Clear Sky Science · en
Touch and manual action in chemotherapy-induced peripheral neuropathy: a mixed-methods study
Why this matters for everyday life
Cancer survivors often expect side effects like fatigue or nausea, but many are surprised when their fingers suddenly feel numb, tingly, or painful long after treatment ends. This condition, called chemotherapy-induced peripheral neuropathy, can quietly undermine the simple hand movements we rely on every day—like writing a note, doing up a shirt, or opening a jar. This study listens closely to patients’ own stories and then uses knowledge of how the hands and brain work together to explain why some everyday tasks become especially tricky, and how future tests and treatments might better target these problems.
Changes in feeling after treatment
The researchers worked with 25 adults who had developed nerve-related side effects from chemotherapy, most of whom still felt symptoms in their hands several years after treatment. People commonly described numbness and tingling in their fingertips, sometimes joined by sharp or burning pain. For some, these sensations improved over time, but for many they stayed the same or even worsened. Participants explained that it was often the very tips of the fingers that felt most affected—the same area we normally use for the finest, most delicate touch.
Everyday tasks that become unexpectedly hard
Using questionnaires and online discussion groups, the team asked which daily activities were most disrupted. Three stood out: holding a pen to write, fastening small buttons, and opening jars or bottles. Many people also struggled with other two-handed tasks like tying shoelaces, doing up buckles or jewellery, sewing, or handling fragile objects such as crockery. Some reported dropping things because they misjudged their grip, or feeling clumsy when picking up small items or turning pages. Others found that using touchscreens, phones, or keyboards could be harder, especially when their hands were cold, painful, or especially numb. 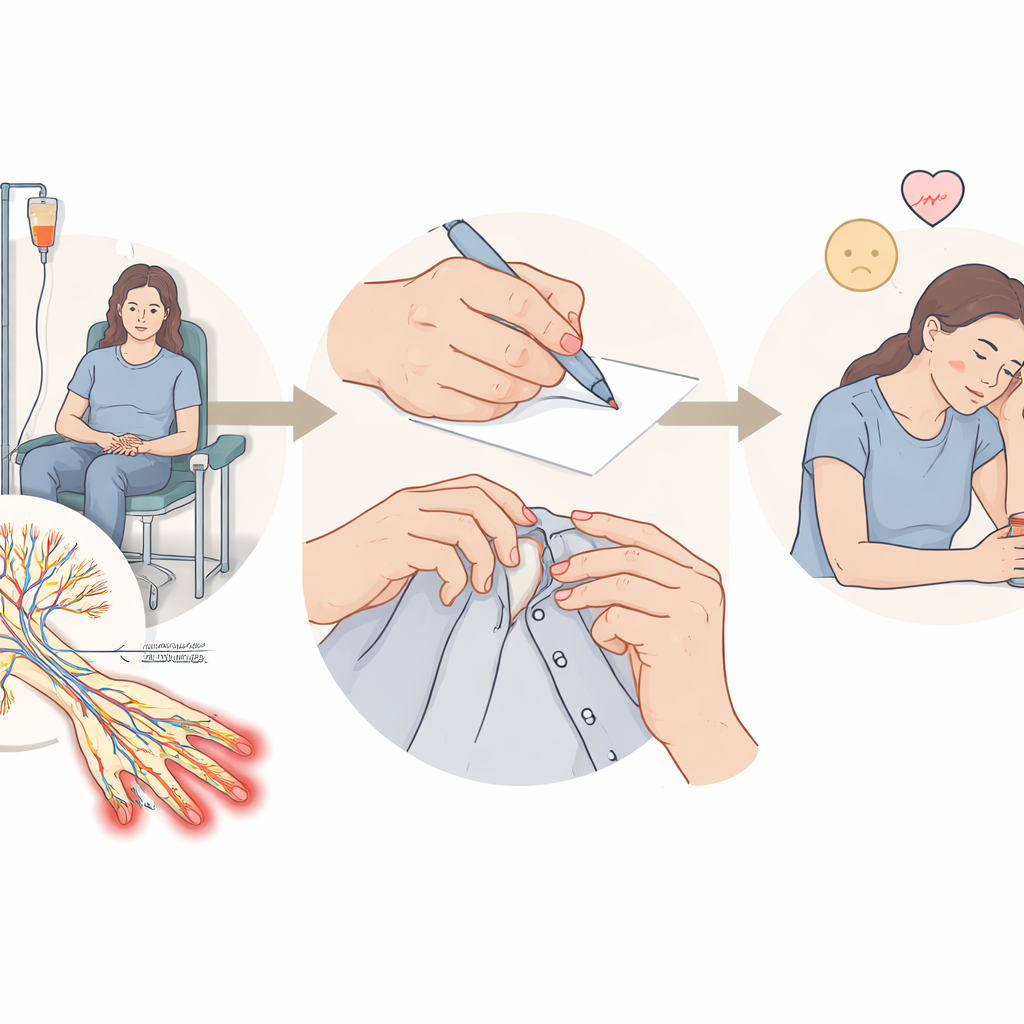
What is going on inside the hand
To make sense of these reports, the authors drew on what is known about how our nervous system controls hand movements. When we pinch a pen, a button, or a jar lid, the skin on our fingertips senses tiny changes in pressure and vibration as we push and pull. The brain uses this information to fine-tune grip: squeeze just hard enough so the object does not slip, but not so hard that it hurts or becomes tiring. In neuropathy, damaged nerves dull or distort these signals, so the brain gets poorer feedback about what the fingers are doing. That can lead to slips, dropped objects, or the need to grip much harder, which in turn can cause pain—especially in cold conditions or with rough surfaces.
