Clear Sky Science · en
ProSeg: multi-scale context fusion for high-precision prostate segmentation in MRI
Why this matters for prostate cancer care
Magnetic resonance imaging (MRI) has become a key tool for finding and treating prostate cancer, but doctors still spend a lot of time tracing the gland and its internal zones by hand. Those outlines help decide where to biopsy, how to aim radiation, and how much tissue to remove during surgery. This paper introduces ProSeg, an artificial intelligence system designed to draw those boundaries automatically and more precisely, even when MRI scans come from different hospitals and machines.
Seeing the prostate as two very different regions
The prostate is not a uniform organ. Its outer shell, called the peripheral zone, is thin, irregular, and often where cancers first appear. Its inner core, the central gland, looks more uniform on MRI, with fuzzier borders. This contrast creates a double challenge: the outer layer demands extremely sharp boundary detection, while the inner region requires steady recognition of subtle texture patterns. On top of that, MRI scans vary widely in quality and appearance depending on scanner strength, coils, and imaging settings, which can blur or sharpen boundaries in unpredictable ways. Traditional computer vision systems struggle to meet all these demands at once.
How ProSeg learns from slices and from the whole volume
ProSeg tackles this problem with a specialized building block that works on two scales at the same time. One pathway focuses on local detail using direction-sensitive filters that follow the curved, paper-thin outline of the peripheral zone within each MRI slice. The other pathway looks across multiple slices, using an attention mechanism to recognize long-range patterns and relationships that define the central gland in three dimensions. A gated fusion step then decides, at each location, how much to trust the local boundary signals versus the broader context, producing a combined feature map that respects both fine edges and the organ’s overall shape. 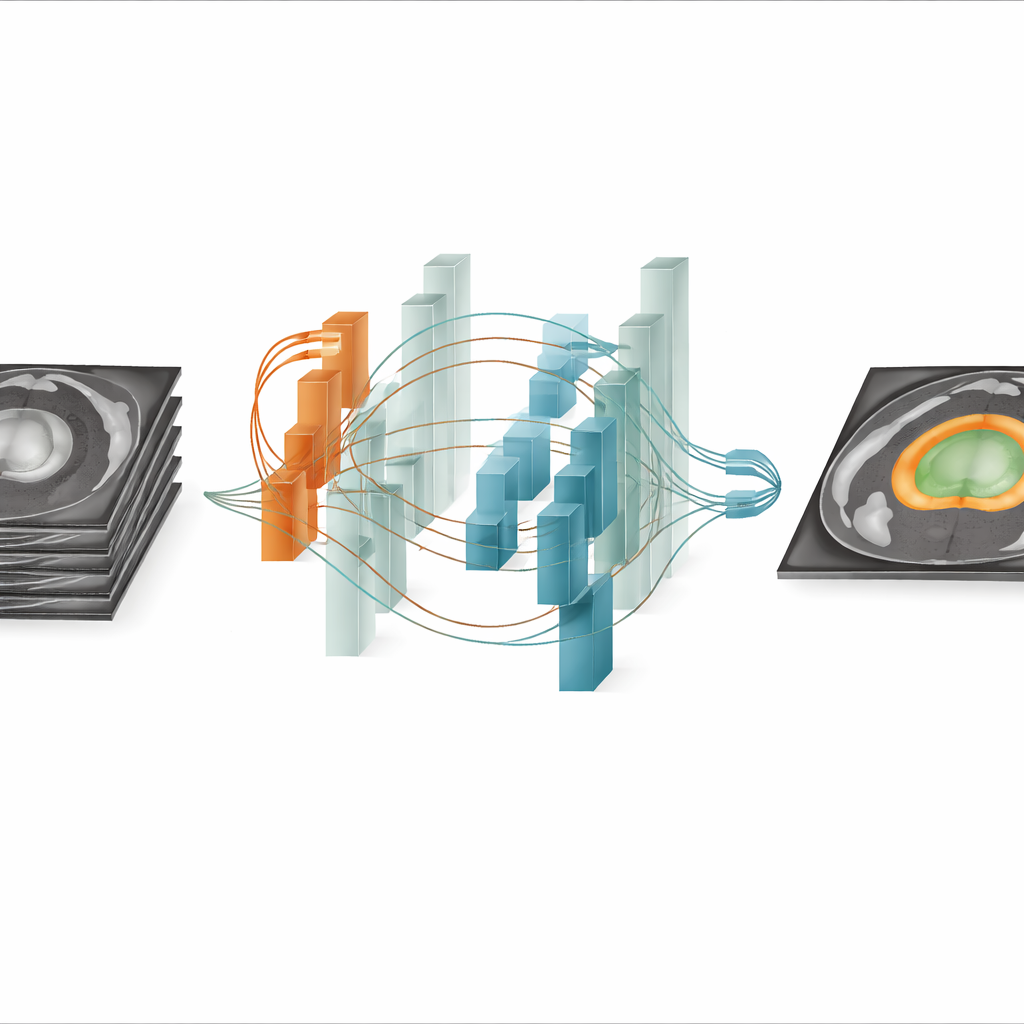
From raw images to clean 3D outlines
ProSeg is embedded in a classic encoder–decoder layout that compresses the 3D MRI data into multi-scale features and then reconstructs a full-resolution segmentation mask. Along the way, a feature pyramid network mixes detailed early information with deeper, more abstract cues. Special normalization layers help the model cope with differing MRI protocols, and a tailored loss function combines a region-overlap term (Dice loss) with a focal loss that pays extra attention to hard-to-classify border pixels. This design encourages the system to capture small structures without being misled by noise or uneven contrast. The end result is a voxel-by-voxel map that separates background, peripheral zone, and central gland in three dimensions.
How well it performs on real clinical datasets
The authors tested ProSeg on three widely used prostate MRI datasets—Promise12, Prostate158, and ProstateX—which include scans from different vendors, field strengths, and resolutions. Across these benchmarks, ProSeg consistently outperformed strong baselines such as UNet, Swin UNETR, and SegMamba. It achieved higher Dice scores for both the thin outer zone and the bulkier central gland, as well as better recall, meaning it missed fewer true prostate pixels and suspicious regions. Notably, ProSeg showed clear gains in challenging areas such as the apex of the gland and in small suspicious lesions, where millimeter-level accuracy can influence surgical margins or radiation targeting. 
What this could mean in the clinic
For a lay reader, the key message is that ProSeg offers a more reliable way for computers to "trace" the prostate and its key subregions on MRI scans, even when the images come from many different sources. By combining sharp local edge detection with a broad, slice-to-slice understanding of anatomy, the system produces cleaner, more consistent outlines than previous methods. In practical terms, this could shorten the time radiologists spend correcting automatic contours, reduce differences between observers, and support more precise biopsies, surgery, and radiation plans. While further work is needed—especially to handle the most ambiguous central gland regions and to integrate additional imaging types—the study suggests that carefully designed AI tools like ProSeg can move MRI-based prostate cancer care toward faster, more standardized, and more accurate decisions.
Citation: Qin, J., Yang, Y. ProSeg: multi-scale context fusion for high-precision prostate segmentation in MRI. Sci Rep 16, 13620 (2026). https://doi.org/10.1038/s41598-026-43589-3
Keywords: prostate MRI, medical image segmentation, deep learning, cancer diagnosis, radiation therapy planning