Clear Sky Science · en
SPIONs-labeled hUCMSCs for in vitro safety analysis and in vivo tracking in scarred monkey uteri
Why this research matters
As cesarean births become more common worldwide, many women are left with lasting scars in the wall of the uterus. These scars can make later pregnancies riskier, raising the chances of complications like abnormal placental growth or even uterine rupture. Doctors and scientists are exploring stem cells as a way to help damaged uteruses heal more completely, but one big question remains: once stem cells are placed into the body, where do they go and how long do they stay? This study tests a way to label human stem cells with tiny iron particles so they can be safely followed inside the body using standard hospital MRI scanners.
Tiny helpers from the umbilical cord
The team focused on a particular type of stem cell taken from leftover human umbilical cords, usually discarded after birth. These cells can multiply well, turn into several kinds of tissue, and tend to trigger fewer immune reactions than cells taken from adult organs. Because of these advantages, they are front-runners for future treatments to repair the uterine wall after cesarean section. To make them visible on MRI scans, the researchers mixed the cells in the lab with superparamagnetic iron oxide nanoparticles—extremely small iron-containing spheres coated with a friendly polymer so they disperse well in water and are gentle on cells.
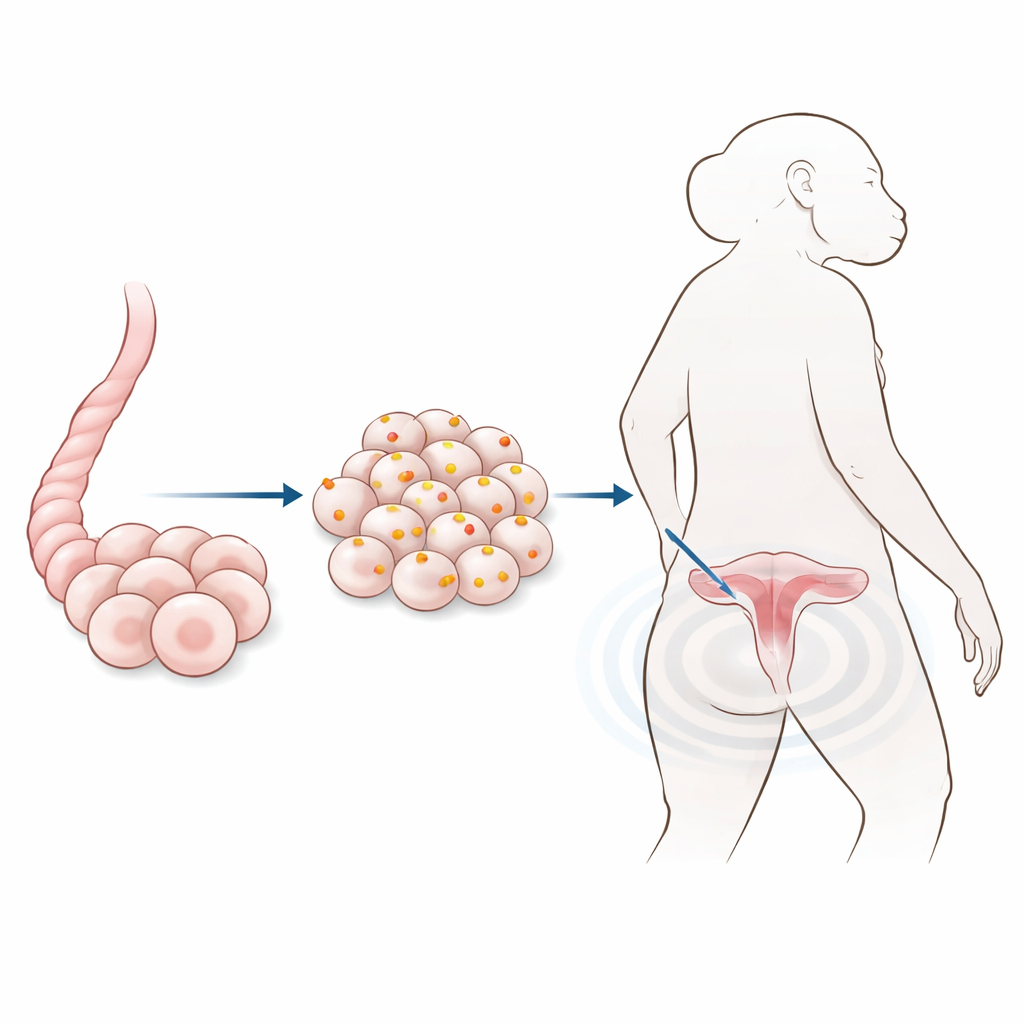
Checking that labeling does not harm the cells
Before using the labeled cells in animals, the scientists had to make sure the iron particles did not damage the stem cells or change their behavior. They exposed the cells to a range of particle doses and then ran a series of standard laboratory tests. Under the microscope, labeled cells kept their normal shape. Special stains and electron microscopy confirmed that iron particles were taken up into small pockets within the cell fluid. Over a week of growth, cell survival and division were similar across most doses, and in some cases slightly better than in unlabeled cells. The labeled cells could still mature into fat, bone, and cartilage–like cells, and they kept the same pattern of surface markers and internal proteins that define this stem cell type.
