Clear Sky Science · en
Sex-biased plasma inflammatory protein profile in obesity
Why this matters for everyday health
Obesity is often discussed in terms of weight, diet, or exercise, but less attention is paid to what is happening silently in the blood. This study looks under the hood at the tiny signaling proteins that drive inflammation in people with excess body fat, asking a simple but important question: do women and men with obesity show different inflammatory patterns that could help explain why their heart disease risks are not the same?
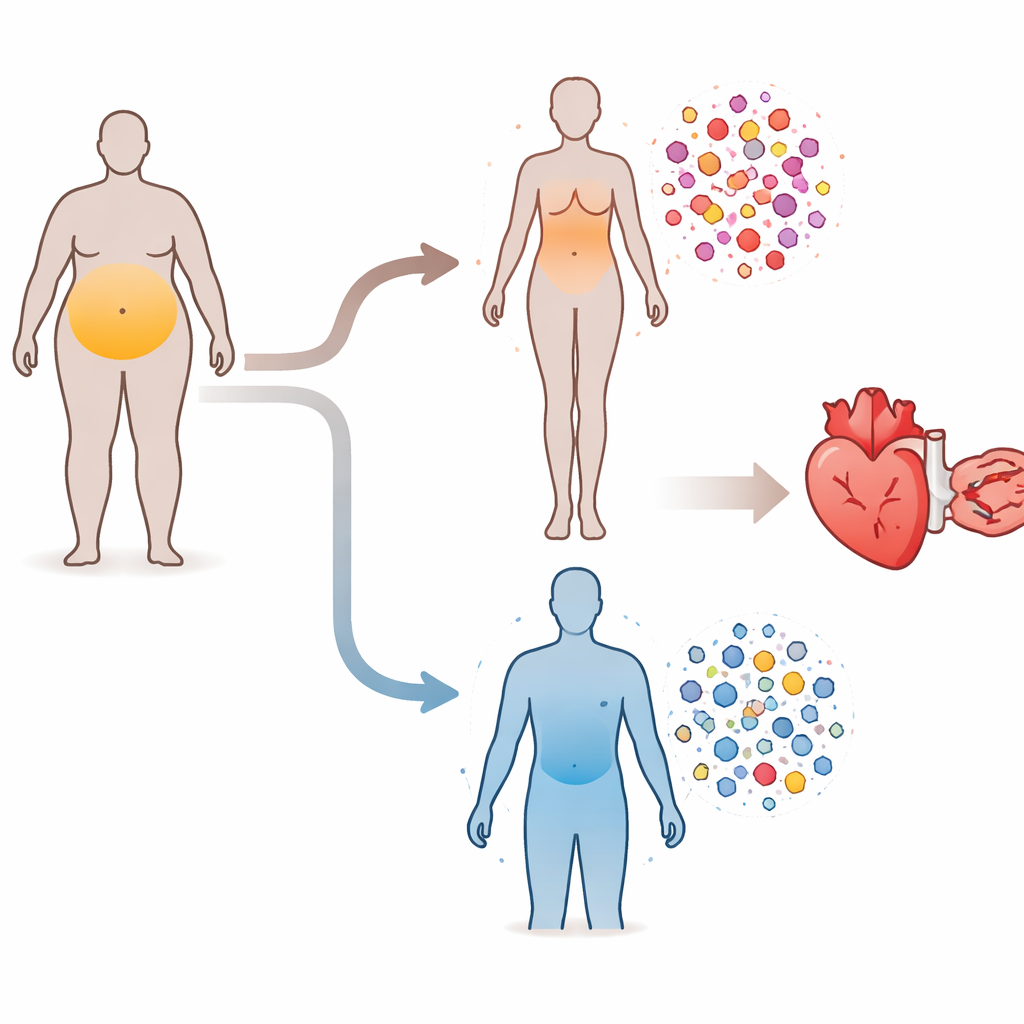
How body fat and inflammation are linked
Doctors have long known that carrying extra weight is tied to a higher risk of heart attacks, heart failure, and other cardiovascular problems. A key player in this link is chronic, low-grade inflammation—an ongoing, smoldering immune reaction that never fully turns off. Certain proteins in the blood, produced by immune and other cells, help control this response. When these proteins are out of balance, blood vessels and the heart can be damaged over time. Earlier research has suggested that women with obesity may carry a heavier inflammatory burden than men with similar body size, but the detailed patterns of these proteins had not been fully mapped in a sex-specific way.
Who was studied and what was measured
The researchers examined 450 adults in Norway, all with higher-than-normal body mass index and no known cardiovascular disease. Women and men were similar in age, body mass index, and rates of obesity, diabetes, and smoking, though high blood pressure was more common in men. From stored blood samples, the team measured 92 inflammation-related proteins using a sensitive panel; 81 proteins with reliable readings were used in the final analysis. They then compared people with and without obesity and looked separately at women and men, while also accounting for age, smoking, diabetes, blood pressure, and kidney function to isolate the specific contribution of obesity.
