Clear Sky Science · en
Automated grading and diagnosis of sacroiliitis on CT images using a 3D convolutional neural network: a multicenter retrospective study
Why this matters for back pain and joint health
Lower back pain that strikes in early adulthood and slowly worsens can sometimes signal ankylosing spondylitis, a long‑lasting form of spinal arthritis. Doctors rely on detailed imaging of the sacroiliac joints—where the spine meets the pelvis—to spot damage early and guide treatment. But these images can be hard to read and different specialists may disagree. This study explores whether a modern form of artificial intelligence can learn to read CT scans of these joints consistently, helping catch serious disease sooner and support doctors in busy clinics.
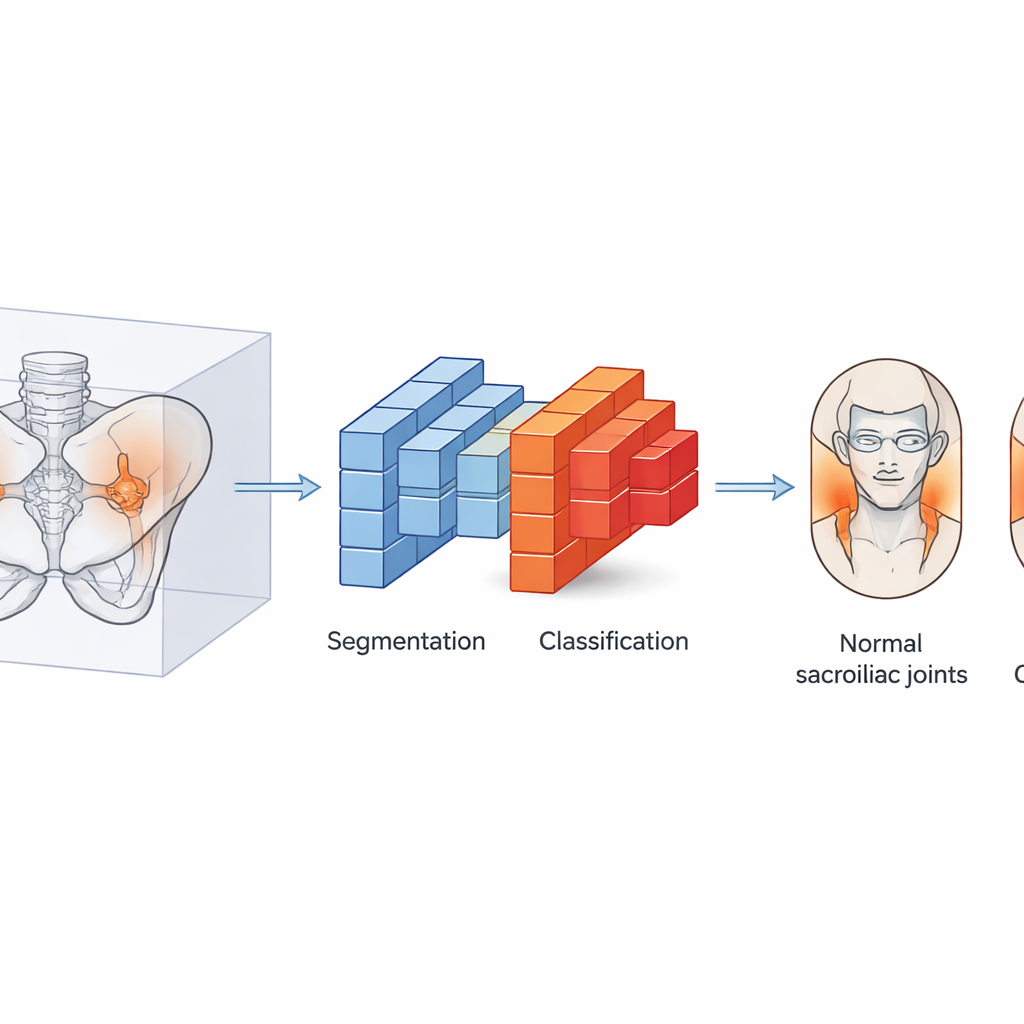
The hidden joints at the base of the spine
The sacroiliac joints sit deep in the pelvis, carrying the weight of the upper body into the legs. In ankylosing spondylitis, long‑term inflammation can gradually erode these joints and eventually fuse them into solid bone, leading to pain, stiffness, and reduced mobility. Doctors grade the damage on a five‑step scale, from normal to completely fused. Hitting certain grades is what confirms the diagnosis and shapes treatment decisions. Yet on standard X‑rays, early changes are subtle, and even experienced radiologists often disagree about which grade a scan deserves. While CT scans reveal bone detail much more clearly, systematically grading thousands of them is time‑consuming, and many hospitals lack subspecialist readers.
