Clear Sky Science · en
Combined PLGA scaffolds and therapeutic stem cells for locomotion recovery in spinal cord-injured rats: a systematic review and meta-analysis
Why Fixing Broken Spinal Cords Matters
Spinal cord injury can turn a split-second accident into a lifetime of paralysis, pain, and medical dependence. Current treatments help stabilize the spine and limit early damage, but they rarely restore lost movement. This article looks at an emerging strategy that combines two powerful tools—biodegradable scaffolds and stem cells—to help injured spinal cords in rats rebuild the nerve connections needed for walking. By pulling together results from many animal studies, the authors ask a simple but crucial question: does this combo really work better than existing experimental approaches on their own?
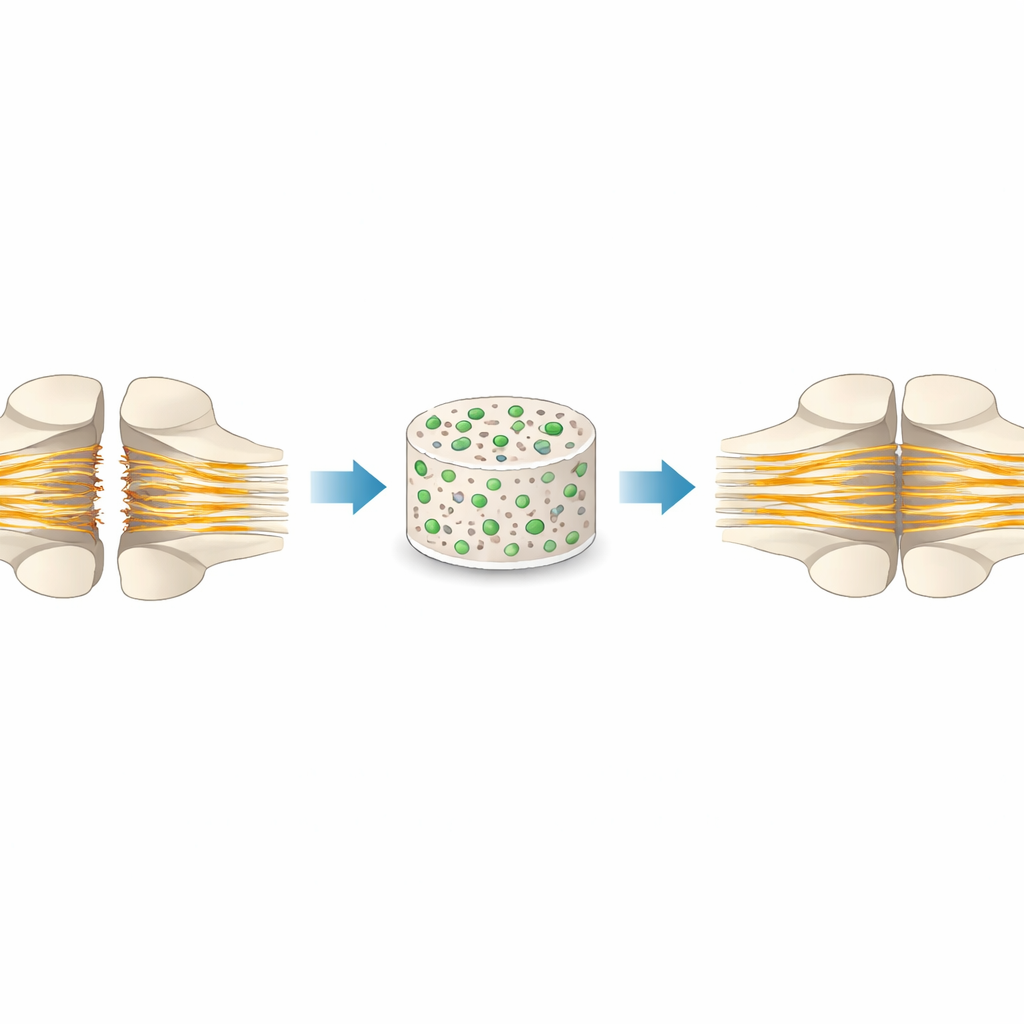
A Tiny Bridge for a Big Gap
After a severe spinal cord injury, the central nervous system is left with a gap filled by scars and fluid-filled cavities that block nerve regrowth. The authors focus on scaffolds made from PLGA, a biodegradable plastic already used in medical devices. Shaped into porous structures, these scaffolds can be placed into the injury site like a tiny bridge, providing physical support so nerve fibers have something to grow along. Because PLGA breaks down safely inside the body and its stiffness and structure can be tuned, it is an attractive base material for engineering new tissue inside the damaged cord.
Helping Cells Settle, Survive, and Heal
On their own, transplanted stem cells often die quickly or fail to connect properly inside the hostile environment of an injured spinal cord. The idea behind combining them with PLGA scaffolds is to give these cells a supportive home. The studies included in this review used different types of therapeutic stem cells, mainly bone marrow mesenchymal stem cells, neural stem cells, and induced pluripotent stem cells. Seeded onto the scaffold and then implanted into the injury, these cells are expected to stick to the structure, live longer, and send out helpful signals that calm inflammation, protect surviving nerve cells, and encourage new nerve fibers and blood vessels to grow through the damaged area.
