Clear Sky Science · en
Can classification strategies improve automated cervical vertebral maturation staging? A comparative study
Why the timing of a growth spurt matters
For children and teenagers who need braces or jaw correction, catching the body’s natural growth spurt at the right moment can make treatment smoother, shorter, and more effective. Dentists often look at spine bones in ordinary head X-rays to estimate how far along a young person is in their growth. But these visual checks can be inconsistent, with different specialists sometimes giving different answers. This study asks whether carefully designed artificial intelligence (AI) systems can read those X-rays more consistently—and how best to train such systems.
Reading growth from neck bones
When orthodontists plan treatment, they do not just look at teeth. They also need to know how much growing a patient has left to do. One common method is to examine the small neck bones called cervical vertebrae on a side-view X-ray of the head. Their shapes subtly change as a child moves from early growth, through a pubertal growth spurt, and into late adolescence. A popular system divides this change into six steps, but the differences between neighboring steps can be so slight that even experienced doctors often disagree. This variability makes it hard to standardize care and to confidently time treatments that depend on catching the growth spurt.
Teaching computers to spot subtle shape changes
The researchers assembled 1,750 routine orthodontic X-rays from one hospital, covering patients with an average age of about 13 years. Two board-certified orthodontists independently assigned each image to one of the six growth stages and then resolved any disagreements together, creating a trusted reference. A computer vision model first found and cropped the small region of the image containing three neck vertebrae. These cropped images were then fed into deep learning systems—specialized AI programs that learn patterns directly from many examples—to predict the growth stage.
Do expert hints help or get in the way?
The team compared two main training ideas. In one, the AI learned end-to-end: it saw only the cropped vertebra images and directly learned to predict the six growth stages. In the other, the AI was first trained to find specific landmark points on the vertebrae—key positions along their edges that human experts use—and only afterward retrained to classify growth stage, reusing what it had learned about those landmarks. Surprisingly, the direct end-to-end approach did better. It correctly identified the exact six-stage category about two-thirds of the time, and when it made mistakes, they almost always fell into a neighboring stage. The landmark-guided versions never quite caught up, even when their internal layers were more thoroughly adjusted during retraining.
Fine detail training for broader clinical decisions
In everyday practice, orthodontists often do not need all six stages. Instead, they care about three broader phases: before, during, and after the pubertal growth spurt. The researchers therefore tested whether it was better to train a model directly on these three groups, or to first train on the full six-step scale and then merge its outputs into three. Both approaches reached similar overall accuracy of around 79 percent, but the model that started with the finer six-step training paid more attention to the exact vertebra features that clinicians rely on, such as the lower borders and the hollowing of the bone edges. Visual maps of what the AI “looked at” showed tighter focus on these meaningful shapes, while the directly trained three-step model spread its attention more broadly to less relevant areas.
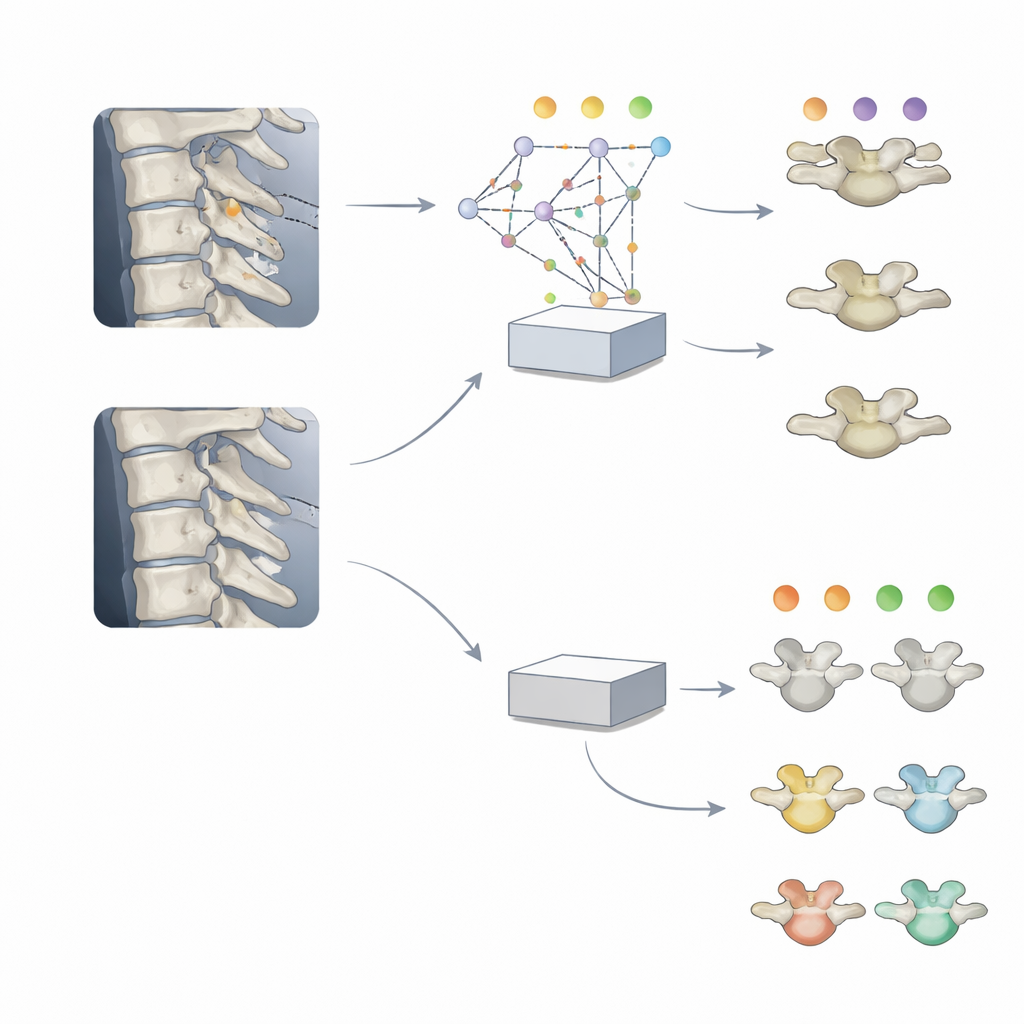
What this means for future dental care
This study suggests that AI can grade growth from routine orthodontic X-rays with errors mostly confined to neighboring stages, much like the natural uncertainty human experts face. It also shows that giving the computer pre-programmed anatomical hints is not always helpful and can even hold it back if those hints do not match the final task. By contrast, training on more detailed growth stages, even when only broad categories are needed in the clinic, can lead to models that look at the same features human specialists use. In the long run, such carefully trained systems could support orthodontists in timing treatment more consistently and transparently, making better use of each patient’s growth spurt while still leaving final decisions in human hands.
Citation: Lee, SY., Ryu, J., Kim, YH. et al. Can classification strategies improve automated cervical vertebral maturation staging? A comparative study. Sci Rep 16, 10645 (2026). https://doi.org/10.1038/s41598-026-46004-z
Keywords: skeletal maturity, orthodontic growth, deep learning, medical imaging AI, cervical vertebrae