Following the cells inside monkey uteruses
To mimic the human situation as closely as possible, the researchers used cynomolgus monkeys, whose reproductive organs and body systems resemble ours. The animals first underwent cesarean delivery to create a realistic uterine scar. Six months later, the team injected the iron-labeled stem cells into several locations in the uterine wall. Using a clinical 3‑tesla MRI scanner, they imaged the abdomen repeatedly: one day, one week, about one month, and almost two years after injection. The labeled cells appeared as dark spots against the brighter uterine tissue, and these spots stayed in the same place for more than 600 days, especially where higher iron doses had been used.
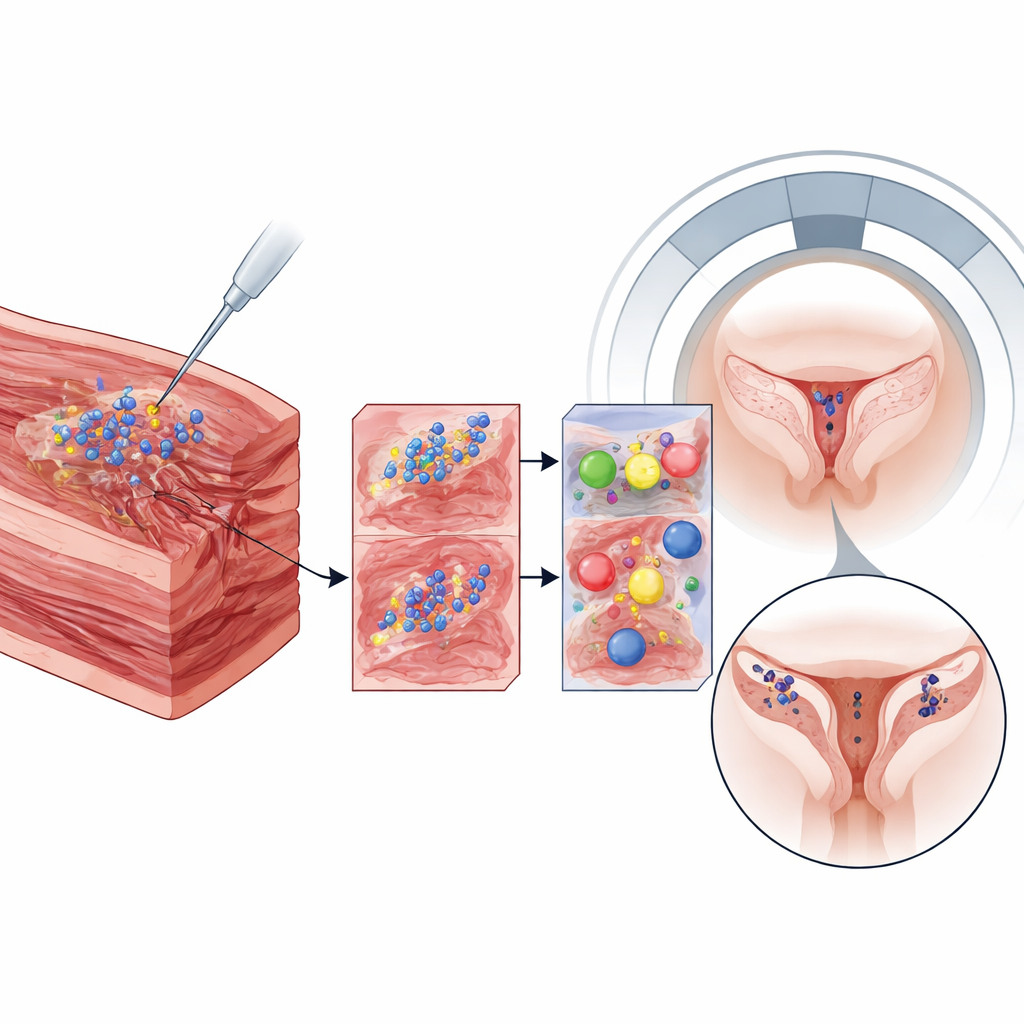
Safety checks inside organs and tissue
Tracking the labeled cells was only half the story; the other half was safety. The monkeys remained healthy for over two years after surgery and injection. Extra MRI scans of the brain, kidneys, and other major organs showed no abnormal dark regions that would suggest iron buildup elsewhere. When the study ended, the researchers examined the uteruses under the microscope. Usual tissue stains showed normal cell shapes and scar structure, with no obvious damage linked to the iron particles. A special iron stain revealed blue dots in the injection regions, confirming that particles were still present locally, likely inside a mix of surviving stem cells and nearby immune cells, but without clear signs of toxicity.
What this could mean for future treatments
Overall, the work shows that umbilical cord stem cells can be loaded with iron nanoparticles and used as long-lasting beacons on MRI scans without clearly harming the cells themselves or the surrounding monkey tissues. For patients, this approach does not yet fix the problem of uterine scars on its own, and it does not prove that transplanted stem cells survive for years. Instead, it offers a powerful way for doctors and researchers to see where stem-cell-based treatments actually reside in the body and for how long, using noninvasive imaging tools already present in many hospitals. That tracking ability will be crucial for safely developing future therapies aimed at helping scarred uteruses—and possibly other organs—heal more completely.
Citation: Ma, H., Wan, Y., Shen, X. et al. SPIONs-labeled hUCMSCs for in vitro safety analysis and in vivo tracking in scarred monkey uteri. Sci Rep 16, 14199 (2026). https://doi.org/10.1038/s41598-026-45156-2
Keywords: uterine scar repair, stem cell tracking, iron oxide nanoparticles, MRI imaging, cesarean section