Clear Sky Science · en
Fixel-based analysis reveals whole-brain white matter microstructural alterations in axial spondyloarthritis
Why back disease and the brain are connected
Axial spondyloarthritis is best known as a painful inflammatory disease of the spine and pelvis. Yet many people with this condition also struggle with fatigue, poor sleep, and low mood. This study asks a simple but important question: does long‑lasting inflammation in the body quietly reshape the brain’s wiring, and could that help explain these hidden burdens? Using a new kind of MRI analysis that looks closely at the brain’s communication cables—its white matter—the researchers mapped subtle changes across the whole brain in young adults with axial spondyloarthritis.
Looking inside the brain’s wiring
Instead of focusing only on painful joints, the team scanned the brains of 39 people with axial spondyloarthritis and 41 healthy volunteers of similar age and sex. They used diffusion MRI, which tracks how water moves along bundles of nerve fibers, and then applied a technique called fixel‑based analysis. Rather than treating each tiny block of brain tissue as a single structure, this approach can separate different fiber bundles that cross through the same spot. It measures how tightly packed the fibers are and how thick each bundle is, allowing scientists to detect whether white matter is thinning, staying stable, or even expanding.
Where the brain looked different
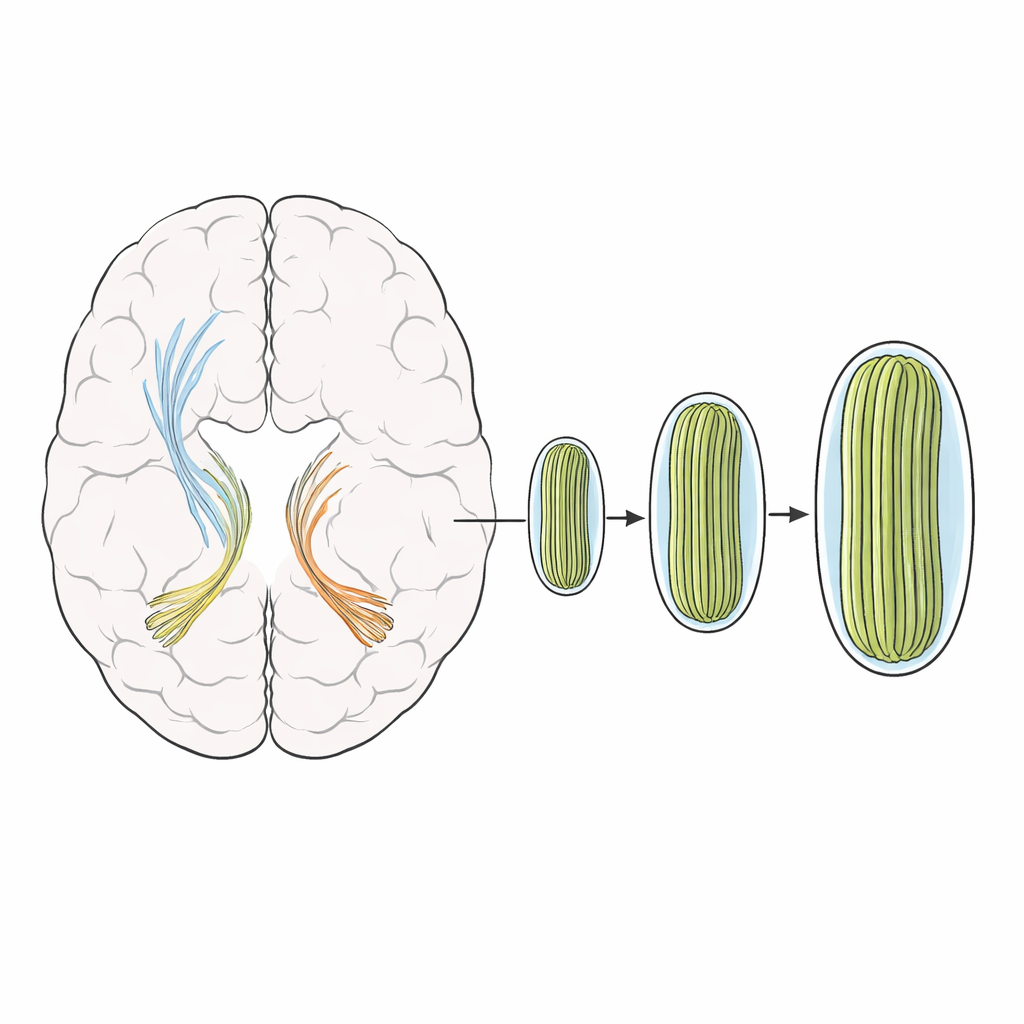
The scans revealed that people with axial spondyloarthritis had slightly larger cross‑sections of certain white matter bundles, mainly in the so‑called external capsule on both sides of the brain and in a pathway called the uncinate fasciculus on the right. These tracts help link frontal brain regions with deeper structures involved in movement, decision‑making, memory, and emotion. Interestingly, the density of fibers within these bundles did not drop, suggesting that the tissue was not being lost or frayed. Instead, the affected tracts appeared subtly enlarged, hinting at structural remodeling rather than outright damage. When the researchers re‑ran their analyses after excluding patients taking biologic drugs, the same pattern appeared, suggesting that medication alone could not explain the findings.
What these changes might mean
Why would white matter bundles thicken in a disease driven by inflammation? One possibility is that ongoing immune activity in the body spills over into the brain. Inflammatory molecules can loosen the blood–brain barrier, activate support cells such as microglia and astrocytes, and trigger local tissue growth. Animal studies show that this phase of inflammation can actually increase tissue volume before any shrinkage sets in. The authors argue that the enlarged bundles they observed may reflect such an early, potentially reversible stage of brain involvement—more like overgrown wiring than worn‑out cables. Because standard diffusion imaging methods missed these differences, the work also demonstrates that more refined tools are needed to capture these nuanced brain changes.
Links to daily life and symptoms
The participants with axial spondyloarthritis reported worse physical function, more bodily pain, poorer sleep, and higher anxiety than healthy volunteers, underscoring how deeply the disease affects everyday life. The researchers then tested whether the altered white matter measures tracked with symptoms such as pain levels, quality of life, mood, or routine blood tests of inflammation. A weak hint emerged that people with slightly larger bundles in the left external capsule might perform better physically, but this trend vanished after strict statistical correction. Overall, the brain changes did not show clear one‑to‑one links with specific complaints, suggesting that larger studies—or more specialized cognitive and emotional testing—will be needed to connect structure and experience more firmly.
What this means for people with spinal arthritis
For people living with axial spondyloarthritis, these findings add an important piece to the puzzle: the disease appears to touch the brain’s wiring, even in relatively young adults, but in a way that looks more like remodeling than degeneration. Rather than showing early signs of tissue loss, the key white matter pathways involved in movement planning and emotion appear slightly bulked up, possibly as a response to the constant inflammatory environment. This raises the possibility that advanced MRI measures could one day serve as sensitive markers of how the disease affects the nervous system and how it responds to treatment. It also reinforces a broader message: conditions that begin in the joints can reach far beyond them, shaping how the brain is built and, ultimately, how people feel and function.
Citation: Wang, W., Yang, Y., Xue, Y. et al. Fixel-based analysis reveals whole-brain white matter microstructural alterations in axial spondyloarthritis. Sci Rep 16, 14271 (2026). https://doi.org/10.1038/s41598-026-45157-1
Keywords: axial spondyloarthritis, brain white matter, neuroinflammation, diffusion MRI, structural remodeling