Different inflammatory fingerprints in women and men
When all participants were pooled together, obesity was linked to changes in only a small set of inflammatory proteins. But once the researchers split the data by sex, a striking pattern emerged. In women with obesity, several proteins tied to immune cell development and hormone and liver function shifted up or down in a characteristic way. In men with obesity, an entirely different set of proteins changed, including one involved in nerve and blood vessel health and others that help control how strongly inflammation is switched on or off. Surprisingly, there was no overlap at all between the specific proteins altered by obesity in women and those altered in men, even though both sexes shared an increased risk landscape for heart and blood vessel disease.
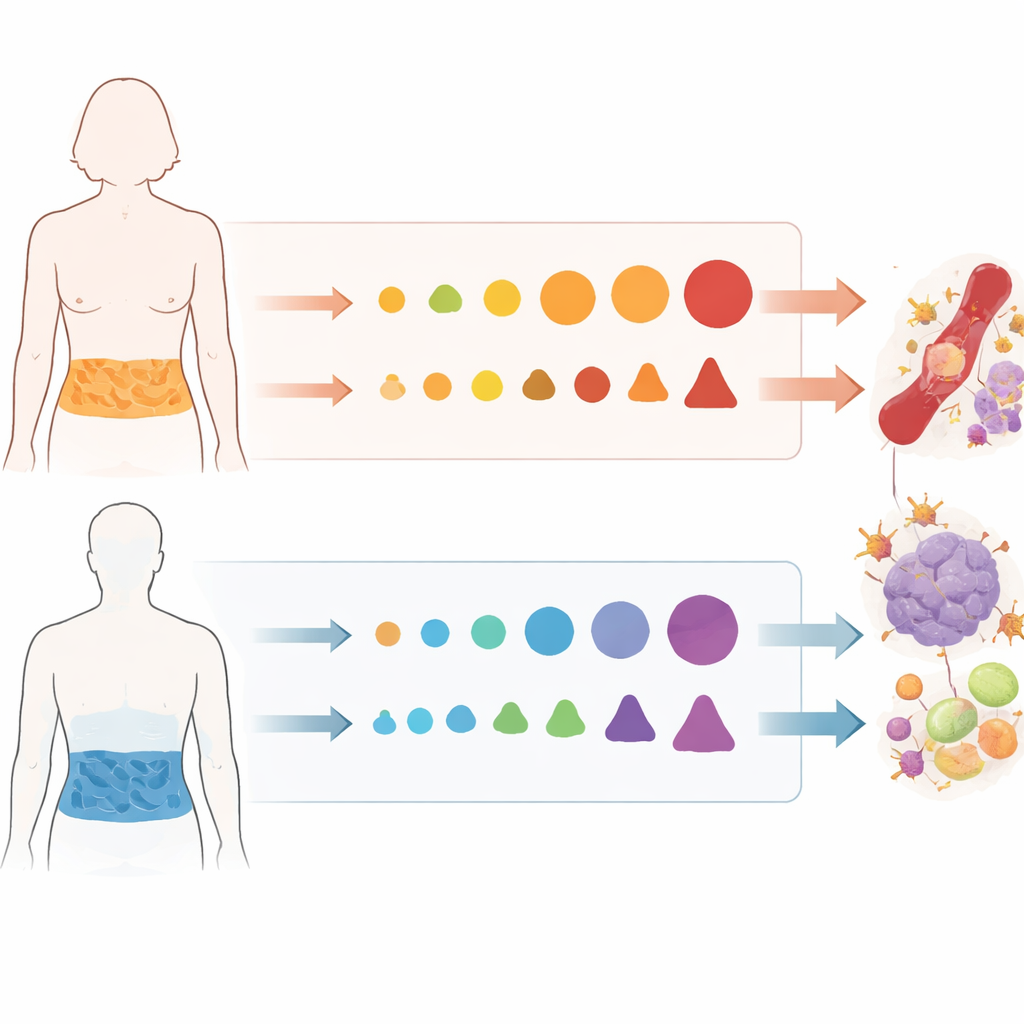
What this means for the heart and blood vessels
These sex-specific protein patterns suggest that the pathways leading from excess fat to cardiovascular harm are not identical in women and men. For women, shifts in proteins that guide immune cell traffic and long-term low-grade inflammation may gradually erode the health of blood vessels, helping explain why obesity can be a particularly strong risk factor for certain heart conditions in women. For men, changes in proteins that limit inflammation and support healthy cell survival may blunt the body’s ability to resolve inflammation, potentially worsening metabolic problems and damage to the cardiovascular system. The study also found that whether a woman was before or after menopause did not neatly sort people into distinct protein patterns, pointing to a more complex interaction between hormones, fat, and immunity.
Takeaway for future care and prevention
In plain terms, this research shows that “inflammation in obesity” is not a one-size-fits-all process: women and men appear to travel different biological roads that may lead to similar endpoints, such as heart disease. While the study is exploratory and based on one Scandinavian cohort, it highlights the need to consider sex when designing strategies to prevent and treat obesity-related heart problems. In the future, blood tests that read these inflammatory fingerprints could help doctors tailor prevention and treatment more precisely for women and men living with obesity.
Citation: Halland, H., Vitorino, R., Gerdts, E. et al. Sex-biased plasma inflammatory protein profile in obesity. Sci Rep 16, 14249 (2026). https://doi.org/10.1038/s41598-026-44223-y
Keywords: obesity, inflammation, sex differences, cardiovascular disease, proteomics