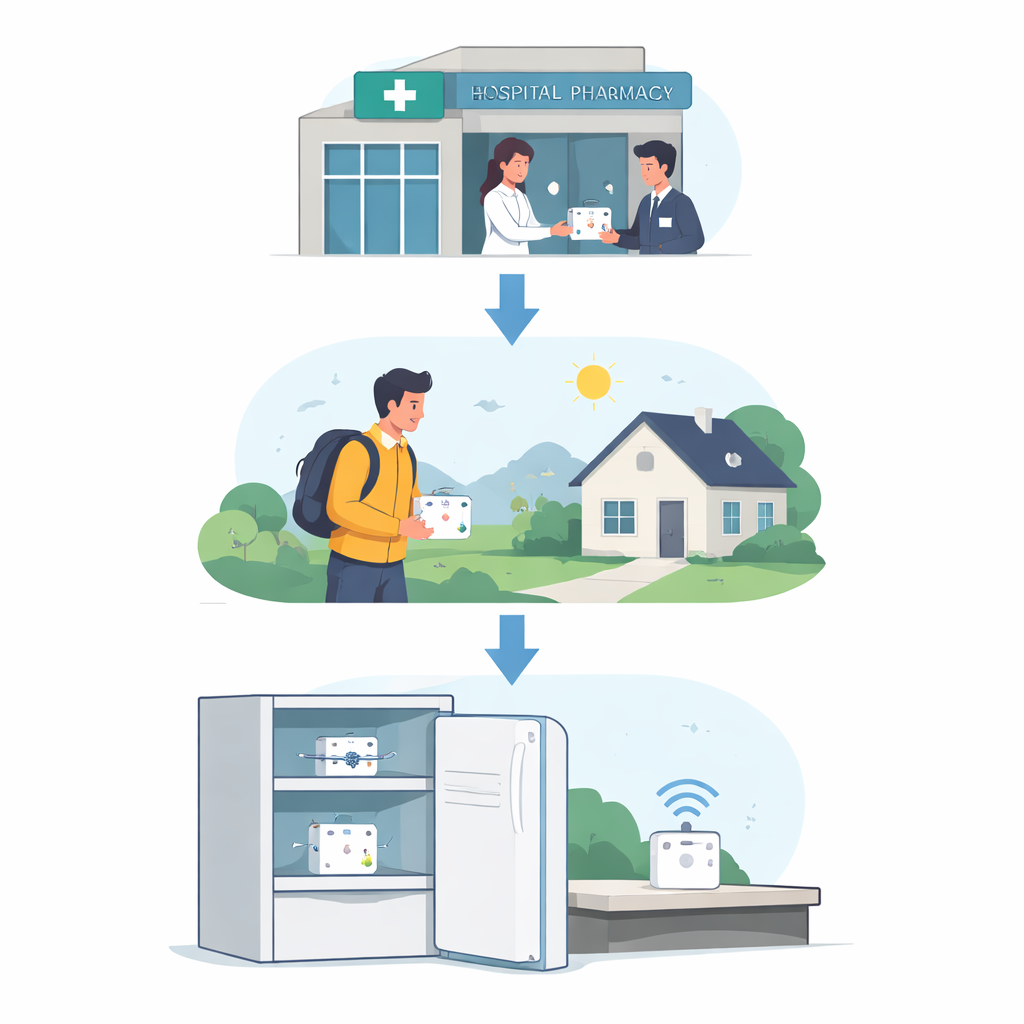
From factory to hospital, strict rules and special equipment keep temperature-sensitive drugs within a narrow safe range, typically a few degrees above freezing. But when a box is finally handed to a patient to take home, that careful control often stops. Earlier research in several countries showed that most people do not keep these medicines within the recommended temperatures, even when they try to follow instructions. Short car trips in hot weather, crowded fridges, or putting the box too close to the freezer compartment can all quietly damage an expensive treatment, reducing its benefit without leaving any visible trace.
A smart sensor that travels with the medicine
To close this weak link, the researchers created QChainMED, a small sensor-based system designed to follow a single box of medicine from the hospital to the patient’s fridge. A sensor, attached to one package, continuously records temperature and other environmental data. At home, a compact gateway device receives these measurements and sends summaries to the hospital using either the household’s WiFi or a long-range, low-power network. The team focused on three phases of the drug’s journey: initialization at the hospital, transport by the patient, and storage in the home refrigerator. The goal was not only to collect data, but also to give timely feedback when conditions drifted toward unsafe zones.
