Clear Sky Science · en
LDL-C modifies the association between triglycerides and depression identified by threshold scanning in US adults
Why Your Blood Fats Might Matter to Your Mood
Many people know that triglycerides and cholesterol affect heart health, but far fewer realize these same blood fats may also be linked to how we feel emotionally. This study asks a simple but important question: do certain combinations of blood fats make depression more likely, even when each fat alone looks harmless? By analyzing a large, nationally representative sample of U.S. adults, the researchers show that one particular pairing—high triglycerides together with high LDL cholesterol—appears to go hand in hand with a higher chance of depression.
Looking Beyond the Usual Suspects
Depression is one of the leading causes of disability worldwide, and a substantial share of patients do not improve enough with standard antidepressant drugs. At the same time, problems with blood fats—often called dyslipidemia—are extremely common. Earlier studies looking at single measures, like total cholesterol or triglycerides alone, have reported mixed and sometimes contradictory results about their connection to depression. The authors of this paper suspected that the missing piece might be how different fats interact with each other, rather than whether any one of them is high or low in isolation.
A Nationwide Health Survey as a Living Laboratory
To explore this idea, the researchers turned to the U.S. National Health and Nutrition Examination Survey, which regularly collects detailed health data from thousands of adults. They combined seven survey waves from 2005 to 2018, focusing on 8962 participants who had complete information on fasting blood fats and mood. Depression symptoms were measured using a standard nine-item questionnaire, and a commonly used score cut-off was applied to classify people as having or not having depression. The team also accounted for many other factors that could influence both mood and metabolism, such as age, sex, body weight, smoking, alcohol use, physical activity, income level, kidney function, high blood pressure, diabetes, and use of antidepressant or cholesterol-lowering drugs.
When Two Blood Fats Act Together
First, the scientists checked whether any single blood fat—triglycerides, total cholesterol, HDL "good" cholesterol, or LDL "bad" cholesterol—was clearly linked with depression after adjusting for all of those other influences. None showed a strong, independent relationship. The picture changed when they examined how pairs of fats behaved together. They found a statistically significant "synergy" between triglycerides and LDL cholesterol: as LDL rose, the connection between triglycerides and depression steadily grew stronger. Using a stepwise scanning method across the distribution of LDL values, they identified a threshold around 3.6 mmol/L. Above this point, higher triglycerides were clearly associated with greater odds of depression, while below it, triglycerides showed no meaningful link to mood.
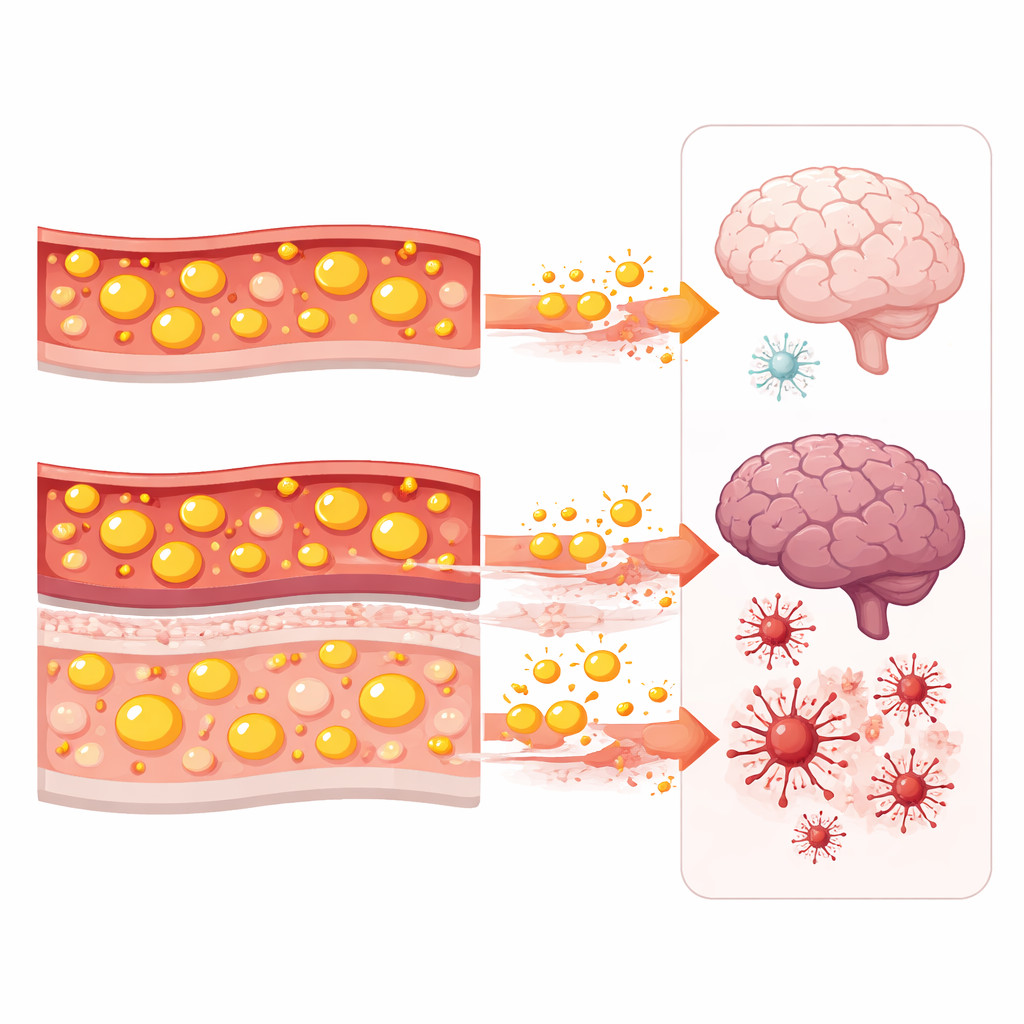
Stress at the Brain’s Front Door
What might explain this partnership between two types of blood fat and depression? The authors discuss emerging evidence that high LDL cholesterol can weaken the blood–brain barrier, the protective shield that normally limits what enters the brain from the bloodstream. When this barrier is impaired, fatty acids derived from triglycerides may slip into the brain more easily and activate immune-like cells called microglia. This activation can fuel low-level inflammation in brain tissue, which many studies have connected to depressive symptoms. In that scenario, LDL acts as a kind of gatekeeper: when it is high, the brain is more exposed to the inflammatory impact of elevated triglycerides, and mood may suffer as a result.
What This Means for Everyday Health
The study does not prove that blood fats cause depression, and because it is cross-sectional, it cannot show which came first—unhealthy lipids or low mood. Depression itself can alter diet, activity, and stress hormones in ways that disrupt fat metabolism. Still, the results point to a simple, practical idea: rather than looking at a single cholesterol number, clinicians might better judge depression risk by considering the overall pattern of blood fats, especially when both triglycerides and LDL cholesterol are elevated. If future long-term studies confirm that an LDL level of about 3.6 mmol/L truly marks a tipping point, combined lipid screening could become one more tool for identifying people whose mental health might benefit from closer monitoring—and from lifestyle or medical steps that improve both heart health and mood.
Citation: Li, S., Li, J., Xiang, F. et al. LDL-C modifies the association between triglycerides and depression identified by threshold scanning in US adults. Sci Rep 16, 11710 (2026). https://doi.org/10.1038/s41598-026-44940-4
Keywords: depression, triglycerides, LDL cholesterol, blood lipids, mental health