What the Animal Studies Show
The authors systematically searched the scientific literature and found 14 rat studies that met strict inclusion rules. Together, these studies involved 385 animals and compared several groups: no treatment, scaffold alone, stem cells alone, and the combined scaffold-plus-cell therapy. Across all experiments, rats receiving the combined treatment regained more movement in their hind limbs than those in any of the other groups. The improvements were measured using a common rating scale for rodent walking ability. Although the exact size of the benefit varied from study to study, the overall trend strongly favored the combination over doing nothing, using just the scaffold, or giving only stem cells.
Which Ingredients Work Best
Diving deeper, the review examined which design choices seemed most promising. Scaffolds made by an electrospinning technique—producing fine, aligned fibers that resemble the spinal cord’s natural support mesh—gave more consistent results than other fabrication methods. Among the cell types, bone marrow mesenchymal stem cells stood out: when combined with PLGA scaffolds, they reliably improved movement compared with no treatment and appeared more practical for future human use. In contrast, pairings with neural stem cells did not clearly outperform controls, and combinations using induced pluripotent stem cells sometimes did no better—or even worse—than scaffolds alone. Higher cell doses and the use of immune-suppressing drugs also failed to add clear benefits, suggesting that more is not always better.
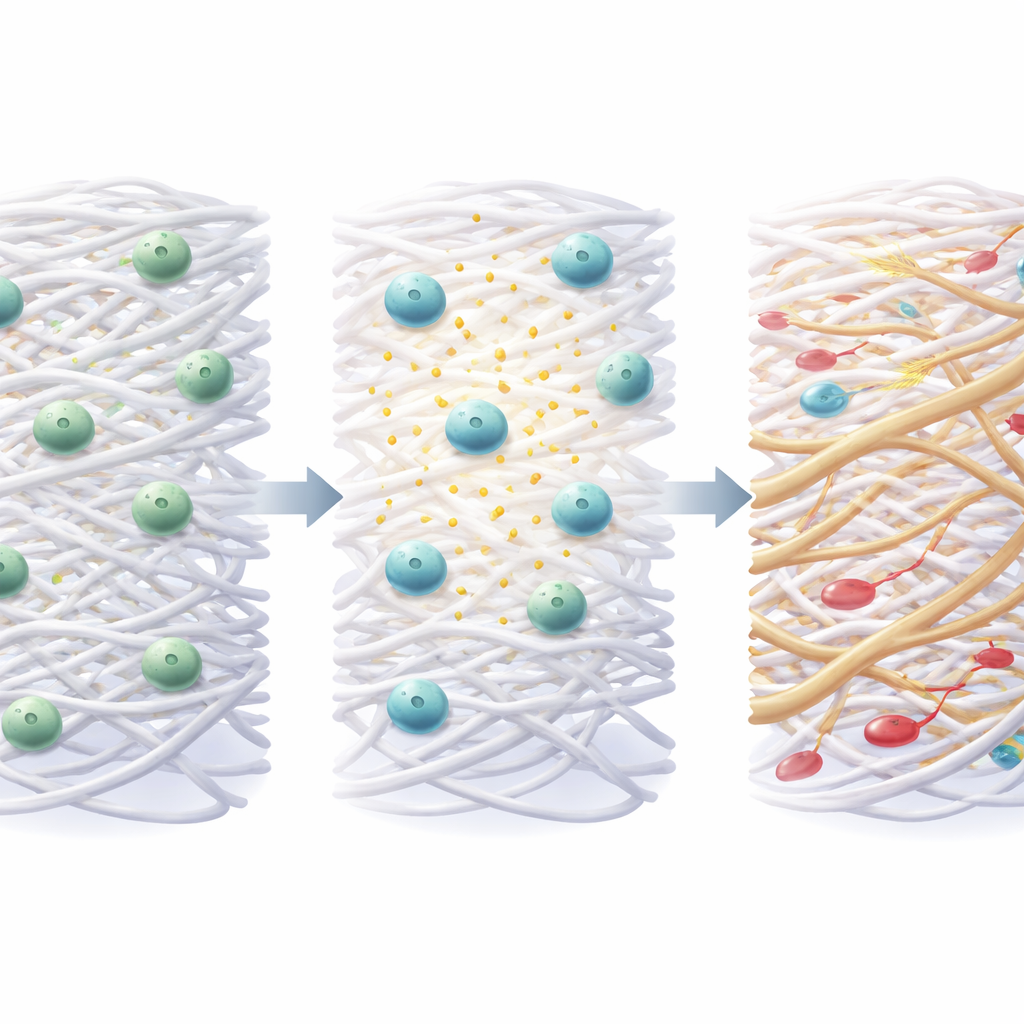
From Rat Lab to Hospital Ward
The authors conclude that PLGA scaffolds loaded with bone marrow stem cells, especially in electrospun form, represent a particularly promising recipe for repairing traumatic spinal cord injury in rats. The scaffold acts as a bridge and support, while the cells provide healing signals that together boost recovery of walking. Still, they caution that animal experiments are highly controlled and often exaggerate how big an effect looks when translated into human terms. People with spinal injuries differ widely in age, injury type, and health, and their spinal cords are larger and more complex than those of rats. Moving this approach into the clinic will therefore require careful optimization of scaffold design, cell dose, and timing, followed by rigorous trials to make sure the therapy is both safe and truly helpful for patients living with paralysis.
Citation: Tang, L., Xie, Q., Li, S. et al. Combined PLGA scaffolds and therapeutic stem cells for locomotion recovery in spinal cord-injured rats: a systematic review and meta-analysis. Sci Rep 16, 14364 (2026). https://doi.org/10.1038/s41598-026-45065-4
Keywords: spinal cord injury, tissue engineering, stem cell therapy, biodegradable scaffolds, neural regeneration