Clear Sky Science · en
Short-term intermittent hypoxia induces biphasic apoptotic responses in the murine heart
Why this matters for people who snore
Obstructive sleep apnea, a common condition where breathing stops and starts during sleep, repeatedly deprives the body of oxygen. This study in mice asks a simple but important question for anyone worried about snoring and heart health: do these short drops in oxygen briefly help the heart toughen up, or do they start harming it right away?
Sleep, oxygen dips, and the heart
In sleep apnea, the airway collapses over and over, causing intermittent hypoxia, or repeated cycles of low and normal oxygen. Doctors know that people with untreated sleep apnea have a higher risk of high blood pressure, heart disease, irregular heartbeats, and heart failure. What has been less clear is how quickly the heart begins to respond to these oxygen swings, and whether the first changes are protective or harmful.
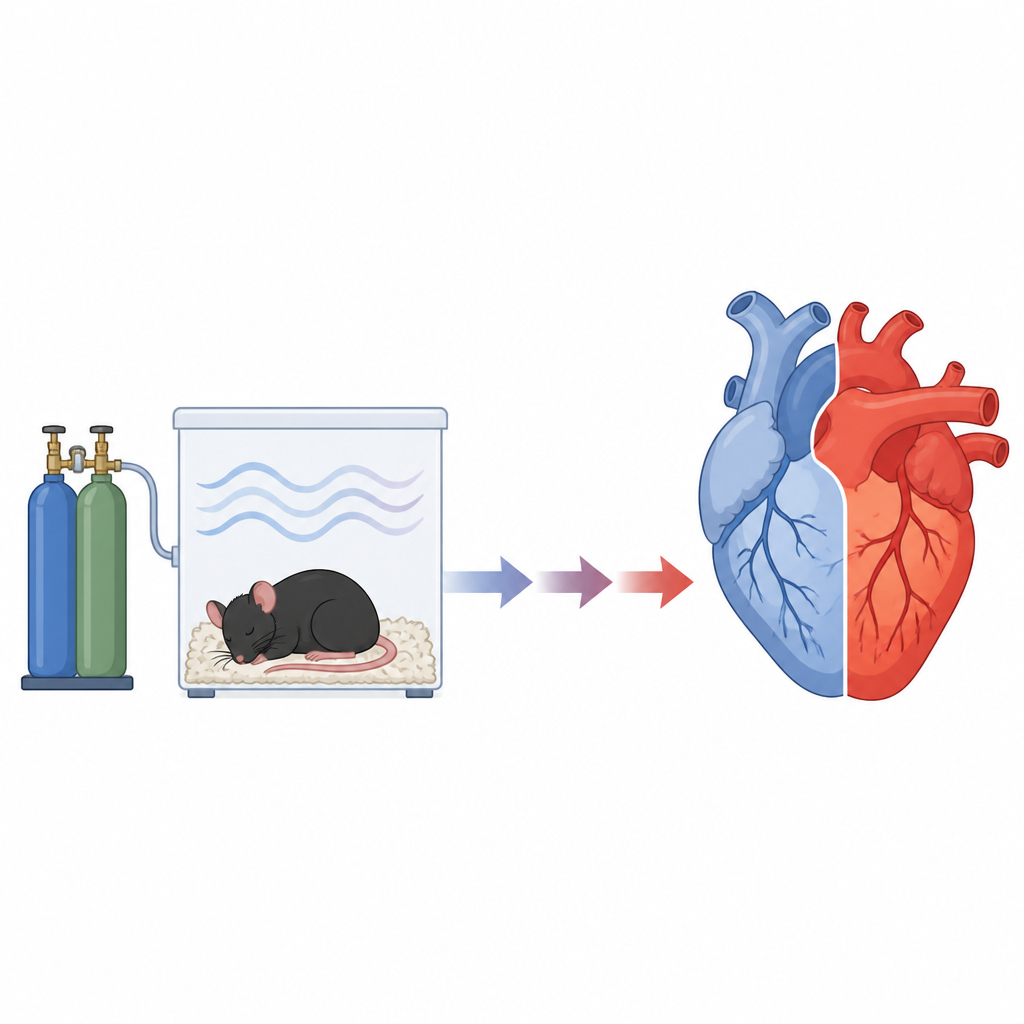
How the study was set up
The researchers used healthy adult male mice and exposed them to controlled cycles of normal and low oxygen that mimic sleep apnea. One group breathed normal air, while other groups spent 8 hours per day in a chamber where oxygen levels alternated every 30 seconds between normal and low. Some mice experienced this for just one day, while others went through seven days. Afterward, the scientists examined different parts of the heart under the microscope and measured key proteins that signal whether cells are trying to survive or are moving toward programmed cell death.
A short boost turns into damage
The heart’s response turned out to be two phased. After just one day of intermittent low oxygen, the hearts actually showed fewer dying cells than normal, and higher levels of a protein that helps cells resist death. This pattern resembles a well known effect called preconditioning, where brief, mild stress can make heart cells more resilient to later injury. However, by seven days, the picture flipped. The number of dying cells rose sharply, especially in the right side of the heart, which pumps blood to the lungs. At the same time, proteins that push cells toward self destruction increased, and stress-related signals became stronger, indicating that the heart was now being injured rather than protected.