Why some tasks are worse than others
By comparing tasks, the researchers developed ideas about what makes certain actions especially vulnerable. Buttoning a shirt, for example, demands very precise fingertip control from both hands at once: the button must be guided through a tight hole using tiny movements at the very skin area where touch loss is greatest. Writing also relies on fine control, but usually with one hand and over a larger contact area, so it may be slightly less affected. Opening jars, by contrast, requires less precision but much more force. Here, dry or damaged skin may reduce friction, so people must squeeze harder, which can be painful and still not prevent slipping. These different demands—precision, force, number of fingers involved—help explain why patients’ difficulties cluster around particular everyday actions. 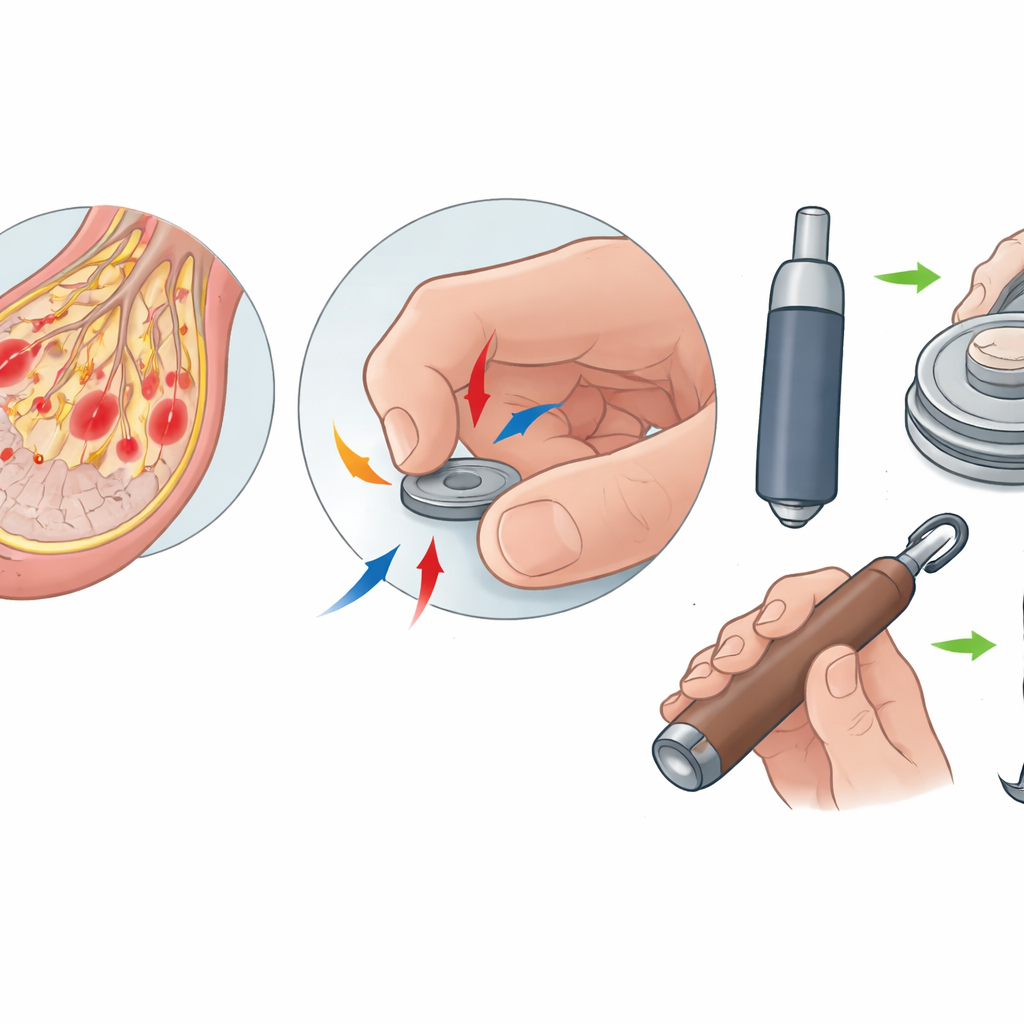
Finding ways to adapt and improve care
Participants described practical coping strategies: wearing gloves to keep hands warm, rubbing the skin to “wake up” sensation, switching to thicker or textured pens and yarns, using jar openers or button hooks, moving more slowly, or relying more on vision or “muscle memory” instead of touch. The authors argue that current clinical tests, which often focus on simple measures like feeling light pressure or vibration, do not fully capture these real-world struggles. They suggest that future assessments should include hands-on tasks that measure how well people can grasp, move, and manipulate objects, as well as precise recordings of grip forces and movement patterns. In plain terms, the study concludes that chemotherapy-related nerve damage in the hands does not just change how things feel—it changes how people can act on the world. Understanding this link between touch and action, and measuring it objectively, could lead to better support, better tools, and better treatment decisions for people living with these long-lasting side effects.
Citation: Roberts, R.D., Chua, W., Khatibi, A. et al. Touch and manual action in chemotherapy-induced peripheral neuropathy: a mixed-methods study. Sci Rep 16, 10689 (2026). https://doi.org/10.1038/s41598-026-46039-2
Keywords: chemotherapy side effects, peripheral neuropathy, hand dexterity, touch and sensation, cancer survivorship