Clear Sky Science · en
Imaging improvements reveal guttae development and posterior fibrillar layer formation in fuchs endothelial corneal dystrophy
Why tiny bumps in the eye matter
The clear front window of the eye, the cornea, must stay perfectly smooth and transparent for sharp vision. In a common age‑related disease called Fuchs endothelial corneal dystrophy, people slowly lose this clarity and often need corneal transplants. This study looks closely at two microscopic changes on the inner surface of the cornea—little bumps called guttae and a veil‑like sheet of fibers—to understand how they form, how they relate to worsening vision, and how new imaging methods can help doctors judge disease severity and plan treatment.
Inside the eye’s clear window
The inner surface of the cornea is lined by a single layer of cells that act like tiny pumps, keeping the tissue free of excess water so it stays clear. These cells sit on a thin supporting sheet called Descemet’s membrane. In Fuchs dystrophy, stressed or aging cells begin to deposit extra material into this sheet, creating round protrusions known as guttae. Over time, these bumps scatter light and disturb the regular cell pattern, contributing to haze and swelling in the cornea. When the pump cells die off, the cornea fills with fluid, vision becomes cloudy, and many patients ultimately require a type of corneal transplant that replaces this inner layer.
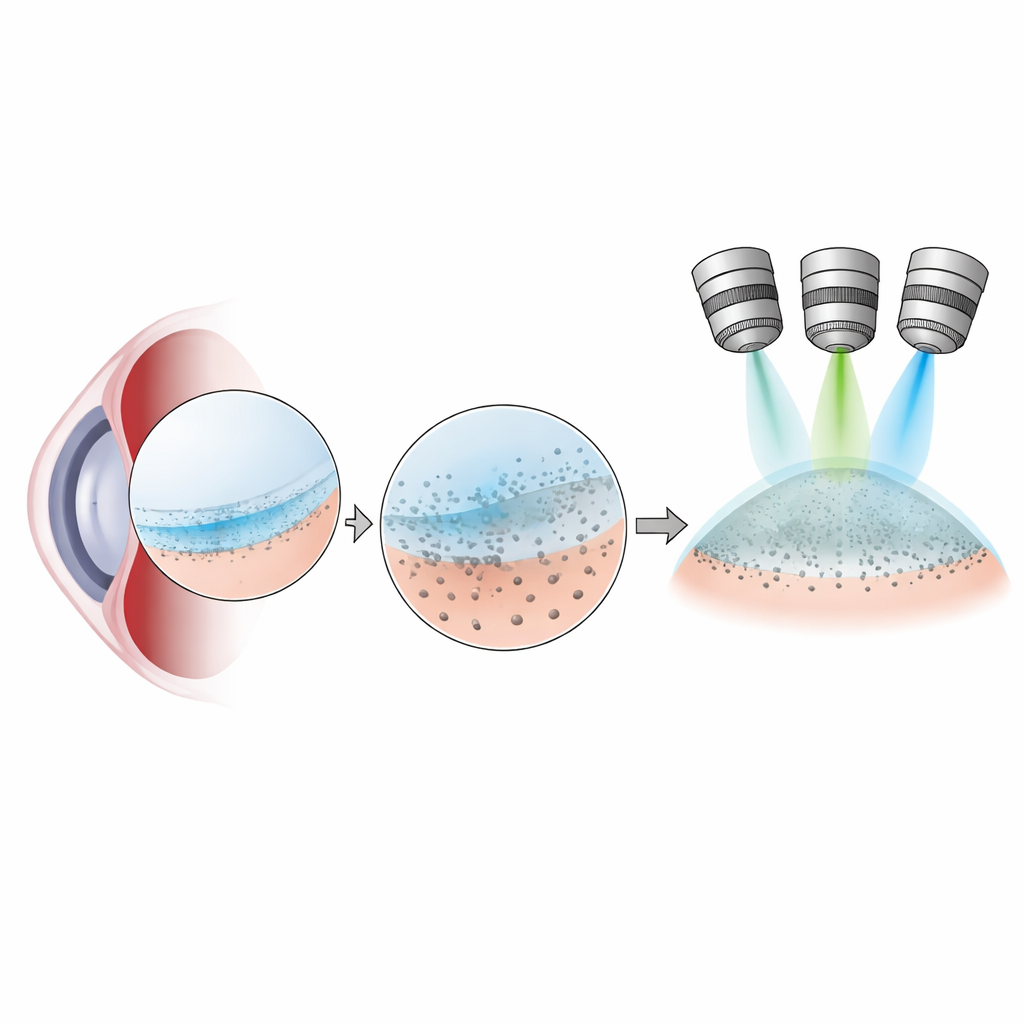
Sharper ways to see hidden damage
Traditionally, eye doctors spot guttae as shiny dots at the slit‑lamp microscope, and pathologists can see them at low detail in tissue removed during surgery. The authors set out to improve this view. Using corneal tissue taken during endothelial keratoplasty and from donor eyes, they applied a trio of imaging techniques: differential interference contrast (DIC) to show fine surface relief, autofluorescence to highlight naturally glowing deposits in the membrane, and polarized light microscopy to reveal ordered fibers, especially collagen. Together, these methods turned the inner corneal surface into a detailed landscape where individual guttae, their stages of growth, and a thin posterior fibrillar layer could be mapped across the entire specimen.
How bumps grow and a fibrous veil appears
The team found that guttae near the corneal edge are usually tall, knob‑like, and sharply outlined, while those in the center tend to be flatter and blurred by a mesh of fibers. Guttae glowed green when excited with blue light, and the brightness of this glow matched how much they stuck up from the surface, suggesting a progression from small, faint deposits to large, highly raised bumps. Early in the process, living endothelial cells still covered the guttae; later, the cells were pushed aside and often disappeared. In advanced central regions, the spaces between guttae filled with a collagen‑rich posterior fibrillar layer that spread as a thin cap over many bumps, creating a mushroom‑like profile in cross‑section.
From microscopic patterns to patient symptoms
By stitching together image series across each cornea, the researchers quantified how many guttae were present, how large they were, and how much of the surface was coated by the posterior fibrillar layer. Guttae turned out to be common not only in patients with Fuchs dystrophy but also in some older donor eyes, and guttae density did not reliably track how sick the cornea was. In contrast, the extent of the fibrillar layer strongly matched clinical signs of advanced disease: more of this fibrous sheet was linked to higher light scatter in front parts of the cornea and to greater swelling that needed to resolve after transplant surgery. The fibrillar layer also concentrated where endothelial cells were largely lost, underscoring it as a late, degenerative feature.
What this means for people with Fuchs dystrophy
For non‑specialists, the key message is that not all tiny bumps in the cornea are equal. While guttae signal that something is wrong, it is the spread of a collagen‑based fibrous veil between and over these bumps that best reflects severe, vision‑threatening damage. The imaging approach described here offers a clearer way to see and measure that veil in laboratory samples and could inspire improved tools for examining living eyes. In practical terms, focusing on the posterior fibrillar layer rather than just counting guttae may help doctors stage Fuchs dystrophy more accurately, choose the right timing for surgery, and better predict how quickly the cornea will clear after a transplant.
Citation: Zander, D.B., Kladny, AM.S., Lieberum, JL. et al. Imaging improvements reveal guttae development and posterior fibrillar layer formation in fuchs endothelial corneal dystrophy. Sci Rep 16, 10501 (2026). https://doi.org/10.1038/s41598-026-44926-2
Keywords: Fuchs endothelial corneal dystrophy, corneal guttae, posterior fibrillar layer, corneal imaging, Descemet membrane endothelial keratoplasty