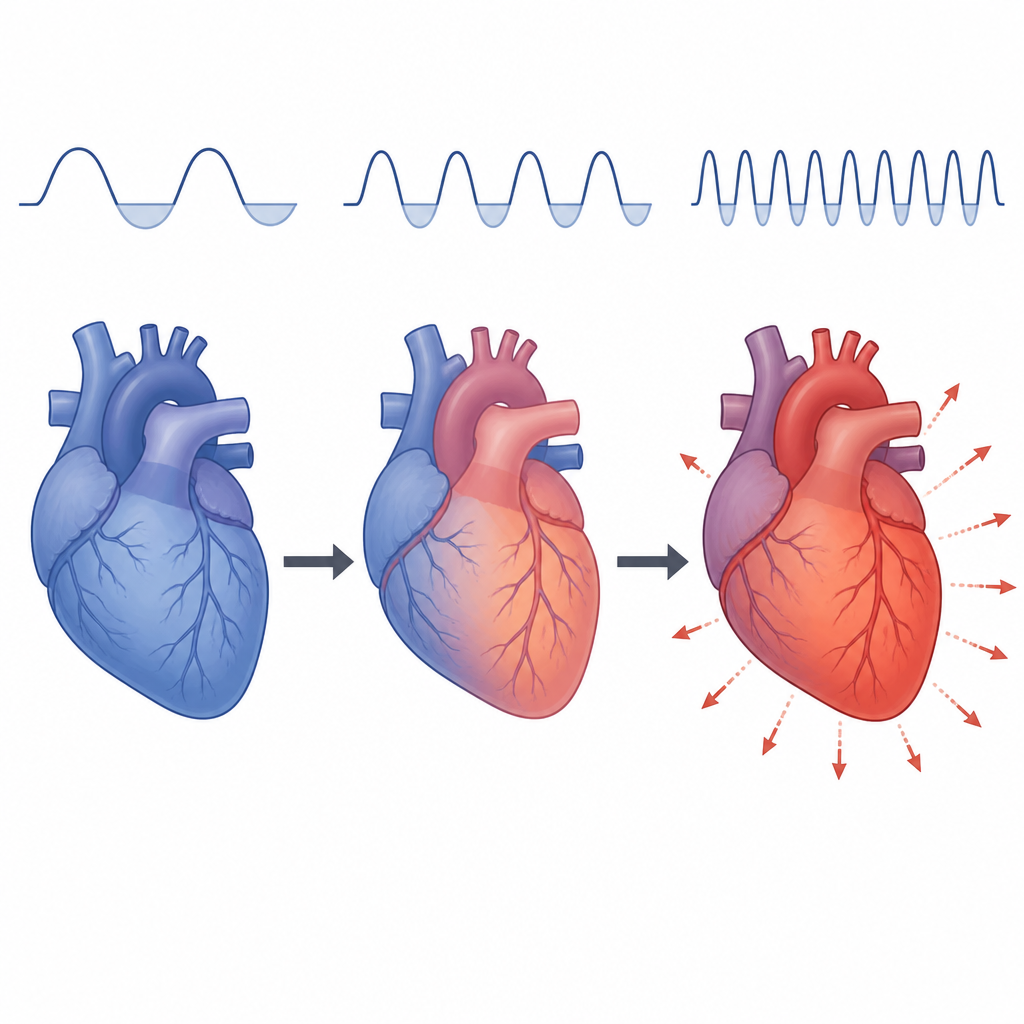
Early warning signs without scarring
Even though more heart cells were dying after a week of intermittent low oxygen, the heart tissue did not yet show obvious scarring or thick bands of collagen, which are hallmarks of long term damage. The overall structure of the heart muscle stayed mostly intact. This suggests that increased cell death appears before lasting structural changes, offering a potential early warning stage when harm might still be reversible if the underlying cause, such as untreated sleep apnea, is addressed.
What this may mean for people with sleep apnea
For a layperson, the main takeaway is that brief, mild bouts of low oxygen might temporarily trigger the heart’s self defense systems, but continuing to expose the heart to these nightly oxygen swings likely shifts the balance toward cell loss and future heart problems, particularly in the right side of the heart. While this work was done in mice and does not directly translate into treatment advice, it strengthens the idea that the duration and intensity of oxygen drops in sleep apnea matter greatly for heart health, and that there may be a window of time during which preventing or reducing these episodes could help protect the heart from longer term damage.
Citation: Arbatli, S., Peker, Y. Short-term intermittent hypoxia induces biphasic apoptotic responses in the murine heart. Sci Rep 16, 14974 (2026). https://doi.org/10.1038/s41598-026-45151-7
Keywords: intermittent hypoxia, sleep apnea, heart apoptosis, right ventricle, cardiac remodeling