Clear Sky Science · en
Correlation between anti-retinal antibodies and lupus retinopathy in systemic lupus erythematosus
Why the Eyes Matter in Lupus
For many people living with systemic lupus erythematosus (SLE), a disease in which the immune system attacks the body’s own tissues, joint pain and fatigue are familiar problems. Less well known is that lupus can quietly injure the light‑sensing tissue at the back of the eye, the retina, sometimes leading to permanent loss of sight. This study asks a practical question with real impact for patients: can a simple blood test help doctors spot which lupus patients are at higher risk of vision‑threatening retinal damage?
The Immune System’s Mistaken Targets
The researchers focused on antibodies—immune proteins that normally fight infection—that in lupus can mistakenly recognize parts of the retina. They measured four such “anti‑retinal” antibodies in blood samples from 89 hospitalized lupus patients and 81 healthy people. Among the patients, 34 had clear signs of lupus retinopathy, the eye complication of lupus, while 55 did not. By comparing these groups, the team hoped to see whether certain antibodies were more common or reached higher levels in those with damaged retinas, pointing to potential warning markers that could be picked up long before serious vision loss occurs.
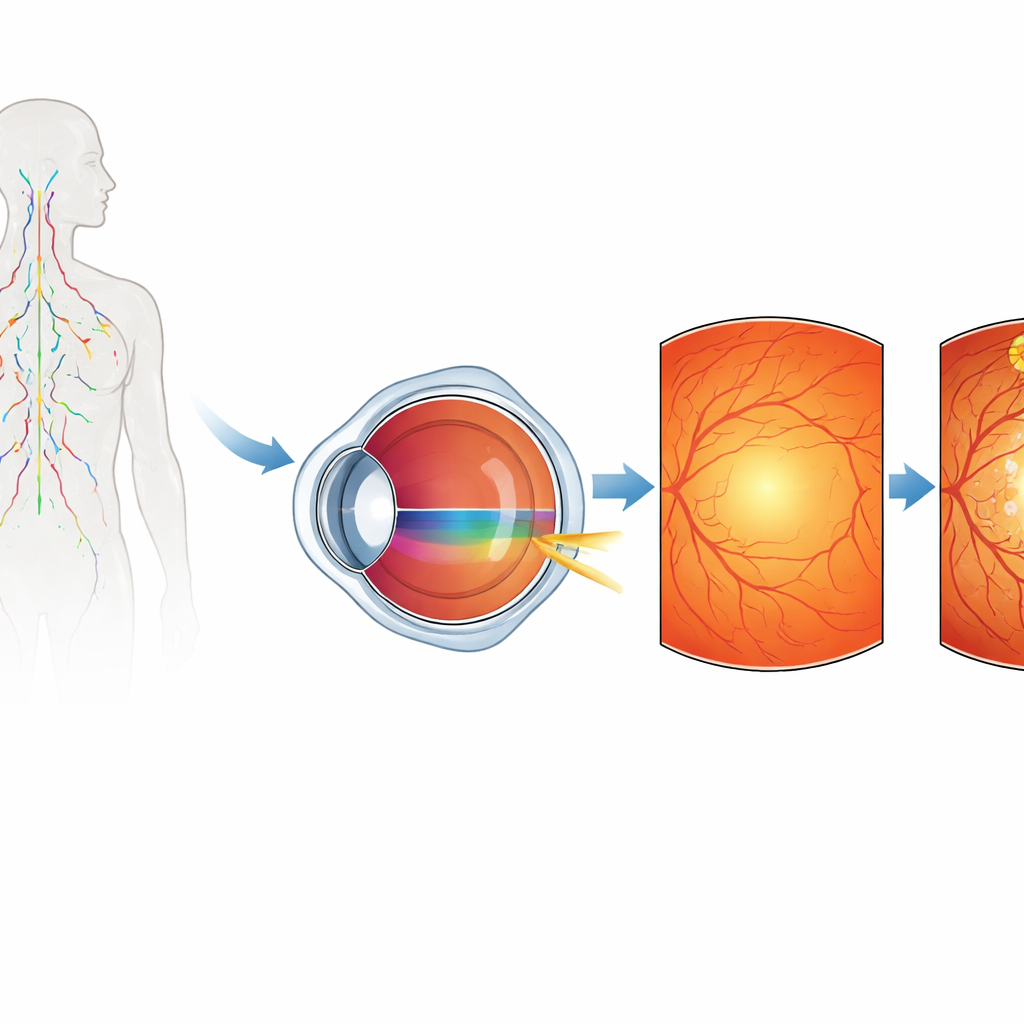
Who Was Studied and How
All participants underwent detailed eye examinations, including imaging of the back of the eye, along with standard blood tests used to track lupus activity. The patients with lupus retinopathy showed a wide mix of retinal problems: bleeding spots, cotton‑wool patches from tiny areas of nerve fiber damage, inflamed blood vessels, and in some cases swelling or blockage of major retinal vessels. As a group, these patients tended to have more active disease overall, more inflammation of the lung lining (pleurisy), and lower hemoglobin levels than lupus patients without retinopathy, suggesting that eye involvement often occurs in the context of more severe systemic illness.
Antibodies That Stand Out
When the team compared antibody levels, two patterns emerged. First, antibodies against a protein called alpha‑enolase were higher in lupus patients with retinopathy than in those without it, and both patient groups had higher levels than healthy controls. Second, antibodies against another retinal protein, recoverin, were clearly elevated only in the retinopathy group; levels in lupus patients without eye disease looked similar to those in healthy people. In contrast, antibodies against arrestin and IRBP3 did not differ meaningfully between patients with and without retinopathy, suggesting they are less useful for signaling who is at risk of retinal injury, at least in the early or moderate stages captured in this study.
Testing How Well the Markers Predict Eye Damage
To see how these findings might work in practice, the researchers used statistical tools commonly applied to diagnostic tests. Alpha‑enolase antibodies alone could distinguish retinopathy from no retinopathy with high accuracy on the “rule‑in” side: above a certain threshold, almost everyone with a high level truly had retinal disease, but many patients with retinopathy fell below that cutoff. Recoverin antibodies alone were more sensitive—catching more people with eye disease—but less specific, because elevated levels also appeared in some without retinal damage. When the two antibody measurements were combined in a simple mathematical model, performance improved: the combined marker did a better job of balancing sensitivity and specificity than either antibody by itself, suggesting that a dual‑antibody blood test could meaningfully aid clinical decision‑making.
What This Means for Patients and Doctors
In everyday terms, this work points toward a future in which regular blood tests might help eye doctors and rheumatologists decide which lupus patients most urgently need detailed retinal imaging and close visual follow‑up. Elevated alpha‑enolase and recoverin antibodies do not by themselves prove that sight will be lost, and the authors stress the study’s limits: the number of patients was modest, they were relatively severely ill, and the healthy comparison group was not perfectly matched in age and sex. Still, the pattern is clear enough to suggest that these two antibodies act as early warning flags for lupus‑related retinal damage. With larger and more diverse studies, such markers could become part of a screening toolkit that helps preserve vision in people living with lupus.
Citation: Zou, Q., Zhang, L., Li, M. et al. Correlation between anti-retinal antibodies and lupus retinopathy in systemic lupus erythematosus. Sci Rep 16, 13439 (2026). https://doi.org/10.1038/s41598-026-44125-z
Keywords: lupus retinopathy, systemic lupus erythematosus, retinal antibodies, autoimmune eye disease, biomarkers