Simple color warnings for everyday use
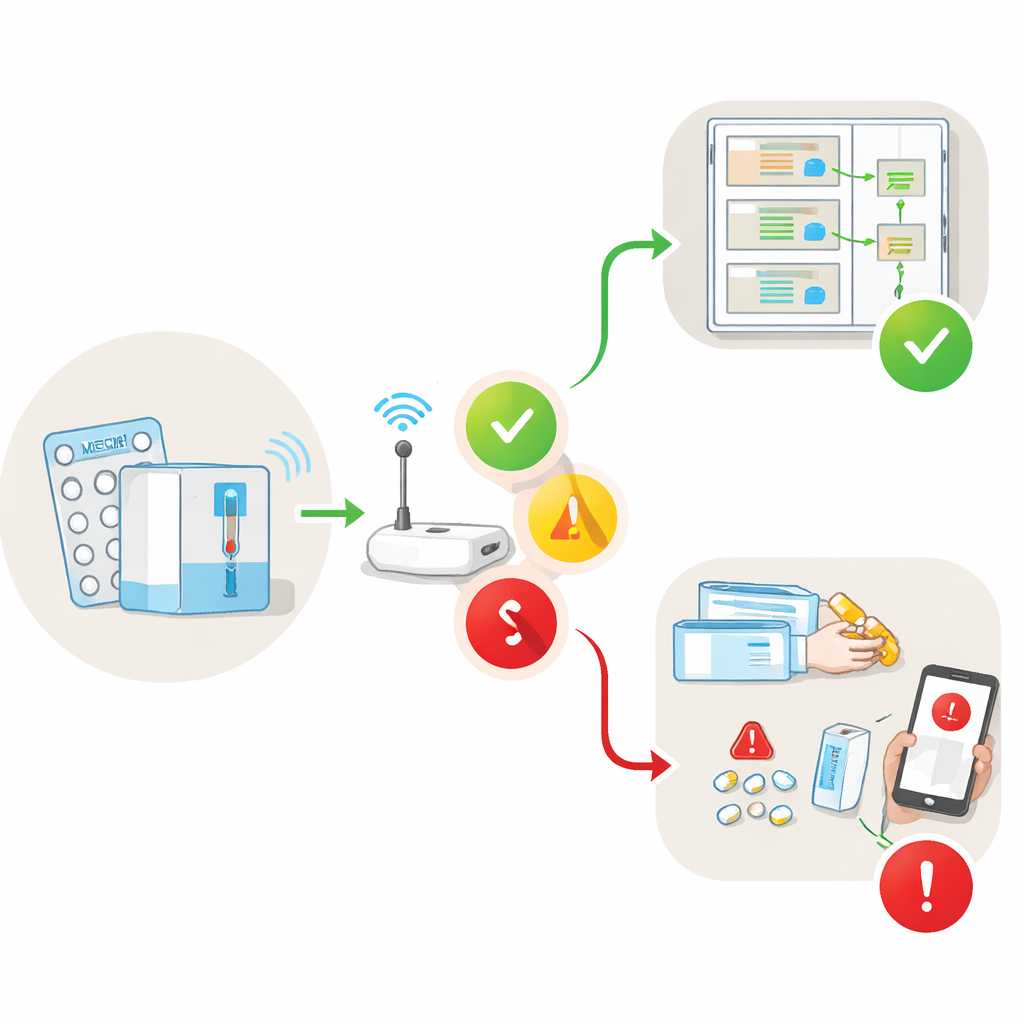
Because each medicine can tolerate only a limited amount of time outside its ideal temperature range, the system keeps a running count of these exposures. Based on this tally, it classifies the situation into three easy-to-understand states. In the safest state, conditions are fine or far below the allowed limit. As exposure time approaches the limit, the system moves into an intermediate warning state, prompting the patient to adjust how or where the drug is stored. If the cumulative exposure goes beyond the safe threshold, the system marks the situation as risky, signaling that the medicine may no longer be reliable. This stepwise approach is designed to encourage early action while still protecting safety when problems persist.
What happened when patients tried it at home
The team invited adults receiving common cold-stored medicines, such as certain treatments for arthritis, high cholesterol, and blood disorders, at a Spanish hospital to use QChainMED. Of 40 people approached, 23 were ultimately enrolled, and most completed the study. Over several weeks, the sensors ran on average for more than two weeks at a time, with some deployments lasting up to almost four months. Technical glitches, mainly brief communication outages, occurred in all systems but did not lead to data loss because information was resent once connections were restored. During the study, 13 alerts were triggered; a few were resolved by patients changing how they stored the medicine, but several progressed to risky conditions, confirming that real problems with home storage do occur.
How patients felt about living with the system
After using QChainMED, participants rated how easy it was to handle and whether they would recommend it to others. On a standard usability survey, the system earned a high score that falls in the range typically labeled “excellent,” similar to well-received health apps and wearable devices. A separate measure that asks whether users would promote the system to friends or family produced a modestly positive result, suggesting that most patients were comfortable with the idea of quiet, background monitoring in their homes. Some people declined participation mainly because they lacked internet access or did not want another device watching their daily life, highlighting practical and personal barriers that future versions will need to address.
What this means for everyday treatment safety
In simple terms, this pilot study shows that a small, affordable sensor system can realistically keep an eye on fragile medicines after they leave the hospital and enter the messy reality of everyday life. Most patients were willing and able to use it, and the system successfully spotted real storage problems that might otherwise have gone unnoticed. While this early work did not measure whether the monitoring actually changes health outcomes, it lays the groundwork for larger studies. If refined and widely adopted, tools like QChainMED could help protect expensive, life-improving treatments from silent temperature damage, giving both patients and pharmacy teams greater confidence that every injection or dose is as effective as intended.
Citation: do Pazo-Oubiña, F., Frontera-Bergas, M., Gomez-Zamora, M. et al. Feasibility, acceptability and usability of a thermolabile drugs storage monitoring system at patient’s home: a pilot study. Sci Rep 16, 10731 (2026). https://doi.org/10.1038/s41598-026-46095-8
Keywords: thermolabile drugs, cold chain monitoring, home medication storage, digital health sensors, patient safety