Clear Sky Science · en
Predicting aggressiveness of clear cell renal cell carcinoma via mri using artificial intelligence: implications for surgical planning in a retrospective multicenter study
Why this matters for people facing kidney cancer
When a kidney tumor is found, one of the most urgent questions is how dangerous it is and how much of the kidney surgeons really need to remove. Today, doctors usually learn how aggressive a tumor is only after surgery, by examining it under a microscope. This delay can mean some patients lose more kidney tissue than necessary, while others may not receive treatment that is strong enough. This study explores whether artificial intelligence (AI) can read routine MRI scans to predict tumor aggressiveness in advance, helping doctors choose the safest, most effective operation.
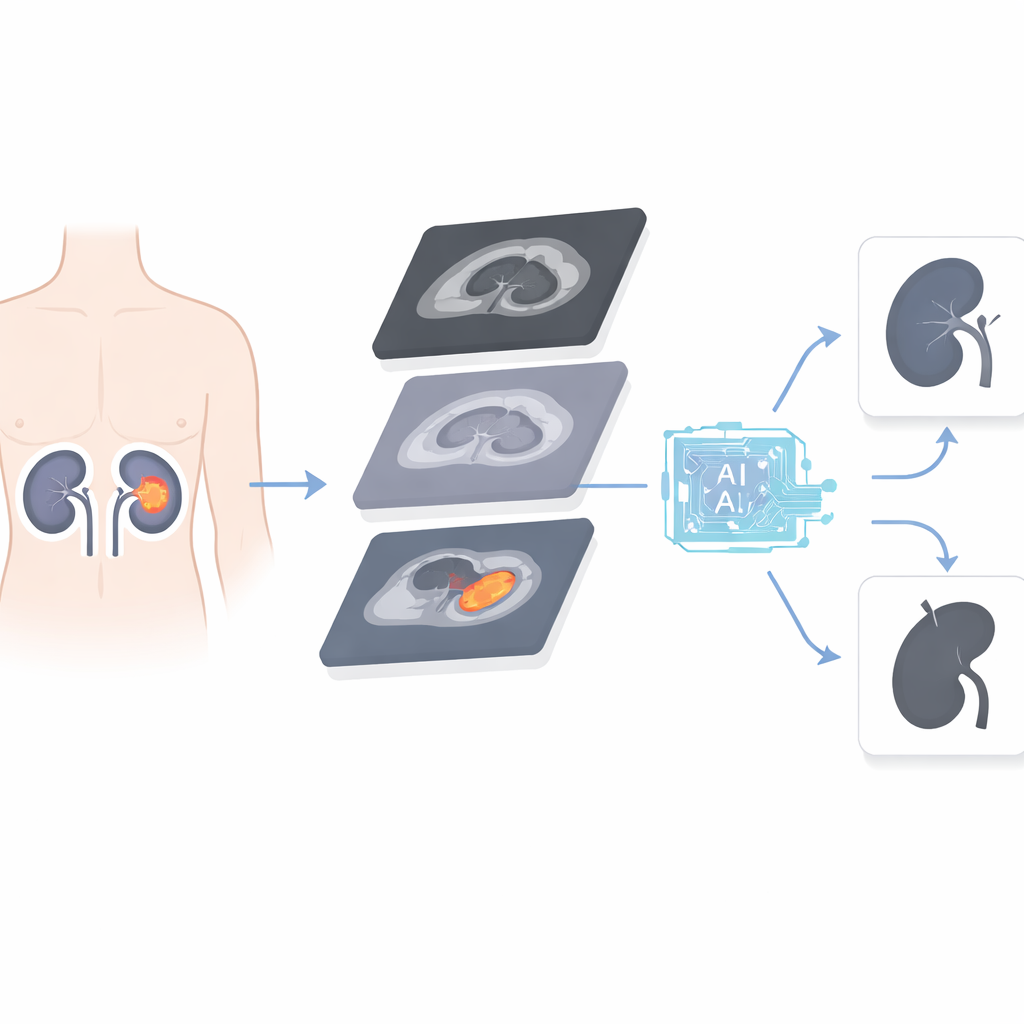
A closer look at a common kidney cancer
The research focuses on clear cell renal cell carcinoma, the most frequent type of kidney cancer. These tumors can behave very differently: some grow slowly and stay confined, while others spread quickly and threaten life. Surgeons must often decide between removing the whole kidney or just the tumor-bearing part. Current tools, such as a widely used scoring system based on a tumor’s size and position, estimate how difficult surgery might be but do not fully capture how aggressive the cancer really is. Needle biopsies can provide more detail but are invasive, time-consuming, and sometimes miss the most dangerous parts of a tumor.