Teaching a computer to see what radiologists see
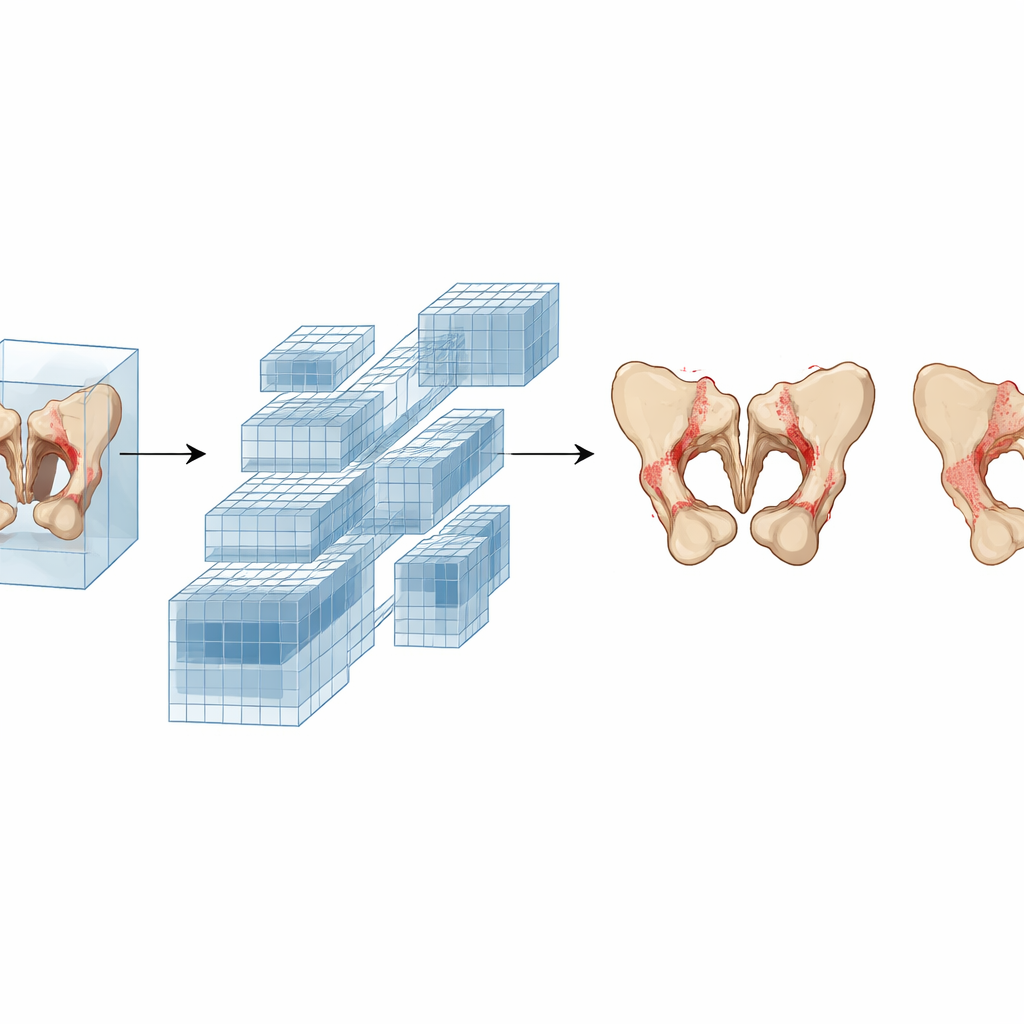
The researchers built an automated system that mimics how a careful specialist would approach a CT scan, but in three dimensions and at high speed. First, a segmentation model isolates the pelvic bones from the rest of the scan, focusing the analysis on the relevant region. Then a second model—based on a type of deep learning architecture called a 3D DenseNet—examines the bone structures slice by slice and assigns a grade. The team trained this system using CT scans from 2,144 people, including both healthy individuals and patients with suspected ankylosing spondylitis. Three radiologists graded every scan according to international criteria, and any disagreements were resolved by a senior expert, creating a rigorous "teaching set" for the AI.
How well the AI recognized joint damage
When asked to distinguish all five traditional grades of joint damage, the AI’s performance was strong across the board and excellent for the most advanced disease. Its ability to separate normal joints and fully fused joints from the rest was especially high, matching what would be expected from well‑trained human readers. The system was somewhat less certain when distinguishing the earliest visible damage from very mild change—exactly the range where doctors themselves most often disagree, because the signs blend into one another. To better match everyday clinical decision‑making, the team also grouped the five grades into three broader categories: normal or suspicious, definite structural damage, and advanced fusion. In this simplified setup, the AI became even more reliable and stable.
Proving it works beyond one hospital
A key question for any AI tool is whether it works only where it was born or also in other hospitals with different scanners and patient populations. To test this, the researchers evaluated their three‑category model on CT scans from two additional centers that had not been used during training. The system maintained high accuracy and confidence, correctly separating people without structural damage from those with clear disease, and identifying most cases of advanced fusion. Visualization techniques showed that the model focused its attention where a human would look—the sacroiliac joints themselves—rather than on unrelated anatomy, adding to clinicians’ trust in its decisions.
Working alongside radiologists, not replacing them
The team also studied what happens when radiologists use the AI’s suggestions while grading scans. Two experienced readers first graded images on their own, then reviewed the same cases with the model’s output. With this digital second opinion, both radiologists improved their accuracy by about 7–8 percentage points, and their agreement with each other rose noticeably. The AI did not remove all uncertainty, especially in borderline early cases, but it reduced disagreement and provided consistent support, particularly for recognizing more advanced damage.
What this means for patients and future care
In practical terms, this work shows that a well‑designed 3D deep learning system can automatically grade sacroiliac joint damage on CT scans with a level of consistency that rivals expert readers. Used as an assistant rather than a replacement, it could help catch serious structural changes earlier, standardize diagnoses across hospitals, and free radiologists to focus on the most complex cases. The authors note that CT reveals damage only after it has become permanent, so MRI and clinical judgment remain essential for spotting the very earliest disease. Still, as part of a broader toolkit, this AI‑driven approach offers a promising step toward more objective, reproducible care for people at risk of ankylosing spondylitis.
Citation: Du, Yk., Liu, R., Guo, H. et al. Automated grading and diagnosis of sacroiliitis on CT images using a 3D convolutional neural network: a multicenter retrospective study. Sci Rep 16, 14099 (2026). https://doi.org/10.1038/s41598-026-44911-9
Keywords: ankylosing spondylitis, sacroiliitis, CT imaging, deep learning, radiology AI