Turning MRI scans into early warnings
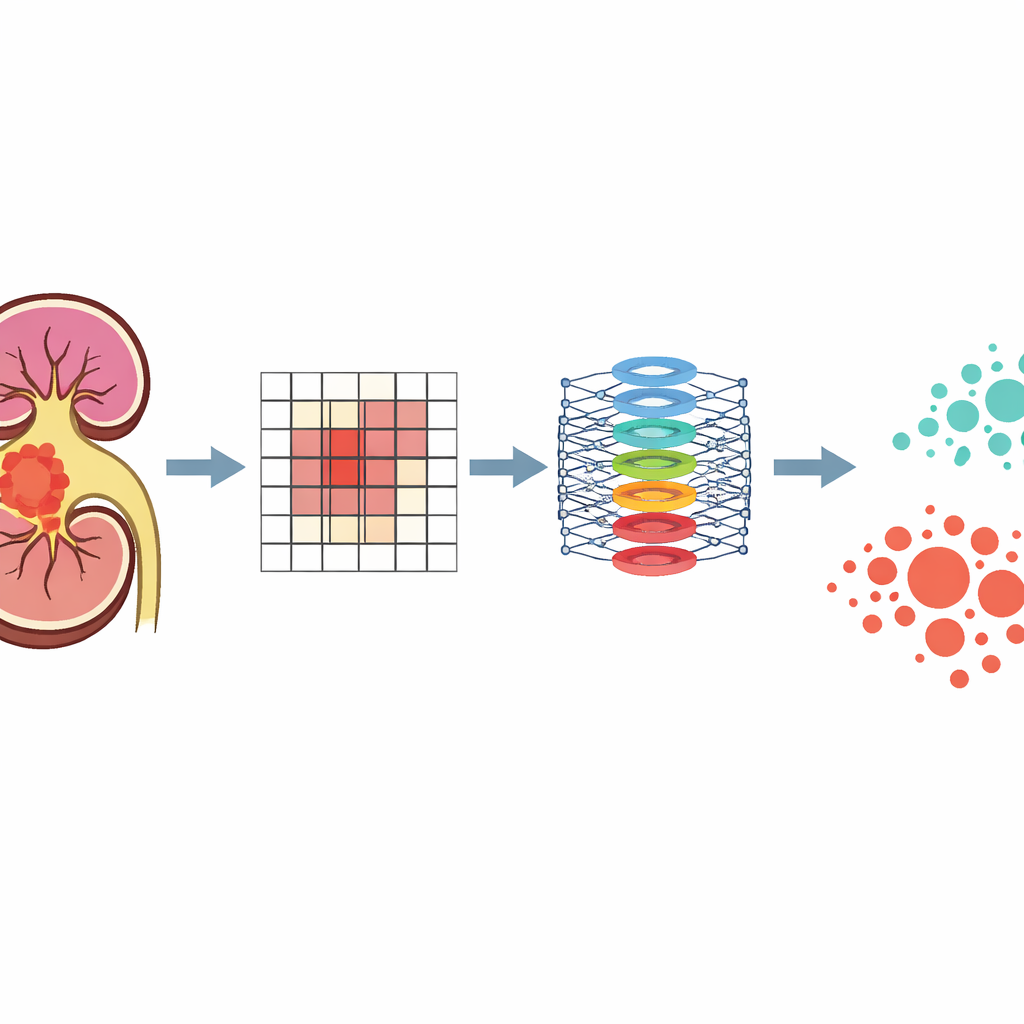
The team assembled MRI scans from 288 people treated for this kidney cancer at three hospitals in China over several years. All patients had standard MRI sequences that many hospitals already use: images that show anatomy clearly, pictures of how water moves through tissues, and maps of how tightly packed the cells are. The researchers built a two-step AI system based on a modern image-analysis method known as a vision transformer. First, they trained a “foundation” model on kidney MRI images that had no markings or labels, teaching the system to recognize general kidney structures and patterns. Then they fine-tuned this model using a smaller, carefully labeled group of cases where both the tumor’s location and its final laboratory grade were known.
How well the AI judged tumor danger
Once trained, the AI was asked to sort tumors into two groups: less aggressive (lower grade) and more aggressive (higher grade). In patients from the main hospital, the system correctly distinguished high-grade tumors at rates that exceeded the traditional anatomical score, especially in overall accuracy and in how often a “high-risk” flag truly meant the tumor was dangerous. In an independent group of patients from two other hospitals, the model performed even better, showing that it could handle different scanners and imaging conditions. Importantly, when the standard scoring system underestimated or overestimated tumor danger, the AI often got it right, especially in borderline cases where images could easily mislead the human eye.
What this could mean in the operating room
Because the AI works directly from pre-surgery MRI scans, it offers a non-invasive, repeatable way to estimate how threatening a tumor is before any cut is made. In practice, this kind of tool could sit alongside existing scores and the surgeon’s judgment, adding a “biological” view of the tumor on top of its shape and location. For a tumor that looks manageable but is flagged as highly aggressive, doctors might lean toward a more extensive operation. For one that appears complex but seems biologically mild, they might safely preserve more kidney tissue. The model also showed well-calibrated risk estimates and potential clinical benefit in formal decision analyses, suggesting it could meaningfully reduce both over-treatment and under-treatment.
From smart scans to more tailored care
The authors conclude that an AI system built on routine MRI scans can reliably forecast how aggressive clear cell kidney tumors are before surgery, and can outperform current imaging-based scoring methods. While the approach still needs to be tested in prospective, real-world studies and refined to be more transparent to clinicians, it points toward a future where kidney cancer surgery is guided not only by what tumors look like, but also by what their hidden patterns reveal. This shift could help patients keep more of their healthy kidney when it is safe to do so, or receive stronger treatment earlier when the danger is high.
Citation: Zhao, J., Wang, H., Liao, R. et al. Predicting aggressiveness of clear cell renal cell carcinoma via mri using artificial intelligence: implications for surgical planning in a retrospective multicenter study. Sci Rep 16, 13534 (2026). https://doi.org/10.1038/s41598-026-43983-x
Keywords: kidney cancer, MRI, artificial intelligence, tumor aggressiveness, surgical planning